Blind esophagus and esophagotracheal fistula€¦ · 1.Jejunoileal atresia 2.Meconium ileus...
Transcript of Blind esophagus and esophagotracheal fistula€¦ · 1.Jejunoileal atresia 2.Meconium ileus...

Pediatric radiology
Endre Szabó

A child is not a small adult!

• Water content of a baby’s body is higher than that of an adult, there are more free radicals and bigger damage due to radiation!
• Baby’s chest film means almost full body irradiation with higher genetic effect for the gonads and higher somatic effect for the eye, thyroid gland and bone marrow!
• There is more red marrow in a baby – thus bigger danger of leukemia!

ALARA – As Low As Resonably Achievable
• Our aim is to minimize risk and maximize diagnostic benefit from any imaging examination - to obtain the required diagnostic information using the minimum radiation dosage.
• This approach is especially valid in pediatric radiology: any radiation is harmful to the child!

The benefits of each examination must be carefully balanced
against any potential risk!

• 1. Indication of X-ray, CT examinations must be well established.
• 2. Examinations based on non-ionising radiation should be used whenever possible: US, MRI
Reduction of radiation dosage

Reduction of radiation dosage
3. Radiation protection: gonads must be shielded

Reduction of radiation dosage
4. Immobilisation: proper immobilisation techniques improve image quality, decrease the length of the examination, and decrease the need for repeat studies.

Intrauterine circulation

Intrauterin keringés

Neonatal Chest Diffuse Pulmonary Disease Causing Respiratory Distress
• Respiratory distress in the newborn is most commonly related to diffuse pulmonary disease
1. Small babies with decreased lung volumes – on chest X-ray film granular opacities – Surfactant deficient disease – Beta-hemolytic Streptococcal pneumonia
2. Large babies with increased lung volumes – streaky perihilar opacities on the X-ray film
-Meconium aspiration syndrome -Other neonatal pneumonias -Transient tachypnoe of the newborn

Diffuse Pulmonary Disease Causing Respiratory Distress Small babies with decreased lung volumes - RDS
Surfactant deficient disease / RDS / Hyalin membrane disease
Pathology: disease of premature infants less than
36 weeks- due to deficiency of surfactant of the lungs - the alveoli collapse and prevent gas exchange
Radiography: – Low lung volumes secondary to micro-
collapse – Diffuse granular opacities represent
collapsed alveoli interspersed with open alveoli.
– Air bronchograms demonstrate patent bronchi in abnormal lung

Diffuse Pulmonary Disease Causing Respiratory Distress Large babies with increased lung volumes – streaky perihilar opacities
on the X-ray film
Meconium aspiration syndrome • Postmature infants and infants with inrauterine stress
• Intrapartum or intrauterine aspiration of meconium
• Meconium is the tenacious, thick viscous material in the neonatal bowel
• When the fetus is hypoxic, there is passage of meconium into the amniotic fluid which can enter to the lung
• Aspirated meconium has three effects: – Airway obstruction due to tenacious meconium
– Surfactant dysfunction
– Chemical pneumonitis

Meconium aspiration sy. • Rad. signs:
– High lung volumes • diaphragm is lower than normal due
to airways obstruction
– Areas of asymmetric patchy hyperinflation and atelectasis
• extensive patchy reticulo-granular shadowing throughout both lung fields
– Rope-like perihilar densities • aspirated meconium in the airways
• Complication: • Difficulty ventilating with air block • Severe pulmonary hypertension • Anoxic brain injury • Chronic lung disease
• Therapy: – mechanical ventillation
• Conventional or high frequency ventilation

Complications of the mechanical ventillation
• Arises from barotrauma and high oxygen pressures
• Barotrauma results in increased alveolar pressure and alveolar rupture – Air leak – Pulmonary interstitial emphysema (PIE) – Pneumothorax, pneumomediastinum, pneumopericardium, pneumoperitoneum
– Pulmonary hemorrhage – Bronchopulmonary dysplasia

Air leak - Pulmonary interstitial emphysema
• Radiographic signs: multiple small
radiolucencies scattered throughout the affected lung- gas bubbles in the parenchyma
• increased volume of affected lung
• mediastinal shift towards the contralateral side

Pneumothorax - Pneumomediastinum - Pneumopericardium
Clinical sign: sudden deterioration in the clinical state of the baby and increased respiratory distress
Radiographic sign: detection of the lung edge and contralateral mediastinal shift
Pneumothorax Pneumopericardium Pneumomediastinum

Bronchopulmonary dysplasia Chronic lung disease of infancy
• Path.: fibrotic process in the lung interstitial tissues due to barotrauma and high oxygen pressure
• Rad. signs: – heterogeneous appearance with
focal lucencies separated by coarse reticular and band-like opacities of fibrosis
– More opacities in the upper lobes with hyperinflation at the bases
• The surviving infants may subsequently develop normal radiographs in childhood!

Congenital heart disease
• Imaging modalities: 1. Echocardiography: prenatal!

Congenital heart disease
• Imaging modalities: – MRI
– Angiocardiography
– Radiography: A major role of chest radiograph is access pulmonary vascularity.

Increased pulmonary blood flow Left to right shunt
• ASD • VSD • Persisting truncus arteriosus • Transposition of great vessels

Decreased pulmonary blood flow
• Tetralogy of Fallot • Pulmonary stenosis • Pulmonary atresia • Tricuspidal atresia • Ebstein anomaly

Decreased pulmonary blood flow Tetralogy of Fallot
• Radiographic signs:
• oligaemia of the lungs
• „boot-shaped heart” elevated cardiac apex
• (PS, VSD, dextroposition of the Ao, RV hypertrophy)

Esophageal atresia – Esophagotracheal fistula
• Path: •esophagus ends as a blind pouch •abnormal connection between tracheal and esophageal lumen
• Clinical signs: aspiration into the lungs

Esophageal atresia –Esophagotracheal fistula
•air in the bowel if a fistula is present •soft tube into the esophagus and the tube curves in the blindly ending pouch

Esophageal atresia without tracheoesophageal fistula
air-less scaphoid abdomen

Congenital and developmental anomalies of the small bowel
• May be associated with olygohydramnion
• Frequently present postnatally in the first 24 hours
• Clinical evidence of obstruction: bilious vomiting and abdominal distension
• Common clinical signs: – usually normal birth weight neonate
– after birth abdominal distension and vomiting
– failure to pass meconium
– rectal digital examination: tiny rectum

Obstruction of the small bowel
Dg: abdominal-plain film • distal extent of bowel gas help to determine the level
of any obstruction -proximal: duodenal obstruction
-distal: aganglionosis -intermediate: ileal or jejunal obstruction

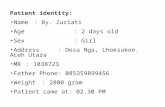
Proximal obstruction: Duodenal atresia and stenosis
•Path: failure of recanalisation of the fetal gut, typically near the ampulla of Vater •Clin signs: bilious vomiting within the first 24 hr •Diagnosis: plain radiograph- dilatation of the stomach and duodenum, „double-bubble” sign, gasless abdomen below •Therapy: surgery

Intermediate obstruction: 1.Jejunoileal atresia
2.Meconium ileus
Jejunoileal atresia
„in utero vascular accident”, failure of recanalisation
Intrauterine: malrotation, volvulus, herniation, intussusception
Postnatally: gangrene, perforation, peritonitis
Meconium ileus
Manifestation of cystic fibrosis - inspissation of abnormaly thick and tenacious meconium in distal small bowel
• Clinical signs: – abdominal distension
– Bile emesis
– Rectal digital examination: tiny rectum

Jejunoileal atresia and meconium ileus
Diagnosis: 1. plain radiograph of abdomen
– distended loops of gas-filled small bowel
– bubbly pattern of bowel gas: gas and inspissated meconium
2. Contrast enema – may be useful for separating
meconium ileus, ileal atresia and other causes of obstruction

Distal obstruction Congenital aganglionosis - Hirschsprung’s
disease
• Pathology: – Absence of both myenteric and submucosal plexus
– Usually in the sigmoid or rectosigmoid region
• Clinical signs: – Distension – Vomiting – Initial difficulty to pass meconium

Congenital aganglionosis- Hirschsprung’s disease
Diagnosis: 1. plain radiograph of abdomen
– distended loops with air-fluid level
2. Contrast enema – Normal (or small) caliber rectum – Transition zone abnormaly small
distal to dilated proximal colon – Dilated proximal sigmoid and
remainder of the colon

Intussusception
Path: invagination of one segment of the bowel into another – between ages of 6 months and 2 years – more common in boys – seasonal incidence: when respiratory and gastrointestinal infections occur
– most common type: ileum invaginating into the colon - „ileo-colic”
Clinical signs: abdominal mass, pain, vomiting, rectal bleeding

Intussusception
Dg: sonography - „target” sign
sonolucent outer rim surrounding a central echogenic area on cross-section

Anorectal malformation / Imperforate anus / cloacal malformation
• Abnormal termination of the hindgut • Spectrum -True imperforate anus – thin
membrane -Atresia of distal rectum • Clin signs
– lack of passage of meconium – absence of normal anus
• Relation of rectal pouch to pubococcygeal line
1.Low -usually visible perineal orifice,
stenotic or membrane -no GU tract communication 2.High -GU tract communication:
rectourinary-vaginal-vestibular fistula

Anorectal malformation - Imperforate anus
Dg: sonography -
meconium filled large bowel
distance from the rectal blind end to the perineum can be measured
Low lesion: less than 10mm
High lesion: more than 10mm (pouch terminates above the base of the bladder)

•Radiography: (Wangensteen-Rice) plain lateral radiograph with the patient in an inverted position + a lead marker is placed on the perineum •Distance between the rectal pouch and perineal marker is measured •Th: colostomy or perineal surgery
Anorectal malformation - Imperforate anus

Congenital and Developmental Anomalies of the Urinary Tract
Imaging modalities:
1. Sonography
2. MR-urography
2. Radionuclid imaging
3. Excretory urography
4. Voiding cystourography
5. MRI-MRA / CT-CTA

Congenital and Developmental Anomalies of the Urinary Tract
• Anomalies of number – Renal agenesis
• Anomalies of position – Dystopia/ectopia renis
• Anomalies of form: – Ren arcuatum/ horseshoe kidney

Congenital and Developmental Anomalies of the Urinary Tract
• Anomalies of structure: – Dysplasia:
• Aplasia • Hypoplasia
– Cystic disease • Ren polycysticum • Ren multicysticum
• Anomalies of the renal pelvis and ureter – Ren et ureter duplex – Ureterocele

Urinary obstruction: Hydronephrosis
Most common causes: 1. Uretero-
pelvic junction obstruction 2. Uretero-
vesical obstruction 3. Bladder outlet
obstruction 4. Urethral
obstruction The principal structural changes:
dilation and elongation of the urinary channels above the level of the obstruction!

Ureteropelvic junction obstruction
• Dilated renal collecting system but no ureter
1. Intrinsic stenosis: abnormal development of the muscle fibers at the ureteropelvic junction
2. Extrinsic stenosis: band, adhesion, aberrant vessel
• Clinical signs: palpable mass, abdominal pain, haematuria, urinary tract infection
• Diagnosis: sonography - large renal pelvis and calyces, lack of visualisation of distal ureter
• Therapy: surgical

Ureteropelvic obstruction
• MR-urography
• Excretory urography: – Contrast excretion into dilated collecting system
• Dg: – marked hydronephrosis that ends abruptly at the ureteropelvic junction with normal caliber ureter downstream

Ureterovesical obstruction
• Dilated renal collecting system with ureter

Ureteropelvic duplication - Ureterocele
Ureteropelvic duplication: presence of two separate collecting systems in one kidney
Two draining ureters may join above the bladder (partial duplication) or insert into the bladder separarely (complete duplication)
The ureter draining the cephalad portion of the kidney tends to insert in the bladder inferior and medial to the ureter draining the lower segment of the kidney.
The upper pole tends to obstruct. The lower pole tends to have vesicoureteral
reflux The upper pole ureteral orifice is ectopic in
location and often associated with ureterocele

Ureteropelvic duplication - Ureterocele
Ureterocele: • Herniation into the
bladder of the dilated distal end of the ureter
• Categorised according to their position: – Intravesical – Extravesical
• Categorised according to their insertion: – Orthotopic – Ectopic

Brain • Imaging modalities: 1. Sonography 2. MRI 3. CT • Sonography is extremely valuable in identifying normal and abnormal intracranial structure.
• The special technique is the transcranial US scanning through the anterior fontanelle.

Intracranial hemorrhage
1. Periventricular - intraventricular: in premature, most common and most severe
2. Subarachnoideal: in premature common, but almost always clinically benign
3. Subdural: in full-term infant, uncommon, but usually severe
4. Intracerebellar: in premature, uncommon, but usually severe

Periventricular-Intraventricular Hemorrage
• Premature infant: weigthing less than 1500g or under 32 weeks of gestation
• Common site: germinal matrix at the junction of the head of the caudate nucleus and choroid plexus in the floor of the lateral ventriculus
• Possible causes: hypoxia or ischaemia hyperperfusion or venous distension increased vascular pressure rupture of vessels of germinative matrix PVH

Congenital dysplasia of the hip
• Abnormal position of the femoral head relative to the acetabulum which results in abnormal growth of both components of the hip
• More common in breech babies, fetuses with oligohydramnios
• Much more common in girls than boys

Early diagnosis is important because even a short delay can
lead to abnormal hip development!
• Diagnosis: 1. sonography – visualize the cartilaginous
components of the hip - position of the femoral head, depth
of the acetabulum 2. radiography – the angle of the acetabular roof
(should be less than 30 degrees) - Shenton line

Sonography: coronal image of the normal hip with the transducer positioned lateral to the femur