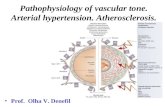
Pathophysiology of vascular tone. Arterial hypertension. Atherosclerosis. Prof. Olha V. Denefil.
The Pathophysiology of Atherosclerosis
description
Transcript of The Pathophysiology of Atherosclerosis
Definition of Atherosclerosis
Atherosclerosis can be described as the hardening and narrowing of the arteries that occur due to a build up of atherosclerotic plaque in the arterial wall. This plaque usually contains white blood cells, smooth muscle cells, cholesterol, lipids, calcium, collagen and fibrin and over time increases in size.
The plaque eventually encroaches on the lumen of these vessels
How are plaques formed?
An initial injury or dysfunction of the vascular endothelium is believed to trigger plaque formation or atherogenesis
Injury could be caused by Elevated levels of cholesterol and triglycerides in the
blood High blood pressure Cigarette smoking
Injury causes increased permeability of the endothelium to low density lipoproteins (LDLs)
How plaques are formed
LDLs penetrate endothelium and deposit in the arterial intima where they become oxidized by reactive oxygen species released by the dysfunctional endothelial cells
Oxidized LDLs activate endothelial cells to produce adhesion molecules
How plaques are formed The adhesion molecules bind
to leukocytes namely, monocytes and T-helper cells.
Once bound to the adhesion molecules, the leukocytes enter the intima where the monocytes differentiate into macrophages.
The macrophages take up oxidized LDLs and become “foam cells” which form a fatty streak in the artery wall.
How plaques are formed
The foam cells release chemokines to attract more macrophages
They also release IGF-1 which promotes Smooth muscle cell (SMC) migration from the tunica media into the intima, and their subsequent proliferation
The increased proliferation of SMC cells leads to increased synthesis of collagen which causes hardening of the plaque
How plaques are formed
T-Helper cells produce IFNγ which activate endothelial cells to produce more adhesion molecules and bind more white blood cells to produce even more foam cells
How plaques are formed When foam cells die, they
release their lipid contents into the plaque which drives the growth of the plaque
Foam cells also release proinflammatory cytokines and reactive oxygen species which both increase inflammation in the area
Pressure increases in the plaque which can cause the plaque to rupture and lead to thrombus formation
Thrombus formation
If the plaque ruptures, coagulation occurs to prevent the plaque from spilling its contents into the lumen of the vessel
The thrombus formed can impede blood flow leading to ischemia