Acute Tonsil Lo Pharyngitis Uti
-
Upload
patty-boone -
Category
Documents
-
view
229 -
download
1
Transcript of Acute Tonsil Lo Pharyngitis Uti

RN HEALS
CASE PRESENTATION

General Data A case of Meting. 7 y.o., male, Filipino,
Roman Catholic, residing at Benolho, Albuera,Leyte was check for the several times at this center last January 17,2011.

Chief Complaint “Nag-sige siya hilanat, balik-balik” as verbalized by the mother.

History of Present Illness 1 day prior to check-up
febrile (Temp 38.5°C) (+) headache (+) productive cough (+) decreased appetite & activity (-) colds, vomiting, diarrhea Paracetamol at 250mg every 4 hours

Few hours prior to check-up fever persisted (+) dizziness (+) loss of appetite consulted private physician CBC = ↑ WBC 31.30/hpf

Review of SystemsGeneral : no weight lossSkin : no rashesHead : no lightheadednessEyes : no pain, no blurring of visionEars : no pain, no vertigoNose :no colds, no epistaxisThroat : (+) pain, no hoarsenessNeck : no pain, no stiffnessRespiratory : no dyspneaCardiovascular : no chestpainGIT : (+) abdominal pain, no dysphagiaGUT : no dysuria, no hematuria, no oliguria, no
urgency/frequencyMusculoskeletal : (+) body malaise, no muscle/joint painNeurological : no seizure

Past Medical HistoryPast hospitalization : Pneumonia (2007)
Dengue Fever( 2006), admitted at OSPA-FMC x 5days, tx unrecalled meds
Past illness :FeverPast surgery : noneAccidents & Injuries : FallAllergies : none

Maternal/Birth History born to 29y.o G1P0, non smoker and non
alcoholic mother prenatal check up started 2mos. AOG,
monthly thereafter regular intake Multivitamins & Ferrous
sulfate no illness, bleeding, exposure to radiation,
teratogen delivered full term via spontaneous vaginal
delivery, no complications observed

Feeding History exclusively breastfed x 6 months shifted to formula milk consuming 6-8 bottles
(4oz)/ day supplementary feeding at 6 mos. with no
particular food preference

Growth and Development 6 mos.- rolls over, can chew 9 mos.- stands with support, says Ma,Da18 mos.- walks well, drinks from cup2 y.o- runs well, able to remove clothes3 y.o- can tell little stories, play with peers, toilet
trained by day4 y.o- able to count nos. up to 10, toilet trained by
day5 y.o- daycare student, able to draw6 y.o- kinder student, can write fairly well7 y.o- grade one student, able to add & subtract
nos., participate in class activityPatient is at par with age.

Immunization (all vaccines given at a local health center in
Benolho,Albuera)
(+) BCG- 1 dose (+) DPT- 3 doses (+) OPV- 3 doses (+) Hep B- 3 doses (+) Measles- 1 dose

Family History Mother- 29y.o, apparently well Father- 36 y.o, apparently well Siblings:
None Heredofamilial diseases: (-) HTN, (-) DM, (-) CA Others: (-) exposure to person with PTB

Psychosocial History lived with parents and siblings in well-lit and
ventilated house use purified water for drinking grade one student, achiever in class

Physical ExaminationGeneral Survey: awake, conscious,
ambulatory, weak-looking, fairly nourished, fairly groomed, not in distress:
BP: 100/60 mmHg Wt: 20.7 Kg (p10)
HR: 124 bpm (60-100) Ht: 115 cm (p10)
RR: 32 cpm (14-22) Temp: 38.6°C (≥37.8)

Skin: warm, moist, good turgor, no active lesions
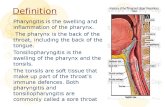
HEENMT: atraumatic, normocephalic, pink palpebral conjunctivae, anicteric sclerae, no tragal tenderness, patent auditory canal, intact tympanic membrane, no alar flaring, moist lips and buccal mucosa, hyperemic enlarged grade 2 tonsils, no exudates, nonhyperemic posterior pharyngeal wall
Neck: supple, no palpable cervical lymph nodes, no nuchal rigidity

Chest and Lungs: symmetrical chest expansion, no retraction, equal tactile fremitus, resonant all lung fields, clear breath sounds
Heart: adynamic precordium, PMI palpable at 5th ICS L MCL, tachycardic at 124bpm regular rhythm, no murmur
Abdomen: flat, soft, no tenderness, no organomegaly, normoactive bowel sounds

Genital: grossly male, uncircumcisedBack & Spine: no deformity, no
costovertebral tendernessExtremities: no edema, no cyanosis, good
capillary refill, full and equal pulses

Neurological Examination GCS: 15 Mental / Speech status: awake, conversant, follows commands Cranial Nerves: I- able to smell coffee candy II- pupils 2-3mm, equally reactive to light III ,IV, VI- EOM intact V- able to chew VII- no facial asymmetry VIII- hearing intact IX, X- (+) gag reflex XI- able to raise shoulder, can turn head side to side XII- tongue at midline Motor: 5/5 on all extremities Sensory: no sensory deficits Reflexes: ++ in all reflexes

Impression
Tonsilitis and UTI


Urinalysis color- yellow leuc. est. (-) transparency- hazy blood (-) pH 5.0 RBC 5.50/uL sp gr 1.030 ↑ WBC 33/hpf(0-1)
sugar trace protein trace Bact. 88.80/uL ketones +1 crystals (-)nitrites (-) casts (-)

ESR = ↑72mm/H (0-15)
Na = ↓132meq/L (136-145) K = 3.90meq/L (3.5-5.1)




Final Diagnosis Urinary Tract Infection

Salient FeaturesAcute Tonsillopharyngitis
Urinary Tract Infection
7y.o throat pain enlaged hyperemic
tonsils CBC: ↑WBC
31.30/hpf
↑segmenters 95%
febrile episodesvomiting abdominal pain uncircumcised UA: ↑ WBC 33/hpf


Acute TonsillopharyngitisStreptococcal pharyngitis: AKA strep throat or
strep tonsillitisthroat infection caused by Streptococcus bacteria.
Complications: rheumatic fever, acute glumerolonephritis
Causative agents: Viruses: adenoviruses, coronaviruses, enteroviruses,
rhinoviruses, RSV, EBV, HSV , metapneumovirusgroup A β-hemolytic streptococcus (GABHS)

PathogenesisViral URTI transmission
Streptococcal pharyngitis – peaks early in shool years
Colonization of pharynx by GABHS- result either asymptomatic carriage or acute infection
M protein – major virulence factor of GABHS

Manifestations sore throat, fever, absence of cough headache, abdominal pain & vomiting pharynx is red, tonsils enlarged with
yellow, blood-tinged exudatepetechiae or “doughnut” lesions on soft
palate & posterior pharynxuvula red, stippled & swollen anterior cervical lymph nodes enlarged &
tender

Diagnosis Goal: to identify GABHS infection Diagnostics: throat culture & rapid strep
test

TREATMENTPenicillin- narrow spectrum & few
adverse effectsOral amoxicillinsingle IM dose Benzathine penicillin or
Benzathine-Procaine penicillin G combination

Erythromycin- for patients allergic to β-lactam antibiotics
Cephalosporins- more effective in eradicating streptococcal carriage
Paracetamol- for aches, pains or fever

Urinary Tract Infection State in which organisms actively multiply and
persist in the GUT occur in 3–5% of girls and 1% of boys In girls: first UTI usually occurs by the age of 5
years, with peaks during infancy and toilet training
In boys: 1st yr of life, much more common in uncircumcised boys, male : female ratio 2.8–5.4 : 1
Beyond 1–2 years striking female preponderance, male : female ratio of 1 : 10

Etiology UTIs caused mainly by colonic bacteria In females: 75–90% of all infections caused by E.
coli, followed by Klebsiella spp. and Proteus spp. In males (› 1 yo): Proteus as common as E. coliStaphylococcus saprophyticus and enterococcus
are pathogens in both sexes.UTIs are ascending infections: arise from the
fecal flora, colonize the perineum, and enter the bladder via the urethra.
In uncircumcised boys: bacterial pathogens arise from the flora beneath the prepuce.

PathogenesisIs based on the presence of bacterial pili or
fimbriae on the bacterial surfaceType I fimbriae: found on most strains of E.
coli., referred as “mannose-sensitive”
Type II fimbriae: known as “mannose-resistant, can agglutinate by P blood group erythrocytes, known as P fimbriae
Bacteria with P fimbriae are more likely to cause pyelonephritis.

ManifestationsIn neonates: lethargy, fever or temperature
instability, irritability & jaundice In older infants: fever, vomiting and irritability In young children: nocturnal enuresis or daytime wettingIn older children: low-grade or no fever, dysuria, urinary frequency, or urgency

Risk Factors female gender uncircumcised male vesicoureteral reflux toilet training voiding dysfunction obstructive
uropathy urethral
instrumentation wiping from back to
front in females
tight clotting (underwear)
pinworm infestation constipation anatomic
abnormality ( labial adhesion)
nerupathic bladder sexual activity pregnancy

DiagnosisUA & Urine culture are necessary for
confirmation and appropriate therapy. A midstream urine sample usually is satisfactory. If the culture shows >100,000 colonies of a
single pathogen, or if there are 10,000 colonies and the child is symptomatic, the child is considered to have a UTI.
In uncircumcised males - prepuce must be retracted prior to urine collection.
In infants - adhesive, sealed, sterile collection bag after disinfection of the skin of the genitals can be useful, particularly if the culture is negative.

Treatment Empiric antibiotic- started in
symptomatic patients with a suspicious UA while culture result are pending
Toxic-appearing children- admitted to the hospital for initial IV antibiotics and hydration.
Oral antibiotics - are started once the child has shown initial improvement.