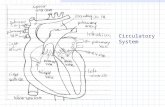
Fig. 20-1, p. 670 The Cardiovascular System Overall function: transport nutrients, gases, hormones,...
-
Upload
belen-lane -
Category
Documents
-
view
214 -
download
0
Transcript of Fig. 20-1, p. 670 The Cardiovascular System Overall function: transport nutrients, gases, hormones,...

Fig. 20-1, p. 670
The Cardiovascular System• Overall function: transport
nutrients, gases, hormones, wastes, immune cells, etc. throughout the body
• It has 3 main parts:– Fluid = blood (Ch. 19),
which is a fluid connective tissue
– A pump = the heart (Ch. 20)– Pipes/tubes/hoses = blood
vessels (Ch. 21)

Ch. 19 – Blood• = a specialized fluid CT containing cells that
are suspended in a fluid matrix
Blood keeps you happy!

Functions of blood• 1. Transportation of:
– Dissolved gases, nutrients, hormones, metabolic wastes, heat, etc.
• 2. Regulation of the pH and ion composition of interstitial fluid– Blood contains buffers to stabilize pH– The constant diffusion between blood and interstitial fluid
eliminates ion concentration differences between them• 3. Restriction of fluid loss at injury sites
– Due to hemostasis and clotting• 4. Defense against toxins and pathogens
– By white blood cells and antibodies• 5. Body temperature stabilization
– Blood can absorb, redistribute, and/or dissipate heat

Characteristics of normal whole blood• 1. Temperature ~ 38°C (100.4°F)• 2. Viscosity = stickiness, cohesiveness, or
thickness– Blood is 5X more viscous than water– When viscosity ↑ even more (e.g. during
dehydration), → ↑ resistance to flow, so it’s harder for the heart to pump
• 3. pH = 7.35-7.45 (slightly alkaline)• 4. Blood volume
– Can be estimated (in liters) as ~ 7% of body weight (in kg)• Adult male: 5-6 liters• Adult female: 4-5 liters

The composition of whole blood• 1. Plasma (~ 55%) = a fluid
matrix• 2. Formed elements (~ 45%)
= blood cells and cell fragments– Red blood cells (RBCs, or
erythrocytes)– White blood cells (WBCs, or
leukocytes)– Platelets (“thrombocytes”)
• Hemopoiesis = blood cell formation– Hemocytoblasts in the bone
marrow differentiate → myeloid stem cells + lymphoid stem cells
• Lymphoid stem cells differentiate → lymphocytes
• Myeloid stem cells differentiate → other formed elements
Fig. 19-1, p. 640

Plasma• Is similar in composition to
interstitial fluid, except plasma has many more proteins
Fig. 19-1, p. 640-641

Fig. 19-1, p. 640-641
Formed elements
See Table 19-3 for more details

Red blood cells
+ Platelets
Fig. 19-2a, p. 644
• Are a.k.a. RBCs, or erythrocytes • Make up 99.9% of formed elements • There are ~ 4-6 million RBCs per μL
(mm3) of whole blood• Are packed full of hemoglobin = a
red-pigmented protein which carries most (~ 98.5%) of the O2 in blood, and some CO2 too
• Hematocrit = the % of whole blood that is formed elements– It’s a.k.a. the packed cell volume (PCV)– Average in males = 46%– Average in females = 42%
• The sexes are different because androgens stimulate erythropoiesis

Fig. 19-2bc, p. 644
RBC structure• RBCs are biconcave discs about 8 μm in diameter• In mammals, RBCs do not contain a nucleus or most other
organelles when mature– They retain the cytoskeleton – They do not have mitochondria – No nucleus means they cannot divide, so they have a limited lifespan
(~ 120 days)• That’s OK: ~ 3 million new RBCs are produced per second in the red
bone marrow

Fig. 19-2d, p. 644
Advantages of a biconcave disc shape• 1. A large surface area-to-volume ratio, which…
– ↑ Diffusional exchange across the RBC membrane • 2. It facilitates flow through narrow vessels
– RBCs stack single-file like dinner plates• 3. It allows bending and flexing of the RBC
membrane– RBCs can flow through 4 μm diameter vessels!

Fig. 19-3, p. 645
Hemoglobin (Hb)• = globin (4 polypeptides) + 4 heme units
– The polypeptides (in adults) = 2 α and 2 β chains – Heme = an iron-containing pigment (which is bright red when O2 is
bound to it) • O2 reversibly binds to the iron (Fe2+) in the heme
– Each Hb molecule can therefore bind to and carry 4 O2
– Hb (hemoglobin or deoxyhemoglobin) + O2 ↔ HbO2 (oxyhemoglobin)
• Note: the globin of Hb can bind to and transport CO2 during low-O2 conditions (forming carbaminohemoglobin)
Normal Hb range (in whole blood) = 12-18 g/dL

RBC formation
and turnover
Fig. 19-5, p. 647
(from globin)

Fig. 19-6, p. 648
Erythropoiesis = RBC production
(beginmaking Hb)
Reticulocytes:• Make up < 1% of circulating RBCs• Mature after about a day in the blood
Hemocytoblast Myeloid stem cell

More on erythropoiesis• It requires:
– Amino acids (for the globin of Hb)– Iron (for the heme of Hb)– Vitamins (B12, B6, and folic acid), which are necessary cofactors– Intrinsic factor from the stomach (to absorb B12 from dietary sources)
• The stimulus for RBC production is hypoxia = low tissue O2– Some causes of tissue hypoxia:
• Anemia (= ↓ O2-carrying capacity of the blood)– This is often caused by a decreased hematocrit or [functional Hb]
• Low blood flow to the kidneys• Decreased O2 content of the air (e.g. high altitude)• Lung damage
• Hypoxia causes erythropoietin (EPO) to be released from the kidneys– EPO stimulates erythropoiesis, by:
• 1. Stimulating mitosis in erythroblasts and their associated stem cells• 2. Increasing RBC maturation and Hb synthesis rate
– EPO can increase RBC production 10X (up to 30 million/sec!!!)

Blood types• Antigens = substances (usually proteins) that can trigger an immune response
– Surface antigens are found on cell membranes; they’re “ID tags” that are recognized by immune cells as being either from you (“self” or “normal”) or not from you (“non-self” or “foreign”)
• Antibodies (immunoglobulins) = plasma proteins that can recognize and bind to specific antigens
• RBC membranes may have glycolipid or glycoprotein surface antigens (specifically called agglutinogens)– The most important agglutinogens = A, B, and Rh; which ones are present is genetically
determined• The plasma may contain certain anti-RBC antibodies (specifically called agglutinins)
– E.g. anti-A and anti-B (their presence is also genetically determined); anti-Rh (previous exposure to Rh is needed for it to be present)
• The binding of antibodies to antigens can cause:– Agglutination (clumping) – causing downstream tissue to die; and/or– Hemolysis (rupture of RBCs) – causing vasoconstriction, shock, and kidney damage
Fig. 19-7b, p. 651

Fig. 19-7a, p. 651
ABO blood types and transfusions
• When figuring out if a particular blood transfusion will be theoretically successful (i.e., the recipient won’t have a potentially lethal cross-reaction), ask yourself:
“Does the recipient’s blood contain antibodies that can attack antigens on the donated red blood cells?”
Yes? – Very BAD No? – Probably O.K.

The Rh factor• “Rh” comes from the Rhesus monkey, in which this antigen
was first studied– They’re also called D antigens
• A person with Rh antigens on their RBCs is Rh+ (Rh positive) • A person without Rh antigens on their RBCs is Rh- (Rh
negative)
• Major differences compared to A and B antigens:– An Rh- person who has never been exposed to Rh+ blood does
NOT have anti-Rh antibodies– Anti-Rh antibodies from a mother can cross the placenta and
enter the fetal bloodstream• This can cause hemolytic disease of the newborn (HDN), a.k.a.
erythroblastosis fetalis – see the next slide

Fig. 19-9, p. 654-655
Rh factor and
pregnancy

Fig. 19-8, p. 652
Blood type testing
• In a lab, the blood sample is mixed with various antibodies
• Cross-reaction (clumping) indicates the presence of the cor-responding antigen
(Anti-Rh)

White blood cells• Are a.k.a. WBCs, or leukocytes• Make up < .1% of formed elements (5000-10,000/μL)• Are nucleated• Do not have hemoglobin • Circulate in the blood for a limited time
– They migrate to connective and lymphoid tissues in the body• So circulating WBCs are only a fraction of the total WBCs in the
body• General function: defense against pathogens, toxins,
and abnormal cells (more on this in Chapter 22)• Traditional classification:
– Granulocytes (have stained vesicles):• Neutrophils, eosinophils, and basophils
– Agranulocytes (apparently lack vesicles after staining):• Monocytes and lymphocytes

Characteristics of circulating WBCs• 1. They can migrate out of the bloodstream
– First, they adhere to the wall of a blood vessel (margination)
– Then, they squeeze between the endothelial cells of the vessel wall to escape into the tissues (emigration or diapedesis)
• 2. Amoeboid movement– They can move along vessel walls and throughout the
tissues• 3. Positive chemotaxis
– They are attracted to specific chemical stimuli• 4. Phagocytosis (= engulfing pathogens, cell debris,
etc.)– Microphages = neutrophils and eosinophils– Macrophages = monocytes

Fig. 19-10a, p. 656
Neutrophils• Are a.k.a. polymorphonuclear leukocytes
• Normally are the most numerous WBC (50-70%)
• Are highly mobile, but have a relatively short lifespan
• Structure:– They contain relatively neutral-staining
granules (i.e. not very pink or very purple)– They are ~ 12 μm in diameter– They have a multi-lobed nucleus
• Functions – the “first line of defense”:– 1. Phagocytize pathogens (usually bacteria):
• Especially those “marked” by antibodies or complement proteins– 2. Destroy pathogens by using:
• Strong oxidants (e.g. H2O2)• Defensins = chemicals that poke holes in bacterial membranes• Digestive enzymes (e.g. lysozyme)
– 3. Release signaling chemicals, such as:• Prostaglandins (which promote inflammation)• Leukotrienes (which attract other WBCs)

Fig. 19-10b, p. 656
Eosinophils• Normally make up 2-4% of
WBCs• Structure:
– They contain pink-, red-, or orange-staining granules
– They usually have a bi-lobed nucleus
– They are ~ 12 μm in diameter• Functions:
– 1. Via exocytosis, release toxic compounds (e.g. nitric oxide) onto large pathogens (such as some parasitic worms)
– 2. Phagocytize antigen-antibody complexes– 3. Release antihistamine
• Which inhibits the inflammatory response, limiting the spread of inflammation to adjacent tissues

Fig. 19-10c, p. 656
Basophils• Are normally rare: they make
up < 1% of WBCs• Structure:
– They contain purple-staining granules
– They often have an obscure (purple) nucleus
– They are 8-10 μm in diameter
• Function – intensify inflammation:– Release histamine, which dilates small vessels and
increases capillary wall permeability (→ edema/swelling)– Release heparin (an anti-coagulant)

Fig. 19-10d, p. 656
Monocytes• Normally make up 2-8% of WBCs• Structure:
– They are agranular– They are LARGE cells (12-20
μm in diameter)• (In lab, look for a cell 2-3X larger
than a RBC)– They have a kidney- or U-shaped
nucleus• Functions:
– Migrate to tissues; they may become wandering or fixed macrophages
– Aggressive phagocytosis– Act as antigen-presenting cells for other WBCs– Release chemotactic chemicals, which call other WBCs to
the site of the battle

Fig. 19-10e, p. 656
Lymphocytes• Make up 20-30% of the WBCs in the blood
• Structure:– They have a roundish nucleus, with a sliver
of cytoplasm visible (no distinctive granules)– They are 6-14 μm in diameter
• Frequently migrate between the blood and peripheral tissues– At any given time, most are in the tissues
and lymphoid organs• Functions:
– 1. B cells are responsible for “humoral/ antibody-mediated immunity”
• They mature in the bone marrow, and migrate to the lymph nodes• When activated, they differentiate into plasma cells, which secrete
antibodies – 2. T cells are responsible for “cell-mediated immunity”
• They mature in the thymus• They attack virus-infected and cancerous cells, and transplanted tissues• They include cytotoxic T cells, helper T cells, and suppressor T cells
– 3. Natural killer (NK) cells perform “immune surveillance”• They recognize a wide variety (i.e., they are nonspecific) of antigens that
they can attack and kill, such as microbes and cancerous cells

Fig. 19-11, p. 659
WBC origins/ differentiation
This figure is for big picture ideas only – DO NOT memorize the whole thing!
when activated, lymphocytes release…

Platelets• Are sometimes a.k.a. “thrombocytes” (but
they’re not really cells in humans—just cell fragments)
• There are 150-500K per μL of whole blood• Structure:
– They are fragments of megakaryocytes– They are about 1-4 μm in diameter– They stain purple in lab– They contain vesicles (but the vesicles are not really visible in lab)
• Production = thrombocytopoiesis– This process is stimulated by thrombopoietin from the kidney, interleukin-6,
and multi-CSF – 1 megakaryocyte → ~ 4000 platelets
• “Live” (circulate) for about 9-12 days• About 1/3 of the total amount in the body are stored in the spleen and
other organs, ready to be mobilized if needed• Functions:
– 1. Release clotting chemicals– 2. Form a platelet plug (= a temporary patch over a hole in a blood vessel)– 3. Contract after the clot has formed, which reduces the size of hole in the
vessel
Fig. 19-2a, p. 644
Platelets

Fig. 19-12, p. 663
Hemostasis• = the stoppage of bleeding
• Consists of 3 phases:– 1. The
vascular phase
– 2. The platelet phase
– 3. The coagulation phase (blood clotting)

Fig. 19-12, p. 662
1. The vascular phase• A. Vascular spasm = a reflexive
contraction of the smooth muscle in the wall of the blood vessel– The vessel diameter ↓, blood flow ↓,
so blood loss ↓• B. Endothelial changes:
– The endothelial cells contract, exposing the basement membrane to the blood
– The endothelial cells release chemicals and hormones, including endothelins, which:
• ↑ The smooth muscle contraction• ↑ Endothelial cell division to
accelerate repair– The endothelial cell membranes
become “sticky”• So the vessel walls may stick
together to repair small breaks (such as in capillaries), and it’s easier for platelets to attach

Fig. 19-12, p. 662
2. The platelet phase• A. Platelet adhesion –
platelets adhere to the sticky endothelium, and the exposed basement membrane and collagen
• B. Platelet aggregation → platelet plug formation
• C. Newly arriving platelets are activated and secrete chemicals (this is the 1st positive feedback loop):– ADP → ↑ aggregation and
secretion
– Thromboxane A2 and serotonin → vasoconstriction
– Clotting factors (see the next phase)
– Platelet-derived growth factor (PDGF) → vessel repair
– Ca2+ → ↑ aggregation and clotting

3. The coagulation phase (blood clotting)• Plasma contains clotting factors (procoagulants), which include Ca2+
and 11 different proteins (many of which are proenzymes)• Activation (damage to a blood vessel wall) produces an enzyme cascade,
ultimately leading to a blood clot (which traps blood and effectively seals the damaged area)
• There are 2 clotting pathways (both of which are activated upon damage):– A. The extrinsic pathway (faster) – begins outside the bloodstream, in the
vessel wall• When endothelial cells or peripheral tissues are damaged, they release tissue
factor (TF or Factor III) – B. The intrinsic pathway (slower, but more fibrin is produced) – begins inside
the bloodstream, with the activation of circulating proenzymes• Proenzymes (usually Factor XII) are activated when they contact the exposed
collagen fibers at the site of damage• This pathway is assisted by the release of platelet factor (PF-3) from platelets
• Both the extrinsic and intrinsic pathways → activation of Factor X, which = the 1st step of the common pathway, ultimately leading to: – Fibrinogen (soluble) → fibrin (an insoluble web) → a clot
The coagulation phase starts ~ 30 seconds after the damage; hemostasis usually occurs within a few minutes if the damage is not too severe

Fig. 19-12, p. 663
3. The coagulation
phase (blood
clotting)

More on blood clotting• Control
– Thrombin from the common pathway re-stimulates both the extrinsic (via TF) and intrinsic (via PF-3) pathways• This is the 2nd positive feedback loop
– However, to keep clot formation from getting out of hand, at least 7 blood agents (enzymes, cofactors, and other chemicals) inhibit the process• E.g. anticoagulant enzymes, heparin, prostacyclin, etc.
• Ca2+ and vitamin K are required for proper clotting– All three pathways require Ca2+
– Vitamin K is required for the synthesis of clotting factors by the liver
• Clot retraction and fibrinolysis– After coagulation, the platelets contract → clot retraction– As healing occurs, the clot is eventually dissolved (=
fibrinolysis) by the enzyme plasmin (which is activated by plasminogen)