Unit I: Framework Bone Structure Chapter 6. The Human Skeleton AdvantageDisadvantage Weight...
-
Upload
claude-malone -
Category
Documents
-
view
218 -
download
2
Transcript of Unit I: Framework Bone Structure Chapter 6. The Human Skeleton AdvantageDisadvantage Weight...

Unit I: Framework
Bone Structure
Chapter 6

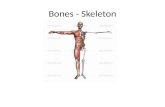
The Human Skeleton
Advantage Disadvantage
Weight
Structure
Number of Bones

Bone Shapes
Figure 6.1 1
Long Bones• long and slender
• serve as levers to produce movement Humerus
Humerous
Radius
Ulna
Metacarpals
Phalanges
Femur
Tibia
Fibula
Metatarsals

Bone Shapes
Figure 6.1 1
Flat Bones• thin, roughly parallel surfaces
• provide protection and surface area for the attachment of skeletal muscles.
Parietal bone
Cranial
Ribs
Sternum
Scapula
Pelvis

Bone Shapes
Figure 6.1 1
Short BonesCarpalbones
•small and boxy
• movement in multiple directions
Tarsals
Carpals

Bone Shapes
Figure 6.1 1
Sesamoid Bones• small, flat, sesame seed shaped
• develop inside tendons
• knees, hands, and feet
Patella

Bone Shapes
Figure 6.1 1
Sutural Bones• small, flat, irregularly shaped
• between the flat bones of the skull
Suturalbone
Sutures

Bone Shapes
Figure 6.1 1
Irregular Bones• complex shapes
Vertebra
Vertebrae
Facial bones

Bone Structure
• Osseous tissue (bone) is a connective tissue
• Hardened by calcification/mineralization
• Ossification
• Osteogenesis
• “Bone” can include many other types of tissues
• Bone is a composite for strength and flexibility
• Collagen – strong and flexible
• Minerals – rigid
Osteoporosis:• Loss of bone mass compromises normal function• ↓ osteoblast activity• Impacted by other systems: Endocrine, Integumentary, Digestive, Muscle

Diaphysis – shaft
Epiphysis – enlarged ends
Metaphysis – found between the diaphysis and epiphysis

Bone Structure
• Compact bone – strength
• Spongy bone - lightweight
• Medullary cavity –
•Red marrow –
•Yellow marrow –

Bone Structure
• Nutrient Foramen – allows nutrients and blood vessels passage
•Articular cartilage – hyaline cartilage covering the joint surface
• Periosteum – external sheath bone covering
• Epiphyseal plate/line – zone of growth

Bone Development
1. Intramembranous Ossification
2. Endochondral Ossification

Intramembranous Ossification
• Produces the flat bones of the skull and the clavicle
Connective Tissue
Site of future bone
Membrane-like layers of connective tissue form at sites of future bones.
Some of the connective tissue cells enlarge and differentiate into osteoblasts.
Osteoblasts on inside of periosteum form compact bone.
Cells of the membrane-like layer of connective tissue that remain outside the developing bone give rise to the periosteum.

Endochondral Ossification
• Most bones of the skeleton develop this way
• Bones develop from an existing model made of hyaline cartilage

Bone Remodeling
• Osteoprogenitor – stem cells divide to produce osteoblasts
• Osteoblasts – deposit new tissue, produces collagen fibers
• Osteoclasts – remove matrix
• Regulated by hormones: Parathyroid, Calcitonin, Calcitriol

Figure 6 Section 2
Composition of Bone Bone Contains …
99% of the body’s calcium
4% of the body’s potassium
35% of the body’s sodium
50% of the body’s magnesium
80% of the body’s carbonate
99% of the body’s phosphate
Calcium 39%
Potassium 0.2%
Sodium 0.7%
Magnesium 0.5%
Carbonate 9.8%
Phosphate 17%
67%Total inorganiccomponents
Organiccompounds
(mostly collagen)33%
Intestines absorb calciumand phosphate ions from the diet.
Rate of absorption ishormonally regulated.
Normal Ca2+
levels inplasma
Kidneys excrete calcium and phosphate ions in the urine.
Rate is hormonally regulated.
Bone
In the skeleton, osteoblasts and osteoclasts are working simultaneously.
Rate is hormonally regulated.

Homeostasis
• Disturbances can disrupt the functioning of the nervous and muscular systems in particular.
– Hypercalcemia
– Muscle weakness and sluggish reflexes
– Hypocalcemia
– Muscle spasms and tremors

Factors That Increase Blood Calcium Levels
Secrete parathyroid hormone (PTH).
(below 8.5 mg/dL)Low Calcium Ion Levels in Plasma
Parathyroid Gland Response
Osteoclast
Bone
•stimulates osteoclasts
•accelerates erosion of bone matrix
Enhances thecalcium-absorbingeffects of calcitriolon the intestines.
Increases renal production of calcitriol,which iscontinuously secreted at low levels.
PTH
more
calcitriol
Calcium released Calcium absorbed quickly Calcium conserved
Less calcium lostin urine
Ca2+
levels inplasma increase
Bone Response Intestinal Response Kidney Response
Figure 6.9 1

Figure 6.9 2
Factors That Decrease Blood Calcium Levels
Bone Response Intestinal Response Kidney Response
High Calcium Ion Levels in Plasma(above 11 mg/dL)
Thyroid Gland Response
C cells secrete calcitonin.
Calcitonin
• Inhibits osteoclasts
• osteoblasts continue todeposit calcium withinthe matrix of bones.
Bone
less
calcitriol
Decrease inthe rate ofcalcium ionabsorptionfrom theintestinalcontents.
Inhibitory effect: Suppresses calcium ion reabsorption.
Calcium storedCalcium absorbed slowly Calcium excreted
More calcium lostin urine
Ca2+
levels inplasma decrease