Physical Diagnosis Scalp, Ears,Nose, Sinuses. Describe Scalp. Diagnosis?
Diagnosis and treatment of physical urticaria
-
Upload
chulalongkorn-allergy-and-clinical-immunology-research-group -
Category
Documents
-
view
7.376 -
download
4
description
Transcript of Diagnosis and treatment of physical urticaria

Physical Urticaria
Theerapan SongnuyDec 7, 2012

Overview
• Definition• Epidemiology• Classification• Diagnosis• Treatment

UrticariaUrticaria : - The appearance of pruritic,erythematous skin elevation which blanch with pressure - Small venules & capillaries dilation in superficial dermis - Collagen fiber swelling Angioedema : - similar pathologic reaction - Involves deep dermis & subcutaneous tissue - Fewer mast cell & sensory nerve ending - More painful or burning sensation than pruritus - Often on face, tongue ,genitalia & extremities
Middleton’s Allergy 7th Edition

Physical Urticaria
• A heterogeneous group of inducible conditions that includes:
- Symptomatic dermographism/urticaria factitia - Cold contact urticaria - Heat contact urticaria - Delayed pressure urticaria - Vibratory urticaria /angioedema - Solar urticarias - Aquagenic urticaria - Contact urticaria - Exercise induced urticaria /anaphylaxis Allergy 2009; 64 (12): 1715-1721

Physical Triggers• Symptomatic dermographism / Urticaria factitia :
mechanical stroking• Cold contact urticaria : skin contact with cold
air/water/solids• Heat contact urticaria : skin contact with hot
air/water/solids• Delayed pressure urticaria: vertical sustained pressure• Vibratory urticaria/angioedema : vibration (e.g. pneumatic
hammer) • Solar urticaria : UV and/or visible light • Aquagenic urticaria : water contact at any temperature• Contact urticaria : contact with an allergic or nonallergic
stimulus• Exercise induced urticaria /anaphylaxis : physical exercise• Cholinergic urticaria : increased core body temperature Allergy 2009; 64 (12): 1715-1721

Epidemiology
• Urticaria - The life-time prevalence of any subtype is 20%
• Physical urticaria - prevalence 20% of chronic urticaria - In children prevalence ranges from 6.2-25.5%
Allergy 2009;64: 1417-1426Ann Allergy 1993:71:205-12Ann Allergy 1992; 69: 61-65


Aim: To study the prevalence, type, clinical data & natural history of physical urticaria includingprognostic factors for remissionMaterial & Methods : - A retrospective study - The Dermatologic Unit, Siriraj Hospital - Jan 2003-Dec 2008 - Patients aged above 18 years - Demographic data, causes of urticaria, associated diseases, physical exammination, lab etc.JEADV 2011 ; 25: 1194-1199.

• Tests to categorize type
- Dermographometer ( pressure at 4900 g/cm2 ) - Delayed-pressure ( sandbags 15 lbs over one shoulder for 15 min) then observe 2-8 hr. later
- Cold urticaria ( Ice-cube test, place ice inside plastic bag on forearm 10 min then observe 15 min later
- Cholinergic ( run until exhausted & sweaty ) then observe within 15 min
- Adrenergic ( ID noradrenalin 3-10 ng in 0.02 ml saline observe erythematous papule & halo ) JEADV 2011 ; 25: 1194-1199.

• Tests to categorize type - Solar urticaria ( photo test with visible light UVA, UVB ) - Others ; CBC, UA, ESR, ANA, cryoglobulin HBsAg, anti-HCV Ab etc.
Remission: non-urticarial wheal for at least 6 months after stop medication & negative test
JEADV 2011 ; 25: 1194-1199

JEADV 2011 ; 25: 1194-1199

JEADV 2011 ; 25: 1194-1199

JEADV 2011 ; 25: 1194-1199

JEADV 2011 ; 25: 1194-1199

• From chronic urticaria: physical urticaria was 7.2%• The most common type is symptomatic dermographism
• Only 13.9% associated with chronic spontaneous urticaria• No multiple types of physical urticaria
• ESR was the most common abnormal labs• The median time after onset before 50% remission - Cholinergic urticaria took the shortest course - Delayed-pressure took the longest period - After 1 y & 5 y from onset of symptom, 13 % & 50% of physical urticaria were free of symptoms

Symptomatic Dermatographism
• Syn : urticaria factitia, dermographic urticaria• The most common subtype of physical urticaria• Has to be differentiated from simple
Dermographism where wealing, but not pruritus, occurs after moderate stroking of the skin
• Develope itching & wealing at a lower force than that required to induce simple dermographism
• Other types of dermographism such as white dermographism (in atopic patients) are unrelated to symptomatic dermographism
Immunol Allergy Clin North Am2004;24:225–246.

Symptomatic Dermatographism
• Provocation testing
- A dermographometer : to apply a rubbing stimulus to a subject’s skin using predefined and reproducible pressures
- A calibrated dermographometer is commercially available (HTZ Limited, Vulcan Way, New Addington, Croydon, Surrey, UK)
- It has a spring-loaded smooth steel tip 0.9 mm in diameter. The pressure on the tip can be varied by turning a screw at the top of the instrument.
- The scale settings from 0 to 15 ( tip pressures from 20 to 160
g/mm2 )
Immunol Allergy Clin North Am2004;24:225–246.

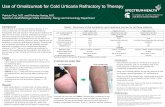
Figure 3 Dermatographism. Linear stroking of skin elicits a wheal within several minutes.
The American Journal of Medicine 2008; 121 ( 5) : 379 - 384

Symptomatic Dermatographism
• Diagnosis of symptomatic dermographism -the smooth blunt object should be held
perpendicular to and used to apply a light stroking pressure to the skin of the upper back or volar forearm
- The skin at the test site should be unbroken and free of obvious signs of infection
-Three parallel lines (up to 10 cm long) should be made with dermographometer settings equivalent to 20, 36 and 60 g/mm2.
Immunol Allergy Clin North Am2004;24:225–246.

Symptomatic Dermatographism
• The positive reaction : showing a wheal response & report pruritus at the site of provocation at 36 g/mm2 (353 kPa) or less
• A wheal response without itch on provocation at 60 g/mm2 (589 kPa) or higher indicates
simple dermographism• The test response should be read 10 min
after testing
J Am Acad Dermatol2008;59:752–757.

Management of Symptomatic Dermatographism
• Diphenhydramine or hydroxyzine 25-50 mg. qid for severe patient
• Non-sedating antihistamine in mildly to moderately severe cases, can be triple the usual dose
Middleton’s Allergy 7TH Edition



Conclusion
• Cyclosporin may be worth trying for antihistamine-resistant DU,
especially in those patient cases characterized by severe itching
. Further studies on a larger scale are expected to be conducted in order to generate stronger levels of clinical evidence.

Cold Urticaria & Related Disorders
• Trigger by a cold stimulus ; wind, liquid holding cold objects• Total body exposure can lead to hypotension ( swimming)• Disease begin in any age group, young adult• “Ice-cube Test” placing a plastic containing ice cube
inside on patient’s forearm for 4 min, then observe 10 min
Middleton’s Allergy 7th Edition

Cold Urticaria• Positive : a palpable & clearly visible weal & flare reaction with
itchy and/or burning sensation• In a positive test reaction, threshold testing should be performed
• Threshold level may help patients to avoid risky situations and their physician to optimize treatment
• Determining the stimulation time threshold, which is the shortest duration of cold exposure required to induce a positive test reaction
• Temperature thresholds, i.e. the highest temperature sufficient to induce a positive test reaction, can be assessed with TempTest
J Allergy Clin Immunol1986;78:417–423.

Cold-Dependent Syndromes• Idiopathic cold urticaria• Systemic cold urticaria( ice cube test negative) sensitive to
cold air• Cold-induced cholinergic urticaria• Cold-dependent dermographism• Delayed cold urticaria ( edema, pain)• Localized cold urticaria ( previous insect stinging)• Cold reflex urticaria• Associated with abnormal serum protein - cryoglobulinemia - cold agglutinin disease - cryofibrinogenemia - paroxysmal cold hemoglobinuria
Middleton’s Allergy 7th Edition

Cold Urticaria
• Mediators releasing from mast cell - histamine - PAF - LTE2 - Prostaglandin D2 - TNF-alpha - IL-3
Middleton’s Allergy 7th Edition

Management of Cold Urticaria
• Avoidance• Cyproheptadine is the drug of choice• Non-sedating H1 antihistamine• For patient where IgE has a role,
monoclonal IgG anti-IgE may be effective
Middleton’s Allergy 7th Edition

Atopic dermatitis and skin disease High-dose desloratadine decreases wheal
volume and improves cold provocation thresholds compared with standard-dose treatment in patients with acquired cold urticaria
: A randomized, placebo-controlled, crossover study
Frank Siebenhaar, MD, Franziska Degener, MD,Torsten Zuberbier, MD, Peter Martus, PhD,andMarcus Maurer, MD Berlin, Germany
J Allergy Clin Immunol 2009;123:672-9

- Aim: assess the effects of 5 and 20 mg of desloratadine and placebo on cold-induced
urticarial reactions in patients with acquired
cold urticaria (safety & efficacy)
- A prospective, double-blind, randomized, placebo-controlled crossover study
J Allergy Clin Immunol 2009;123:672-9

• Materials & Methods - OPD of urticaria specialty clinic of the Allergie-Centrum-
Charite´ of the Charite´-Universita¨tsmedizin, Berlin, Germany
- Patients aged 18 to 75 years with a confirmed diagnosis of Acquired Cold Urticaria , made at least 6 week before
- Signs/symptoms were assessed by using the Acquired Cold Urticaria Severity Index (ACUSI), & triggering stimuli, previous medication use, and concomitant disease
J Allergy Clin Immunol 2009;123:672-9

J Allergy Clin Immunol 2009;123:672-9

J Allergy Clin Immunol 2009;123:672-9

J Allergy Clin Immunol 2009;123:672-9

J Allergy Clin Immunol 2009;123:672-9

B, Example of thermographic images of the cold-induced wheal response over 20 minutes in a patient with ACU treated with placebo, 5 mg/d and 20 mg/d desloratadine for 7 days
J Allergy Clin Immunol 2009;123:672-9

J Allergy Clin Immunol 2009;123:672-9

J Allergy Clin Immunol 2009;123:672-9

J Allergy Clin Immunol 2009;123:672-9

J Allergy Clin Immunol 2009;123:672-9

Conclusion
Treatment with desloratadine at doses of 5 and 20 mg daily significantly decreased wheal volume/size , improved CTTs & CSTTs in patients with ACU
Treatment with the higher dose of desloratadine yields higher outcomes in wheal volume and CTTs and CSTTs comparing with standard-dose desloratadine
J Allergy Clin Immunol 2009;123:672-9

Solar Urticaria Treated With Intravenous Immunoglobulins
HenriAdamski,MD, Christophe Bedane, MD, Annie Bonnevalle, MD, Pierre Thomas, MD, Jean-Louis Peyron, MD, Bernard Rouchouse, MD, Frederic Cambazard, MD, Michel Jeanmougin, MD,and Manuelle Viguier, MD Rennes, Limoges, Lille, Montpellier, Saint-Etienne, and Paris, France
J Am Acad Dermatol 2011;65:336-40

Solar urticaria treated with intravenous immunoglobulins
• To report the effectiveness of intravenous immunoglobulins (IVIG) in severe solar urticaria ( SU)
• A retrospective multicentric study via the mailing of a questionnaire to the French Photodermatology Units
• Severe SU was defined as having a poor response to antihistamine use and impairment of the quality of life (impact on daily and professional life)
• Collected age, sex, medical history, medications, clinical features, pho-tobiological characteristics, laboratory investiga-tions, and clinical response to IVIG
J Am Acad Dermatol 2011;65:336-40

Table 1 Characteristics of patients before receiving IVIG
J Am Acad Dermatol 2011;65:336-40

Table 1 Characteristics of patients before receiving IVIG
J Am Acad Dermatol 2011;65:336-40

J Am Acad Dermatol 2011;65:336-40

J Am Acad Dermatol 2011;65:336-40

Solar Urticaria
- A rare idiopathic photodermatosis- Sun avoidance and antihistamine - Severe solar urticaria needs more modality such as intravenous immunoglonulins- Further trials are needed

Thank You Very Much

![17466593 Physical Diagnosis Information Overview[1]](https://static.fdocuments.us/doc/165x107/577cc1ca1a28aba71193e3d1/17466593-physical-diagnosis-information-overview1.jpg)
![01 physical diagnosis [respiratory system] [pashto]](https://static.fdocuments.us/doc/165x107/5878b3f41a28ab724c8b6237/01-physical-diagnosis-respiratory-system-pashto.jpg)