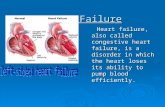
Heart Failure 2013
-
Upload
rahim-foreman -
Category
Documents
-
view
25 -
download
1
description
Transcript of Heart Failure 2013

Heart Failure 2013

Definition
• Inability of the heart to supply blood to meet metabolic demands of tissues resulting in inadequate tissue perfusion and volume overload

Heart Failure
• Implies “biventricular failure”
• Origin usually left sided
• Left ventricle (LV)enlarges capacity, muscle size & shape = “ventricular remodeling”
• LV weakens decreased ejection of blood, decreased stroke volume, decreased cardiac output

Incidence
5 million cases660,000 new cases/yearMost common discharge diagnosis age >65

Causes of Heart Failure• Myocardial infarction• Pulmonary embolism (RV failure)• Cardiomyopathy (both RV & LV failure)• Mitral insufficiency (LV failure)• Aortic regurgitation/stenosis (LV failure)• Hypertension (LV failure)• Volume overload• Myocarditis• Infections/toxins

Mechanism of Failure• Decline in cardiac function decreased cardiac
output• Drop in cardiac output decreased ejection
fraction• Ejection Fraction= percentage of blood left
ventricle pumps out with each beat– Normal= 55-70%– <40% = impaired function

Inciting EventInciting Event
Increased myocardial demandIncreased myocardial demand
Ventricular RemodelingVentricular Remodeling
Decreased cardiac outputDecreased cardiac output
Neurohormonal ActivationNeurohormonal Activation
Increased intravascular volumeIncreased intravascular volume
Increased wall stress and afterloadIncreased wall stress and afterload
Chronic Congestive FailureChronic Congestive Failure
Vasoconstriction(renin-angiotensisn)
Vasoconstriction(renin-angiotensisn)
Sodium & water retention
(Aldosterone)
Sodium & water retention
(Aldosterone)Sympathetic
increase in heart rate & contractility
Sympathetic increase in heart
rate & contractility

Compensatory Mechanisms

Etiology
• Cardiac Output dependent on:– Preload: amount of blood in left ventricle (LV)– Afterload: pressure against which LV must eject– Contractility: strength of contraction– Coordination of contraction between atria/ventricles– Heart Rate: amount of time available for filling and
emptying ventricles


Systolic Dysfunction“Poor Contraction”
• Heart enlarges/does not contract normally
• Decrease in muscle strength (thin walls)
• Forward blood flow decreases systemic hypoperfusion
• Stroke volume & ejection fraction decrease (EF<40%)
• Pulmonary congestion

Diastolic Dysfunction“Impaired Filling”
• Inability of the ventricle to fully relax
• Increased pressure & volume in ventricle
• Pressures back up to pulmonary veins pulmonary congestion
• Stroke volume reduced
• Echo: normal EF?, left atrial enlargement, pulmonary hypertension, heart wall abnormalities, right ventricular dilation


Clinical Manifestations• Left sided Failure (“Forward Failure”)
– Blood backs into pulmonary veins & capillaries lung congestion
• Dyspnea on exertion• Paroxysmal nocturnal dyspnea• Orthopnea• Pulmonary edema• Crackles• Cough• Tachycardia • S3, S4, systolic murmur• Insomnia, restlessness

Clinical Manifestations• Right Sided Failure (“Backward Failure”)
– Elevated pressures & congestion in systemic veins & capillaries
• Peripheral/Dependent edema
• Weight gain
• Liver congestion
• Distended neck veins
• Abnormal fluid in body cavities – Pleural, abdominal
• Anorexia & nausea
• Nocturia
• Weakness

Assessment
• History of symptoms
• Limits of activity/response to rest
• Peripheral pulses: quality, character
• Inspect/palpate precordium for lateral displacement of point of maximum impulse
• Sleeping patterns/sleep aids

Diagnostic Evaluation

Stages: American College of Cardiology/ American Heart Association
Stage Definition Examples
A High risk, no structural heart disease or HF
HTN, CAD, diabetes, family hx cardiomyopathy
B Structural heart disease, no signs of failure
Prior MI, systolic dysfunction, valvular disease, RV hypertrophy
C Structural heart disease, signs of failure
Dyspnea, fatigue, exercise intolerance, orthopnea
D Refractory HF despite maximal medical therapy

Classification: New York Heart Association
Class Functional Capacity
I Patients with cardiac disease: no limitation on physical activity
II Patients with cardiac disease: slight limitation on physical activity(fatigue, SOB, palpitation, anginal pain). Comfortable at rest
III Marked limitation of physical activity (fatigue, SOB, palpitation, anginal pain). Comfortable at rest
IV Inability to carry on any physical activity without discomfort. Symptoms of HF at rest

Goal: improve ventricular dysfuncton & prevent progression

Management• Inotropes
– Improve contractility, stroke volume, ejection fraction, cardiac output
– Increase myocardial oxygen consumption– Dobutamine, milrinone, digoxin
• Biventricular pacing: cardiac resynchroniztion therapy (CRT). Synchronizes LV systolic function so that LV walls contract at same time

Management• Reduction of Afterload
– Decrease in resistance of blood, valves, blood vessels
– Decreases work of left ventricle– Improved contractility, stroke volume, cardiac output
• Angiotensin Converting Enzyme (ACE) inhibitors (captopril, enalapril)
• Calcium Channel Blockers (nifedipine,verapamil)• Beta Blockers (metoprolol)• Angiotensin Receptor Blockers (ARBs) (valsartan,
losartan)

Management• Reduction of Preload
– Diuretic therapy• Loop Diuretics: lasix, bumex• Thiazide Diuretics: hydrochlorothiazide• Potassium Sparing: spironolactone, triamterene
– Venodilators (nitroglycerin)– Fluid & sodium restriction

Interventions
• Maintain adequate cardiac output
• Physical/emotional rest
• Evaluate for progression of left sided failure– Lowered systolic pressure– Narrowing of pulse pressure– Alterations in strong/weak pulsations– Auscultate heart sounds

Interventions
• Improve oxygentation– Raise head of bed– Auscultate lung fields– Observe for respiratory distress– Small frequent feedings– Oxygen as needed

Interventions
• Restore fluid balance– Diuretics– Strict I & o– Daily weight
• Assess for weight fluctuations • *Include weight assessment in intershift report*
– Observe for electrolyte depletion– Monitor for edema– Diet education

Complications
• Intractable/refractory heart failure
• Cardiac dysrhythmias
• Myocardial failure
• Digitalis toxicity
• Pulmonary infarction
• Pneumonia
• Emboli

Core Measures
• Evaluation of LV Function (EF)
– Echo report– Cath report– Nuclear stress test

Core Measures
• Adult Smoking Cessation– Heart failure patient with a history of smoking
within the past year
• ACEI or ARB presecribed at discharge– Left Ventricular ejection fraction (LVEF) <40%

Core Measure Exclusions• Patient refusal• Patient on LVAD• Patient <18 years of age• Transfer to acute care hospital• Comfort/Hospice care• Discharged to hospice• Expired• Left AMA• Patient involved in clinical trial

Patient Education
• Disease process: pumping action
• Signs & symptoms of recurrence– Weight gain– Swelling of ankles, feet, abdomen– Cough– Fatigue– Frequent urination at night
• Review medications, activity, diet

Teach Back
http://ruralhealth.uams.edu/health-literacy/teachback

References• Aherns, T., Prentice, D., & Kleinpell, R. (2011).
Progressive care nursing certification. New York: McGraw Hill Medical.
• Alspach, J. (2006). Core curriculum for critical care nursing. (6th ed., pp. 271-284). St Louis: Saunders Elsevier.
• American Heart Associatin. (2005). Guideline update for the diagnosis and management of chronic heart failure in the adult. Circulation, 112, 154-235.
• Aronow, W. (2006). Heart failure update. Geriatrics, 61(8), 16-20.