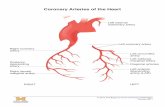
Coronary artery disease & its prevention
-
Upload
ashraf-uddin-chowdhury -
Category
Health & Medicine
-
view
884 -
download
1
Transcript of Coronary artery disease & its prevention

CORONARY ARTERY DISEASE&
ITS PREVENTION
DR MD ASHRAF UDDIN CHOWDHURY
FCPS (MEDCINE), MD (CARDIOLOGY)
CENTRAL POLICE HOSPITAL
DHAKA

CORONARY ARTERY DISEASE
Coronary artery disease is the most common
form of heart disease in all over the world.
A narrowing of the coronary arteries prevents
adequate blood supply to the heart muscle in
this condition.
Usually caused by atherosclerosis, it may
progress to the point where the heart muscle is
damaged due to lack of blood supply.
Such damage may result in infarction,
arrhythmias, and heart failure.

CORONARY ARTERY DISEASE IS ALSO KNOWN AS;
ATHEROSCLEROTIC CARDIOVASCULAR DISEASE (ASCVD)
CORONARY ATHEROSCLEROSIS
CORONARY HEART DISEASE
ISCHAEMIC HEART DISEASE

CORONARY ATHEROSCLEROSIS
CORONARY ATHEROSCLEROSIS is theabnormal accumulation of lipid or fattysubstances or fatty atheroma (plaque) in thelumen of coronary artery

RISK FACTORS
Non Modifiable
Modifiable

MODIFIABLE
Atherogenic dyslipidaemia
Cigarette smoking, tobacco use
Hypertension
Diabetes mellitus
Physical inactivity or sedentary lifestyle
Obesity

NON MODIFIABLE
Family history of premature CAD in first degree relatives.
Increasing age
Gender(male)
Race(non white populations)

Emerging risk factors:
Metabolic syndrome High Triglyceride Apo Lipoprotein B Dietary trans fat intake Poor oral health Fibrinogen Homocysteine Urine microalbuminuria/creatinine
ratio (CKD) High sensitivity CRP Impaired fasting glucose

Synergy of risk factors:
The CAD death risk in men who smoke, have DBP>90 mm Hg, TC>250 mg/dl, the actual risk is more than all the three risk factors are added
Thus there is multiplicative effect of multiple risk factors acting in concert.
Also control of one risk factor provides substantial benefit in persons with multiple risk factors

PATHOPHYSIOLOGY
Normal arterial wall has three layers:
Intima- limited by internal elastic lamina
Media- between internal and external elastic lamina
Adventitia
Intima is the site at which the atherosclerotic lesions form

PATHOPHYSIOLOGY
?? ETIOLOGICAL FACTORS
INJURY TO THE ENDOTHELIAL CELL LINING THE ARTERY
INFLAMMATION AND IMMUNE REACTIONS
LDL OXIDATION: ACTS AS FREE RADICALS AND INITIATES INFLAMMATORY PROCESS
OXIDIZED LDL ENTERS THE ARTERY INTIMA & THERE IS ACCUMULATION OF LIPIDS IN THE INTIMA OF ARTERIAL
WALL


T LYMPHOCYTES AND MONOCYTES THAT BECOMES AS MACROPHAGES INFILTRATE THE AREA TO INGEST THE LIPIDS AND BECOME FOAM CELL
PROLIFERATION OF SMOOTH MUSCLE CELLS WITH IN THE VESSEL
FORMATION OF FIBROUS CAP OVER FATTY CORE (ATHEROMA)
PROTRUSION OF ATHEROMA IN TO THE LUMEN OF VESSEL

NARROWING AND OBSTRUCTION
IF CAP IS THIN THE LIPID CORE MAY GROW CAUSING IT TO RUPTURE
HEMORRHAGE INTO PLAQUE ALLOWING THROMBUS TO DEVOLOP
THROMBUS OBSTRUCT THE BLOOD FLOW LEADING TO SUDDEN CARDIAC DEATH OR MYOCARDIAL INFARCTION
ANGINA AND OTHER SYMPTOMS


The process of atherosclerosis begins in childhood and has clinical manifestations in late adulthood
The process develops over years to decades and progression is not linear and smooth but discontinuous with periods of quiescence and rapid evolution.


IHD – Clinical Spectrum
Chronic
Stable Angina
Silent Ischemia
Mixed Angina
Microvascular Angina (Syndrome X)
Stunned & Hibernating
Acute
Unstable Angina
Acute Myocardial Infarction (NSTEMI, STEMI)
Sudden Cardiac Death
Prinzmetal Angina
18

ANGINA PECTORIS
Angina pectoris is a clinical syndrome usually characterized by central chest pain, discomfort or breathlessness that is precipitated by exertion or any stress and promptly relieved by rest or nitrate.
It may occur when there is imbalance between myocardial oxygen supply and demand.
Coronary atheroma is the commonest cause of angina.

Variant angina
Also called prinzmetal angina.
Pain at rest with reversible ST segment elevation thought to be caused by coronary artery vasospasm

21
Prolonged bouts of chest pain at rest with EKG ST seg. elevation.
PRINZMETAL OR VARIANT ANGINA
A = Marked transitory ST Elevation during a bout of severechest pain
B = Thirty min. after A (Normal EKG)
Pathophysiology: profound spasm of one of
the three major epicardial coronary arteries.

Microvascular angina
Also known as syndrome X
Patient have chest pain with ECG change
In this condition stress test (ETT) is positive
But does not have any blockage in epicardialcoronary artery in angiogram.
The pain is due to blockage or spasm in cardiac microvasculature.

23
Pathophysiology: Dynamic small vessel constriction (vasospasm)
(positive stress testing)

Silent ischaemia
Objective evidence of ischaemia (such as electrocardiographic changes with a stress test) but patient has no symptoms
Commonly seen in diabetic patients.

Is the objective evidence-ST segment shifts- of myocardial ischemia which is not associated with angina or angina equivalents.
25
Silent Ischemia
ST seg. depression
Iceberg’s sign
Angina

ANGINA PAIN FEATURES
Squeezing burning tightening aching pain or discomfort across chest
The pain often spread to neck, jaw, arms, shoulders, throat, back or even teeth
Angina pain starts with exertion which is mostly predictable.
It is relieved with rest or after taking nitrate.


ACUTE CORONARY SYNDROME(ACS)
ACS is a term that encompasses both unstable angina and Myocardial Infarction (MI).
After rupture of an ulcerated or fissured plaque, there is a dynamic process whereby degree of obstruction may either increase leading to complete vessel occlusion and MI, or regress due to endogenous fibrinolysis.

Unstable angina
New onset or rapidly worsening angina or angina on minimal exertion or angina at rest in the absence of myocardial damage.
Also called preinfarction angina
Symptoms occur frequently and last longer than stable angina
Pain may occur at rest.
The culprit lesion is usually an ulcerated or fissured atheromatous plaque with adherent platelet rich thrombus and local coronary artery spasm.

MYOCARDIAL INFARCTION
Myocardial infarction refers to the dynamicprocess in which a region of the heartexperience a severe prolonged lack ofoxygen supply due to complete occlusion ofcoronary artery with subsequent necrosis ordeath to myocardial tissue.
The process of infarction progress overseveral hours.


Progression of coronary plaque over time Clinical Findings
32
Acute Coronary SyndromesSudden Cardiac Death
Acute silent occlusive process
Angina pectoris
Thrombogenicrisk factors
Atherogenic risk factors
Endothelial dysfunction
20 years 60 yearsAge

IS CORONARY ARTERY DISEASE PREVENTABLE?
WHAT CAN WE DO TO PREVENT CAD?

Lifestyle changes / Health behaviours
Lifestyle changes that may be useful in
coronary disease include:
•Smoking cessation
•Exercise
•Healthy diet
•Stress management
•Weight control / Obesity reduction

Control of risk factors
Control of Hypertension
Control of diabetes
Management for dyslipidaemia

Stress
Psychosocial factors associated with CAD risk:
– Type A personality
– Hostility/Anger
– Depression/Anxiety
3 to 4 times increased risk of death in first year following MI

Stress
Influence CAD risk via 2 main mechanisms:
Catacholamine release
– increased BP
– increased HR
– vasoconstriction
– increased O2 demand
Decreased adherence to lifestyle modification recommendations

Healthy Diet
Diets high in fruits, vegetables, whole grains, fish and unsaturated fatty acids have lower risk for CAD

Good and Bad CholesterolActually, some cholesterol is necessary for proper body function. But dietary saturated fat and cholesterol both raise levels of LDL "bad" cholesterol. High levels of LDL cholesterol can cause plaque to build up in arteries, leading to heart disease and stroke. HDL is a "good" cholesterol in that it helps eliminate bad cholesterol from blood. It is possible to lower LDL cholesterol and raise HDL cholesterol with diet.

Serve Up Heart-Healthy FoodWhen it comes to fruits and vegetables, pick up the pace! Multiple servings throughout the day can help lower LDL "bad" cholesterol. Moreover, these foods have antioxidantsthat can be beneficial. Also, eating more vegetables and fruits often results in eating fewer high-fat foods. This can lower blood pressure promote weight loss.

Think Fish For Heart Health
Fish is generally exceptionally heart healthy because it is high in healthy omega-3fatty acids and low in saturated fat. It is the omega-3 fatty acids that help lower blood levels of triglycerides. Especially emphasize fatty fish. Keep in mind that deep oil frying of any food diminishes the health benefits.

Start the Day With Whole Grains
Oatmeal or whole-grain cereal have fiber and complex carbohydrates that help to feel fuller for longer, so a person is less inclined to overeat later in the day. These breakfasts help reduce LDL "bad" cholesterol and can help with our weight control.

Go Nuts for Cardiovascular Health
Nuts help to lower cholesterol because they are high in monounsaturated fat. This form of fat lowers LDL "bad" cholesterol while maintaining HDL "good" cholesterol levels. This can lower the risk of heart disease. Only eat a handful, though, because nuts are high in calories, especially if they are coated in sugar or chocolate.

Unsaturated Fats Protect the HeartOur daily fat needs are only about a third of our daily calories. However, the form of fat makes a difference. Unsaturated fats (in canola, olive, and sunflower oils) lower LDL "bad" cholesterol levels. Saturated fats (in butter and palm oil) and trans fats increase LDL cholesterol. All fats have calories. Moderation is the key.

Eat More Beans, Fewer Potatoes
Carbohydrates are important for energy production. However, there are differences in the quality of carbohydrates, too. Whole grains like beans, quinoa, whole-wheat pasta, and brown rice are high in fiber that can help lower cholesterol. Whole grains also keep you feeling full longer. The carbohydrates in pastries, white rice, white bread, and potatoes boost blood sugar levels rapidly. This can lead you to feel hungry sooner, potentially leading to overeating.

Obesity Body Mass Index (BMI)
Measured in weight in Kg /height in m2
BMI Targets
Underweight <18.5
Normal 18.5-24.9
Overweight 25.0-29.9
Obese >30
Definition of central obesity in South asians :– Waist circumference of Men >90cm or 36 inches,
Women >80cm or 32 inches

Sedentary Lifestyle & Exercise
Regular exercise- at least 30 minutes , 3 or 4 times a week.
Physical activity reduces the risk of CAD through:
Improved balance between myocardial O2 supply and demand
Decreased platelet aggregation
Decreased susceptibility to malignant ventricular arrhythmias
Improved endothelial tone
Beneficial effect on other CAD risk factors (ie. diabetes, dyslipidaemia, hypertension, obesity, stress)

Blood pressure target
Normal <120 / 80
Prehypertensive (120/80 to 139/89 mm Hg)
Stage 1 (140/90 to 159/99 mm Hg)
Stage 2 (≥160/100 mm Hg)
*JNC 7

Lipid Targets for CAD
Primary Targets for very high risk patients*:
LDL-C < 1.8mmol/L (70 mg/dl) or <50% reduction
(< 100mg/dl in moderate risk patients)
Non HDL-C ≤ 2.6 mmol/L (100 mg/dl)
(< 130mg/dl in moderate risk patients)
Alternate: Apolipoprotein B < 0.80 g/L
Can J Cardiol 29 (2013) 151–167.*National lipid association Annual summary 2015
*ESC guideline 2015

Lipid Targets for CAD
Secondary Targets: (once LDL cholesterol is at goal)
Total Cholesterol to High Density Lipoprotein (HDL) cholesterol ratio less than 4.0
Non HDL cholesterol < 3.5 mmol/L
Triglycerides < 1.7 mmol/L (150 mg/dl)
Apolipoprotein B to apolipoprotein AI ratio < 0.8
High-sensitivity C-reactive protein (CPR) < 2 mg/L
Can J Cardiol 2009; 25(10): 567-579.

Diabetes
People with diabetes have 2 to 7 times increased risk of developing CAD than people without diabetes
Mechanism of atherosclerosis is unclear
Endothelial damage
Increased platelet aggregation
Insulin promotes synthesis of lipids and uptake of lipids by smooth muscle
Excess sugar in vessels damages the endothelial lining making it vulnerable to plaques and clots

Diabetes
Careful control of blood sugar levels reduces the risk of developing the complications of diabetes
Targets for diabetic control-as near normal as possible
Canadian guideline:
FBG 4-7 mmol/L
2 hr pc BS 5-11 mmol/L
HbA1C <7

Emerging Risk Factors
Nontraditional factors that are associated with increased risk of CAD, but a causal link has not yet been proved with certainty
– Poor oral health
– Dietary trans fat intake
– Homocysteine
– Lipoprotein A
– Infectious agents
– Adhesion molecules
– Cytokines
– Fibrinogen
– High sensitive C-reactive protein

Lifestyle interventions to reduce TC & LDL-C levels
Reduce dietary saturated fat
Reduce dietary trans fat
Reduce dietary cholesterol
Increase dietary fibres
Utilize functional foods enriched with phytosterols
•Reduce excessive body weight •Increase physical activity•Utilize Soy protein products
**ESC guideline on dyslipidaemia 2015

Drugs to lower LDL
Statins – atorvastatin, rosuvastatin, simvastatin,
Ezetimibe
Investigational agent- evolocumab & alirocumab (PCSK9 inhibitors)- >50% reduction in LDL-c and nonHDL-c levels

Lifestyle interventions to reduce TG levels
Reduce excessive body weight
Reduce alcohol intake
Reduce intake of mono and disaccharides
Reduce total amount of dietary carbohydrate
Increase habitual physical activity
Utilize supplements of n-3 polyunsaturated fat
Replace saturated fat with mono or poly unsaturated fat.
**ESC guideline on dyslipidaemia 2015

Drugs to lower Tg
Fenofibrate
Gemfibrozil, colestipol, cholestyramine etc

Lifestyle interventions to increase HDL-C levels
Reduce dietary trans fat
Increase habitual physical activity
Reduce excessive body weight
Reduce dietary carbohydrate and replace them with unsaturated fat.
Use alcohol with moderation
Prefer carbohydrate with low glycaemic index and high fibre content
Quit smoking
Reduce intake of mono and disaccharides**ESC guideline on dyslipidaemia 2015

Drugs to raise HDL-c
Currently none in clinical use.
Investigational agent- anacetrapib, evacetrapib, - 150% increase in HDL-c.

SUMMARY
Control of -
Dyslipidaemia, Hypertension & DM
Healthy behaviours-
Smoking cessation
Weight control
Exercise
Healthy diet
Stress free life

Important Trials that showed role of statins in CAD AVERT(atorvastatin versus revascularization treatment)-
incidence of ischaemic evects was 36% lower in atorvastatingroup compared with revascularization group(PTCA)
ASTEROID (a study to evaluate effects of rosuvastatin on intravascular ultrasound derived coronary atheroma burden)–9.1% reduction in atheroma volume in heavy plaque burden area of coronary artery.
JUPITER (Justification for the use of statins in primary prevention: an intervention trial evaluating rosuvastatin)– this trial was stopped prematurely as it was seen unequivocally rosuvastatin reduces morbidity and mortality than placebo in primary prevention.
SATURN- study of coronary atheroma by intravascular ultrasound: effects of rosuvastatin versus atorvastatin. Both were effective in reducing coronary atheroma.

Thank you all !!

This presentation was prepared for a group of physicians working in various disciplines in a large generalhospital. Very often they ask me whether he or she have CAD and what they should do to avert this deadly disease. Here I have discussed how to diagnose coronary artery disease clinically, its pathophysiology in short and how to prevent it (primary prevention). Investigations and management was not discussed in this presentation. If anyone find this presentation helpful, I shall be very happy. I convey my thanks to people who made some of these slides, pictures and also thanks in advance to those who intend to use these.Thanking you,Dr md ashraf uddin chowdhuryFCPS, MD (Cardiology)Clinical and interventional cardiologist. [email protected]