Female Reproduction Pathology Review
Transcript of Female Reproduction Pathology Review
-
8/11/2019 Female Reproduction Pathology Review
1/23
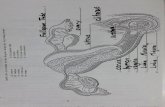
Pathology of uterine corpus:
Endometrium
mucosal lining of uterine cavity
hormonally sensitive
Estrogen --> proliferation
progesterone --> preparation for implantation (secretory phase)
loss of progesterone --> menses
Myometrium
s mooth mus cle
proliferative secretory
http://missingli nk.ucsf.edu/lm/IDS_107_Cervix_Ovary_Uterus/homepage.htm
Asherman syndrome:
secondary amenorrhea due toloss of basalis+ scarring
secondary of overaggressive D+C
http://www.google.com/url?q=http%3A%2F%2Fmissinglink.ucsf.edu%2Flm%2FIDS_107_Cervix_Ovary_Uterus%2Fhomepage.htm&sa=D&sntz=1&usg=AFQjCNFEwjx64BADBatKNZGgHy1vSTJ0Dw -
8/11/2019 Female Reproduction Pathology Review
2/23
Abnormal Uterine Bleeding: Anovulatory cycle
polymenorrhea: bleeding occurs in intervals 7 days)/ excess ive (>80mL) bleeding - at regular intervasoligomenorrhea:> 35 day cycleMetorrhagia: frequent / irregular intervalsMenometrorrhagia:prolonged/excess ive, frequent, irregulardysfunctional uterine bleeding:anovulatory vs ovulatory
excessive / prolonged estrogen stimulation WITHOUT counteractive effect of progestational phase
Estrogen -- builds up endometrium
built up endometrium (due to E) will breakdown/shed --> irregular bleeding
progesterone -- stabilize endometrium (withdrawal of progesterone --> menses)
most common in menarche + perimenopausal women
Causes:
usually subtle hormone imbalance - no obvious cause
endocrine: thyroid, adrenal, pituitary disorders
functioning ovarian tumor or polycystic ovaries
metabolic disturbance --- obesity
Histology: proliferative glands- secondary to estrogen exposure
no secretory changes
breakdown of stroma (stromal condensation) when estrogen levels diminish
estrogen withdrawal
glandular + stromal breakdown
-
8/11/2019 Female Reproduction Pathology Review
3/23
Changes induced by exogenous progesterone
seen in women on OCP + in women attempting to control bleeding
undeveloped glands with stromal cells showing enlargement + abundant
eosinophilic cytoplasm (Decidualized stroma)
enlarged stromal cells with more abundant pink cytoplasm (Decidualized)
with inactive glands
Chronic endometritis:
may cause pelvic pain, infertility, bleeding May be due to:
retained products of conception retained IUDs previous instrumentation chronic PID often cause unknown
Histology **plasma cells**
Rx:AB
Endometrial polyps:
-
8/11/2019 Female Reproduction Pathology Review
4/23
proliferation of endometrial glands + stroma benign -- may contain hyperplasia or carcinoma
increased in patients taking tamoxifen tomaxifen:
antiestrogenic effect on the breast but a weak pro-estrogenic effect on theendometrium
Endometriosis
https://secure.health.utas.edu.au/intranet/cds/pathprac/Files/Cases/Female/Case58/Case58.htm
presence of endometrial glands or stroma in abnormal extra-uterine locations reproductive age F (10%) symptoms:
inferti lity - 30-40% scarring increases risk of ectopic (fallopian tube mucosa)
dysmenorrhea (painful menstruation) cycles with the normal endometrium
Pain: pelvic pain: uterine ligament pain w/ urination: bladder wall
pain w/ defecation: pouch of douglas Sites of involvement:
ovaries, uterine ligaments, rectovaginal septum, cul de sac, pelvic peritoneum, GI, cervix,vagina. fallopian tubes , laparotomy scars
https://www.google.com/url?q=https%3A%2F%2Fsecure.health.utas.edu.au%2Fintranet%2Fcds%2Fpathprac%2FFiles%2FCases%2FFemale%2FCase58%2FCase58.htm&sa=D&sntz=1&usg=AFQjCNF5GxVef4SpooYtuMJJH_v5vfBGcQ -
8/11/2019 Female Reproduction Pathology Review
5/23
Theories for development: Metastatic theory:
retrograde menstruation through the fallopian tubes arises directly from the coelomic epithelium
mesothelium of pelvis or abdomen
Gross: white, tan nodule in
cul-de-sac,rectovaginal space,peritoneum
ovary bleeding =chocolate cyst
Complications: scarring --> infertility malignancy can develop
ovary and gynecologic tract rare cases in the intestine
Adenomyosis:
endometrial glands and stroma in the myometrium 20% of uteri removed symptom = pelvic pain
-
8/11/2019 Female Reproduction Pathology Review
6/23
Endometrial carcinoma most common invasive cancer of the female genital tract in US post-menopausal (55-65)
presents as post-menopausal bleeding(must do an endometrial biopsy) endometrial biopsy & curettage
two types type I: hyperplasia type II: sporadic pathway
preneoplastic / neoplastic lesions precurs or
s imple hyperplas ia complex hyperplasia simple atypical hyperplasia (rare) complex atypical hyperplasia alternative endometrial intraepithelial neoplasia (EIN) for precursor lesions
Endometrial carcinoma type I/II carcinoma
Type 1 -75% type 2
increase in the gland: stroma ratio associated with prolonged estrogen
stimulation of the endometrium obesity late menopause polycytic ovarian disease functioning ovarian tumors prolonged estrogen administration
Genetic alterations: inactivation of the PTEN (TSG)
Histologic types: serous:
high cytologic atypia/ mitosis/papillary
clear cells
carcinosarcoma (malignant mixedmullerian tumor - MMMT)
-
8/11/2019 Female Reproduction Pathology Review
7/23
http://ww w .w ebpathology.com/image.asp?n=15&Case=569
combined sarcoma carti lage / bone/
rhabdomyoblasts + carcinoma (metaplastic) aggressive 5yr 25-30% survival F > 60
high grade generally > aggressive than type 1
55-65 65-75
unopposed es trogenobesityHTNDM
atrophythin
endometriod morphology serous , clear cell, carcinosarcoma, MMMT
hyperplas ia endometrial intraepithelial carcinoma (rare)
PTEN, PIK3CA, KRAS, MSI, B-catenin P53, aneuploidy, PIK3CA
less aggress ive -- spread via lymphatics aggress ive -- intraperitoneal / lymphatic spread
incidence = 85% incidence = 15%
Histologic grade: grade 1: well differentiated (< 5% solid) grade 2: moderately differentiated (5-50% solid) grade 3: poorly differentiated (>50% solid)
Prognosis: most are stage 1 (confined to the uterus) > 90% survival grade III - stage I ~75% 5yr survival
survival drops to 50% for stage II/III
Mesenchymal tumors- uterus
http://www.google.com/url?q=http%3A%2F%2Fwww.webpathology.com%2Fimage.asp%3Fn%3D15%26Case%3D569&sa=D&sntz=1&usg=AFQjCNFrMJ1I0XGz2aOSoGDJ5LWM6o1GVghttp://www.google.com/url?q=http%3A%2F%2Fwww.webpathology.com%2Fimage.asp%3Fn%3D15%26Case%3D569&sa=D&sntz=1&usg=AFQjCNFrMJ1I0XGz2aOSoGDJ5LWM6o1GVg -
8/11/2019 Female Reproduction Pathology Review
8/23
smooth muscle tumor endometrial stromal tumor
leiomyoma leiomyosarcoma
endometrial stromal nodule endometrial stromal sarcoma
Leiomyoma - fibroid
very common (increased incidence in AA) 75% are reproductive age F
Symptoms: abnormal bleeding / urinary fq fq cause of spontaneous abortion + infertility Malignant change = very rare
not regarded as a precursor to leiomyosarcoma Rx:
myomectomy hysterectomy uterine artery embolization GnRH agonists: continuous stimulation = inhibitory --> hypoestrogen state
used to shrink fibroid prior to Sx Pathology
well circumscribed, white, tan, firm mass size: range - microscopic --> 20 cm often multiple enlarged during pregnancy / shrink post menopause (E sensitive)
-
8/11/2019 Female Reproduction Pathology Review
9/23
location: intram ural submucosal subserosal +/- broad ligamanet / cervix
Histology: smooth muscle cells no significant cytologic atypia - few/no mitoses
leiomyosarcoma:
malignant smooth muscle tumor peak incidence 40-60 aggressive malignancy with frequent lung mets gross:
bulky, fleshy mass, not well circumscribed, hemorrhage Histologic criteria:
mitotic activity cytology (nuclear) atypia necrosis/hemorrhage
Gestational + Placental disorders spontaneous abortions
ectopic pregnancy abnormalities in placental implantation placent previa placental accreta/incretia/percretia
placental infections pre-eclampsia / eclampsia gestational trophoblastic disease
Ectopic Pregnancy:
-
8/11/2019 Female Reproduction Pathology Review
10/23
implantation of the products of gestation in any site outside the normal intrauterine location occurrence:
1/150 pregnancies symptoms
severe abdominal pain about 6 wks after last menstrual period Predisposing conditions:
prior peritubal scarring(chronic salpingitis) adhesions (appendicitis, endometriosis, prior surgery) location
fallopian tube (90%) abdominal cavity, intrauterine portion of the fallopian tube, ovary (rare)
histologic: chorionic villi + trophoblastic cells
may see only trophoblastic cells only
abnormalities in placental implantation:
-
8/11/2019 Female Reproduction Pathology Review
11/23
Placental previa Placenta Accreta placenta increta
placental implants in the lower uterinesegment or cervix and may result inbleeding
3rd tr imester painlessbleeding often requires C-section
partial or completeabsence of deciduawith adherence of the placental villoustissue directly to the myometrium
failure of the placenta to separate fromthe myometrium is a cause ofpostpartum bleeding (life-threatening)
often rq hysterectomy
placenta dissectingthrough themyometrium
Placental infections:
bacterial: acute chorioamnionitis + acute villitis opaque membrane (normal = translucent) acute inflammation in the chorionic membrane extending --> amnion
TORCH + syphilis + TB + rubella + CMV + HSV --> chronic villitis
-
8/11/2019 Female Reproduction Pathology Review
12/23
Gestational trophoblastic disease:tumor/ tumor-like conditions characterized by a proliferation of placental tissue
hydatiform mole: complete/ partial / invasive choriocarcinoma placental site trophoblastic tumor
Hydatidiform Molar Pregnancies
US incidence is 1 / 1000 2000 pregnancies. 7-10 times higher in Asia than in North America and Europe.
Patients with > four pregnancies and increased number of abortions are at high risk >50% are complete moles. 25-43% partial moles.
complete partial
genetics empty ovum + 2 sperm (46) normal ovum + 2 sperm (69)
fetal tissue none present
villous edema most some
trophoblastic proliferation diffuse, circumfrentialproliferation around hydrophic
villi
focal proliferation aroundhydrophic villi
choriocarcinoma risk 2-3% minimal
Clinical symptoms: Uterus larger than expected for date of gestation
-
8/11/2019 Female Reproduction Pathology Review
13/23
passage of grape-like masses High HCG level that expected for date of gestation Often diagnosed in the first trimester today
Fetal heart sounds absent Snow storm appearance on ultrasound
Complete Mole
Histologic Features
Enlarged and dilated villi with central cistern formation (cavitations) Circumferential trophoblastic proliferation
atypia Early complete mole can be a diagnostic challenge as the proliferation is not as well
developed
Partial mole
karyotype: triploid 69, XXY or tetraploid 92, XXXY +/- fetal parts some vi ll i are edematous trophoblastic proliferation - not as marked as that of a complete mole
Rx: D&C + BHCG monitoring
Px: molar pregnancies have ~10% chance of persis tent moles/invasive mole complete molar pregnancies have 2.5% risk of subsequent choriocarcinoma ***note:
choriocarcinomas arising from gestational pathway - respond to chemo ones that arise from germ cell pathway do not!
partial moles increased risk of persistent molar disease/minimal risk of subsequent choriocarcinoma
-
8/11/2019 Female Reproduction Pathology Review
14/23
post ovulation: corpus luteum secretes progesterone --> prepares endometrium for possible implantation(secretory phase)
PCOS: (Stein-leventhal syndrome)
-
8/11/2019 Female Reproduction Pathology Review
15/23
3-6% reproductive aged F obese young inferti le oligomenorrhea hirsutism +/- DM (insulin R)
numerous cystic foll icles oligomenorrhea persistent anovulation, hirsutism, obseity
Pathophys: unclear increased secretion of LH --> excessive androgen production (theca cells) --(Aromatase)->
estrone estrone negative feedback on FSH --> cystic degeneration of follicles high estrone levels --> risk of endometrial carcinoma
LH:FSH > 2
Ovarian cancer:
3% of all cancers US- F 1/70 american women lifetime incidence
risk increases with age 3/100,000 F
-
8/11/2019 Female Reproduction Pathology Review
16/23
pariety + OCP = protective more deaths than cervical/endometrial cancer clinical:
abdominal distention, ascites, pan complications --> rupture / torsion urinary or GI symptoms No well-validated screening
Genetic risk factors: About 5-10% patients have a first degree relative with ovarian cancer
Compared to a 1-2% risk for the general population women who have relative with ovarian cancer have a 9.4% risk Women who inheri t the BRCA1 or BRCA2 have a 15-40% absolute risk
estimated risk by age 70 -- 20-60% BRCA still explain < 1/3 familial ovarian cancers Usually serous carcinoma and display p53 dysregulation.
Histologic classification of primary ovarian surface epithelial tumors / site of origin serous: fallopian tube / surface epithelial lining
cystadenoma/adenofibroma 70% borderline 10% CA 20-25%
endometrioid: endometriosis
clear cell:endometriosis mucinous:unclear primary
About 10-15% of ovarian tumors; May be combined with other types tumors (serous tumor), teratoma, sex cord stromal tumors. Mean age 51-54
transitional (Urothelial)- poss ible walthard nests
benign - cystadenoma
single cyst w/ simpleflat lining (30-40)
borderline: low malignant potential,atypical proliferating*proliferation - no stromal invasion*
malignant:stromal invasion
serous - 70% Serous Borderline Tumor - 15%
Histology: Proliferation of epithelialcells, but no invasionSynonyms:
Serous borderline tumor (SBT) Serous tumor of low malignantpotential (SLMP)
Atypical proliferating s erous tumor(APST)
low metastatic potential ifconfined to the ovary, may progressover many years
Serous Carcinoma: 5%40-50% of all ovarian malignanciesMean age 56 (45-65)67% BilateralStage distribution:
I: 14% confined to the ovary II: 7% confined to the pelvis III: 63% in the peri toneum
IV: 16% distant metastasis
Size-microscopic to over 20 cmSolid and cystic confluent areas
BRCA1: increased risk serouscarcinoma ovary/fallopian tube
Microscopic
-
8/11/2019 Female Reproduction Pathology Review
17/23
Destructive stromal invasion
Mucinouscystadenoma 80%
benign: 2-5% bilatlargest ovarian tumorsmulti/uni-cystic
single layer ofcolumnar cells w/ lotsof intracellular mucin(endocervical or GI)
Mucinous borderline 15% increases epithel ial
proliferation w/o destructivestromal invasion
Mucinous Carcinoma 5-10%
5% present stage II+ 5% bilateral gross:large tumors
(15-30cm), multiloculatedcysts w/ mucin
hemorrhage, necrosis, solid+/- papillary areas
http://www.webpathology.com/image.asp?n=14&Case=526
Ovary: Endometrioid Carcinoma
Often (15%-20% of cases) co-exist with endometriosis. Frequent mutations in thePTEN tumor suppressor geneand in the KRAS and -catenin
oncogenes. 40% are bilateral. About 15%-30% are accompanied by a synchronous carcinoma in the endometrium
Microscopic: Resemble endometrioid carcinoma of the uterine corpus
glands and nests of cells invading the ovarian stroma Grade identical to endometrial carcinoma May find adjacent endometriosis
Clear Cell Tumors of the Ovary
http://www.google.com/url?q=http%3A%2F%2Fwww.webpathology.com%2Fimage.asp%3Fn%3D14%26Case%3D526&sa=D&sntz=1&usg=AFQjCNERKdkOapH2WHfYCWxr8kQt4k2ZHQ -
8/11/2019 Female Reproduction Pathology Review
18/23
Benign and borderline variants are rare, most are carcinomas Similar histology to clear cell carcinomas of the endometrium
clear cytoplasm Frequently arise in endometriosis Frequently admixed with endometrioid carcinomas
Transitional Cell Tumors
Epithelial elements histologically resembling urothelium May arise from benign Walthards Nests
Vast Majority are benign Brenner tumor uncommon borderline and malignant Brenner tumors
Benign Brenner Tumor
Common incidental finding (microscopic size to several cm) about 4-5% of all benign ovariantumors.
7-8% Bilateral Microscopically:
Mature urothelial-like cells arranged in solid or cystic within a fibromatous stroma
-
8/11/2019 Female Reproduction Pathology Review
19/23
Associations : mucinous cystic tumors serous cystadenoma dermoid cys t
Metastatic Tumors to the Ovary ~5% of ovarian tumors Non-ovarian primary may present after ovarian met Metastatic mucinous carcinomas are more common than primary ovarian mucinous carcinomas Krukenburg tumor
metastatic mucin-produing signet-ring cell carcinoma typically gastric origin
Common tumors metastasizing --> ovary GYN tract: Tube, endometrium, cervix.
GI tract: Colon, appendix, stomach, pancreas, hepatobill iary tree.
Breast.
Lung. Melanom a.
GU tract: Bladder and kidney. Sarcoma.
Pseudomyxoma Peritonei
Clinical term indicating the presence of mucinous material in the peritoneum (jelly belly)surrounded by fibrous tissue.
almost all are metastatic tumors rather than primary tumors (GI tract, appendix) Generally regarded as malignant, but may have a protracted clinical course.
-
8/11/2019 Female Reproduction Pathology Review
20/23
Germ Cell Tumors
Teratoma, seminoma, yolk sac, choriocarcinoma, embryonal, mixed type
mature cystic teratomas:
46 xx -- usually reproductive years (but seen all ages 2-80) 27-40% of all ovarian tumors
58% of all benign tumors (almost all benign) mos t form a mas s
Variety of cells from all three germ cell layers: endoderm, mesoderm, ectoderm. Skin and sebaceous glands, hair shafts, bone, cartilage, gastrointestinal epithelium,
bronchial epithelium , thyroid, neural tiss ue.
Skin only dermoid cyst Monodermal teratoma-composed of only one cell type such as thyroid
Teratoma with Secondary Malignant Transformation ~1.5%. usually post-menopausal women,
Squamous cell carcinoma, melanoma, thyroid, adenocarcinoma, carcinoid, skin adnexaltumors, basal cell carcinoma, thyroid carcinoma, chondrosarcoma, etc
Immature Teratoma contains a variable amount of immature, embryonal-type (generally immature neuroectodermal) tissue.
1-2 weeks of gestation-germ cell tumor. 2-8 weeks embryonal. >8 weeks fetal .
Generally seen in patients less than 40, peak incidence of 14-19 years. Raised HCG and AFP levels. Treatm ent
Rapidly growing tumor - graded by amount of immature elements grade I, stage I surgery. > stage I , or higher histologic grade or very large tumors are given chemotherapy
-
8/11/2019 Female Reproduction Pathology Review
21/23
Mature cystic teratoma- majority and are benign young adult to middle age Multiple different types of cells.
Malignancy Malignant transformation older patients, rare. Immature teratoma younger patients, immature neuroepithelium.
Dysgerminoma
primitive germ cell tumor. +/- elevated Serum LDH His tology:
Proliferation of primitive germ cells large cells w/ clear cytoplasm and central nuclei Lymphocytes and macrophages. Identical to a testicular seminoma.
Respond to chemotherapy and radiation therapy. Stage - significant factor.
yolk sac
#2 malignant tumor of germ cell origin Derived from differentiation of malignant germ cells along the extra-embryonic yolk sac lineage. rich in -fetoprotein. Characteristic feature
glomeruloid-like structure composed of central blood vessel enveloped by germ cells within aspace lined by germ cells (Schiller-Duval body).
Identical morphology to testicular counterpart.
choriocarcinomaNon-gestational
Trophoblastic differentiation within a germ cell tumor. Strict definition of combination of cytotrophoblast and syncytiotrophoblasts (NO villi)
Secrete -HCG
-
8/11/2019 Female Reproduction Pathology Review
22/23
Less favorable outcome than gestational choriocarcinoma- which is chemo sensitive. Rx: Cytoreductive surgery followed by chemotherapy.
embryonal
Least differentiated form with large, highly atypical cells Highly malignant aggressive malignancy
Treated with chemotherapy
Sex cord stromal tumors
granulosa cell tumor
call-exner bodies
Adult Granulosa Cell Tumors >95% of granulosa cell tumors Middle aged to postmenopausal women Average size 12.5 cm - Commonly encapsulated.
Sectioned surface is yellow to tan withvarious amounts of solid and cysticareas.
Hemorrhage is common
Generally regarded as malignant but low risk formetastasis May show metastasis years after
diagnosis 10-year survival is about 85% may have late > 10 year recurrences and
metastasis
Histopathology Small round cells with scant cytoplasm, and
round to oval nucleus (coffee bean) withlongitudinal grooves.
Variety of patterns microfoll icular insular, moire silk (water silk),
trabecular, diffuse. Call-Exner body gland-like structure filled with
eosinophilic material. Mitotic rate rarely exceeds 1-2 per 10 hpf.
Call-Exner bodies and grooved, coffee bean nuclei Secrete estrogen-may be associated with
endometrial hyperplasia. Inhibin product of granulosa cells.
-
8/11/2019 Female Reproduction Pathology Review
23/23
Juvenile type granulosa cell tumor 5% of all granulosa cell tumors Firs t 30 yrs Almost always stage I
Less than 5% bi lateral 2% have extraovarian spread. Vast majority are benign.
Associated with precocious puberty.
fibromas, trhecoma, fibrothecoma Composed of plump spindle cells (fibroma) withlipid droplets cells within the cells (thecoma).
Unilateral: 90%. Hormonally inactive Gros sly:
White tan mass. His tology:
Well-differentiated fibroblasts withinterspersed collagen.
Thecoma-fibroma group Generally have a favorable prognosis Association with Meigs syndrome
Ovarian tumor Hydrothorax right side. Ascites
sertoli-leydig cell tumorandroblastoma
Composed of Sertoli cells tubules that resemble testisLeydig cells and primitive gonadal stroma
May see Reinke crystals