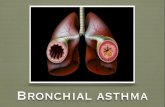
Bronchial asthma (VK)
-
Upload
an-vijaykumar -
Category
Education
-
view
19 -
download
1
description
Transcript of Bronchial asthma (VK)

PHARMACOLOGICAL BASIS OF
TREATMENT OF BRONCHIAL
ASTHMA

Asthma - Greek word meaning “to stay awake in order to breath” or “difficulty in breathing”
Asthma is a chronic inflammatory disorder of the airways.

Chronically inflamed airways are hyper responsive; they become obstructed and airflow is limited by :
1. Broncho-constriction 2. Mucus plugs 3. Increased inflammation when airways are exposed to various risk factors.

Asthma is a chronic inflammatory disease in
which the patient suffers with reversible
episodes of airways obstruction due to
bronchial hyper-responsiveness.

Predisposing factors:
Heredity Age: Pediatric group most affected Sex: within 10 years of age male:
female ratio(2:1) and equal in adults.
Allergens – Food, Inhalants, Bacteria.

Respiratory infections, pharmacologic stimulants occupational factors, exercise, climatic factors, low socio-economic status.
Passive smoking. Air pollution. Obesity.

Triggering Factors
Domestic dust mites
Air pollution
Tobacco smoke
Occupational irritants
Cockroach
Animal with fur
Pollen

Asthma affects 8% in adults and 10% in
children.
Asthma is common in industrialized nations
such as Canada, England, Australia, Germany,
and New Zealand, where much of the data have
been collected.
The prevalence rate of severe asthma in
industrialized countries ranges from 2-10%




Bronchial ToneBronchial Tone
BronchoconstrictionBronchoconstriction
BronchodilitationBronchodilitation
Bronchial Smooth Bronchial Smooth MuscleMuscle
IgE-Antigen ComplexIgE-Antigen Complex
BasophilBasophil
ActivatioActivationn
EosinophEosinophilil
ActivatioActivationn
Chemical mediatorsChemical mediators
Histamine, LTCHistamine, LTC44, LTD, LTD44, LTB, LTB44,,
Cytokines, Adenosine, PGDCytokines, Adenosine, PGD22, PAF,, PAF,ECP and NeuropeptidesECP and Neuropeptides
Cause inflammation, oedema, Cause inflammation, oedema, bronchospasm, muscus bronchospasm, muscus secretion, epithelial damagesecretion, epithelial damage
ββ22 AGONISTS AGONISTS Inhibit Inhibit releaserelease
ββ22
SALBUTAMOSALBUTAMOLLββ22 AGONISTS AGONISTS
ATATPP
ACAC
cAMPcAMP
CORTICOSTEROIDCORTICOSTEROIDSS
PDPDEE
AMPAMP
THEOPHYLLINETHEOPHYLLINE
MM33
GTGTPP
GCGC
cGMPcGMP
IPRATR
OPI
UM
IPRATR
OPI
UM
MM33
ANTA
GONIS
T
ANTA
GONIS
T
SS
AdenosineAdenosine
Mast CellMast CellDegranulatioDegranulationn
Pathophysiology

Bronchial Tone
Bronchoconstriction
Bronchodilitation
Bronchial Smooth Muscle
IgE-Antigen Complex
Basophil
Activation
Eosinophil
Activation
Chemical mediators
Histamine, LTC4, LTD4, LTB4,
Cytokines, Adenosine, PGD2, PAF,ECP and Neuropeptides
Cause inflammation, oedema, bronchospasm, muscus secretion, epithelial damage
CORTICOSTEROIDS
LT-ANTAGONIST
Leukotrienes
SOD. CROMOGLYCATE
Stabilises Mast Cells
Mast CellDegranulation
INFECTION
NITRIC OXIDE
DONORS


NEURAL CONTROLPARASYMPATHETICPARASYMPATHETIC
AcetylcholineAcetylcholine
Bronchial Bronchial Smooth MuscleSmooth Muscle
++
MM33
22
Circulating CatecholaminesCirculating Catecholamines
AdenosineAdenosine
AA22Mast CellMast Cell
AA33
NONO
++++
Neurokinin A Neurokinin A Substance PSubstance P++
NNAANNCC
MediatorsMediators
Unmyelinated Unmyelinated Sensory C fiberSensory C fiber
SOSO22, ,
Cigarette SmokeCigarette Smoke
SYMPATHETICSYMPATHETIC
Neuro-Neuro-peptidespeptides

ASTHMA MANIFESTS AS
1. Breathlessness and
2. Cough
3. Recurrent episodes of wheezing
4. Chest tightness

Goals of asthma therapy
› To prevent chronic and troublesome symptoms
› To maintain near normal pulmonary function
› To maintain normal activity levels (including
exercise and other physical activity)
› To prevent recurrent exacerbations of asthma
and minimise the need for emergency
department visits to hospitalizations

› To provide optimal pharmacotherapy with
minimal or no adverse effects
› To meet pts & families expectations and
satisfaction with asthma care.

Drugs used in Bronchial Drugs used in Bronchial Asthma Asthma
1. Selective β2- Agonists Short acting Salbutamol Terbutaline Remiterol Fenoterol
Long-acting Salmeterol, Formoterol, Bambuterol.
2. Non-selective Sympathomimetics
Adrenaline Ephedrine, Isoprenaline, Orciprenaline,
(Metaproterenol). Isoetharine.
BronchodilatorsBronchodilators

3. Anticholinergics - Ipratropium, Tiotropium,
Oxitropium,
4. Methyl Xanthines- Theophylline, Aminophylline,
Diprophylline, choline theophyllinate.
Anti inflammatory drugs.Corticosteroids
1. Oral: Prednisolone, Methylprednisolone,
2. Parenteral: Mehtyl Prednisolone, Hydrocorticsone
3. Inhalational: Beclomethasone, fluticasone,
Triamcinolone, Budesonide, Flunisolide

Mast Cell Stabilisers
Sodium Cromoglvcate, Nedocromil, Ketotifen,
Leukotriene Modulators:
1. 5-Lipoxygenase inhibitor: Zileuton
2. LT-rceptor Antagonists: Zafirlukast,
Montelukast, Iralukast, Pranlukast,
Monoclonal Anti-lgE Antibody
omalizumab

1. β2-Selective adrenoceptor agonist
most widely used sympathomimetics for the
treatment of asthma at the present time.
1. Short acting:- albuterol-Terbutaline
used only for acute attack of
bronchospasm
1. Long acting:- salmeterol –formeterol
used for only prophlaxis and not for acute
attack of bronchospasm.

Selective β2 receptor agonist
mechanism of action
Bronchial smooth
muscle relaxation
Stimulation of Stimulation of β2-receptors
Intracellular Intracellular cAMPcAMP

Selectively β2 receptor agonist
1. Route of administration: Usually delivered via a metered dose inhaler
with immediate effect Orally used in children. i.v used for acute attack. S.C. (terbutaline)2. Adverse effect: Cardiac arrhythmias (at high dose has β1
effects) Tolerance to β agonist (tachyphylaxis) Skeletal muscle tremors.

Non-selective
Sympathomimetics Adrenaline/epinephrineAdrenaline/epinephrine:
Agonist of α and β receptor
Adverse effect of cardiovascular system usually
occurs thereby less usable
S.C. injection
Ephedrine:Ephedrine:
Orally administered
Similar action to Adrenaline
Less usable for central excitation

Mechanism of Action: It stimulates the β2 receptors and cause bronchodilation.
Rout of administration:
As aerosol
Adverse effects:
Tachycardia,
Hypertension
Worsening of angina and even arrhythmias

They are divided into two types:
1. Salt complex: increased water solubility
without augmentation of pharmacological
action, such as: aminophylline.
2. Slow-release form: small fluctuation of
blood concentration after oral administration
thus used for nocturnal attack of asthma.

Theophylline
Mechanism of action
Inhibit activity of PDE cAMP
bronchial relaxation
cAMP AMP
3. Inhibition of the cell surface receptor of
adenosine
PDEPDE

Theophylline
1. Route of administration: Orally Metabolised by P450 enzyme system
2. Pharmacodynamics Direct positive chronotropic and inotropic
effects on the heart. In large dose, these agents also relax
vascular smooth muscle.

Theophylline:
Adverse effect
It has a narrow therapeutic index
Its therapeutic and toxic effects are related to
its plasma concentration.
<20mg/L: nausea, vomiting, headache,
anxiety, abdominal discomfort.
20-40mg/L: arrhythmia

Muscarinic antagonist
1. Mechanism: Act by competitive blocking of muscarinic
receptors (M3 subtype)
2. Route of administration: Metered dose inhaler e.g Ipratropium
bromide
3. indication: Used as adjuncts to β2-adrenoceptor agonist
in treatment of asthma.

Anti-inflammatory drug Glucocorticoids
Mechanism:
1. Depress the inflammatory response in bronchial
mucosa thus diminish bronchial
hyperresponsiveness.
2. Anti-inflammatory effect (inhibit
phospholypaseA2)
3. Immunosuppressive effect.

Glucocorticoids
Route of administration
1. Metered dose inhaler: (deeply & slowly
inhale) Beclomethasone, dexamethasone
2. Intravenous used for: severe asthma status
asthmaticus (prednisolone or
hydrocortisone)
3. oral

Monoclonal anti IgE antibody Omalizumab
Mechanism of action:
It prevents the binding of IgE to mast cell &
thus prevents mast cell degranulation
Rout of administration:
i.v or s.c
Side effects:
Redness, stinging, itching, induration.

1. NSAIDS like aspirin,ibuprofen,diclofenac etc.
(paracetamol can be used)
2. Beta-adrenergic blockers
3. Cholinergic agents.

1. Mild episodic asthmaInhaled short-acting beta2
agonist at onset of each episode (step-1)
2. Seasonal asthmastart regular inhaled cromoglycate/low dose
inhaled steroid(200-400micro g/day) 3-4 wks before
anticipated seasonal attacks continue till 3-4 wks
after the season is over treat individual episodes
with inhaled short acting β2 agonist.

3. Mild chronic asthma with
occasional exacerbations: regular inhaled cromoglycate, episodic-short
acting β2 agonist(step-2)
4. Moderate asthma with frequent
exacerbations: increases doses of steroid (up to 800μg/day)
+inhaled long acting β2 agonist(step-3)

5. Severe asthma:
Regular high dose inhaled (steroids 800-2000μg/day)
though a large volume spacer device + inhaled long-
acting β2 agonist (salmeterol) twice daily .

6. Status asthmaticus
Any pt of asthma has the potential to develop
acute severe asthma which may be life
Threatening.
upper respiratory tract infection is the most
common precipitant.

Hydrocortisone hemisuccinate 100mg I.V stat
followed by 100-200mg 4-8 hourly infusion
Nebulized salbutamol (2.5-5mg)+ipratropium
bromide (0.5mg) intermittent inhalations driven
by 02.
Management of status asthmaticus

High flow humidified oxygen inhalation.
Salbutamol/terbutaline 0.4mg i.m/s.c may be
added, since inhaled drug may not reach smaller
bronchi due to severe narrowing/plugging.
Intubation & mechanical ventilation, if needed.

Treat chest infection with intensive antibiotic
therapy.
Correct dehydration and acidosis with
saline+sod. bicarbonate/lactate infusion.

Aerosol Delivery of Drugs
High local concentration in bronchioles
Low systemic side effect.
Increased bioavailability.
Optimal particle size for deposition in small
airways – 1to 5μm

Four classes of antiasthma drugs, i.e β2 agonists,
anti-cholinergics, cromoglycate and
Glucocorticoids are available for inhalational use.
They are aimed at delivering the drug to the site
of action so that lower dose is needed and
systemic side effects are minimized.
Most asthma patients are now maintained on
inhaled medication only.

Aerosol Delivery Devices:
Liquid aerosols Metered dose inhaler (MDI)
Nebulizer
Powdered drugs Dry powder inhaler (DPI), Spinhaler, Rotahaler

Pressurized Metered Dose Inhaler (pMDI)
In pMDI drug is dissolved or suspended in propellant under pressure and when actuated releases a predetermined dose.
Pressurized MDI can be used with spacer or without spacer.
User of spacer improves drug deposition in lungs and reduces oropharyngeal drug deposition.
Use of spacer reduces oropharyngeal drug deposition by 10-15 folds when compared to pMDI alone.

Spacer acts as reservoir for drug from which
patients can breathe easily.
Depending on patient’s technique, drug
delivery varies from 7 to 20%.
An oropharyngeal drug deposition is about
80% with pMDI.

The particle size distribution through HFA was
1.07 micrometer and that of with CFC is 3.36
micrometer.
Lung deposition of drug with HFA is 50% while
with CFC it is 10-20%.
With HFA the oropharyngeal deposition is 30%
whereas with CFC it is 90-94%.

Spacer/holding chamber
Slow (3-5 secs) inhalation or tidal breathing
immediately following actuation
Easier to use than MDI alone
Recommended for anyone using MDI
Spacer

Nebulizers Nebulizer convert a liquid solution or
suspension into an aerosol using either a jet or ultrasonic energy.
Aerosol is then delivered to the patient through either a face mask or a mouthpiece.

Nebulzer requires least patient cooperation and coordination.
Nebulzers are preferred in patients who are unable to use other devices or in acute attacks when inspiratory flow is
limited.

Only about 13% of the dose used is
deposited in the lungs.
The doses used in nebulizers are higher than
those used in other aerosol devices.
Therefore patients will receive 10-20 times
the dose received from a MDI.

Dry Powder Inhaler (DPI) In PDI drug is provided as micronized particles in
large aggregates with or without carrier substances.
Drug delivery in DPI depends on patient’s inspiratory effort to disperse the drug and deliver it to the lungs.
Drugs deposition in lungs with DPI is 15-40% with considerable inter device variability and drug deposition in oropharynx is <60%.
DPI dose not require propellants and hand breath
coordination

› Rapid (1-2 secs), deep inhalation; dose lost if
client exhales through device
› Population: > 4-5 years
Rotahaler

Spinhaler
1. Hold spinhaler upright with mouthpiece downwards, and unscrew body
2. Put coloured end of spincap into cup of propeller, making sure it spins freely3. Screw the two parts together and hold horizontal. Move grey sleeve up and down

once or twice, this will pierce capsule
4. Breathe out gently, tilt head back, put
spinhaler into mouth so lips touch flange and breathe in quickly and deeply
5. Remove spinhaler from mouth and hold
breath for about 10 seconds, then breathe out
slowly
6. If any powder is left in spincap, repeat steps
4 and 5 until it is empty
Always Demonstrate To The Patient How To Use The Spinhaler

Route of Administration & Dose
Drug Route & Dose
1. Selective β2 Agonists Salbutamol
Inhalant: 90 μg/puff aerosol; 0.83, 0.5% solution for nebulized Oral: 2,4 mg tab; 2mg/5ml syrup.
Formoterol Inhalant: 12 μg/puff aerosol. 12mg/unit inhalant powder.
Salmeterol Inhalant aerosol: 25 μg salmeterol base/puff in 60 & 120 dose containers inhalant powder50 μg/ unit
Terbutaline Inhalant: 0.2mg/puff aerosol.Oral: 2.5, 5 mg tab.

Cont….2. Selective Sympathomimetics Ephedrine
Oral: 25mg capsules Parenteral: 25,50mg/ml/ injection
Epinephrine Inhalant: 0.1,1, 2.25% for nebulization Parenteral: 1:10000 (0.1mg/ml)
3. Anti-cholinergics Ipratropium.
Aerosol: 18mg/μg/puff in 200 metered-dose inhaler.
4. Methyl xanthenes Aminophylline
Oral: 105mg/5ml liquid, 100, 200mg tablet
5. Leukotriene Inhibitors Montelukast Zafirlukast Zileuton
Oral: 10 mg tablets, chewable tabletsOral: 20 mg tabletsOral: 600 mg tablets

Cont…
6. Corticosteroids Beclomethasone Budesonide Dexamethasone
Aerosol Powder: 42 μg/puff in 200 dose container Aerosol Powder: 160 μg/activation
Aerosol powder: 84 μg/puff in 170 dose container
7. Mast cell stabilisers Cromolyn sodium Nedocromil sodium
Pulmonary aerosol: 800 μg/puff in 200 dose container; 20mg/2ml for nebulization. Pulmonary aerosol: 1.75 mg/puff in 113 metered-dose container.

Asthma cannot be cured but can be controlled
with regular use of medications.
Asthma is treated with two types of medicines:
Long term control
Quick-relief medicines

Long term control medicines help to reduce
airway inflammation and prevent asthma
symptoms.
Quick-relief,or “rescue", medicines relieve
asthma symptoms that may flare up.
Initial asthma treatment will depend on
severity of the disease.

Patient counseling on drug therapy should
concentrate on drugs used to relieve
symptoms, drugs used to prevent asthma
attacks and those drugs which are given only
as reverse treatment for severe attacks.