The Future of Healthcare: Accountability and Transparency for Outcomes and Costs Excel for New...
-
Upload
lesley-lester -
Category
Documents
-
view
223 -
download
0
Transcript of The Future of Healthcare: Accountability and Transparency for Outcomes and Costs Excel for New...

The Future of Healthcare: Accountability and Transparency for Outcomes and Costs
Excel for New LeadersCurt Steinhart, MD – OU Medical System
Dale W. Bratzler, DO, MPH – OU Physicians

OBJECTIVES
• Give examples of what is “Right Here, Right Now”
• Show relevance to stakeholders– Physicians– Leaders– Administrators
• Place current and near-term imperatives in the context of the “Four Actions Framework”

Why was health reform inevitable?

1980
1981
1982
1983
1984
1985
1986
1987
1988
1989
1990
1991
1992
1993
1994
1995
1996
1997
1998
1999
2000
2001
2002
2003
2004
2005
2006
2007
2008
2009
2010
2011
2012
2013
0
2
4
6
8
10
12
14
16
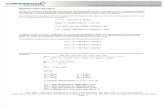
18US (17.1%)FR (11.6%)SWE (11.5%)GER (11.2%)NETH (11.1%)SWIZ (11.1%)DEN (11.1%)NZ (11.0%)CAN (10.7%)JAP (10.2%)NOR (9.4%)AUS (9.4%)*UK (8.8%)
Notes: GDP refers to gross domestic product. Dutch and Swiss data are for current spending only, and exclude spending on capital formation of health care providers.Source: OECD Health Data 2015.
Exhibit 1. Health Care Spending as a Percentage of GDP, 1980–2013
Percent
* 2012.


http://www.iom.edu/Reports/2011/~/media/Files/widget/VSRT/healthcare-waste.swf

Background
JAMA. 2013;310(18):1947-1963.
Where do we spend our healthcare dollar?
Hospitals and other care facilities, along with professional services are the primary target of most efforts to reign in healthcare spending.

http://www.iom.edu/Reports/2011/~/media/Files/widget/VSRT/healthcare-waste.swf

Rising “Consumerism” around Health Care
• Consumer groups increasingly demanding data about the quality and costs of care (“transparency”)– Rising co-pays and deductibles– Costs for insurance growing much faster
than incomes– Increased lay reports about quality issues in
healthcare• Legislators responded

Growing Recognition………
• US has the best “sick care” (not chronic care) system in the world– High tech– Complex care– Heavily hospital- and specialty-based– Very costly
But………• Our population is not healthy

JAMA. 2013;310(18):1947-1963.
How are those paying the bills responding?


Many Quality and Payment Provisions in the ACA
• Required by law….– Public quality reporting:
• Hospitals, dialysis units, nursing homes, home health agencies, physician practices, cancer centers…..
– Value-based payment• Reward high quality care – penalize poor quality care
– Hold providers accountable for overall costs of care (“efficiency”)

Healthcare quality is in the public domain for most
settings of care!

Move to “Value”
Value = Quality (and Service)/Costs
Goal: We want the highest quality of care (and service) at the lowest costs.

Incremental FFS payments
for value
Bundled payments for acute episode
Bundled payments for chronic care/
disease carve-outs
Accountability for Population
Health
Current State: Payments for
Reporting
Range of Models in Existence or Development
Increasing assumed risk by provider
Increasing coordination/integration required
From…. ..get paid more for doing more
To…. ..profiting by keeping your population of patients healthy, delivering high-quality care, and doing so at less cost

Physician Practices

Physician Quality Reporting System (PQRS)Impact on Physician Payment
PQRS Incentives
Year Successful Not Successful
2009 2.0% --
2010 2.0% --
2011 1.0% --
2012 0.5% --
2013 0.5% --
2014 0.5% --
2015 No Incentive -1.5%
2016 + No Incentive -2.0%
http://www.cms.gov/Medicare/Quality-Initiatives-Patient-Assessment-Instruments/PQRS/

Physician Medicare Value Modifier

Quality and Resource Use Report (QRUR)
The Medicare Report Card!

Quality and Resource Use Report (QRUR)

Nine percent (9%) of a physician’s Medicare payment in 2017 is tied to performance on PQRS
measures, meaningful use, and the physician value modifier for care provided in 2015.

Payment reform is very bipartisan….. ..and not limited to Medicare or Medicaid

http://www.gpo.gov/fdsys/pkg/BILLS-114hr2enr/pdf/BILLS-114hr2enr.pdf
Medicare Access and CHIP Reauthorization Act of 2015 (MACRA)Is payment reform bipartisan??
Facts about MACRA:
Bill sponsor in the House was a Republican (a physician) from Texas
The Senate vote was 92 to 8!
The House vote was 392 to 37!

TITLE I—SGR Repeal and Medicare Provider Payment Modernization
• Creates incentives to use alternate payment models (APMs)– ACOs– Medical Homes– Bundled payment arrangements– Other (being developed)
• Financial incentives to participate in APMs as well as exclusion from the MIPS assessment
http://www.gpo.gov/fdsys/pkg/BILLS-114hr2enr/pdf/BILLS-114hr2enr.pdf

TITLE I—SGR Repeal and Medicare Provider Payment Modernization
Eligible Professional
Alternate Payment Mechanisms• “Substantial portion” of revenues*
from “approved” alternate payment models
5% bonus each year from 2019-2024
0.75% increase per year beginning in 2026
Merit-based Incentive Payment System†• Providers receive a score of 0-100• Each year, CMS will establish a
threshold score based on the median or mean composite performance scores of all providers
Providers scoring below the threshold will be subject to payment reductions (capped at 4% in 2018, 5% in 2019, 7% in 2020, and 9% in 2021 to 2023).
Providers scoring above the threshold will receive bonus payments (up to three times the annual penalty cap).
*25% of Medicare payments 2019-2020 50% of Medicare payments 2021-2022
75% of Medicare payments 2023 and beyond
†Scores will be posted to Physician Compare website

It’s not just Medicare
• Humana• UnitedHealthcare• BlueCross• Medicaid• Others (including some employers)
Most of the third-party payers have some incentive programs for quality metrics, or have begun focusing on cost and quality.

What are they measuring for quality?
• Most are focused on primary care services in the office setting– Common conditions (diabetes, hypertension,
COPD, ischemic vascular and coronary disease)– Preventive services
• Vaccinations• Screening examinations – particularly cancer screening
– At risk behaviors – smoking, obesity• Some specialty-specific quality metrics
(particularly specialty-specific registries)

What are they measuring for quality?
They are also measuring costs of care and “efficiency”……and they are holding us accountable for the
“episode of care.”

Hospital Stay
Medicare Part A costs
30 days post-discharge3 d
Admission Discharge
All Medicare Part A and Part Charges
An “episode” of care
Medicare Spending per Beneficiary
Cost Efficiency Measure

http://www.optuminsight.com/transparency/etg-links/episode-treatment-groups/
Aetna’s model for cost efficiency

http://managedcaremag.com/archives/1202/1202.narrow_networks.html

http://www.bizjournals.com/seattle/blog/health-care-inc/2013/10/seattle-childrens-suit-raises.html?page=all

What about hospitals?
• A long list of quality and cost metrics now impact hospital payment!– Publicly reported on Hospital Compare
website– Used to adjust hospital payments!

Examples of hospital metrics
• Hospital-acquired infections and complications
• Hospital-acquired conditions• Avoidable hospital readmissions• Avoidable hospital admissions• Hospital mortality rates for common
conditions• Patient satisfaction

Going forward…. ..most assuredly there will be…
• …greater accountability for costs and quality
• …greater transparency for all providers of care
• …market pressure to improve efficiency
………….and the pace is speeding up dramatically!

Sylvia M. Burwell, January 26, 2015

Hip and knee replacements are some of the most common surgeries that Medicare beneficiaries receive. In 2013, there were more than 400,000 inpatient primary procedures in Medicare, costing more than $7 billion for hospitalization alone.
http://innovation.cms.gov/initiatives/ccjr/


FOUR ACTIONS FRAMEWORK