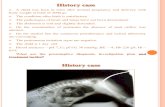
imperforate ani
-
Upload
oktania-putri-kusnawan -
Category
Documents
-
view
235 -
download
0
Transcript of imperforate ani
-
8/12/2019 imperforate ani
1/24
CLINICAL SCIENCE SESSION
IMPERFORATE ANUS
Diajukan untuk memenuhi tugas Program Pendidikan Profesi Dokter (P3D)
SMF Ilmu Bedah
Disusun oleh:
Cyndee Bayu Naga Dewata 12010011044
Khairuli Amri 12010011028Ilham Rizky Ernawan 12100100908
Partisipan :
Dety Nur Rachmawati 12010011021
Marry Nadya Elmiera 12010011007
Eva Noviani Lestari 12010011035
Dini Paramita Defrin 12010011068
Preseptor:
Liza Nursanti dr.,Sp.B
SMF ILMU BEDAH
PROGRAM PENDIDIKAN PROFESI DOKTER
FAKULTAS KEDOKTERAN
UNIVERSITAS ISLAM BANDUNG
RS AL-ISLAM BANDUNG
2011
-
8/12/2019 imperforate ani
2/24
CHAPTER I
PREFACE
1.1 BackgroundAnorectal malformations include a wide spectrum of defects in the
development of the lowest portion of the intestinal and urogenital tracts. Many
children with these malformations are said to have an imperforate anus because
they have no opening where the anus should be. Although the term mayaccurately describe a child's outward appearance, it often belies the true
complexity of the malformation beneath. When a malformation of the anus is
present, the muscles and nerves associated with the anus often have a similar
degree of malformation. The spine and urogenital tract may also be involved
The position and nature of these malformations made repair difficult for early
surgeons. The affected organs are located deep in the pelvis and are not well
visualized through abdominal incisions. Traditional surgical dictum did not allow
for division of the posterior midline because this division of the muscle was
believed, somewhat erroneously, to cause incontinence in the child. Therefore,
surgeons approached these malformations using a combined abdominal, sacral,
and perineal approach, with limited visibility. Such approaches have put
continence, and surrounding genitourinary structures, at greater risk than simply
cutting sphincter muscles because of the difficulty of adequately visualizing the
malformation through limited incisions. This principle was central to the
development of the surgical techniques currently used to repair these
malformations.
In 1982, Pea et al reported the results of the use of a posterior sagittal
surgical repair approach.[1] Pea et al used the traditional approach with a sacral
incision and made the incisions progressively larger in an attempt to adequately
visualize the anatomy. Eventually, the entire posterior sagittal plane was opened,
-
8/12/2019 imperforate ani
3/24
-
8/12/2019 imperforate ani
4/24
CHAPTER II
LITERATURE REVIEW
2.1 Embriology of Digestive
As a result of cephalocaudal and lateral folding of the embryo, a portion of
the endoderm-lined yolk sac cavity is incorporated into the embryo to form the
primitive gut. Two other portions of the endoderm-lined cavity, the yolk sac and
the allantois, remain outside the embryo (Fig. 13.1, AD). In the cephalic and
caudal parts of the embryo, the primitive gut forms a blind-ending tube, the
foregut and hindgut, respectively. The middle part, the midgut, remains
temporally connected to the yolk sac by means of the vitelline duct, or yolk stalk
(Fig. 13.1D). Development of the primitive gut and its derivatives is usually
discussed in four sections:
1. The pharyngeal gut, or pharynx, extends from the buccopharyngeal
membrane to the tracheobronchial diverticulum (Fig. 13.1D); since this
section is particularly important for development of the head and neck, it isdiscussed in Chapter 15.
2. The foregut lies caudal to the pharyngeal tube and extends as far caudally as
the liver outgrowth.
3. The midgut begins caudal to the liver bud and extends to the junction of the
right two-thirds and left third of the transverse colon in the adult.
4. The hindgut extends from the left third of the transverse colon to the cloacal
membrane (Fig. 13.1). Endoderm forms the epithelial lining of the digestive
tract and gives rise to the parenchyma of glands, such as the liver and
pancreas. Muscle, connective tissue, and peritoneal components of the wall of
the gut are derived from splanchnic mesoderm.
-
8/12/2019 imperforate ani
5/24
-
8/12/2019 imperforate ani
6/24
Figure 2.2 Diagrams of the mid- and hindgut regions. The morphogen sonic
hedgehog (SHH) is secreted by gut endoderm and induces a nested expression of
HOX genes in surrounding mesoderm.HOX expression then initiates a cascade of
genes that instruct gut endoderm to differentiate into its regional identities.
Signaling between the two tissues is an example of an epithelial-mesenchymal
interaction.
The hindgut gives rise to the region from the distal third of the transverse
colon to the upper part of the anal canal; the distal part of the anal canal originates
from ectoderm. The hindgut enters the posterior region of the cloaca (future
anorectal canal), and the allantois enters the anterior region (future urogenital
sinus). Breakdown of the cloacal membrane covering this area provides
communication to the exterior for the anus and urogenital sinus. Abnormalities in
the size of the posterior region of the cloaca shift the entrance of the anus
anteriorly, causing rectovaginal and rectourethral fistulas and atresias (Figs. 2.3
and 2.4).
-
8/12/2019 imperforate ani
7/24
Figure 2.3 Cloacal region in embryos at successive stages of development.A. The hindgut enters the posterior portion of the cloaca, the future anorectal
canal; the allantois enters the anterior portion, the future urogenital sinus. The
urorectal septum is formed by merging of the mesoderm covering the allantois
and the yolk sac (Fig. 13.1D). The cloacal membrane, which forms the ventral
boundary of the cloaca, is composed of ectoderm and endoderm.
B. As caudal folding of the embryo continues, the urorectal septum moves closer
to the cloacal membrane, although it never contacts this structure.
C. Lengthening of the genital tubercle pulls the urogenital portion of the cloaca
anteriorly; breakdown of the cloacal membrane creates an opening for the hindgut
and one for the urogenital sinus. The tip of the urorectal septum forms the perineal
body.
Figure 2.4 Abnormal development of the cloacal region at 7 weeks.
-
8/12/2019 imperforate ani
8/24
A. High urorectal fistula resulting from a large decrease in size of the posterior
portion of the cloaca and cloacal membrane that shifts the opening of the hindgut
further anteriorly.
B. Imperforate anus. The anal canal fails to recanalize, leaving a diaphragm
between the upper and lower portions of the anal canal.
2.2 Anatomy of Anorectal
The rectum is approximately 12 to 15 cm in length. Three distinct
submucosal folds, the valves of Houston, extend into the rectal lumen. Posteriorly,
the presacral fascia separates the rectum from the presacral venous plexus and the
pelvic nerves. At S4, the rectosacral fascia (Waldeyer's fascia) extends forward
and downward and attaches to the fascia propria at the anorectal junction.
Anteriorly, Denonvilliers' fascia separates the rectum from the prostate and
seminal vesicles in men and from the vagina in women. The lateral ligaments
support the lower rectum. The surgical anal canal measures 2 to 4 cm in length
and is generally longer in men than in women. It begins at the anorectal junction
and terminates at the anal verge. The dentate or pectinate line marks the transitionpoint between columnar rectal mucosa and squamous anoderm. The 1 to 2 cm of
mucosa just proximal to the dentate line shares histologic characteristics of
columnar, cuboidal, and squamous epithelium and is referred to as the anal
transition zone. The dentate line is surrounded by longitudinal mucosal folds,
known as the columns of Morgagni, into which the anal crypts empty.
-
8/12/2019 imperforate ani
9/24
-
8/12/2019 imperforate ani
10/24
Anorectal Vascular Supply begin the superior rectal artery arises from the
terminal branch of the inferior mesenteric artery and supplies the upper rectum.
The middle rectal artery arises from the internal iliac; the presence and size of
these arteries are highly variable. The inferior rectal artery arises from the internal
pudendal artery, which is a branch of the internal iliac artery. A rich network of
collaterals connects the terminal arterioles of each of these arteries, thus making
the rectum relatively resistant to ischemia (Fig. 2.7)
Figure 2.7 Arterial Supply of the rectum and anal canal
The venous drainage of the rectum parallels the arterial supply. The superior
rectal vein drains into the portal system via the inferior mesenteric vein. The
middle rectal veindrains into the internal iliac vein. The inferior rectal veindrains
into the internal pudendal vein, and subsequently into the internal iliac vein. A
submucosal plexus deep to the columns of Morgagni forms the hemorrhoidal
plexusand drains into all three veins.
-
8/12/2019 imperforate ani
11/24
Lymphatic drainage of the rectum parallels the vascular supply. Lymphatic
channels in the upper and middle rectum drain superiorly into the inferior
mesenteric lymph nodes. Lymphatic channels in the lower rectum drain both
superiorly into the inferior mesenteric lymph nodes and laterally into the internal
iliac lymph nodes. The anal canal has a more complex pattern of lymphatic
drainage. Proximal to the dentate line, lymph drains into both the inferior
mesenteric lymph nodes and the internal iliac lymph nodes. Distal to the dentate
line, lymph primarily drains into the inguinal lymph nodes, but can also drain into
the inferior mesenteric lymph nodes and internal iliac lymph nodes.
Both sympathetic and parasympathetic nerves innervate the anorectum.
Sympathetic nerve fibers are derived from L1-L3 and join the preaortic plexus.
The preaortic nerve fibers then extend below the aorta to form the hypogastric
plexus, which subsequently joins the parasympathetic fibers to form the pelvic
plexus. Parasympathetic nerve fibers are known as the nervi erigentes and
originate from S2-S4. These fibers join the sympathetic fibers to form the pelvic
plexus. Sympathetic and parasympathetic fibers then supply the anorectum and
adjacent urogenital organs.
The internal anal sphincter is innervated by sympathetic and
parasympathetic nerve fibers; both types of fibers inhibit sphincter contraction.
The external anal sphincter and puborectalis muscles are innervated by the
inferior rectal branch of the internal pudendal nerve. The levator ani receives
innervation from both the internal pudendal nerve and direct branches of S3 to
S5. Sensory innervation to the anal canal is provided by the inferior rectal branch
of the pudendal nerve. While the rectum is relatively insensate, the anal canal
below the dentate line is sensate
-
8/12/2019 imperforate ani
12/24
CHAPTER III
IMPERFORATE ANUS
3.1 Definition
Anorektal malformation of defects in the development of the lowest
portion of the intestinal. Figure Although the precise embryologic defect that
causes anorectal malformations has not been determined, cloacal membrane
formation and subsequent breakdown into urogenital and anal openings should
occur by 8 weeks' gestation. Defects in the formation or shape of the posterior
urorectal septum account for many of the described abnormalities of imperforate
anus. Mllerian ducts appear after this critical period; how they are incorporated
into this development is unclear.
3.3 Incidence and epidemologi
United States Anorectal malformations occur in approximately 1 newborn
per 5000 live births. Mortality/Morbidity Anorectal and urogenital malformations
are rarely fatal, although some associated anomalies (cardiac, renal) can be life
threatening. Intestinal perforation or postoperative septic complications in a
newborn with imperforate anus can result in mortality or severe morbidity. no
known racial and no known sex predilection has been reported.
3.4 Clinical Manifestation
In males, the testicles must be palpated in the scrotum. The perineum is
then examined. Perineal fistulas are diagnosed upon discovery of openings on the
perineum, meconium or mucus in a small strip running up into the scrotal median
raphe, a perineal groove, or a bucket-handle malformation in the anal dimple skin.
If no opening is present, urine is obtained for study, and the child is observed for
24 hours.
-
8/12/2019 imperforate ani
13/24
In females, a perineal fistula can be directly identified as a small opening
on the perineum. If none is present, the labia are separated to search for a
vestibular fistula. A fourchette fistula is a type of vestibular fistula that straddles
the spectrum of malformation between perineal and vestibular; it is characterized
by wet mucosa of the vestibule anteriorly and a dry anoderm posteriorly at the
junction of the vestibule and perineum
Imperforate Anus And Associated Malformation
If the child has a normal urethra and no vestibular fistula, she may haveimperforate anus without fistula. If she appears to have trisomy 21, the likelihood
increases that she does not have a fistula. Girls with normal urethra and no visible
fistula are observed for 24 hours to allow a perineal fistula to present before
operation is required. This waiting period is beneficial in differentiating between
children with perineal fistula who may be effectively treated using only a minimal
anoplasty from those who require colostomy with further evaluation using distal
colostography. Examples of colostography findings are shown in the images
below.
Cardiovascular malformations occur in 12-22% of patients. The most
common lesions are tetralogy of Fallot and ventricular septal defects.
Transposition of the great arteries andhypoplastic left heart syndrome have been
reported but are rare.
Many GI malformations have been described in association withimperforate anus. As many as 10% of patients have tracheoesophageal
abnormalities. Duodenal obstruction due to annular pancreas or duodenal atresia
occurs in a small percentage of patients. Malrotation with Ladd bands that causes
obstruction has also been described.Hirschsprung disease has been well described
in association with imperforate anus, although the incidence of this combined
condition is unknown. Constipation is common.
http://emedicine.medscape.com/article/163628-overviewhttp://emedicine.medscape.com/article/892980-overviewhttp://emedicine.medscape.com/article/900574-overviewhttp://emedicine.medscape.com/article/890196-overviewhttp://emedicine.medscape.com/article/929733-overviewhttp://emedicine.medscape.com/article/929733-overviewhttp://emedicine.medscape.com/article/890196-overviewhttp://emedicine.medscape.com/article/900574-overviewhttp://emedicine.medscape.com/article/892980-overviewhttp://emedicine.medscape.com/article/163628-overview -
8/12/2019 imperforate ani
14/24
The association of imperforate anus and vertebral anomalies has been
recognized for many years. Patients with high lesions have an increased risk of
this association. Lumbosacral anomalies predominate and occur in approximately
one third of patients with imperforate anus.
The frequency of spinal dysraphism (evaluated with ultrasonography or
MRI) had been thought to increase with the severity of the lesion, with higher
malformations having greater frequency than lower malformations. Several
studies have disputed this and have even shown higher incidence of spinal
malformations in children with low malformations. The most common type of
dysraphism is tethered spinal cord, which is present in as many as 35% of
patients. The normal spinal cord terminates between the first and second lumbar
vertebral bodies. In patients with a tethered spinal cord, the cord ends lower in the
lumbar spine. Cord lipomas and syringohydromyelia are also common. All
lumbosacral spinal malformations negatively affect the child's prognosis with
respect to urinary and fecal incontinence.
Currarino described a triad of sacral defect, presacral mass, and
imperforate anus.[2] All patients with an anorectal malformation must be screened
for these vertebral abnormalities in the newborn period using sacral radiography
and lumbosacral spinal ultrasonography. As many as one half of patients with
anorectal malformations have urologic abnormalities. Urinary anomalies are more
common in patients with more complex lesions. Improved imaging studies have
provided the ability to document an increased range of abnormalities. Mild
hydronephrosis is the most common abnormal ultrasonography finding.
Vesicoureteric reflux is also a frequent finding, followed by renal agenesis and
dysplasia.Cryptorchidism reportedly occurs in 3-19% of males.
Vaginal and uterine abnormalities are common. Bicornate uterus and
uterus didelphys occur in 35% of female patients with imperforate anus. A vaginal
septum is the most common vaginal abnormality and is seen in as many as one
half of girls born with a cloacal malformation. Vaginal duplication and agenesis
http://emedicine.medscape.com/article/1017420-overviewhttp://emedicine.medscape.com/article/1017420-overview -
8/12/2019 imperforate ani
15/24
have also been reported. Vaginal agenesis may be associated with ipsilateral
absent ovary and kidney.
3.5 Classification
Pena proposed a classification system that specifically describes the
location of the fistulous opening. In males the fistula may communicate with:
A. The perineum (cutaneous perineal fistula).
B. The lowest portion of the posterior urethra (rectourethral bulbar fistula).
C. The upper portion of the posterior urethra (rectourethral prostatic fistula).
D. The bladder neck (rectovesicular fistula).
-
8/12/2019 imperforate ani
16/24
Figure 3.1 Classification of anorectal malformation
In females, the urethra may open onto the perineum between the female
genitalia and the center of the sphincter (cutaneous perineal fistula), or into the
vestibule of the vagina (vestibular fistula). In both sexes, the rectum may end in a
completely blind fashion (imperorate anus without fistula). In rare cases, patients
may have a normal anal canal, yet there may be total atresia or severe stenosis of
the rectum.
3.5 Diagnosis
-
8/12/2019 imperforate ani
17/24
Patients with Imperforate anus are usually stable, and the diagnosis is
readily apparent. Despite the obstruction, the abdomen is initially not distended,
and there is rarely any urgency to intervene.
D
Figure 3.2 Distal colostogram, posteroanterior view. The initial phase of
augmented-pressure distal colostography aims to determine where the colostomy
was placed in the colon and how much colon is available for pull-through, without
taking down the colostomy.
The principles of management center around diagnosing the type of defect
that is present (high versus low), and evaluating the presence of associated
anomalies. All patients should therefore have an orogastric tube placed and be
monitored for the appearance of meconium in or around the perineum, or in the
urine. Investigation for associated defects should include:
A. Ultrasound of the abdomen to assess for the presence of urinary tractanomalies.
B. Echocardiogram.C. Spinal radiographs. An ultrasound of the spine should be performed to look
for the presence of a tethered cord.
D. To further classify the location of the fistula as either high or low, a lateralabdominal radiograph can be obtained with a radiopaque marker on the
http://refimgshow%281%29/ -
8/12/2019 imperforate ani
18/24
perineum. By placing the infant in the inverted position, the distance between
the most distal extent of air in the rectum and the perineal surface can be
measured. However, this study is imprecise.
Figure 3.3 Distal colostogram, lateral view. This image shows the second phase
of distal colostography, in which the patient is placed in the lateral position. Aradio-opaque marker is clearly visible in the lower right side of the image,
marking the muscle complex on the skin. This image shows that the rectal pouch
joins the urinary tract at the level of the bulbar urethra, a relatively common
malformation in boys.
3.5 Treatment
The surgical management of infants with imperforate anus is determinedby the anatomic defect. It may take up to 24 hours before the presence of a fistula
on the skin is noted, and thus it is important to observe the neonate for some time
before definitive surgery is undertaken. In general, when a low lesion is present,
only a perineal operation is required, without a colostomy. Infants with a high
lesion require a colostomy in the newborn period, followed by a pull-through
procedure at approximately 2 months of age.
http://refimgshow%282%29/ -
8/12/2019 imperforate ani
19/24
Figure 3.4 Prone Position
When a persistent cloaca is present, the urinary tract needs to be carefully
evaluated at the time of colostomy formation to ensure that normal emptying can
occur, and to determine whether the bladder needs to be drained by means of a
vesicostomy. If there is any doubt about the type of lesion, it is safer to perform a
colostomy rather than jeopardize the infant's long-term chances for continence by
performing an injudicious perineal operation. The type of pull-through procedure
favored by most pediatric surgeons today is the posterior sagittal anorectoplasty
(PSARP) procedure, as described by Pea and DeVries. This involves dividing
the levator ani and external sphincter complex in the midline posteriorly, and
bringing down the rectum after sufficient length is achieved.
Figure 3.5 Electrical stimulator probe used to show sphincteric contractions.
Used with electrical stimulator
http://www.emedicine.com/cgi-bin/foxweb.exe/makezoom@/em/makezoom?picture=/websites/emedicine/ped/images/Large/2276ped2924-40.jpg&template=izoom2http://www.emedicine.com/cgi-bin/foxweb.exe/makezoom@/em/makezoom?picture=/websites/emedicine/ped/images/Large/2277ped2924-41a.jpg&template=izoom2http://www.emedicine.com/cgi-bin/foxweb.exe/makezoom@/em/makezoom?picture=/websites/emedicine/ped/images/Large/2274ped2924-38.jpg&template=izoom2http://www.emedicine.com/cgi-bin/foxweb.exe/makezoom@/em/makezoom?picture=/websites/emedicine/ped/images/Large/2276ped2924-40.jpg&template=izoom2http://www.emedicine.com/cgi-bin/foxweb.exe/makezoom@/em/makezoom?picture=/websites/emedicine/ped/images/Large/2277ped2924-41a.jpg&template=izoom2http://www.emedicine.com/cgi-bin/foxweb.exe/makezoom@/em/makezoom?picture=/websites/emedicine/ped/images/Large/2274ped2924-38.jpg&template=izoom2http://www.emedicine.com/cgi-bin/foxweb.exe/makezoom@/em/makezoom?picture=/websites/emedicine/ped/images/Large/2276ped2924-40.jpg&template=izoom2http://www.emedicine.com/cgi-bin/foxweb.exe/makezoom@/em/makezoom?picture=/websites/emedicine/ped/images/Large/2277ped2924-41a.jpg&template=izoom2http://www.emedicine.com/cgi-bin/foxweb.exe/makezoom@/em/makezoom?picture=/websites/emedicine/ped/images/Large/2274ped2924-38.jpg&template=izoom2 -
8/12/2019 imperforate ani
20/24
.
Figure 3.6 Recommended colostomy with divided stomas, the proximal stoma in
the descending colon.
http://www.emedicine.com/cgi-bin/foxweb.exe/makezoom@/em/makezoom?picture=/websites/emedicine/ped/images/Large/2271ped2924-35.jpg&template=izoom2http://www.emedicine.com/cgi-bin/foxweb.exe/makezoom@/em/makezoom?picture=/websites/emedicine/ped/images/Large/2271ped2924-35.jpg&template=izoom2 -
8/12/2019 imperforate ani
21/24
Figure 3.6 Algorithm for treatment of newborn boy and female with anorectal
malformation
The type of pull-through procedure favored by most pediatric surgeons today is
the posterior sagittal anorectoplasty (PSARP) procedure, as described by Pea and
DeVries. This involves dividing the levator ani and external sphincter complex in the
midline posteriorly, and bringing down the rectum after sufficient length is achieved. Themuscles are then reconstructed and sutured to the rectum. The outcome of 1192 patients
who had undergone this procedure was recently reviewed by Pea and Hong. Seventy-
five percent of patients were found to have voluntary bowel movements, and nearly 40%
were considered totally continent. As a rule, patients with high lesions demonstrate an
increased incidence of incontinence, whereas those with low lesions are more likely to be
constipated.
-
8/12/2019 imperforate ani
22/24
Figure 3.7 posterior sagittal anorectoplasty
-
8/12/2019 imperforate ani
23/24
Post operation surgery complication is constipation that the major of the
complication which is happen to the patien that have a surgery of anorectal
malformation
3.6 Prognosis
Patients with a low opening has an excellent outcomes. Almost 75%
patient with low opening anorectal malformation become soiling, and later the
soiling will relieve by it self. Almost 25% of patient have a fecal incontinence and
should have a gut toilet management.
Patients with a high opening (more than 3cm) is have a bad outcomes
which functionally.
Pasien-pasien dengan MAR letak rendah seperti rectoperineal fistula
mempunyai excellent outcomes,juga pada vestibular fistula.Hampir 75% pasie-pasien
dengan anorectal malformations sering terjadi soiling.Episode dari soiling ini sering
berhubungan dengan konstipasi.Dengan terapi yang baik kejadian soiling biasanya
berkurang sampai menghilang.25% pasien mempunyai fekal inkontinens dan harus
mendapat managemen pembersihan usus.
Pencernaan harus dievaluasi ketika anak sudah berusia lebih dari 3 tahun.Pada
kasus ini maka diperlukan laxantive,special diet,dan enema. Pasien dengan fistula
rektourethral dan normal sacrum juga mempunyai out come yang baik.Hampir 80%
pasien dengan persisten kloaka dan normal sacrum mempunyai pencernaan yang
terkontrol.Pasien dengan MAR yang letak sangat tinggi seperti fistula bladder neck pada
pasien laki-laki mempunyai out come yang jelek,meskipun dengan sacrum yang normal.
-
8/12/2019 imperforate ani
24/24
Sakrum sendiri dapat menjadi predictor yang baik entuk menilai out
come.Pasien dengan hipodevelopmental sacrum sering mengalami masalah inkontinens
dan juga keadaan ini sering disertai dengan masalah-masalah di spinalnya.Ketika defek
spesifik tsb sudah ditemukan maka secara fungsional prognosis atas pasien tersebut
dapat diprediksi.
Jika pasien mempunyai defek dengan prognosis yang kurang baik seperti high
cloaca terutama tingginya lebih dari 3 cm;bladder neck fistula,maka keluarga perlu di
informed concent bahwa pasien nantinya memerlukan program bowel
managemen,biasanya saat berusia 3-4 tahun.