CONTINUOUS MICRODIALYSIS OF BLOOD PROTEINS DURING ...
Transcript of CONTINUOUS MICRODIALYSIS OF BLOOD PROTEINS DURING ...

CONTINUOUS MICRODIALYSIS OF BLOOD PROTEINS DURING
CARDIOPULMONARY BYPASS
by
ALEXANDER FOK
A Thesis submitted to the
Graduate School – New Brunswick
Rutgers, The State University of New Jersey
And
The Graduate School of Biomedical Sciences
University of Medicine and Dentistry of New Jersey
in partial fulfillment of the requirements
for the degree of
Master of Science
Graduate Program in Biomedical Engineering
written under the direction of
Professor Jeffrey D. Zahn
and approved by
_____________________________________
_____________________________________
_____________________________________
_____________________________________
New Brunswick, New Jersey
October 2009

ii
ABSTRACT OF THE THESIS
Continuous Microdialysis of Blood Proteins During Cardiopulmonary Bypass
By Alexander Fok
Thesis Director: Jeffrey Zahn, PhD
Cardiopulmonary bypass is a procedure that temporarily substitutes a patients’
heart and lung functions with an extracorporeal heart-lung machine. This allows surgeons
to operate on motionless heart and lungs, while still providing the body with proper blood
circulation. However, the heart-lung machine has been shown to activate the body’s
systemic inflammatory response, resulting in short- and long- term organ dysfunction,
and even death. The severity of this inflammatory response is strongly correlated to the
production levels of specific cytokines and complements found in the bloodstream.
Current detection methods require taking discrete blood samples during surgery and
waiting at least several hours, but typically one to two weeks when including laboratory
queue times in hospitals, for results. I propose a microdialysis device that continuously
samples the patient’s blood for biomarkers during surgery. The primary function of this
device is to prepare a purified solution, with complement concentrations that closely
matches that of the patient’s bloodstream, to be used in a continuous microimmunoassay
device.
The microdialysis device was fabricated using photolithography and
softlithography techniques to create microfluidic channels and bonded to commercially
available semi-permeable membranes with biocompatible epoxy. The device was
designed based on computational simulations and fabrication constraints for optimal

iii
performance. It was tested for its analyte-recovery capabilities for complements C3a,
C4a, and C5a, in human blood continually circulating through a mock heart-lung
machine.
Two slightly different designs were tested, one using a membrane pore-diameter
of 0.1 µm and the other using 0.4 µm. Both devices operated at a perfusion flowrate of
4.1 µL/min, which is considered to be relatively fast for microdialysis probes. For the 0.1
µm pore membrane device, the relative recoveries were 79%, 75%, and 70% for C3a,
C4a, and C5a, respectively. For the 0.4 µm pore membrane device, the relative recoveries
were 112%, 135%, and 101% for C3a, C4a, and C5a, respectively. These findings show
promising results for the proposed microdialysis device, but further investigation is
needed to improve statistical significance.

iv
ACKNOWLEDGEMENTS
This work would not have been possible without the guidance of my advisor, Dr.
Jeffrey Zahn. His combination of technical expertise and creative ideas has shown me
what it takes to approach new problems and how to solve them. I will continue to use
these lessons in whatever career comes my way and in my own life.
I would also like to thank our collaborator, Dr. Akif Undar, who has supported
this project in many ways. His generosity and willingness to share his laboratory space
and resources at Hershey Medical Center was vital for conducting experiments.
I thank my committee members, Dr. David Schreiber and Dr. Li Cai, who were
also my instructors at Rutgers University, for broadening my knowledge in the
biomedical engineering field. Their dedication to helping students learn has been
influential to me.
To my friends and colleagues at Rutgers University, I thank them for creating a
supportive and positive learning environment. Special acknowledgements go to the
members of my lab, whom I also consider as friends: Mercedes Morales, Kiana Aran,
Larry Sasso, and Pantelis Athanasiou, who have provided immense support with my
research and life in general.
To the faculty and administrative staff of Rutgers’ Biomedical Engineering
Department, I would like to express my appreciation for their help, advice, and friendly
demeanor that made for a pleasant experience at Rutgers University.
Finally, to the most important people in my life, I would like to thank my parents
and my brother for their seemingly infinite love and support.

v
DEDICATION
To my family and friends for their love and support.

vi
TABLE OF CONTENTS
ABSTRACT OF THE THESIS ....................................................................................... ii
ACKNOWLEDGEMENTS ............................................................................................ iv
DEDICATION................................................................................................................... v
TABLE OF CONTENTS ................................................................................................ vi
LIST OF TABLES ........................................................................................................... ix
LIST OF ILLUSTRATIONS .......................................................................................... xi
Chapter 1 - Introduction .................................................................................................. 1
1.1 The Need for Microdialysis during CPB .............................................................. 1
Chapter 2 - Background ................................................................................................... 6
2.1 Cardiopulmonary Bypass Procedure .................................................................... 7
2.1.1 History of Development ................................................................................... 7
2.1.2 Main CPB Components ................................................................................... 9
2.1.2.1 Pumps......................................................................................................... 9
2.1.2.2 Oxygenators............................................................................................. 12
2.1.2.3 Heat Exchangers ..................................................................................... 13
2.1.3 Systemic Inflammatory Response ................................................................ 14
2.1.3.1 Inflammatory Cascade ........................................................................... 15
2.1.3.2 Complement System ............................................................................... 16
2.1.3.3 Red Blood Cell Damage.......................................................................... 18
2.1.3.4 Neutrophil and Vascular Endothelium................................................. 18
2.1.3.5 Organ Dysfunction.................................................................................. 20
2.1.3.6 Ischemia Reperfusion Injury ................................................................. 20

vii
2.2 Measuring Complement Components................................................................. 21
2.3 Microdialysis ......................................................................................................... 22
2.3.1 Development of microdialysis ....................................................................... 22
2.3.2 Basic Principles of Operation ....................................................................... 23
2.3.2.1 Perfusate .................................................................................................. 24
2.3.2.2 Membrane Material................................................................................ 25
2.3.3 Quantitative Microdialysis Models .............................................................. 27
2.3.4 Calibration Techniques ................................................................................. 28
2.3.4.1 Flowrate Method ..................................................................................... 29
2.3.4.2 No-net flux Method ................................................................................. 29
2.3.4.3 Retrodialysis ............................................................................................ 31
2.3.5 Microdialysis on a Chip................................................................................. 31
2.3.5.1 Methods for integrating membranes into devices................................ 33
Chapter 3 - On-chip Microdialysis System................................................................... 35
3.1 Theory .................................................................................................................... 35
3.1.1 Mass Transfer Prediction.............................................................................. 35
3.1.2 Fluid Pressure and Resistance ...................................................................... 38
3.2 Device Design and Fabrication ............................................................................ 40
3.2.1 General Design Considerations .................................................................... 40
3.2.1.1 First design: no bifurcation.................................................................... 43
3.2.1.2 Final Design: Bifurcating Tree .............................................................. 44
3.2.2 Photolithography and Soft Lithography...................................................... 46
3.2.3 Bonding to membrane ................................................................................... 49

viii
3.2.3.1 Thermal.................................................................................................... 49
3.2.3.2 Thin film deposition ................................................................................ 51
3.2.3.3 Epoxy Stamping ...................................................................................... 52
3.3 Numerical Studies - Electric Circuit Model ....................................................... 53
3.3.1 Observing Trends from Matlab Code.......................................................... 59
3.4 Microdialysis Experiments................................................................................... 67
3.4.1 Experimental Setup: Glucose and PBS........................................................ 68
3.4.2 Results and Discussion: Glucose and PBS ................................................... 70
3.4.3 Introduction: Blood with Mock CPB Circuit .............................................. 73
3.4.3.1 Experimental Setup: Blood with Mock CPB Circuit........................... 74
3.4.3.2 Results and Discussion: 0.1 µm membrane .......................................... 77
3.4.3.3 Results and Discussion: 0.4 µm membrane .......................................... 80
3.4.3.4 Time Course Data ................................................................................... 82
Chapter 4 - Conclusions and Future Work .................................................................. 86
Bibliography .................................................................................................................... 89
Appendix A: Preliminary Experiments ....................................................................... 95
Appendix B: Matlab Code........................................................................................... 100

ix
LIST OF TABLES
Table 1: Photolithography recipe for 30 micron thick Perfusion Channel ....................... 48
Table 2: Photolithography recipe for 130 micron thick Reservoir Channel ..................... 48
Table 3: Whatman Nucleopore Polycarbonate Track-etched Membranes ....................... 59
Table 4: Finalized Microdialysis Design for CPB integration.......................................... 67
Table 5: 100 nm membrane: p-values, pairwise t-test. Blue/bold values denote acceptance
of the null hypothesis. ........................................................................................... 80
Table 6: 100 nm membrane: correlation coefficient......................................................... 80
Table 7: 400 nm membrane: p-values, pairwise t-test. Blue/bold values denote acceptance
of the null hypothesis. ........................................................................................... 82
Table 8: 400 nm membrane: correlation coefficient......................................................... 82

x

xi
LIST OF ILLUSTRATIONS
Figure 1.1: A cardiopulmonary bypass machine being used during surgery [3] ................ 2
Figure 2. 1: The Gibbon type cardiopulmonary bypass machine first used in March 1955
by Kirklin’s team at the Mayo Clinic [1]................................................................ 9
Figure 2.2: Blood pump designs. (A) Two-roller, roller pump. The tubing sits on the
inner surface of the raceway. (B) Impeller pump with vanes connected to a
rotating shaft. (C) Centrifugal pump. The inner concentric cone rotates rapidly,
propelling blood radially outwards. [22] .............................................................. 10
Figure 2.A: Diagram of a hollow fiber membrane oxygenator and heat exchanger unit.
Blood flows through the heat exchanger, over temperature-controlled coils and
then enters the oxygenator, which is made up of woven strands of hollow fibers.
Oxygen flows from one end of the fiber to the other, supplying oxygen and
exchanging carbon dioxide with blood. [22] ........................................................ 13
Figure 2.B: Contact activation cascade systems that cause SIRS [26] ............................. 15
Figure 2.C: The three pathways of the complement system: Classical pathway,
Alternative pathway, and Lectin pathway [26]..................................................... 16
Figure 2.6: A cannula-based commercial microdialysis probe. The cannula tip is placed in
extracellular fluid or on bare tissue, where analytes diffuse across the membrane
and into the analyte-free perfusate solution. [64] ................................................. 24
Figure 2.D: Scanning electron micrographs of a polycarbonate hollow fiber: (a) cross-
sectional view; (b) outer surface; (c) cross-section under higher magnification.
[71]........................................................................................................................ 26

xii
Figure 2.E: No-net flux method. Net difference between the dialysate and perfusate
concentrations plotted against varying perfusate inlet concentration. The x-
intercept represents where the perfusate concentration is equal to the tissue
concentration. [67] ................................................................................................ 30
Figure 2.F: Graph showing an increasing interest in the microfluidics and membranes
field over the last 12 years. [Source: Rutgers University Libraries Searchlight,
with keywords: “microfluidics” and “membranes”]............................................. 32
Figure 3. 1: A side-view diagram showing the layer reservoir channels and the layer of
perfusion channels on opposite sides of a porous membrane [13] ....................... 36
Figure 3.2: Exploded view of the three main components (right to left): PDMS layer for
the reservoir channel, a thin polymer membrane, and a PDMS layer for the
perfusion channel. ................................................................................................. 40
Figure 3.3: Demonstrating how improperly aligned channels can affect the diffusion area.
Solid lines represent one layer of parallel channels and the dotted lines represent
the other layer. Left: proper alignment results in full overlap. Center: even a small
lateral shift can result in no overlap. Right: a small rotational shift can also reduce
overlap areas. ........................................................................................................ 42
Figure 3.4G: CFD analysis of the non-bifurcating channel design. Fluid enters from the
short channel on the left and exits on the right. Most of the flow goes through the
center channels, while the outer channel have negligible flowrates. .................... 44
Figure 3.5: Bifurcating channel design: a CFD analysis showing a surface plot of the
velocity field. Red denotes high velocity and blue denotes low velocity. At each

xiii
bifurcation stage, the flowrate splits up equally. This is only a partial model due to
computational constraints. .................................................................................... 45
Figure 3.6: Stacked view of the perfusion layer (blue) aligned on top of the reservoir
layer (red). The staggered design in the bifurcating tree section is intended to
minimize interaction between the two layers, except for the main section in the
center..................................................................................................................... 46
Figure 3.7H: Dark-field masks for photolithography. Left: Perfusion mask. Right:
Reservoir mask...................................................................................................... 47
Figure 3.8: Soft-lithography steps used to create microfluidic channels in PDMS.......... 47
Table 1: Photolithography recipe for 30 micron thick Perfusion Channel ....................... 48
Table 2: Photolithography recipe for 130 micron thick Reservoir Channel ..................... 48
Figure 3.10: Schematic for the epoxy stamping procedure. A) a small amount of epoxy is
placed on top of a clean glass slide; B) an object with a flat edge, such as another
glass slide, is used as a squeegee on the epoxy until a thin, uniform layer of epoxy
remains; C) the first PDMS layer is placed onto the thin layer of epoxy, with the
channel side facing down; D) and E) a membrane is placed on top of the epoxy-
side of the first PDMS layer; F) steps A-C are repeated for the second PDMS
layer and aligned with the first layer under a dissection microscope. .................. 53
Figure 3.11: A circuit diagram representing the microdialysis chip. The reservoir side is
given a voltage source to represent the pressure source given by the CPB pump.
The perfusate side is given a current source to represent the predetermined
flowrate put out by a syringe pump. Resistors represent hydrodynamic resistance,
which is a function of channel geometry and fluid viscosity................................ 55

xiv
Table 3: Whatman Nucleopore Polycarbonate Track-etched Membranes ....................... 59
Figure 3.12: Results from Matlab model: Perfusion flowrate recovery vs CPB Pressure,
for various pore sizes. ........................................................................................... 61
Figure 3.13: Results from Matlab model: Perfusion flowrate recovery vs Perfusion
flowrate, for various pore sizes............................................................................. 62
Figure 3.14: Results from Matlab model: Perfusion flowrate recovery vs Reservoir inlet
tubing length, for various pore sizes. .................................................................... 62
Figure 3.15: Results from Matlab model: Perfusion flowrate recovery vs CPB Pressure,
for various reservoir channel heights. ................................................................... 63
Figure 3.16: Results from Matlab model: Perfusion flowrate recovery vs Perfusion
flowrate, for various reservoir channel heights..................................................... 64
Figure 3.17: Results from Matlab model: Perfusion flowrate recovery vs Reservoir inlet
tubing length, for various reservoir channel heights............................................. 64
Figure 3.18: Results from Matlab model: Perfusion flowrate recovery vs CPB Pressure,
for various perfusion channel heights. .................................................................. 65
Figure 3.19: Results from Matlab model: Perfusion flowrate recovery vs Perfusion
flowrate, for various perfusion channel heights.................................................... 66
Figure 3.20: Results from Matlab model: Perfusion flowrate recovery vs Reservoir inlet
tubing lengths, for various perfusion channel heights. ......................................... 66
Table 4: Finalized Microdialysis Design for CPB integration.......................................... 67
Figure 3.21: A revised circuit diagram for the bench-top glucose/PBS experiments, based
off of Fig 3.11, where the reservoir channel is driven by a syringe pump, instead

xv
of a CPB pump. Thus, the reservoir inlet tubing resistance can be ignored and the
reservoir inlet is now represented with a current source....................................... 69
Figure 3.22: Theoretical (hollow) and experimental (solid) Volume Recovery values for
perfusion (diamond) and reservoir (square) outlets, versus varying reservoir
flowrates................................................................................................................ 71
Figure 3.23: Glucose concentration recovery for perfusion and reservoir channels, for
varying reservoir flowrates. Data shows that both channels end up with near-
identical concentrations for a wide range of flowrates, causing the data points to
overlap one another............................................................................................... 73
Figure 3.24: The setup for the mock CPB circuit experiments. A relatively small quantity
of blood flow is routed to the reservoir channel of the microdialysis device, via a
Luer connection at the sampling manifold on the arterial side of the oxygenator.76
Figure 3.25: Analyte concentration for the 0.1 µm membrane device: (left) C3a, (center)
C4a, and (right) C5a. Data represents an average of 6 data points over a 1.5 hour
period. A two-sample paired t-Test was performed, where H0 = two means are
equal. The asterisk (*) represents a statistical significance level, α<0.05. ........... 78
Figure 3.26: Relative recovery for the 0.1 µm membrane device: (left) C3a, (center) C4a,
and (right) C5a. Data represents an average of 6 data points over a 1.5 hour
period. The asterisk (*) represents a statistical significance level, α<0.05........... 79
Table 5: 100 nm membrane: p-values, pairwise t-test. Blue/bold values denote acceptance
of the null hypothesis. ........................................................................................... 80
Table 6: 100 nm membrane: correlation coefficient......................................................... 80

xvi
Figure 3.27: Analyte concentration for the 0.4 µm membrane device: (left) C3a, (center)
C4a, and (right) C5a. Data represents an average of 6 data points over a 1.5 hour
period. A two-sample paired t-Test was performed, where H0 = two means are
equal. The asterisk (*) represents a statistical significance level, α<0.05. ........... 81
Figure 3.28: Relative recovery for the 0.4 µm membrane device: (left) C3a, (center) C4a,
and (right) C5a. Data represents an average of 6 data points over a 1.5 hour
period. The asterisk (*) represents a statistical significance level. ....................... 81
Table 7: 400 nm membrane: p-values, pairwise t-test. Blue/bold values denote acceptance
of the null hypothesis. ........................................................................................... 82
Table 8: 400 nm membrane: correlation coefficient......................................................... 82
Figure 3. 29: Time course data with error bars representing 2 standard deviations for C3a.
............................................................................................................................... 84
Figure 3. 30: Time course data with error bars representing 2 standard deviations for C4a.
............................................................................................................................... 84
Figure 3.3 1: Time course data with error bars representing 2 standard deviations for C5a.
............................................................................................................................... 85
Figure A. 1: Various orientations of the channels: (left) reservoir channel is directly over
perfusion channel; (middle) reservoir channel is perpendicular to perfusion
channel; and (right) the two channels are offset laterally by one-half the channel
width. Arrows denote direction of flow. ............................................................... 95
Figure A. 2: Glucose recovery at the perfusion outlet shown in Fig. A.1 (left), “parallel”
configuration. ........................................................................................................ 96

xvii
Figure A. 3: Glucose recovery at the perfusion outlet shown in Fig. A.1 (middle), “cross”
configuration. ........................................................................................................ 98
Figure A. 4: Glucose recovery at the perfusion outlet shown in Fig. A.1 (right), “shifted
parallel” configuration. ......................................................................................... 99

1
Chapter 1 - Introduction
1.1 The Need for Microdialysis during CPB
Cardiopulmonary bypass (CPB) is a procedure where a patients’ heart and lung
functions are temporarily taken over by, what is commonly referred to as, an
extracorporeal “heart-lung machine” (Fig. 1.1) to maintain the circulation and
oxygenation of blood in the body. This procedure is usually necessary when a surgeon
needs to operate on a motionless heart or lung, such as when repairing internal heart
defects or heart valves [1], but can also be done on a beating heart, such as for minimally
invasive off-pump coronary artery bypass surgery [2]. The CPB circuit consists of:
pumps to circulate blood through the machine, an oxygenator to exchange carbon dioxide
with oxygen in the blood, filters to remove emboli and gas bubbles, ports to introduce
drugs such as the anticoagulant heparin and anesthesia agents, tubing to transport blood
from one part of the circuit to another, and cannulas to remove and deliver blood, to and
from, a patient’s circulatory system [1].

2
Figure 1.1: A cardiopulmonary bypass machine being used during surgery [3]
Although cardiac surgeries are usually life-saving procedures and the patient is
typically only on the CPB pump for several hours, a major disadvantage of using a heart-
lung machine is the damage it imposes on the circulating blood due to hemolysis [4, 5]
and a systemic inflammatory response [6, 7]. As blood circulates through various
components in the circuit, it can experience high shear stresses, and be exposed to
immunological-activating surfaces and endotoxins, all of which may induce a systemic
inflammatory response. As a result, short- or long-term multiple organ dysfunction, or
even death can occur [8-12].

3
Researchers are currently working on correlating the expected degree of organ
dysfunction with the degree of a patient’s inflammatory response, which is done by
measuring blood for levels of specific biomarkers such as complements. Since
complement levels may fluctuate during and even after surgery, multiple discrete blood
samples are taken between pre- and post-surgery and sent to a lab for analysis, which can
typically take several hours to perform (though results may not be available for days or
weeks, depending on laboratory queue time). Given the ability to monitor complement
levels continuously and in near real-time, surgeons may be able to prevent or limit organ
dysfunction by administering therapeutic drugs at times and doses tailored to individual
patients.
This thesis is based on previous work and advances made by Zahn’s group in the
field of microfluidics and microfabrication. Hsieh et al. developed an on-chip, continuous
microdialysis and glucose sensing device for the treatment of diabetic patients [13, 14].
This device incorporated a microdialysis device with in-line sensing electrodes to
continuously track concentration changes with impressive glucose recovery and sensing
capabilities. Yang et al. developed a microfluidic device that continuously separate
splasma from whole blood [15] and another device that continuously monitors blood
plasma proteins via fluorescence intensity detection using biotinylated FITC solution and
streptavidin-coated microbeads [16], both devices utilizing the Zweifach-Fung effect [17,
18].
In this work, a microdialysis chip capable of continuously dialyzing blood
proteins, while excluding cells, is presented. The device uses photolithography and
softlithography techniques to fabricate microfluidic channels on a biocompatible

4
polymer, and an epoxy stamping technique to directly bond two layers of microchannels
on opposite sides of a porous membrane. The porous membrane allows for small analytes
in blood, such as proteins, to cross the membrane into an analyte-free, isotonic solution
while preventing cells and large cellular fragments from crossing and contaminating the
aforementioned isotonic solution.
In Chapter 2, some background information about the invention, design, and
detrimental effects of the heart-lung machine (CPB pump) are discussed. The design of
these components, such as the oxygenator and blood pumps, has a significant impact on
the degree of a patient’s inflammatory response. Current microdialysis techniques are
also introduced here.
In Chapter 3, the methodology for designing the proposed microdialysis chip is
explained as well as the fabrication techniques used. Initial bench-top experiments were
performed using a saline solution doped with glucose, using the sugar molecule as the
analyte of interest, and an analyte-free saline solution as the perfusate. Glucose recovery
ranged from 91% to 95%, over a broad range of flowrates, despite large pressure gradient
changes across the membrane. Further experimentation was performed on a mock CPB
circuit using a full heart-lung machine setup but with several units of human blood in a
blood bag instead of using an actual patient. The concentration levels for complements
C3a, C4a, and C5a were measured at constant flowrate settings, over a period of 90
minutes, for a device using 0.1 µm pore diameter membrane and another using 0.4 µm
pore diameter membrane. Analyte recovery performance varied depending on the pore
size of the membrane as well as the specific complement being measured.

5
Finally, conclusions and future works are discussed in Chapter 4. Though
inconsistencies were observed, the overall results show a promising path for designing an
improved microdialysis system. Based on the evidence from the experiments, further
investigation is necessary to explain several inconsistent observations such as why
complement levels in blood samples from the CPB circuit were sometimes lower than
that of the recovered dialysate; and why the complement levels in the solution recovered
from the reservoir channel’s outlet were significantly lower than that of the blood flowing
in the CPB circuit. The system should then be incorporated into a microimmunoassay
chip, which would continuously measure analyte concentration directly on the chip itself.

6
Chapter 2 - Background
In this chapter, CPB, its development, usage, and physiological complications are
introduced. Studies have shown that the body induces systemic inflammatory responses
during cardiac surgery, especially when cardiopulmonary bypass is used [11, 19-32].
Although much time and effort have gone into developing each component of the CPB
machine, almost every component is still responsible for cell damage and immune
activation to some degree. Clinical evidence has shown a strong correlation between
specific inflammatory response levels with postoperative complications, such as organ
dysfunction, which can potentially lead to death. At present, studies are done by taking
blood samples from the patient pre-, during, and post-operation. Typically, concentration
levels are then analyzed via enzyme-linked immunosorbent assay (ELISA) or immuno-
fluorocytometry. By being able to monitor a patient’s inflammatory response in near-real-
time and continuously during CPB, doctors may one day be able to offer effective
treatments during surgery, or at least understand the syndrome and its causes better.

7
2.1 Cardiopulmonary Bypass Procedure
Today, over 400,000 open-heart operations are performed each year in the United
States [1]. Cardiopulmonary bypass is a procedure that replaces the function of the heart
and lungs during operations that require the patients’ own heart and lungs to be stopped.
A cardiopulmonary bypass pump (often referred to as heart-lung machine or mechanical
pump-oxygenator) is used to maintain the patient’s blood circulation, which keeps tissues
alive by providing nutrients and supplying oxygen to the blood while removing carbon
dioxide. This procedure is used on patients ranging from neonates to seniors and for
reasons ranging from heart-lung transplants to cardiac valve repair and/or replacement.
2.1.1 History of Development
During the 1930’s and 1940’s, prior to the invention of the heart-lung machine,
only simple extracardiac (outside of the heart) surgeries were possible. As doctors gained
experience and confidence from this, they began to expand into intracardiac surgeries,
where repairs are made inside the heart [1]. In order to support a patient’s life during this
more complex type of cardiac repair, surgeons had to somehow support the patient’s
blood circulation and blood-gas transfer. While several worldwide teams began to work
on mechanical pump-oxygenators, C. Walton Lillehei, at the University of Minnesota,
developed a controlled cross circulation procedure where another person’s oxygenated
blood (typically the patient’s parent) was cannulated from their femoral vessel and
pumped into the patient requiring cardiac repair [26]. Lillehei began clinical cases in
1954 and observed a 40% mortality rate (18 deaths out of 45 total cases) [33]. This
procedure also introduced potential risk to the donor. Nevertheless, the procedure was

8
seen as a success and many recommended abandoning further research into mechanical
CPB pumps.
John H. Gibbon, Jr. developed his CPB machine while working at Jefferson
Medical College in Philadelphia, PA, with partial financial support from Thomas J.
Watson, chairman of IBM. In 1952, Gibbon’s first attempt at using his mechanical pump
with a screen oxygenator was unsuccessful due to a fatal misdiagnosis of the one year old
patient’s condition [1]. Gibbon’s only success with his machine came in May 1953 for an
18 year old woman suffering from atrial septal defect (ASD). Gibbons made several more
unsuccessful cardiac surgical attempts, but the patients died and no further attempts were
made [1].
In 1952, John W. Kirklin gathered a team of experts in pathology, physiology,
cardiology, anesthesiology, and mechanical engineering at the Mayo Clinic to develop a
mechanical pump-oxygenator. Using the Gibbon-IBM machine’s blueprint as a starting
point, Kirklin modified and refined the design for 2½ years before its first use in 1955
(Fig. 2.1). In that year, a clinical series of open heart surgeries where Gibbon’s CPB
pump was used on 8 patients (aged between 4 months to 11 years old), where 4 died
postoperatively. Patients were under cardiopulmonary bypass for 20 to 73 minutes, with
blood flowrates of 100 ml/kg [34]. This pioneering effort led by the Mayo Clinic team,
brought forth a new era in intracardiac surgery.

9
Figure 2. 1: The Gibbon type cardiopulmonary bypass machine first used in March 1955 by
Kirklin’s team at the Mayo Clinic [1]
2.1.2 Main CPB Components
A modern-day CPB machine consists of two main components: the pump and the
oxygenator. Secondary components are tubing, which connects components from one
part of the circuit to another, and cannulae, which are tubes that connect to the patients’
veins and arteries. Each component has continually gone through design changes, with
the motive of minimizing physiological effects such as systemic inflammatory response,
hemolysis, and microembolisms.
2.1.2.1 Pumps
Performance characteristics that an ideal CPB pump should have are: 1) the
ability to pump blood at 7 l/min against a pressure of 500 mm Hg for an adult, 2) should
not cause damage to cellular or acellular blood components, 3) should not have dead

10
spaces where blood can stagnate or experience turbulent flow, 4) reproducible pump
flowrates, and 5) ability to be operated manually in case of power failure [26]. Roller
pumps and centrifugal pumps, as seen in Fig. 2.2, are the two most common types of
extracorporeal pumps currently used for blood perfusion.
For the last five decades, the roller pump has been the most commonly used type
for CPB, though recent improvements in centrifugal pumps have helped them gain
popularity. In a roller pump, a length of tubing is located alongside a curved raceway,
which is placed at the travel perimeter of rollers mounted on the ends of rotating arms.
The arms are oriented such that at least one roller pinches the tubing at all times. As the
roller begins to pinch the tubing at the beginning of the raceway, the volume of blood in
the tubing ahead of the pinched section is pushed forward. This action allows for
continuous blood flow, where flowrate is determined by the inside diameter of the tubing
and the speed of the rollers moving along the raceway. Although pumps with varying
amounts of rollers exist, a two-roller pump provides a relatively nonpulsatile flow
compared to a single-roller pump and causes less hemolysis than a multiple-roller pump.
Figure 2.2: Blood pump designs. (A) Two-roller, roller pump. The tubing sits on the inner surface of
the raceway. (B) Impeller pump with vanes connected to a rotating shaft. (C) Centrifugal pump. The
inner concentric cone rotates rapidly, propelling blood radially outwards. [22]

11
When using roller pumps, several complications can arise during an operation. If
a blockage occurs somewhere in the outflow end, pressure in the line can increase
progressively until a tubing or connector fails. If a blockage occurs somewhere in the
inflow end, a high negative pressure in the line can induce blood cavitation (the
production of microscopic air bubbles) or suction of room air through loose valves or
connections. Normal wear in the tubing, caused by the rollers, can create pinhole leaks,
where microscopic air bubbles can enter the line and head towards the patient [35]. In a
study by Stoney et al., line embolism from roller pumps were responsible for 92 deaths
and 61 permanent injuries between 1972 and 1977 [36].
Centrifugal pumps have already replaced roller pumps at many institutions. Its
basic design components consist of an impeller with a series of vanes or a stack of
smooth plastic cones inside a plastic housing. The impeller is either driven directly by a
shaft or indirectly by a magnetic coupling. Typically, fluid enters at the center of rotation.
Then, as the impeller rotates, the fluid is propelled radially outwards due to centrifugal
force, where it exits the pump. Unlike roller pumps, which rely on some amount of
occlusion (closure via pinching) in the tubing, centrifugal pumps are nonocclusive.
Because of this, the degree to which centrifugal pumps can experience extreme positive
or negative pressures are low, when compared to roller pumps. Therefore, the chances of
cavitation and microembolism issues are reduced [35]. Another major advantage is the
reduced risk of introducing macroscopic and microscopic air bubbles, possibly due to a
combination of shear force and positive pressure generation within the pump head [26].
Centrifugal pumps also suffer from several disadvantages. Due to the centrifugal
pump’s nonocclusive design, retrograde flow is possible when the pump stops or slows.

12
Also inherent to this design, even when the rotational speed is fixed, the flowrate can
change automatically when the systemic vascular resistance changes; therefore the
arterial outflow must be monitored with a flow probe.
Although both types of pumps mentioned have advantages and disadvantages, the
medical community has not been able to reach a unanimous opinion on which is
ultimately safer for patients. Some studies have shown less hemolysis with centrifugal
pumps versus roller pumps [37, 38], while others have shown contradictory results [39,
40] or no difference at all [41, 42].
2.1.2.2 Oxygenators
Oxygenators serve several purposes during CPB, besides oxygenating blood. It
acts as an entry point for anesthesia, and as a gas exchanger for oxygen, carbon dioxide,
and other gases. They also serve as a heat exchanger and blood filter. Because of the
natural lung’s complex and highly efficient structures of pulmonary alveoli and
capillaries, the artificial lung was one of the primary challenges for CPB designers.
Although several types of membrane oxygenators exist, the cross-current hollow
fiber membrane (Fig. 2.3) is most commonly used. The hollow polypropylene fibers have
pores of 1 µm in diameter that prevents both gas and blood from crossing the membrane.
Fresh air flows through the inside of bundles of hollow membrane fibers, while blood
flows perpendicularly outside of the fiber. The cross-flow design takes advantage of
secondary-flow that is induced by the fibers “tripping” fluid flowing past it, which
reduces the diffusion boundary layer and improves gas exchange.

13
Figure 2.A: Diagram of a hollow fiber membrane oxygenator and heat exchanger unit. Blood flows
through the heat exchanger, over temperature-controlled coils and then enters the oxygenator, which
is made up of woven strands of hollow fibers. Oxygen flows from one end of the fiber to the other,
supplying oxygen and exchanging carbon dioxide with blood. [22]
2.1.2.3 Heat Exchangers
Heat exchangers are coupled with the oxygenator and can either cool down or
warm up blood circulating through it. Typically, blood flows through spiraling coils made
of stainless steel or aluminum, which are submerged into circulating non-sterile water.
The inner walls of the coils are coated with polymers to limit blood-surface interactions.
The circulating water is chilled to nearly 0oC in an ice bath and heated by an electric
resistance coil to an absolute maximum of 42oC, at which point blood proteins begin to
denature [26]. Blood temperature plays a crucial role during CPB, as it can lead to serious
short- and long-term health issues for the patient.

14
Inducing hypothermia at the onset of CPB reduces the patient’s metabolism,
blood oxygen requirements, complement activation, and overall systemic inflammation
[1, 10, 43]. The blood is cooled as quickly as possible and is only limited by thermal and
fluid dynamics. Conversely, re-warming of the blood is performed at the end of the
procedure and its heating rate is carefully controlled to prevent blood damage, which can
ultimately lead to cerebral injury. Furthermore, overheating blood too quickly can
produce bubble formation due to the decrease in gas solubility, producing gaseous
microemboli.
2.1.3 Systemic Inflammatory Response
SIRS, an acronym for “systemic inflammatory response syndrome,” is a term
used to associate cardiopulmonary bypass with a wide range of ailments due to a “whole
body” inflammatory response such as pulmonary, renal, gut, central nervous system, and
myocardial dysfunctions; vasoconstriction; vasodilatation; hemolysis; leukocytosis; and
an increased risk to infections [11, 27, 28, 32, 35, 44]. Neither the severity of the
response nor the specific ailment(s) to occur, are predictable. However, the duration of
CPB, age, and complexity of the procedure are commonly regarded as risk factors [23,
27, 45, 46].
The origin of SIRS response can be attributed to the damage of cellular and
noncellular (humoral) components of blood, primarily caused by altered arterial blood
flow patterns and blood-surface contact within CPB components [26]. This can then
result in microemboli formation, hemostasis disruption, and most importantly, a chain-
reaction of cytokine-mediated and neutrophil-mediated inflammatory injury.

15
2.1.3.1 Inflammatory Cascade
The inflammatory cascade is primarily caused by the activation of factor XII, a
plasma protein, to factor XIIa, which triggers several inflammatory systems (Fig. 2.4). To
start, surface contact causes factor XII to undergo a conformational change and become
attached to high-molecular-weight kininogen [26]. This complex then adheres to the
foreign surface, undergoes limited proteolysis, then releases kallikrein, bradykinin, and
factor XIIa. A positive feedback system involving factor XIIa and kallikrein, which
activates neutrophils, can further activate the inflammatory cascade via production of
oxygen free radicals and proteolytic enzymes [26].
Figure 2.B: Contact activation cascade systems that cause SIRS [26]

16
2.1.3.2 Complement System
The complement system plays several key roles in the inflammatory process, such
as mediating inflammation, opsonization of antigenic particles, and damaging pathogen
membranes [26]. The product from a complement component interaction becomes the
enzyme for the next step, as shown in Fig. 2.5. The complement system cascade can be
triggered by just a small initial stimulus and result in massive amplification of the initial
activating event. Fortunately, this system is tightly controlled by regulatory molecules,
which makes up half the proteins in the complement system.
Figure 2.C: The three pathways of the complement system: Classical pathway, Alternative pathway,
and Lectin pathway [26]

17
There are two activation pathways in the complement system: the classical
pathway and alternative pathway. The classic pathway, which is the least important in
this discussion, is initiated when antibodies bind to target antigens on a surface. Its
cascade leads to the production of the classical pathway C3 convertase, C4b2b. This
convertase then cleaves C3, the central component of the system, into C3a and C3b
fragments. The alternative pathway has a feedback loop that begins at the C3b component
and leads to the generation of the alternative pathway C3 convertase, C3bBbP. This
convertase also cleaves C3 into its C3a and C3b fragments, where the C3b product can
then be re-initiated to the beginning of the alternative pathway. Although the spontaneous
activation of C3 occurs on a continuous basis, albeit at a low level, the triggering of the
full cascade can be prevented by cellular expression of regulatory proteins that inactivates
C3bBbP [26].
A third and final pathway in the complement system is the lectin pathway. This
pathway uses C3b, from either the classical or alternative pathway, to activate C5 to
produce C5a and C5b. C5a is a soluble molecule, while C5b binds to cell surfaces. As a
result, C6, C7, and C8 binds to the cell surface and C9 polymerizes to form a pore
through the cell membrane; thus resulting in a membrane attack complex (MAC) [26].
During CPB, activation of the complement system can be observed by monitoring
the consumption of components [47] and the presence of C3a and C5a in the circulation
[26]. Several factors have been shown to activate the cascade during CPB including:
surface biocompatibility, release of endotoxin into the system, and the breakdown of C3
caused by blood interaction with oxygen bubbles.

18
2.1.3.3 Red Blood Cell Damage
Red blood cells (RBCs) primarily damaged by shear stress have reduced
deformability due to mechanical damage [48]. Red blood cell deformability affects the
rheological properties of blood and is particularly important to maintain tissue
metabolism and oxygenation. Membrane damage also disrupts the normal function of
ionic pumps and causes an abnormal accumulation of cations within the cell [49]. The
membrane attack complex (MAC), generated during complement activation [11], attacks
the plasma membrane by forming pores, which allow free diffusion of molecules to pass
in and out of the cell. When enough pores are formed, hemolysis can occur. Death or
even damage to RBCs may be one reason for post-operative anemia frequently observed
in patients[50], as RBC damage shortens cell lifespan.
Besides anemia, RBC injury has a destructive effect at cellular, tissue, and organ
levels. An increase in plasma hemoglobin levels increases the plasma oncotic pressure
and viscosity, which is detrimental to tissue function. The auto-oxidation of hemoglobin
releases cytotoxic oxygen free radicals. Potassium released from RBCs and into
extracellular fluid may impair cardiac conduction and cause arrhythmias. Fragments of
RBC lipid membranes can also block microcirculations (arterioles, capillaries, and
venules) and cause organ dysfunction.
2.1.3.4 Neutrophil and Vascular Endothelium
Neutrophils make up most of the leukocytes in the body and are essential against
fighting infections and foreign materials. On the other hand, activated vascular
endothelium triggers neutrophil activation when the two come into contact, resulting in

19
much of the SIRS maladies. CPB circulation triggers a humoral cascade that leads to the
activation of the vascular endothelium. Neutrophil activation occurs via IL-8, C5a, or
platelet activation factor (PAF) to express adhesion molecules on its surface, causing the
activated neutrophils to adhere to activated endothelium. At this stage, cytotoxic
proteases and oxygen-derived free radicals are released by the neutrophils, causing some
of the post-CPB end-organ damage [26].
Under normal physiological circumstances, the vascular endothelium is relatively
inert and allows blood to circulate freely. Inflammatory signals (such as complement
activation products, oxygen-derived free radicals, and cytokines) cause the endothelial
cells to change their gene expression, prompting the release of cytokines and protein
expressions, which leads to inflammatory reactions and thrombosis [19, 51]. Typically,
endothelial activation occurs at a local site, where neutrophil recruitment and coagulation
can occur to contain the local infection. However, cytokines released during CPB causes
this reaction to occur on a systemic level. As a result, large areas of endothelium are
activated, followed by large scale neutrophil activation, adhesion, and release of
cytotoxic proteases and oxygen-derived free radicals. The body’s feedback mechanism
that is normally able to cope with attenuating the response at a local level is not able to
cope proportionately at a systemic level. End-organ damage, microemboli, and clotting
factor depletion are contributing factors to coagulopathy (clotting disorder) complications
after open-heart surgery [24, 25, 52, 53]. Neutrophil-endothelium adhesion can cause
capillaries to become blocked, causing local ischemia [20]. Finally, cytotoxic products
released by activated neutrophils can damage cells directly.

20
2.1.3.5 Organ Dysfunction
Organs that are affected by CPB may include: the lung and pulmonary circulation,
kidneys, brain, and gut. At the end of CPB, the entire cardiac output is sent to the
pulmonary circulation, which will be exposed to a large number of activated cells passing
through. Studies have shown that activated neutrophils are more likely to become lodged
in the pulmonary circulation [54, 55] and release free radicals that cause lung injury.
Studies have shown that intravenous injection of oxygen radical scavengers, such as
superoxide dismutase or catalase, can attenuate pulmonary damage [56]. Renal function
is reduced by the effects of (CPB-induced) hypothermia, which increases vascular
resistance and vasoconstriction. To remedy this during CPB, hemodilution is used to
improve plasma flow and help prevent renal injury [31]. Blood cell aggregates
(microemboli) can cause brain swelling and lead to postoperative cerebral dysfunction
[57].
2.1.3.6 Ischemia Reperfusion Injury
During an on-pump open heart surgery, where the heart is intentionally stopped
and isolated from blood circulation via an aortic cross-clamp, the heart tissue is damaged
due to the lack of oxygen and nutrients, and inability to remove metabolic waste [26].
However, further injury is incurred when blood flow is reintroduced, towards the end of
surgery; this is known as ischemia reperfusion injury. Several mechanisms of reperfusion
injury exist, including: oxidative stress, where the oxygen in the returned blood exposes
cells to damaging oxygen free radicals; neutrophil activation, partially caused by blood
contact with extracorporeal surfaces; and activation of the complement cascade, primarily

21
through the alternative pathway, which produces complement fragments (such as C3a and
C5a) that further activates neutrophils [58]. Examples of reperfusion injury include
myocardial necrosis, endothelial dysfunction, and apoptosis [26]. By monitoring the
levels of specific biomarkers such as complement fragments in circulating blood, it
would be possible to finely tuned doses of complement pathway inhibitors to counteract
the inflammatory response in near-real-time.
2.2 Measuring Complement Components
Immunoassay techniques used in hospitals today (such as radioimmunoassay,
enzyme-linked immunosorbent assay, or cytometric bead assay kit) involve machines that
are typically cumbersome and expensive to operate. Multiple sample-preparation steps
are required from the end-user, especially if the sample contains whole blood. Blood
samples must be collected in tubes and kept on ice until it is ready to be centrifuged at
4oC, at which point, the separated plasma is extracted and frozen at -70
oC [59, 60]. The
centrifuging process removes red blood cells, leukocytes, platelets, and other debris from
plasma since there is evidence that shows blood stored at 4oC contributes to complement
activation via the classical or alternate pathway [61]. Another contributing factor via the
alternate pathway has been reported to be a result of blood contacting plastic surfaces
during storage [62]. As one can see, careful steps must be taken to ensure validity of the
samples such that there is no change in complement concentration from the time at which
they were collected.

22
2.3 Microdialysis
Microdialysis sampling is a technique used to collect analytes from extracellular
fluid (ECF) for analysis. The primary component of all microdialysis devices is its semi-
porous membrane that is placed in between ECF and perfusion fluid. Substances travel
from areas of higher concentration to lower concentration. Small analytes from the ECF
(such as proteins, peptides, and other chemicals) diffuse through the membrane pores and
into the perfusate while large particles (such as cells, platelets, large proteins, etc.) are
excluded. In other words, the device provides “clean” samples to make chemical analysis
easier or even possible.
2.3.1 Development of microdialysis
Microdialysis sampling began as a means to measure the chemical composition
from rodent brain in real-time. By placing a microdialysis probe at specific target sites
instead of using a needle to draw blood samples from the bloodstream, it provides both
temporal and spatial references to the data. Today, it is used essentially on every organ
for applications ranging from endocrinology, immunology, metabolism, and
pharmacokinetics, though a vast majority of biomedical literature has focused in
neuroscience [63]. However, more and more life scientists are realizing the potential uses
for microdialysis sampling beyond neuroscience.

23
2.3.2 Basic Principles of Operation
Currently, microdialysis sampling devices most commonly exist in the form of a
microdialysis probe located at the tip of two concentric cannulae (the “inner” cannula and
“outer” cannula) (Fig. 2.6). Depending on the organ’s fragility, the cannulae can be made
out of rigid or flexible materials. The perfusion fluid (“perfusate”) flows down the
interior of the inner cannula, where it exits the tip of the inner cannula, and then flows
upwards (away from the tip) in between the outer and inner cannulae. At the probe end, a
section of the outer cannula is made of a semipermeable membrane and is the region that
comes into direct contact with the tissue site or fluid-filled space. Analytes from the
probe’s exterior diffuse across the membrane and into the perfusion fluid (referred to as
the “dialysate”), where it then exits the microdialysis device to be collected or analyzed
further downstream.

24
Figure 2.6: A cannula-based commercial microdialysis probe. The cannula tip is placed in
extracellular fluid or on bare tissue, where analytes diffuse across the membrane and into the
analyte-free perfusate solution. [64]
2.3.2.1 Perfusate
The particular perfusate solution is chosen carefully to match the ionic and
osmotic strength of the ECF, which helps maintains fluid and ion balance across the
membrane. An improperly balanced osmotic pressure across the membrane can cause
perfusion fluid to be gained or lost, thereby affecting the analyte concentration to be
measured as well as the normal physiological environment. An improperly balanced
ionic gradient across the membrane can also damage sensitive organs such as the brain.
For these reasons, a form of Ringer’s solution is used as the perfusate and typically
contains 150 mM NaCl, 4 mM KCl, and 2.4 mM CaCl2. The solution can also be

25
supplemented with glucose and ionic salts [64]. If properly balanced, the primary mode
of transport is diffusion, driven by the analytes’ concentration gradients.
2.3.2.2 Membrane Material
The same semipermeable porous hollow fiber membranes used in kidney dialysis
is also used in microdialysis probes (Fig. 2.7). Until recently, membranes were only able
to recover low-molecular mass mediators, metabolites, and xenobiotics. With the current
availability of high molecular weight cutoff (MWCO) membranes, larger molecules such
as plasma proteins, complements, and growth factors can now be recovered as well [65].
Commonly used materials include polycarbonate/polyether blends (PC), polyethersulfone
(PES), polyacrylonitrile (PAN), and cuprophan (CUP), and can have MWCO ranging
from 5 kDa to 100 kDa. Due to its manufacturing process, porous hollow fiber
membranes are made up of a range of pore sizes and its pore size distribution can be wide
or narrow. The manufacturers typically define MWCO as the absolute maximum
molecular weight by which anything greater is rejected but only a small fraction of
molecules at or near that molecular weight will pass through (typically significantly less
than 1%). As another example, a 10 kDa protein crossing a commercial 100 kDa MWCO
membrane at a perfusion flowrate of 1 µl/min typically has a relative recovery below 5%
[66], where relative recovery is simplified to be defined as the ratio of concentration
“recovered” at the perfusion outlet to the concentration at the target site. A more in-depth
explanation of this term is given in the next section.
A common problem associated with large MWCO membranes during
microdialysis is ultrafiltration. Ultrafiltration occurs when the perfusate side of the

26
membrane is over-pressured, driving a convective flow of perfusion fluid through the
pores and out of the probe. This is seen more commonly in large MWCO because of the
inherently lower hydraulic resistance in the pores. If observed, the perfusion flow rate
should be decreased since ultrafiltration dilutes analyte concentration in the tissue.
A membrane’s MWCO cannot be relied upon as a good predictor for recovery
performance during microdialysis [67]. The interaction between membrane material
(“chemistry”) and a particular analyte can also affect performance. For example,
hydrophobic analytes are difficult to recover [68, 69], with little exception [65], and
negatively charged analytes are typically rejected by negatively charged membrane
materials such as polyacrylonitrile [70].
Figure 2.D: Scanning electron micrographs of a polycarbonate hollow fiber: (a) cross-sectional view;
(b) outer surface; (c) cross-section under higher magnification. [71]

27
2.3.3 Quantitative Microdialysis Models
The microdialysis extraction fraction, Ed, or relative recovery, of a probe-styled
microdialysis setup is defined as:
Recovery = Ed in
inout
CC
CC
−
−=
∞
Equation 2.1
where Cin, Cout, and C∞ are the concentrations for the analyte of interest in the inflow
perfusate, outflow dialysate, and the tissue/fluid surrounding the probe, respectively. The
perfusate flowing into the probe is normally devoid of the analyte of interest (Cin equals
zero) and thus the equation can be simplified to:
Recovery = Ed ∞
=C
Cout Equation 2.2
In other words, the recovery term is a measure of how efficient the microdialysis probe
(perfusate) is able to represent the analyte concentration in the tissue or solution.
Bungay et al. developed a steady-state mathematical model [72, 73] to calculate
the expected microdialysis extraction fraction, Ed, from a constant concentration
stationary ECF, given by:
Ed
++−−=
−
−=
∞ )(
1exp1
emddin
inout
RRRQCC
CC Equation 2.3
where Qd is the perfusion flow rate and Rd, Rm, and Re are the dialysate, membrane, and
external medium resistances, respectively. Analytes sequentially diffuse across a region
of the external medium, then the membrane, and finally through to the dialysate in order
to exit the microdialysis probe. Since these resistances are in series and mass transfer
flow is conserved (i.e. equivalent) across the three regions, the resistances are additive.
Eq. 2.3 assumes that the transmembrane pressure is sufficiently small and that there is no

28
convective fluid flow through the membrane; that is, mass transport is primarily due to
diffusion across a concentration gradient [13].
Jacobson et al. developed an empirical model [74] that related microdialysis
extraction with the perfusion flowrate, active area of the membrane, and the mass transfer
coefficient. The resulting equation is:
)/exp(1 0 d
out QAKC
C−−=
∞
Equation 2.4
where K0 is the analyte-specific mass transfer coefficient for the membrane, A is the
active area of the microdialysis membrane, and the remaining terms are described
previously. Extrapolating this equation to the case of zero flowrate reveals that Cout is
expected to equal C∞, i.e., resulting in full recovery of the analyte. The product (-K0A) is
equivalent to resistance terms, 1/( Rd + Rm + Re), from Eq. 2.3, and the entire expression
is equivalent to Bungay’s expression for Ed in Eq. 2.3. Jacobson’s group realized that
different amino acids, even with similar molecular weights, exhibited different in vivo
mass transport coefficients. Therefore, for most cases, K0 values must be determined
experimentally for each analyte-membrane combination.
2.3.4 Calibration Techniques
Obtaining the true interstitial concentration of an analyte (i.e. 100% extraction
efficiency) via microdialysis is difficult with today’s microdialysis probes, as it requires
the perfusion flowrate to be extremely low. Typical sampling flowrates range between
0.5 and 2.0 µl/min [63] and even then, the dialysate will typically have an Ed of less than
30% at 0.5 µl/min and less than 20% at 1.0 µl/min for in vitro recovery of cytokines [75].

29
Operating at even lower flowrates increases the sample collection time significantly,
since there is always some minimum volume of sample required for analysis. Calibration
techniques allow for a more practical means of estimating what the true ECF
concentration is. Several approaches exist to approximate the true concentration, each
with their own limitations.
2.3.4.1 Flowrate Method
Jacobson et al. developed a calibration technique [74] known as the flowrate
method, or the mass transfer method, where the perfusion flowrate is decreased gradually
while changes in the dialysate concentrations are measured. At low flowrates, the change
in dialysate concentration plateaus. By applying appropriate nonlinear regression analysis
on this data, the concentration can be extrapolated for the zero flowrate condition, which
can be approximated to be the true tissue concentration value. However, this method is
not very accurate. Accuracy improves as lower and lower flowrates are used but this
incurs the problem of long collection periods as described earlier.
2.3.4.2 No-net flux Method
Unlike the previous method which uses analyte-free perfusate, another method for
calibrating the microdialysis probe involves perfusing known concentrations of the
analyte of interest into the probe at a specific flowrate and then measuring the dialysate
concentration that comes out (i.e. measuring before and after dialysis). This is known as
the no-net flux method, or equilibrium dialysis, and was first conceived by Lonnroth et al

30
in 1987 [76]. The left hand side of Eq. 2.3 is assumed to be an unknown value P since
neither the perfusion flowrate nor the resistances change. Thus it can be rearranged as
( )∞−−=− CCPCC ininout Equation 2.5
where P is the proportion of analyte transport to and from the probe. The net difference
between the dialysate concentration and perfusate concentration (Cout - Cin) is plotted as a
function of varying perfusate concentrations (Fig. 2.8). Then, a simple linear regression
analysis is performed. Whether the analyte ultimately diffuses into or out of the probe is
assumed to be solely due to the concentration gradient between what is added to the
perfusate and the tissue concentration itself. Theoretically, when the net difference (Cout -
Cin) is zero, it implies that the perfusate concentration is equal to the tissue concentration,
which is represented by x-intercept of the plot. This data from this technique is relatively
simple to analyze and does not necessarily require the use of slow perfusion flowrates
[73, 77].
Figure 2.E: No-net flux method. Net difference between the dialysate and perfusate concentrations
plotted against varying perfusate inlet concentration. The x-intercept represents where the perfusate
concentration is equal to the tissue concentration. [67]

31
2.3.4.3 Retrodialysis
The retrodialysis technique determines Ed by measuring the loss of an analyte
from the perfusate [78, 79]. The perfusate is doped with an analyte of known
concentration of at least ten times that of the tissue concentration surrounding the probe
[67]. For this method, it is necessary to dope the perfusate with an analyte that has very
similar diffusion characteristics as the analyte of interest. Usually, a radiolabled version
of the analyte of interest is used. High concentrations in the perfusate are required to
ensure that the radio-labeled analyte crossing the membrane (from perfusate-side to
tissue-side) is not limited by the concentration of unlabeled analyte (on the tissue-side),
regardless of the concentration on the tissue side of the membrane [77]. By this
assumption, C∞ is negligible compared to the known Cin and the extraction fraction can
be determined by
in
outin
dC
CCE
−= Equation 2.6
However, extremely high concentrations of radiolabled analyte in the perfusate tend to
make the membrane the diffusion-limiting site, and thus, should be avoided [80, 81].
2.3.5 Microdialysis on a Chip
Micrometer-scale total analysis systems (µTAS) are becoming more than just a
novel research concept and beginning to be considered an important tool to improve
global health. Also known as ‘lab-on-a-chip’ devices because of their likeness in size and
similar fabrication processes with computer microprocessors, they are used in diverse
applications such as biochemical assays, polymerase chain reactions, and blood sample

32
separation. Some advantages that microdevices offer include smaller volumes of reagents
and potentially hazardous wastes, reduced cost, portability, and speed of analysis. The
broad field of microfluidics has seen incredible advances in the last 20 years [82]
although the very first µTAS, a micro gas chromatograph, was developed at Stanford
University in the 1970s [83]. In particular, microfluidic devices using membranes for
mass transport control have been garnering increasing amounts of interest over the past
10 years, as illustrated in Fig. 2.9. Some µTAS applications involving membranes
include separation, purification, sample pre-treatment, and dialysis [84].
0
25
50
75
100
125
150
175
200
1996
1997
1998
1999
2000
2001
2002
2003
2004
2005
2006
2007
2008
# articles with "microfluidics"
and "membranes" as keywords
Figure 2.F: Graph showing an increasing interest in the microfluidics and membranes field over the
last 12 years. [Source: Rutgers University Libraries Searchlight, with keywords: “microfluidics” and
“membranes”]

33
2.3.5.1 Methods for integrating membranes into devices
There are several basic fabrication techniques to incorporate membranes into
µTAS devices: membrane preparation during chip fabrication process, in situ preparation
of membranes, and directly incorporating (commercial) membranes. Each method offers
a series of advantages and disadvantages; ultimately, the decision depends on one’s
priorities for cost, ease of fabrication, MWCO control, and chemical compatibility.
One approach is to fabricate the membrane during the fabrication process of the
chip. That is, the pores are created directly on the microfluidic chip itself. Many
semiconductor microfabrication techniques are available to create pores in silicon wafers
such as electrochemical etching [85], back etching [86], and ion beam track etching [87].
Some major advantages with using clean room technology include: using well established
and understood semiconductor processes, excellent control of feature size (to the order of
tens of nanometers), ability to make tailor-made structures, and avoiding sealing issues
altogether. In fact, in most cases, there is no sealing process because the membrane is
created as part of the chip substrate itself [84]. However, just like most other uses of
semiconductor technologies, the production process is complex and expensive.
Another approach for integrating membranes is to fabricate them in situ on a pre-
made microfluidic chip. Several variations for this method exist but usually involve
selective polymerization. Polymerization of acrylate monomers occurs via UV light
exposure, where the position and thickness of the membrane can be controlled simply by
controlling where UV light hits [88]. Non-polymerized monomers are washed out
afterwards. MWCO properties can vary depending on the ratio of monomer and cross-
linking agent used, but ultimately requires trial and error experiments and educated

34
guesses for tailored specifications. The range of applicable materials is also very limited.
Membranes can also form via interfacial polymerization at the interface between two
solutions, as demonstrated by Kitamori et al. [89]. In this case, a thin polyamide
membrane was created at the interface of an organic and an aqueous solution, both
containing a certain monomer that reacts via a poly-condensation reaction to form. Again,
there is only a limited range of membrane materials.
Lastly, in-house or commercial membranes can be directly incorporated into
microfluidic devices by clamping or gluing the membrane between two microfluidic
chips; it is also the most straight-forward of the options. Commercial membranes are sold
as flat sheets and come in varying materials, sizes, and MWCOs and may undergo
surface modification to functionalize the membrane with trypsin [90] or bovine serum
albumin [91], for example. The clamping method offers flexible configurations because it
is possible to swap in/out different types of membranes depending on the application.
However, creating a good seal can be difficult. When clamping hard substrates such as
silicon and glass, the two surfaces that contact the membrane must have a high degree of
flatness and even pressure must be applied to prevent leaking. Also, capillary forces can
cause glue to get sucked into and block microfluidic channels and membrane pores.
In this thesis, a microdialysis chip intended for continuous dialysis of blood
proteins during cardiopulmonary bypass procedures is presented. The device sandwiches
a commercial membrane between two microfluidic chips and bonded with epoxy for cost
savings and ease of manufacturability. The microdialysis chip is designed with high
throughput, extraction efficiency, and robustness in mind.

35
Chapter 3 - On-chip Microdialysis System
In this chapter, a microdialysis chip is developed for continuous blood protein
extraction for, but not limited to, CPB operations. The fabrication steps are based on
semiconductor technology and soft lithography, both of which will be discussed in detail.
3.1 Theory
Fluid dynamics and mass transport theories are used to predict and explain the
performance of the microdialysis device. Optimization of overall device performance
remains a difficult task since the ‘device performance’ is actually made up of a multitude
of factors. Changing an operating parameter one way may be favorable for one factor but
adversely affect another factor.
3.1.1 Mass Transfer Prediction
In the proposed microdialysis chip, there are two flows separated by a
semipermeable membrane (Fig. 3.1) and is intended for in vitro use. Blood flows through
the reservoir channel while a saline solution flows through the perfusate channel.
Analytes in the reservoir fluid are dialyzed across the membrane, into the perfusion fluid.

36
Figure 3. 1: A side-view diagram showing the layer reservoir channels and the layer of perfusion
channels on opposite sides of a porous membrane [13]
The mass transfer coefficient, K0, is assumed to be constant over the diffusion path and
over time. The convective mass flux across the reservoir channel is given by
rrdCQmd −=& Equation 3.1
where Qr is the flowrate through the reservoir channel and Cr is the analyte concentration
in the reservoir solution. Rearranging Eq. 3.1 yields
r
rQ
mddC
&−= Equation 3.2
The convective mass flux of the perfusate is given by
dddCQmd −=& Equation 3.3
and another rearrangement yields
d
dQ
mddC
&−= Equation 3.4

37
where Qd is the flowrate through the perfusion channel and Cd is the analyte
concentration in the perfusate solution.
The mass flux across the membrane can also be given as
( )dACCKmd dr −= 0& Equation 3.5
where K0 is the membrane’s overall mass transfer coefficient (also referred to as the
membrane’s molecular permeability) and A is the diffusional area. By subtracting Eq. 3.4
from Eq. 3.2,
+−=−−=−
drdr
drQQ
mdQ
md
Q
mddCdC
11&
&& Equation 3.6
By substituting Eq. 3.5 into Eq. 3.6,
( ) ( ) dAQQ
CCKCCddr
drdr
+−−=−
110 Equation 3.7
Eq. 3.7 can then be rearranged into
( )( )
dAQQ
KCC
CCd
drdr
dr
+−=
−
− 110 Equation 3.8
By integrating Eq. 3.8 along the membrane diffusional area, Am
+−=
−
−
dr
m
indinr
outdoutr
QQAK
CC
CC 11ln 0
,,
,, Equation 3.9
where Cr,out and Cr,in are the outlet and inlet concentrations of the reservoir channel. Cd,out
and Cd,in are the outlet and inlet concentrations of the perfusion channel. Am is the
diffusional surface area. Qr and Qd are the flowrates through the reservoir and dialysate
channels. Cd,in is always zero for this work; that is, a saline solution, free of the analyte of
interest, enters the perfusion channel of the device. Cr,in and Cr,out are assumed to be
equals since the reservoir flowrate, Qr, is much greater than the perfusion flowrate, Qd. In

38
other words, the amount of analytes diffusing out of the reservoir solution is negligible
because it is constantly being replenished with more reservoir solution. Also, because Qr
is much greater than Qd, the fraction 1/Qr in Eq. 3.9 can be ignored. Therefore, Eq. 3.9 is
simplified to
−=
−
∞ QAK
C
Cm
out 11ln 0 Equation 3.10
where Cout is the dialysate concentration, C∞ is the reservoir concentration, and Q is the
perfusion flowrate. Eq. 3.10 can be rearranged to represent the extraction efficiency (also
known as “relative recovery”) as a function of perfusion flowrate
Q
AK
out
d
m
eC
CE
0
1−
∞
−== Equation 3.11
where a high extraction efficiency is achieved when (K0Am) >> Q.
3.1.2 Fluid Pressure and Resistance
Balancing the hydraulic pressures in the dual-compartment microdialysis system
is important to ensure that diffusion is the primary mode of mass/analyte transport,
instead of convection. If the hydraulic pressure in the reservoir channel is much greater
than that of the perfusion channel, the dialysate concentration will increase by having
blood plasma cross the membrane and enter the perfusion channel. However, this may
also cause large particles in the reservoir solution, mainly blood cells, to become lodged
or lyse as it tries to squeeze into the pores. On the other hand, if the hydraulic pressure in
the perfusion channel is much greater than that of the reservoir channel, perfusate may

39
flow across the membrane, thereby diluting the reservoir solution and reducing the
dialysate sample volume.
The pressure drop for a viscous incompressible fluid flowing through a constant
cross-section is a function of the channel geometry and flowrate, which is given by,
QRP =∆ Equation 3.12
where ∆P is the pressure drop, Q is the fluid flowrate, and R is the geometric resistance
term.
For a rectangular channel, the resistance term is given by
1
,...5,3,1553 2
tanh1192
112
−∞
=
−= ∑n
rectH
Wn
nW
H
WH
LR
ππ
µ Equation 3.13
where µ is the fluid dynamic viscosity, L is the length of the channel, W is the length of
the long edge of the channel cross-section, and H is the length of the short edge of the
channel cross-section. For square, channels, W and H are equivalent.
For a circular channel, such as the cylindrical pores of the membranes or tubing,
the resistance term is given by
4
8
r
LRcirc π
µ= Equation 3.14
where r is the radius of the channel and L is the thickness of the membrane or length of
tubing.

40
3.2 Device Design and Fabrication
The microdialysis chip made up of three main components: a
polydimethylsiloxane (PDMS) layer for the reservoir channel, another PDMS layer for
the perfusion channel, and a polymer track-etch membrane (with either 100 or 400 nm
diameter pores) bonded in between (Fig. 3.2). The design and fabrication protocol created
for this thesis are a result of a series of many developmental iterations.
Figure 3.2: Exploded view of the three main components (right to left): PDMS layer for the reservoir
channel, a thin polymer membrane, and a PDMS layer for the perfusion channel.
3.2.1 General Design Considerations
According to Eq. 3.11, maximizing the diffusion area increases the extraction
efficiency. It is also important to consider the size of the overall device for ease of
manufacturing and to maintain the µTAS form factor. Using these constraints,
commercial track-etched membranes, 47 mm in diameter, were selected. The size of the

41
perfusion and reservoir channels were designed to maximize the diffusion area while
fitting within the membrane’s perimeter.
Instead of using a single-channel design, where the one channel would be several
millimeters wide, a multiple parallel-channel design has two main advantages: 1)
increased rigidity of the device, which is important because PDMS is very soft and
flexible, and 2) provides structural support for the fragile, thin membrane (~10 µm thick).
However, one must also consider the adverse affects of reducing channel width for the
sake of having multiple parallel channels, such as increasing hydraulic resistance and
shear stress. Since the perfusion flow is driven by a syringe pump, i.e. flowrate-
controlled, a large hydraulic resistance increases the pressure drop in the channel and
increases the chance for PDMS-membrane delamination. Also, high shear stresses are
known to cause cell lysis as well as platelet activation.
To ensure consistent and repeatable results from the microdialysis chip, the
perfusion channel and reservoir channel PDMS layers must be properly aligned with
respect to one another, so that the diffusion area does not vary from one produced device
to another (Fig. 3.3). The diffusion area is defined as areas where the perfusion channels
and reservoir channels overlap. Since each channel is only several hundred microns wide,
extra care must be taken in the alignment and bonding process. Small lateral
misalignments and/or rotational misalignments can reduce the diffusion area quite
drastically.

42
Figure 3.3: Demonstrating how improperly aligned channels can affect the diffusion area. Solid lines
represent one layer of parallel channels and the dotted lines represent the other layer. Left: proper
alignment results in full overlap. Center: even a small lateral shift can result in no overlap. Right: a
small rotational shift can also reduce overlap areas.
To overcome this problem, the reservoir channels are designed to be slightly
wider than the perfusion channels, making the alignment and bonding process more
forgiving. There are several advantages for making the reservoir channel width wider
than the perfusion channel: 1) the reservoir solution, blood, is sensitive to high shear
stresses, which is reduced by widening the channel, 2) the reservoir flowrate can increase
to further satisfy the Qr >> Qd assumption in Eq. 3.10, and 3) if the perfusion channel is
wider than the reservoir channel, diffusion becomes limited by the reservoir channel’s
width.

43
3.2.1.1 First design: no bifurcation
The first channel design consisted of a short inlet channel that led directly to a
series of parallel channels. A computational fluid dynamics (CFD) analysis (COMSOL
Inc., Burlington, MA) showed that the flow velocity is highest in the center channels and
quickly decreases for channels farther away, as shown the velocity field contour plot in
Fig. 3.4, where red denotes high velocity and blue denotes low velocity. Predicting
device performance is made difficult by not having uniform flowrates among the parallel
channels. It is also not an efficient way of using the diffusion areas, since there is
essentially no flow going through a majority of the channels farthest from the center.
Hydraulic resistance is a function of the path length, as shown in Eq. 3.13. Since the outer
channels in Figure 3.4 require a much longer detour to reach the outlet than the center
channels, where it is essentially a straight path, the flowrates cannot be expected to be
evenly distributed.

44
Figure 3.4G: CFD analysis of the non-bifurcating channel design. Fluid enters from the short
channel on the left and exits on the right. Most of the flow goes through the center channels, while the
outer channel have negligible flowrates.
3.2.1.2 Final Design: Bifurcating Tree
A bifurcating tree design is used to ensure that the flowrates in each of the parallel
channels are equal, as seen in the CFD analysis in Fig. 3.5. At each bifurcation stage, the
flowrate is divided equally into the next bifurcation stage. Inherent to the bifurcation
design, there are 2n channels, where n is the number of bifurcating stages. For this device,
there are 32 channels (n = 5).
Although both the perfusion and reservoir layers use the bifurcating tree design,
they are given a slightly different design from one another. Fig. 3.6 shows the two layers
properly aligned, in such a way that the long channels in the center have maximum
overlap areas. However, one can notice areas in the bifurcating tree sections where there
are no overlap. This staggered design minimizes the amount of interaction, whether it’s
diffusion or convection, in areas that make theoretical calculations more difficult.

45
Although minimized, it is impossible to avoid all overlap in the staggered areas without
having to make drastic design and manufacturing changes.
Figure 3.5: Bifurcating channel design: a CFD analysis showing a surface plot of the velocity field.
Red denotes high velocity and blue denotes low velocity. At each bifurcation stage, the flowrate splits
up equally. This is only a partial model due to computational constraints.

46
Figure 3.6: Stacked view of the perfusion layer (blue) aligned on top of the reservoir layer (red). The
staggered design in the bifurcating tree section is intended to minimize interaction between the two
layers, except for the main section in the center.
3.2.2 Photolithography and Soft Lithography
The microfluidic channels are created using photolithography and soft lithography
techniques. SU-8 negative photoresist (MicroChem, Boston, MA) is a UV light-sensitive
material used for its ability to create thick and high aspect ratio structures. When exposed
to UV light, negative photoresist become insoluble to photoresist developer, whereas
unexposed portions are dissolved by the developer. Using the dark field masks shown in
Fig. 3.7 and a mask aligner (EVG620, EV Group, Austria), perfusion and reservoir
structures were created on silicon wafers. The schematic of the procedure is shown in
Fig. 3.8 and the full recipe is given in Tables 1 and 2.
The channels in the bifurcating trees for the perfusion and reservoir masks are
400µm wide. The widths of the main channel are 400 and 600 µm for the perfusion and

47
reservoir channels, respectively. The length of the main section is 25 mm long for both
layers. The recipe in Table 1, using SU-8 2025, creates a layer of photoresist 30 µm thick
while the recipe in Table 2, using SU-8 2150, creates a layer of photoresist 130 µm thick.
Figure 3.7H: Dark-field masks for photolithography. Left: Perfusion mask. Right: Reservoir mask.
Figure 3.8: Soft-lithography steps used to create microfluidic channels in PDMS.

48
Table 1: Photolithography recipe for 30 micron thick Perfusion Channel
Perfusion Channel - 30 micron thickness
# Step Description Time
Soak silicon wafer in acetone solution 10 min
Soak silicon wafer in isopropyl alcohol (IPA) solution 10 min
Soak silicon wafer in deionized (DI) water 10 min
Rinse under running DI water 1 min
Blow dry with filtered nitrogen or filtered air 1 min
1 Cleaning Procedures
Bake in vented oven at 200C 30 min
2 Spin Coating
SU-8 2025, 500 RPM for 5 sec @ accl. 100 RPM/sec, then 2875 RPM for 30 sec @ accl. 300 RPM/sec ---
Place on hot plate at 65C 2 min 3 Softbake
Place on hot plate at 95C 5 min
4 Exposure Set exposure dose to 300
mJ/cm^2
Place on hot plate at 65C 1 min 5 Post-exposure Bake
Place on hot plate at 95C 3 min
6 Develop Soak in SU-8 developer solution, agitate 5 min
7 Rinse Rinse in IPA ---
Table 2: Photolithography recipe for 130 micron thick Reservoir Channel
Reservoir Channel - 130 micron thickness
# Step Description Time
Soak silicon wafer in acetone solution 10 min
Soak silicon wafer in isopropyl alcohol (IPA) solution 10 min
Soak silicon wafer in deionized (DI) water 10 min
Rinse under running DI water 1 min
Blow dry with filtered nitrogen or filtered air 1 min
1 Cleaning Procedures
Bake in vented oven at 200C 30 min
2 Spin Coating
SU-8 2150, 500 RPM for 10 sec @ accl. 100 RPM/sec, then 3000 RPM for 30 sec @ accl. 300 RPM/sec ---
Place on hot plate at 65C 6 min 3 Softbake
Place on hot plate at 95C 37 min
4 Exposure Set exposure dose to 250
mJ/cm^2
Place on hot plate at 65C 5 min 5 Post-exposure Bake
Place on hot plate at 95C 13 min
6 Develop Soak in SU-8 developer solution, agitate 16 min
7 Rinse Rinse in IPA ---

49
The photolithography step creates the “master,” a negative mold comprised of
photoresist on a silicon wafer from which many PDMS molds can be made from [92].
The master is placed inside a petri dish, with the photoresist-side facing up. PDMS (Dow
Corning Sylgard 184, Dow Corning, Midland, MI) molds are created by mixing the base
and curing agent at a ratio of 10:1 by mass, then pouring the mixture into the petri dish.
This can then be allowed to cure at room temperature overnight or in a 600C oven for 2
hours to solidify. Cured PDMS is cut and peeled from the master mold and inlet/outlet
access holes are punched out with an 18G flat-tipped needle so that Intramedic PE-10
polyethylene tubing (Becton Dickinson, Franklin Lakes, NJ) can be inserted with a snug
fit. Once the tubing is inserted, a fast-curing sealant is applied around the base of the
tubing to prevent leakage and accidental removal.
3.2.3 Bonding to membrane
The bonding portion of the production process is the most critical, yet most
difficult, step. Several experiments were performed to find the most effective bonding
method between the polycarbonate (PC) track-etched membrane (Fig. 3.9) and PDMS
pieces. No method can be declared a decisive winner because each offers benefits as well
as drawbacks.
3.2.3.1 Thermal
Putting the two materials together and placing it in a 1600C to 180
0C oven for 5 or
more hours resulted in a very strong, non-reversible bond. Unfortunately, extreme
wrinkling of the membrane was observed after the bonded device is removed from the

50
oven. Membrane wrinkling is one of the main manufacturing problems because it
typically leads to partial or complete blockage of the channels, rendering the entire device
unusable. As the temperatures of the PDMS layers and PC membrane rises in the oven,
PDMS expands more than the membrane because of its larger thermal expansion
coefficient. Eventually, this is followed by the two materials being permanently bonding
to one another, at their disproportionately expanded state, once sufficient time and
temperature has been reached. As a result, the membrane takes on a “wrinkled”
appearance, creating peaks and valleys in the membrane, which are easily tall enough to
partially or completely obstruct the 30 µm tall perfusion channels. Although making
perfusion channels thicker than 30 µm can help with channel-blockage issues, that
change would also lower the extraction efficiency of the device by increasing the
diffusion length, thereby increasing the residence time the perfusate would require to
reach equilibrium with the reservoir channel concentration.
Figure 3.9: Commercial track-etched membranes. Left: a circular membrane, 47 mm in diameter,
held by a tweezer. Right: an SEM image of the cylindrical pores on the membrane. [93]

51
3.2.3.2 Thin film deposition
Although Whitesides et al. were able to irreversibly bond PDMS to materials such
as itself, glass, silicon, polyethylene, and polystyrene by simply exposing the surfaces to
oxygen plasma and bringing the surfaces into contact, it failed to work for materials such
as polyimide, PMMA, and polycarbonate [92]. Cremer et al. were able to produce an
irreversible bond between a thin film of titanium dioxide and PDMS by using
Whitesides’ oxygen plasma method.
Utilizing the works of Whitesides and Cremer, experiments were performed to see
if the PC membranes could first be coated with a thin film of titanium dioxide and then
bond it to PDMS, as Cremer had done in a similar manner. A thin film of pure titanium
was sputtered onto a PC membrane via magnetron DC sputtering (PVD75, Lesker,
Clairton, PA). Titanium oxidizes into titanium dioxide on its own when exposed to air,
but surface treating it with oxygen plasma also helps. Freshly cured PDMS and titanium
dioxide-coated PC membranes were treated with oxygen plasma using a variety of power
and time settings to find an optimal recipe. Once the membrane contacted PDMS, it was
left at room temperature over night with weights laying on top. These experiments
produced moderate to excellent bonding strength, similar to that of the thermal bonding
method but without the wrinkling issues. However, the bond disappears once the
membrane is exposed to water. Currently, it is not clear if the bond fails between PDMS
and titanium dioxide or between titanium dioxide and polycarbonate, but further research
into this method may find a way to overcome the water issue.

52
3.2.3.3 Epoxy Stamping
Of the methods mentioned thus far, the most effective method for bonding
membranes (where, in this case, “bonding” is referred to in the mechanical sense) to
PDMS is by using a biocompatible epoxy (Epo-Tek 301, EpoTek, Billerica, MA) as an
intermediate layer between PDMS and the membrane [94]. A major advantage for using a
“mortar” (e.g. glue, PDMS, or even brick mortar) to join surfaces together is that it is
forgiving for rough and imperfect surfaces, such as that found on a porous membrane.
Assuming the epoxy is capable of filling the micro-sized pores of the membrane, part of
its adhesive capability may be due to the bonding of epoxy on one end of a pore, to the
epoxy on the other end; thereby, interlocking the membrane. Because the microfluidic
channels embedded into the PDMS layer are only 30 µm and 130 µm thick for the
perfusion and reservoir channels, respectively, steps must be taken to prevent epoxy from
getting into the channels and causing partial or complete blockage. More importantly,
excess epoxy can spread onto the diffusion areas of the membrane, clogging the pores. In
addition to these problems, the strength of the bond is usually not very strong when only
a thin layer of epoxy is used.
Stamping consists of placing the bonding side of both PDMS layers onto a thin
layer of epoxy and joining the three layers together as shown in Fig. 3.10. Once joined,
the device is given 24 hours to cure to achieve full bonding strength. The simplest and
quickest method to create a thin layer of epoxy is to pour some epoxy onto a flat surface
and use a flat edge to spread the epoxy until a uniform thin layer is achieved. Using a
spin coating machine has the advantage of being able to create repeatable uniform
thicknesses, unlike the manual method of spreading a thin layer by hand. However, spin

53
coating is best used for slow curing adhesives because the spinning process can
completely drive off the solvent in epoxies before the bonding surfaces can come
together. For this reason, uncured PDMS is preferred for its longer curing time but seems
to suffer from a weaker bonding strength than epoxy.
Figure 3.10: Schematic for the epoxy stamping procedure. A) a small amount of epoxy is placed on
top of a clean glass slide; B) an object with a flat edge, such as another glass slide, is used as a
squeegee on the epoxy until a thin, uniform layer of epoxy remains; C) the first PDMS layer is placed
onto the thin layer of epoxy, with the channel side facing down; D) and E) a membrane is placed on
top of the epoxy-side of the first PDMS layer; F) steps A-C are repeated for the second PDMS layer
and aligned with the first layer under a dissection microscope.
3.3 Numerical Studies - Electric Circuit Model
In order to establish a starting baseline for channel geometry, membrane pore
size, tubing length, and flowrate parameters, a Matlab program was written to solve a
circuit diagram representing the experimental setup, as shown in Fig. 3.11. The objective
was to determine a set of conditions for which diffusion of analytes across the membrane
pores, from the reservoir channel to the perfusion channel, was the primary mode of

54
transport. In other words, convective flux was to be minimized and only in the direction
of reservoir-to-perfusate, if it exists at all.
In the circuit diagram, there are two flowrate sources: 1) the reservoir fluid
(blood) is driven by a pressure head generated by the CPB pump, represented by a
voltage source and 2) the perfusate (lactated Ringer’s solution) is driven by a syringe
pump at a specific flowrate, represented by a current source. The reservoir source
undergoes its first pressure drop due to the resistance in the reservoir channel’s inlet
tubing. Comparatively, the perfusion source is not followed by a resistor for the perfusion
channel’s inlet tubing since it is driven by a current source and its pressure drop does not
affect the rest of the circuit. The two nodal points on either side of the pore resistor
represent the pressure difference that determines the flowrate through the membrane
pores. An assumption is made that the pressure at the reservoir node is always greater
than or equal to the pressure at the perfusate node. Under this assumption, the perfusate
should not be able to enter the reservoir channel, which would dilute the reservoir
solution. This assumption is also necessary to provide enough known variables to solve
the set of linear equations described below; otherwise, since the pore’s resistance can
either be a function of the blood plasma’s viscosity or the Ringer’s solution’s viscosity,
depending on which direction fluid travels. This assumption can be verified by solving
for the entire circuit and checking to see if the reservoir node pressure is greater than or
equal to the perfusate node pressure, if not, that particular solution is invalid.

55
Figure 3.11: A circuit diagram representing the microdialysis chip. The reservoir side is given a
voltage source to represent the pressure source given by the CPB pump. The perfusate side is given a
current source to represent the predetermined flowrate put out by a syringe pump. Resistors
represent hydrodynamic resistance, which is a function of channel geometry and fluid viscosity.
Since convective flow through the pores can occur throughout the entire length of
the channel, the problem is simplified by dividing the pressure at the nodes in half when
calculating flowrate through the pores, thereby representing the average pressure over the
length of the channel. Finally, the perfusate and reservoir solutions experience pressure
drops due to their respective PDMS channels, where they eventually reach the end of the
device and into collection tubes, which are at atmospheric pressure. Although there is
tubing connected to the outlet ports of the device, this tubing is much shorter than the
inlet tubing and assumed to have negligible resistance.

56
Using Kirchhoff’s current law (KCL), which states that the sum of currents
flowing into a nodal point is equal to the sum of currents flowing out of the nodal point,
and Ohm’s law,
∆V = IRelec Equation 3.15
where ∆V is the voltage drop which is analogous to a pressure drop, I is the current
which is analogous to flowrate, and Relec is the electrical resistance which is analogous to
the pressure drop equation in Eq. 3.12 if the solutions are assume to behave as Newtonian
fluids..
At the ‘Reservoir Node’ (see circuit diagram in Fig. 3.11), applying KCL gives
pore
Rsrv
Rsrv
Tubing
RsrvsourceCPBQ
R
P
R
PP−−
−= ,
0 Equation 3.16
where PCPB,source is the pressure provided by the CPB circuit, PRsrv is the pressure at the
reservoir node, RTubing is the resistance in the tubing leading from where the reservoir
tubing connects with the CPB circuit to the reservoir-side of the device, RRsrv is the
resistance through the reservoir channels, and Qpore is the flowrate crossing the
membrane.
At the ‘Perfusate Node,’ applying KCL gives
Perf
Perf
PoresourcePerfR
PQQ −+= ,0 Equation 3.17
where Qperf,source is the syringe pump flowrate that is set by the user, PPerf is the pressure at
the perfusate node, and RPerf is the resistance through the perfusate channels.
The flowrate through the membrane is given by applying the hydraulic
equivalence of Ohm’s law,

57
( )Pore
PerfRsrv
PoreR
PPQ
−=
21 Equation 3.18
where the “½” refers to taking the average pressure difference between the channels, as
noted earlier.
For simplification, blood is assumed to be a non-Newtonian fluid in this analysis.
The blood flowrate entering the reservoir channel is given by applying the hydraulic
equivalence of Ohm’s law,
Tube
RsrvsourceCPB
sourceRsrvR
PPQ
−= ,
, Equation 3.19
The overall hydraulic resistance in the reservoir channel is given by applying Eq.
3.13,
1
,...5,3,1553 2
tanh1192
112
−∞
=
−= ∑
n Rsrv
Rsrv
Rsrv
Rsrv
ChanRsrvRsrv
RsrvH
Wn
nW
H
NHW
LR
ππ
µ Equation 3.20
where µBlood is the dynamic viscosity of blood at 35oC, L is the length for both the
perfusion and reservoir channels, WRsrv is the width of a single reservoir channel, HRsrv is
the height of the reservoir channels, and NChan is the number of channels. Without the
NChan term, the equation would only solve the resistance through a single channel.
The overall resistance in the perfusion channels is given by applying Eq. 3.13,
1
,...5,3,1553 2
tanh1192
112
−∞
=
−= ∑
n Perf
Perf
Perf
Perf
ChanPerfPerf
PerfH
Wn
nW
H
NHW
LR
π
πµ
Equation 3.21
where µLRS is the dynamic viscosity of lactated Ringer’s solution at room temperature,
WPerf is the width of a single perfusion channel, and HPerf is the height of the perfusion
channel.

58
The overall resistance in the membrane pores is given by applying Eq. 3.14,
( )[ ] PorePore
MembranePlasma
PoreND
TR
42
8
π
µ= Equation 3.22
where µPlasma is the dynamic viscosity of human blood plasma at 35oC, TMembrane is the
thickness of the membrane, DPore is the pore diameter give in Table 3, and NPore is the
number of pores available in the active diffusion area, Am. The SEM image in Fig. 3.9
(right) shows that the pores can be approximated as straight, uniform tubes.
The number of pores is a function of the pore density and the available diffusion
area given by the equation
( )LWNAN PerfChanPoremPorePore ρρ == Equation 3.23
where ρPore is the pore density which varies depending on the manufacturer’s
specifications (see Table 3). Am is a function of the perfusion channel’s width since the
perfusion channels are purposely designed to be narrower than the reservoir channels,
making perfusion widths the limiting factor.
The hydraulic resistance of the polyethylene tubing (Intramedeic PE-10, Becton
Dickinson, Franklin Lakes, NJ) connected to the reservoir inlet is given by,
( )4,
2
8
Tubing
TubingRsrvBlood
TubingD
LR
π
µ= Equation 3.24
where LRsrv,Tubing is the length of the reservoir inlet tubing and DTubing is the inner
diameter of the tubing.

59
Table 3: Whatman Nucleopore Polycarbonate Track-etched Membranes
Pore Size (micron)
Pore Density (pores/cm^2)
Membrane Thickness (micron)
0.05 6x10^8 6
0.08 6x10^8 6
0.1 3x10^8 6
0.2 3x10^8 10
0.4 1x10^8 10
0.6 3x10^7 10
0.8 3x10^7 9
3.3.1 Observing Trends from Matlab Code
Although the above equations are not used to calculate analyte extraction
efficiency, in this case, microdialysis performance is judged in terms of the perfusion
flowrate recovery (PFR). PFR is the ratio of the flowrate exiting the perfusion outlet to
the perfusion flowrate going in, given as
100,
, ×+
==sourcePerf
PoresourcePerf
Q
tenletFlowraPerfusionI
ateutletFlowrPerfusionOPFR Equation 3.25
where QPerf,source is the perfusion flowrate that is set by the syringe pump, and QPore is the
additional flowrate from blood plasma crossing over the membrane to the perfusion
channels due to some pressure differential. Under ideal conditions where there is no fluid
flux across the membrane, PFR equals 100% since there is no QPore contribution. If the
hydraulic pressure of the reservoir channel is much greater than the pressure of the
perfusion channel, extracellular fluid may cross the membrane and into the perfusion
channel, i.e. PFR > 100%, affecting Ed. In the reverse situation, where the perfusion
channel’s hydraulic pressure is much greater than the reservoir channel’s pressure, i.e.
PFR < 100%, meaning lactated Ringer’s solution crosses over to the reservoir channel,

60
which dilutes the analyte concentration in blood and affecting Ed as well.
In order to see how PFR is affected by operating parameters such as: CPB
pressure, perfusate flowrate, reservoir inlet tube length, and membrane pore size/density;
two parameters varied at a given time. Meanwhile, the remaining parameters are held at a
nominal value. Since commercial membranes are used in the devices, the membrane pore
size, pore density, and thickness are essentially non-customizable except for what is
already available in the product line. Because of this limitation, membrane selection is
important and will be used as the recurring variable in Fig. 3.12-3.14.
Fig. 3.12-3.14 show how small pore sized membranes have a very stable PFR
close to 100% across the span of the x-axis, while large pore sized membranes are very
sensitive to the x-axis parameter. Because the relationship between pore diameter and
pore resistance is 4
1
Pore
PoreD
R ∝ , the small pore sized membranes have such large
resistances that, relative to larger pore sized membranes, the flow on one side of the
membrane is less likely to be able to influence the flow on the opposite side. Pore
density has less of an impact, compared to the pore diameter, on overall resistance due to
its Pore
PoreRρ
1∝ relationship (where ρPore is the pore density), and is not referred to
explicitly when describing the membrane. A stable PFR around 100% across a wide
range of design and operating parameters is a quality that a robust device should have. It
means the device can operate predictably under varying conditions. Unfortunately, it can
also be an indication that the membrane’s pore resistance is too high (i.e. a completely
impermeable membrane would inherently always have a PFR of 100%). Therefore, a
compromise must be made between device robustness and analyte permeability.

61
There is negligible difference in PFR, between the 0.08 µm and 0.1µm pore size
membrane but a significant difference in PFR, between the 0.1 µm and 0.2 µm pore size
membrane (Fig. 3.12-3.14). Since there are no intermediate pore sizes available from the
manufacturer, the 0.1 µm membrane is a reasonable compromise between MWCO and
robustness. Fig. 3.12 shows a linear relationship between PFR and CPB pressure, where
the intersection point represents the chosen nominal value and large deviations from this
value dramatically affects PFR outcome. Meanwhile Fig. 3.13 and 3.14 show an
exponentially decaying relationships between PFR with respect to perfusion flowrate and
reservoir tubing length, where low perfusion flowrates and short reservoir tubing lengths
produce the largest deviations from 100% PFR. On the other hand, using high perfusion
flowrates is not necessarily the solution since it will lower Ed as seen in Eq. 3.11 .
0
50
100
150
200
250
300
0 20 40 60 80 100 120 140 160 180
CPB Pressure (mmHg)
Perfusion Flowrate Recovery %
.05 um pore
.08 um pore
0.1 um pore
0.2 um pore
0.4 um pore
0.6 um pore
0.8 um pore
Figure 3.12: Results from Matlab model: Perfusion flowrate recovery vs CPB Pressure, for various
pore sizes.

62
0
50
100
150
200
250
300
350
400
450
0 1 2 3 4 5 6 7 8 9
Perfusion Flowrate (ul/min)
Perfusion Flowrate Recovery %
.05 um pore
.08 um pore
0.1 um pore
0.2 um pore
0.4 um pore
0.6 um pore
0.8 um pore
Figure 3.13: Results from Matlab model: Perfusion flowrate recovery vs Perfusion flowrate, for
various pore sizes.
0
100
200
300
400
500
600
0 1 2 3 4 5 6 7 8 9
Reservoir Inlet Tubing Length (in)
Perfusion Flowrate Recovery %
.05 um pore
.08 um pore
0.1 um pore
0.2 um pore
0.4 um pore
0.6 um pore
0.8 um pore
Figure 3.14: Results from Matlab model: Perfusion flowrate recovery vs Reservoir inlet tubing
length, for various pore sizes.
Next, a similar analysis is performed using the Matlab program to observe the
effects of the reservoir channel height, CPB pressure, perfusion flowrate, and reservoir

63
tubing length on PFR, as shown in Fig. 3.15-3.17. The important information to extract
from these figures is the trend, rather than the PFR actual values, since the non-varying
parameters are assigned non-optimized values. In these figures, PFR is most stable when
the reservoir height is largest, for all three x-axis parameters. In this case, a reservoir
channel height of 110 µm exhibits very little PFR change, from one end of the x-axis to
the other, when compared to a reservoir channel height of 30 µm. A tall reservoir height
has the additional benefit of reducing the chances of damaging blood and further
activating the inflammatory response by reducing shear stress.
0
500
1000
1500
2000
2500
3000
3500
4000
4500
5000
0 20 40 60 80 100 120 140 160
CPB Pressure (mm Hg)
Perfusion Flowrate Recovery %
Rsrv Height 30 um
Rsrv Height 50 um
Rsrv Height 70 um
Rsrv Height 90 um
Rsrv Height 110 um
Figure 3.15: Results from Matlab model: Perfusion flowrate recovery vs CPB Pressure, for various
reservoir channel heights.

64
0
1000
2000
3000
4000
5000
6000
7000
8000
0 1 2 3 4 5 6 7 8 9
Perfusion Flowrate (ul/min)
Perfusion Flowrate Recovery %
Rsrv Height 30 um
Rsrv Height 50 um
Rsrv Height 70 um
Rsrv Height 90 um
Rsrv Height 110 um
Figure 3.16: Results from Matlab model: Perfusion flowrate recovery vs Perfusion flowrate, for
various reservoir channel heights.
0
1000
2000
3000
4000
5000
6000
7000
0 2 4 6 8 10 12 14 16 18
Reservoir Inlet Tubing Length (in.)
Perfusion Flowrate Recovery %
Rsrv Height 30 um
Rsrv Height 50 um
Rsrv Height 70 um
Rsrv Height 90 um
Rsrv Height 110 um
Figure 3.17: Results from Matlab model: Perfusion flowrate recovery vs Reservoir inlet tubing
length, for various reservoir channel heights.

65
In contrast to the previous figures showing the effects of reservoir heights, Fig.
3.18-3.20 show that a shallow perfusion channel height is more stable than a taller height,
and is preferred when designing for robustness. However, there is a limit to how shallow
a channel height can be before significant problems arise during the fabrication process.
Shallow channel heights suffer from a greater chance for epoxy to partially or completely
block channels during the epoxy stamping procedure.
0
100
200
300
400
500
600
700
800
900
0 20 40 60 80 100 120 140 160
CPB Pressure (mm Hg)
Perfusion Flowrate Recovery %
Perf Height 20 um
Perf Height 30 um
Perf Height 40 um
Perf Height 50 um
Perf Height 60 um
Figure 3.18: Results from Matlab model: Perfusion flowrate recovery vs CPB Pressure, for various
perfusion channel heights.

66
0
200
400
600
800
1000
1200
1400
0 1 2 3 4 5 6 7 8 9
Perfusion Flowrate (ul/min)
Perfusion Flowrate Recovery %
Perf Height 20 um
Perf Height 30 um
Perf Height 40 um
Perf Height 50 um
Perf Height 60 um
Figure 3.19: Results from Matlab model: Perfusion flowrate recovery vs Perfusion flowrate, for
various perfusion channel heights.
0
200
400
600
800
1000
1200
1400
1600
1800
2000
0 2 4 6 8 10 12 14 16 18
Reservoir Inlet Tubing Length (in.)
Perfusion Flowrate Recovery %
Perf Height 20 um
Perf Height 30 um
Perf Height 40 um
Perf Height 50 um
Perf Height 60 um
Figure 3.20: Results from Matlab model: Perfusion flowrate recovery vs Reservoir inlet tubing
lengths, for various perfusion channel heights.

67
With the preceding Matlab simulation results and manufacturing constraints in
mind, design parameters were finalized for use with blood in a mock CPB circuit, shown
in Table 4. Although, theoretically, the objective is to maximize robustness and dialysis
performance, in reality, compromises in these areas must be made for manufacturing
reasons.
Table 4: Finalized Microdialysis Design for CPB integration
Perfusion Height 30 µm
Perfusion Width 400 µm
Reservoir Height 130 µm
Reservoir Width 600 µm
Channel Length 25 mm
Number of Channels 32
Membrane Pore Size 0.1 or 0.4 µm
Perfusion Flowrate (Syringe Pump) 4.1 µl/min
Membrane Bonding Method Epoxy
stamping
3.4 Microdialysis Experiments
In order to test the proof-of-concept of the proposed microdialysis device, bench-
top experiments were conducted using a syringe pump, instead of a CPB pump, and a
glucose/phosphate-buffered-saline (PBS) solution, instead of blood. Samples were then
collected from the device and analyzed for glucose. These bench-tops experiments helped
to establish protocols and techniques that were then used for the mock CPB circuit
experiments.
Before a device was to be used, it was exposed to oxygen plasma (power: 100 W,
time: 60 sec) for sterilization and to render the channel surfaces hydrophilic. Sterile DI
water is then used to completely fill all of the microchannels, including the tubing. This

68
step is vital to reduce the risk of a bubble lodging itself into a channel, thereby blocking
flow through that channel and disrupting the uniform flowrates across the 32 channels.
3.4.1 Experimental Setup: Glucose and PBS
Theoretically, changing perfusate and/or reservoir flowrates affect both the
pressure balance across the membrane and the extraction efficiency of the device (see Eq.
3.11) simultaneously. Bench-top experiments were conducted to find flowrates that
minimize convective flux across the membrane, while attempting to maximize analyte
recovery.
For these experiments, a variation of the final design (Table 4) was used: the
perfusion channel height was 20 µm, the reservoir channel height was 65 µm, the
membrane had a 0.4 µm pore diameter, the reservoir fluid was a ~200 mg/dl glucose/PBS
solution, and glucose-free PBS was used as the perfusate. The perfusate and reservoir
solutions were infused into the device via individually controlled syringe pumps. In this
case, the perfusion flowrate was held constant at 4 µl/min, while the reservoir flowrate
varied between 41 µl/min and 75 µl/min. Before connecting the reservoir syringe to the
device, a sample of the glucose/PBS solution was collected to be used as the reference
concentration, C∞. Once the device was connected and the syringe pumps were turned on
at the appropriate flowrates, the first samples were not collected until a 30 minute waiting
period had passed in order to allow the chemical and flow profiles to stabilize. This
waiting period was also used after every change made to the flowrate. Samples were
collected until there was at least 75 µl of solution in both collection tubes and the
collection time was recorded. Glucose concentration and volume measurements were

69
made at the reservoir and perfusate outlet. Glucose concentration was measured with a
biochemistry analyzer (YSI 2700 Select, YSI Life Sciences, Yellow Springs, OH) and
volume was measured using a pipette.
To verify the accuracy of the numerical simulations with experimental values, the
Matlab code used to simulate Fig. 3.11 was rewritten for the bench-top glucose/PBS
experiment with the following modifications: the reservoir channel became flowrate
driven via a syringe pump, instead of pressure driven by the CPB circuit; the reservoir
inlet tubing resistance is ignored due to the reservoir being current-sourced; the channels’
geometric resistances were modified to represent the changes made to the channel heights
and widths, as described in the previous paragraph; and all dynamic viscosities were that
of PBS since blood was not used. The revised circuit diagram is shown in Fig. 3.21.
Figure 3.21: A revised circuit diagram for the bench-top glucose/PBS experiments, based off of Fig
3.11, where the reservoir channel is driven by a syringe pump, instead of a CPB pump. Thus, the
reservoir inlet tubing resistance can be ignored and the reservoir inlet is now represented with a
current source.

70
3.4.2 Results and Discussion: Glucose and PBS
Results for the experimental and theoretical volume recoveries, as a function of
reservoir flowrate, are shown in Fig. 3.22, where volume recovery is defined as the
volume measured at the outlet of either the perfusion channel (PERF), or reservoir
channel (RSRV), divided by the volume of fluid infused by the respective syringe pump,
which is determined by multiplying the flowrate by the collection time. A volume
recovery greater than 100% implies that more volume exits that particular channel than
was expected, and vice versa. As reservoir flowrate increases, the hydraulic pressure
within the reservoir channels also increases, driving more and more reservoir solution to
cross the membrane into the perfusion channel. As a result, the reservoir volume recovery
decreases. Intuitively, the perfusion volume recovery increases as a result. Linear
regression trendlines for perfusion and reservoir volume recovery data show an
intersection point when the reservoir flowrate is 50 µl/min and the perfusate flowrate is 4
µl/min, at which point both channels have ~100% volume recovery. Theoretically, this
point suggests that there is very little convective flux across the membrane, from either
direction.
Despite the appearance that the theoretical values for the reservoir volume
recovery matches closely to its corresponding experimental values (Fig. 3.22, solid and
hollow square data points) and that the experimental perfusion volume recovery appears
to be quite different than its predicted values, this outcome is partially due to the fact that
the reservoir flowrate was significantly greater than the perfusion flowrate. For example,
4 µl/min “error” between the experimental and theoretical reservoir outlet flowrate is a
relatively small difference compared to its original value ranging between 41 µl/min and

71
75 µl/min). How ever, when that additional 4 µl/min crosses into the perfusion channel, it
doubles the original flowrate of 4 µl/min. Therefore, a better methodology for evaluating
the accuracy of the numerical model would be to run both channels at similar flowrates.
Volume Recovery vs Reservoir Flowrate
20
40
60
80
100
120
140
160
35 45 55 65 75 85
Reservoir Flowrate (uL/min)
Volume Recovery %
Perf, Exper.
Rsrv, Exper.
Perf, Theor.
Rsrv, Theor.
Linear (Rsrv,
Exper.)
Linear (Perf,
Exper.)
Linear (Perf,
Theor.)
Linear (Rsrv,
Theor.)
Figure 3.22: Theoretical (hollow) and experimental (solid) Volume Recovery values for perfusion
(diamond) and reservoir (square) outlets, versus varying reservoir flowrates.
Glucose concentration recovery as a function of reservoir flowrate is shown in
Fig. 3.23, where recovery is defined as the outlet concentration divided by the reference
concentration, C∞. The figure shows the outlet concentration recovery from both channels
overlapping one another throughout the full range of flowrates tested. Both the perfusion
and reservoir fluids reach very similar glucose concentrations throughout the entire range
of reservoir flowrates, despite the direction of convective flux across the membrane. The

72
assumption that the two solutions are fully mixed by the time it exits the device by
verifying that,
totalinitialtotalinitialrsrvfinalrsrvfinalperffinalperffinal CmCmCm ,,,,,,&&& =+ Equation 3.26
where, perffinalm ,& , rsrvfinalm ,
& , and totalfinalm ,& are the glucose mass flow rates from the
perfusion outlet, reservoir outlet, and the total from the perfusion and reservoir inlet,
respectively. perffinalC , , rsrvfinalC , , and totalinitialC , are the glucose concentration values from
the perfusion outlet, reservoir outlet, and the total from the perfusion and reservoir inlet,
respectively.
From solving Eq. 3.26, it was shown that the two solutions were indeed fully
mixing while inside the device, most likely due to the larger 0.4 µm membrane pore size
that was used. The slight dilution of the glucose/PBS reservoir solution is not expected to
be a concern as long as the mass flow rate of the reservoir solution is significantly greater
than that of the perfusate solution.
Based on the numerical studies, shown in Fig. 3.12-3.14, the effect that flowrate
has on volume recovery can be decreased by using membranes with smaller pore sizes.
While this may aid in reducing large changes in volume recovery, it may also reduce
perfusate analyte recovery.

73
Glucose Recovery vs Reservoir Flowrate
50
60
70
80
90
100
110
120
130
140
150
30 40 50 60 70 80 90
Reservoir Flowrate (uL/min)
Glucose Recovery %
PERF, concent.
RSRV, concent.
Linear (RSRV, concent.)
Linear (PERF, concent.)
Figure 3.23: Glucose concentration recovery for perfusion and reservoir channels, for varying
reservoir flowrates. Data shows that both channels end up with near-identical concentrations for a
wide range of flowrates, causing the data points to overlap one another.
3.4.3 Introduction: Blood with Mock CPB Circuit
The microdialysis device, as described in Table 4, was used in a mock CPB
circuit to test the recovery performance for the complements C3a, C4a, and C5a in human
blood. Experiments were conducted under the supervision of Dr. Akif Undar, Director of
the Pediatric Cardiac Research Laboratories at Hershey Medical Center (Hershey, PA).
Two devices were tested on the same day, but separately: the first had a membrane pore
diameter of 0.1 µm and the other had a 0.4 µm diameter. The devices were otherwise
identical.

74
3.4.3.1 Experimental Setup: Blood with Mock CPB Circuit
A mock in vitro CPB circuit was primed by a perfusionist, where packed red
blood cells (PRBCs) are hemodiluted with lactated Ringer’s solution to obtain a
hematocrit level of 26% and pumped through the circuit at 500 ml/min at an arterial
circuit pressure of 100 mmHg. The Hershey Medical Center’s blood bank provided
PRBCs as a substitution for whole blood due to the limited availability of whole blood
for non-medical, non-emergency usage. The “packed cells” are prepared by removing
platelets, plasma, and sometimes white blood cells from whole blood. Although PRBCs
contain little coagulation factors, 4 Units/ml of heparin was added to the circuit to
simulate a real CPB circuit as accurately as possible. A heat exchanger maintained the
blood at normothermic conditions. The perfusionist monitored and controlled blood pH-
levels by supplying appropriate blood-gases
Prior to connecting the microdialysis devices to the CPB circuit, both the
perfusion and reservoir channels were infused with a filtered 0.5% w/v solution of PBS
and bovine serum albumin (BSA) at 60 µl/min and 4 µl/min, respectively, for 30 minutes.
BSA is commonly used to minimize surface adsorption of the analyte to exposed areas
such as the channel walls and membrane surface [95, 96].
The device’s reservoir inlet tubing was then connected to the circuit at a sampling
manifold located downstream of the arterial port of the membrane oxygenator, as shown
in Fig. 3.24. The device’s perfusion inlet tubing was connected to a syringe filled with
lactated Ringer’s solution, which was driven by a syringe pump. The perfusion flowrate
was set to 4.1 µl/min while the reservoir flowrate was determined to be 40 µl/min,
according to timed volume measurements. For the first 45 minutes, the fluid exiting the

75
device was not collected for analysis since this contained the PBS-BSA solution initially
infused into the device. Once this waiting period had passed, reservoir outlet and
perfusate outlet samples were collected in separate 1.5 ml microcentrifuge tubes for 15
minutes, every 15 minutes, for 1.5 hours (i.e. 6 samples).
At the half-way mark of each 15 minute sampling period, a 1 ml blood sample
was collected from a different sampling port downstream of the membrane oxygenator.
This blood sample provided a snapshot of analyte concentrations in the blood before it
enters the reservoir channel, thereby providing a reference point to compare how much
the reservoir solution was being diluted during dialysis, if at all. Collecting this blood
sample at the 7 min. 30 sec. mark provided an estimate of the average analyte
concentration during each 15 minute sampling period, in case C3a, C4a, and C5a levels
fluctuated over time.
Collected samples were stored on ice, until the end of the experiment, when they
were snap-frozen at -80OC. Analysis was performed by Hershey Medical Center using a
commercially available anaphylatoxin cytometric bead kit (BD Biosciences, San Jose,
CA).

76
Figure 3.24: The setup for the mock CPB circuit experiments. A relatively small quantity of blood
flow is routed to the reservoir channel of the microdialysis device, via a Luer connection at the
sampling manifold on the arterial side of the oxygenator.

77
3.4.3.2 Results and Discussion: 0.1 µm membrane
A two-tailed paired t-Test was conducted on the data, where the null hypothesis,
H0, states that the two sample means are equal in concentration or relative recovery. The
statistical significance value, α, used is 0.05.
For the 0.1 µm device, the average C3a, C4a, and C5a concentration recoveries
are shown in Fig. 3.25 for the perfusion outlet, reservoir outlet, and CPB sample. The
graph shown in Fig. 3.26 uses the same data as Fig. 3.25 but converts it to relative
recovery (equivalent to extraction efficiency, Ed) for a quicker evaluation of device
performance, simply by dividing the perfusion or reservoir outlet concentration with the
CPB circuit concentration.
For C3a in the 0.1 µm device (Fig. 3.25, left), the perfusion channel appeared to
reach an equilibrium point with the reservoir channel but at the expense of a diluted
reservoir channel, as demonstrated by the higher C3a concentration from the CPB circuit.
Using the CPB circuit concentration as reference, the relative recovery for the perfusion
outlet and reservoir outlet are 79% and 74%, respectively (Fig. 3.26, left).
For C4a in the same device (Fig. 3.25, center), relative recovery for C4a in the
perfusion and reservoir outlets were 75% and 56%, respectively (Fig. 3.26, center).
However, the perfusion channel resulted in unexpectedly higher relative recovery than
the reservoir channel.
The graph for C5a (Fig. 3.25, right) show yet another difference in device
performance. Relative recovery for C5a in the perfusion and reservoir outlets were 70%
and 93%, respectively (Fig. 3.26, right).

78
By looking at Fig. 3.26 as a whole, one notices that the relative recovery for the
perfusion outlet varies only slightly, between 70-79%, while the reservoir outlet varies
more widely between 74-93%. Unfortunately, it is not yet clear whether the consistency
in the perfusion outlet’s relative recovery is coincidental and, if not, why it would happen
while the reservoir outlet recovery fluctuates significantly more. It is also not clear why
C3a concentration from the perfusion and reservoir outlets were able to equilibrate during
dialysis, but C4a and C5a concentrations were not. One theory is that the difference in
molecular structures of the complements affects its permeability through the pores.
Figure 3.25: Analyte concentration for the 0.1 µm membrane device: (left) C3a, (center) C4a, and
(right) C5a. Data represents an average of 6 data points over a 1.5 hour period. A two-sample paired
t-Test was performed, where H0 = two means are equal. The asterisk (*) represents a statistical
significance level, α<0.05.

79
Figure 3.26: Relative recovery for the 0.1 µm membrane device: (left) C3a, (center) C4a, and (right)
C5a. Data represents an average of 6 data points over a 1.5 hour period. The asterisk (*) represents a
statistical significance level, α<0.05.
The p-values for a two-tailed paired t-Test and correlation coefficient values for
Fig. 3.25 and 3.26 are summarized in Table 5 and 6, respectively. According to these two
tables, the noticeable differences in the paired recovery values of the 0.1 µm membrane
device is unlikely to be coincidental and for the most part, the paired recovery values
show medium to high positive correlation, and surprisingly, with low and negative
correlations as well in C5a. Essentially, no statistical significance can be found for the 0.1
µm device.

80
Table 5: 100 nm membrane: p-values, pairwise t-test. Blue/bold values denote acceptance of the null
hypothesis.
Perf/Rsrv Perf/CPB Rsrv/CPB Perf_RR% / Rsrv_RR% C3a 0.020 0.000 0.000 0.012 C4a 0.004 0.004 0.001 0.001 C5a 0.000 0.000 0.070 0.001
Table 6: 100 nm membrane: correlation coefficient
Perf/Rsrv Perf/CPB Rsrv/CPB Perf_RR% / Rsrv_RR% C3a 0.912 0.830 0.654 0.859 C4a 0.941 0.797 0.745 0.761 C5a -0.142 0.727 0.128 0.465
3.4.3.3 Results and Discussion: 0.4 µm membrane
The 0.4 µm device appeared to have yielded more consistent and overall better
performance than the 0.1 µm device. From Fig. 3.27, one can clearly see more mean
concentrations being comparable to one another, evidence of good recovery performance
for the perfusion and reservoir channels. The reservoir outlet mean relative recoveries for
C3a and C5a, shown in Fig. 3.28, are close to 100% (105% and 106%, respectively),
whereas the reservoir outlet mean relative recovery for C4a is slightly greater, at 118%.

81
Figure 3.27: Analyte concentration for the 0.4 µm membrane device: (left) C3a, (center) C4a, and
(right) C5a. Data represents an average of 6 data points over a 1.5 hour period. A two-sample paired
t-Test was performed, where H0 = two means are equal. The asterisk (*) represents a statistical
significance level, α<0.05.
Figure 3.28: Relative recovery for the 0.4 µm membrane device: (left) C3a, (center) C4a, and (right)
C5a. Data represents an average of 6 data points over a 1.5 hour period. The asterisk (*) represents a
statistical significance level.
The p-values for a two-tailed paired t-Test and correlation coefficient values for
Fig. 3.27 and 3.28 are summarized in Table 7 and 8, respectively. According to these two

82
tables, the noticeable differences in the paired recovery values of the 0.4 µm membrane
device is unlikely to be coincidental and for the most part, the paired recovery values
show medium to high positive correlation in most cases, and similar to C5a in the 0.1 µm
device, the C5a results here had low negative correlations as well. In both cases, Fig. 3.31
in the next section demonstrates these results. The changes in concentration of C5a is so
minimal and seemingly noisy that one cannot expect a strong correlation.
Table 7: 400 nm membrane: p-values, pairwise t-test. Blue/bold values denote acceptance of the null
hypothesis.
Perf/Rsrv Perf/CPB Rsrv/CPB Perf_RR% / Rsrv_RR% C3a 0.089 0.004 0.210 0.092 C4a 0.002 0.000 0.002 0.001 C5a 0.610 0.821 0.278 0.515
Table 8: 400 nm membrane: correlation coefficient
Perf/Rsrv Perf/CPB Rsrv/CPB Perf_RR% / Rsrv_RR% C3a 0.587 0.836 0.592 0.486 C4a 0.944 0.987 0.956 0.871 C5a -0.008 0.839 -0.253 -0.341
3.4.3.4 Time Course Data
The time course data is given in Fig. 3.29-3.31 in order to observe the standard
deviations for a given sample measured using a cytometric bead assay. Although both the
0.1 µm and 0.4 µm devices follow the trend of the CPB concentration over time, albeit
roughly at times, the 0.4 µm device clearly has a better extraction efficiency throughout

83
the time course. The standard deviations, as denoted by the error bars, remain fairly
consistent for the C3a and C4a plots, Fig. 3.29 and Fig. 3.30, respectively. However, the
C5a plot for the 0.1 µm device had a significant jump in standard deviation at t = 15 min.
and t = 75 min., as seen in Fig. 3.31. In the same figure, the 0.4 µm device had a single
inconsistently large standard deviation in the reservoir outlet at the 75 minute marks as
well. The fact that, at the 75 minute mark, the reservoir outlets for both devices
experienced similar results (large standard deviation) does not seem like a coincidence.
Perhaps some form of human error, such as mishandling the samples during collection,
could have caused this outcome.

84
Figure 3. 29: Time course data with error bars representing 2 standard deviations for C3a.
Figure 3. 30: Time course data with error bars representing 2 standard deviations for C4a.

85
Figure 3.3 1: Time course data with error bars representing 2 standard deviations for C5a. (Top)
Zoomed out to see full extent of error bars at 15 and 75 min. (Bottom) Zoomed in.

86
Chapter 4 - Conclusions and Future Work
It appears that the larger pore-sized device resulted in an overall better performing
microdialysis device even though there was an initial concern about the increased risk of
convective flux across the membrane. Although the pore resistance in the 0.1 µm device
was calculated to be 51 times greater than the 0.4 µm device, there seems to be less
reservoir solution dilution in the larger pore-sized device. Another significant benefit
from using the larger membrane pore size is the increased perfusate extraction efficiency.
If whole blood or human patients are used in the experiment, other problems may
develop and have to be accounted for, such as biofouling of the membrane from platelet
activation and influences of blood temperature on device performance. When biofilm
forms on the membrane surface, it can block pores and decrease membrane permeability.
During an open-heart procedure, surgeons will typically cool the patient’s body to
intentionally induce hypothermia and eventually bring them back to normothermic
conditions. This large temperature change will affect the blood viscosity and therefore,
the hydraulic pressure within the microdialysis device, but can be remedied by adjusting
the perfusion flowrate and adjusting calibration values for C∞ as needed.

87
In the future, one major change in the microdialysis setup would be to use a
peristaltic pump, in between the CPB circuit sampling manifold and the reservoir inlet
tubing of the device. The use of a peristaltic pump will improve consistency by changing
the reservoir channels mode of transport from pressure-based to flowrate-based. During
an actual CPB procedure, the arterial circuit pressure may vary from patient to patient,
vary over time, and vary depending on the blood viscosity, which itself can vary due to
hematocrit and temperature. A peristaltic pump will give the microdialysis operator more
control of the flow conditions within the device. During mock CPB circuit experiments, it
was also noted that the pressure gauges were very sensitive to the placements of the
circuit tubing and sampling manifold, since this inherently affects the head pressure in the
circuit. Therefore, relying on the circuit pressure readings to determine expected reservoir
flowrate may yield erroneous predictions.
The fabrication procedure should also be improved upon; more importantly, a
more reliable bonding method is needed. Currently, the benefit from using a low
viscosity epoxy is the ability to create a thin layer of epoxy for stamping, which
minimizes additional diffusion distances required for the analyte to cross over from the
reservoir channel to the perfusion channel. However, this low viscosity property also
increases the chances of the epoxy spreading into the channels as well as spreading to
membrane surfaces beyond the template dictated by the PDMS channels. Since each of
the perfusion channels are only 400 µm wide, the available diffusion area may decrease
significantly. Furthermore, the
Due to the epoxy’s transparent nature, especially since its thickness is only tens of
microns, it is difficult to visually see when epoxy spreads out beyond the intended

88
membrane areas or into the channels themselves. The only method to perform quality
control checks is to perform microdialysis experiments (e.g. dialyzing glucose) on a large
set of devices, of the same design, and compare the extraction efficiency results. If the
variance is small, poorly made devices can be spotted easily and the rest would be
deemed acceptable for actual CPB usage. If the variance is large, it may be difficult to
distinguish which devices are not built to specifications.
To improve the bonding performance, further research into dry bonding
techniques is necessary. Since titanium-dioxide-coated polycarbonate membranes have
been shown to provide excellent bonding strength in air, but not when exposed to liquids,
other combinations of thin film material and membrane material may overcome this
limitation.
Compared to currently available, commercial microdialysis probes, this proposed
device has better extraction efficiency performance, especially at high flowrates (~4
µl/min). Its in vitro design makes it less invasive for the patient and reduces the risk of
infections, whereas microdialysis probes are designed to be placed directly on tissue or in
ECF. Although it is beyond the scope of this project, this microdialysis device is intended
to work in conjunction with a microimmunoassay module (also a µTAS device) that can
continuously track the changing inflammatory protein markers, such as that created by
Yang et al. [16, 97] and currently being investigated by Sasso et al. [98-100]. The
microdialysis chip would therefore serve to continuously prepare a cell-free solution that
contains similar levels of analyte concentration as that in the blood.

89
Bibliography
1. Daly, R.C., et al., Fifty years of open heart surgery at the Mayo Clinic. Mayo Clin
Proc, 2005. 80(5): p. 636-40.
2. Perrault, L.P., et al., On-pump, beating-heart coronary artery operations in high-
risk patients: an acceptable trade-off? Ann Thorac Surg, 1997. 64(5): p. 1368-73.
3. Lukassen, P. [cited; Available from: http://www.mrtwee.nl/Perfusionist.htm.
4. Martin, R., et al., Hemolysis during cardiopulmonary bypass. J Cardiothorac
Anesth, 1989. 3(6): p. 737-40.
5. Vercaemst, L., Hemolysis in cardiac surgery patients undergoing
cardiopulmonary bypass: a review in search of a treatment algorithm. J Extra
Corpor Technol, 2008. 40(4): p. 257-67.
6. Hensel, M., et al., Hyperprocalcitonemia in patients with noninfectious SIRS and
pulmonary dysfunction associated with cardiopulmonary bypass. Anesthesiology,
1998. 89(1): p. 93-104.
7. Sistino, J.J. and J.R. Acsell, Systemic inflammatory response syndrome (SIRS)
following emergency cardiopulmonary bypass: a case report and literature
review. J Extra Corpor Technol, 1999. 31(1): p. 37-43.
8. de Mendonca-Filho, H.T., et al., Circulating inflammatory mediators and organ
dysfunction after cardiovascular surgery with cardiopulmonary bypass: a
prospective observational study. Crit Care, 2006. 10(2): p. R46.
9. Khabar, K.S., et al., Circulating endotoxin and cytokines after cardiopulmonary
bypass: differential correlation with duration of bypass and systemic
inflammatory response/multiple organ dysfunction syndromes. Clin Immunol
Immunopathol, 1997. 85(1): p. 97-103.
10. Moat, N.E., D.F. Shore, and T.W. Evans, Organ dysfunction and
cardiopulmonary bypass: the role of complement and complement regulatory
proteins. Eur J Cardiothorac Surg, 1993. 7(11): p. 563-73.
11. Westaby, S., Complement and the damaging effects of cardiopulmonary bypass.
Thorax, 1983. 38(5): p. 321-5.
12. Westaby, S., Organ dysfunction after cardiopulmonary bypass. A systemic
inflammatory reaction initiated by the extracorporeal circuit. Intensive Care Med,
1987. 13(2): p. 89-95.
13. Hsieh, Y.C., On-chip Microdialysis System with Flow-Through Glucose Sensing
Capabilities, in Dept. of Bioengineering. 2006, Pennsylvania State University.
14. Hsieh, Y.C. and J.D. Zahn, On-chip microdialysis system with flow-through
sensing components. Biosens Bioelectron, 2007. 22(11): p. 2422-8.

90
15. Yang, S., A. Undar, and J.D. Zahn, A microfluidic device for continuous, real time
blood plasma separation. Lab Chip, 2006. 6(7): p. 871-80.
16. Yang, S., A. Undar, and J.D. Zahn, Continuous cytometric bead processing within
a microfluidic device for bead based sensing platforms. Lab Chip, 2007. 7(5): p.
588-95.
17. Fung, Y.C., Stochastic flow in capillary blood vessels. Microvasc Res, 1973. 5(1):
p. 34-48.
18. Yen, R.T. and Y.C. Fung, Effect of velocity of distribution on red cell distribution
in capillary blood vessels. Am J Physiol, 1978. 235(2): p. H251-7.
19. Albelda, S.M., C.W. Smith, and P.A. Ward, Adhesion molecules and
inflammatory injury. FASEB J, 1994. 8(8): p. 504-12.
20. Andersen, L.W., et al., Presence of circulating endotoxins during cardiac
operations. J Thorac Cardiovasc Surg, 1987. 93(1): p. 115-9.
21. Benedetti, M., et al., Blood--artificial surface interactions during
cardiopulmonary bypass. A comparative study of four oxygenators. Int J Artif
Organs, 1990. 13(8): p. 488-97.
22. Cohn, L.H. and L.H. Edmunds, Cardiac surgery in the adult. 3rd ed. 2008, New
York: McGraw-Hill Medical. xx, 1704 p.
23. Cremer, J., et al., Systemic inflammatory response syndrome after cardiac
operations. Ann Thorac Surg, 1996. 61(6): p. 1714-20.
24. Gillinov, A.M., et al., Complement and neutrophil activation during
cardiopulmonary bypass: a study in the complement-deficient dog. Ann Thorac
Surg, 1994. 57(2): p. 345-52.
25. Gillinov, A.M., et al., Inhibition of neutrophil adhesion during cardiopulmonary
bypass. Ann Thorac Surg, 1994. 57(1): p. 126-33.
26. Gravlee, G.P., Cardiopulmonary bypass : principles and practice. 2nd ed. 2000,
Philadelphia: Lippincott Williams & Wilkins. xvi, 768 p.
27. Kirklin, J.K., et al., Complement and the damaging effects of cardiopulmonary
bypass. J Thorac Cardiovasc Surg, 1983. 86(6): p. 845-57.
28. Kirklin, J.W., et al., Studies in extracorporeal circulation. I. Applicability of
Gibbon-type pump-oxygenator to human intracardiac surgery: 40 cases. Ann
Surg, 1956. 144(1): p. 2-8.
29. Nilsson, L., L. Bagge, and S.O. Nystrom, Blood cell trauma and postoperative
bleeding: comparison of bubble and membrane oxygenators and observations on
coronary suction. Scand J Thorac Cardiovasc Surg, 1990. 24(1): p. 65-9.
30. Nilsson, L., et al., Bubble and membrane oxygenators--comparison of
postoperative organ dysfunction with special reference to inflammatory activity.
Scand J Thorac Cardiovasc Surg, 1990. 24(1): p. 59-64.
31. Utley, J.R. and E.A. Ashleigh, Pathophysiology and techniques of
cardiopulmonary bypass. 1982, Baltimore: Williams & Wilkins. xiv, 197 p.
32. van Velzen-Blad, H., et al., Cardiopulmonary bypass and host defense functions
in human beings: II. Lymphocyte function. Ann Thorac Surg, 1985. 39(3): p. 212-
7.
33. Lillehei, C.W., Controlled cross circulation for direct-vision intracardiac
surgery; correction of ventricular septal defects, atrioventricularis communis,
and tetralogy of Fallot. Postgrad Med, 1955. 17(5): p. 388-96.

91
34. Kirklin, J.W., et al., Intracardiac surgery with the aid of a mechanical pump-
oxygenator system (gibbon type): report of eight cases. Proc Staff Meet Mayo
Clin, 1955. 30(10): p. 201-6.
35. Utley, J.R., Cardiopulmonary bypass surgery. Curr Opin Cardiol, 1992. 7(2): p.
267-75.
36. Stoney, W.S., et al., Air embolism and other accidents using pump oxygenators.
Ann Thorac Surg, 1980. 29(4): p. 336-40.
37. Jakob, H., et al., In-vitro assessment of centrifugal pumps for ventricular assist.
Artif Organs, 1990. 14(4): p. 278-83.
38. Oku, T., et al., Hemolysis. A comparative study of four nonpulsatile pumps.
ASAIO Trans, 1988. 34(3): p. 500-4.
39. Lynch, M.F., D. Peterson, and V. Baker, Centrifugal blood pumping for open
heart surgery. Minn Med, 1978. 61(9): p. 536-8.
40. Wheeldon, D.R., D.W. Bethune, and R.D. Gill, Vortex pumping for routine
cardiac surgery: a comparative study. Perfusion, 1990. 5(2): p. 135-43.
41. Kress, D.C., et al., Pump-induced hemolysis in a rabbit model of neonatal ECMO.
ASAIO Trans, 1987. 33(3): p. 446-52.
42. Palder, S.B., et al., Prolonged extracorporeal membrane oxygenation in sheep
with a hollow-fiber oxygenator and a centrifugal pump. ASAIO Trans, 1988.
34(3): p. 820-2.
43. Moore, F.D., Jr., et al., The effects of complement activation during
cardiopulmonary bypass. Attenuation by hypothermia, heparin, and hemodilution.
Ann Surg, 1988. 208(1): p. 95-103.
44. Utley, J.R., Pathophysiology of cardiopulmonary bypass: current issues. J Card
Surg, 1990. 5(3): p. 177-89.
45. Elliott, M.J., Perfusion for pediatric open heart surgery. Semin Thorac
Cardiovasc Surg, 1990. 2(4): p. 332-40.
46. Kirklin, J.K., Prospects for understanding and eliminating the deleterious effects
of cardiopulmonary bypass. Ann Thorac Surg, 1991. 51(4): p. 529-31.
47. Parker, D.J., et al., Changes in serum complement and immunoglobulins following
cardiopulmonary bypass. Surgery, 1972. 71(6): p. 824-7.
48. Hirayama, T., et al., Evaluation of red cell damage during cardiopulmonary
bypass. Scand J Thorac Cardiovasc Surg, 1985. 19(3): p. 263-5.
49. Hoffman, J.F., Cation transport and structure of the red-cell plasma membrane.
Circulation, 1962. 26: p. 1202-13.
50. Kreel, I., et al., A syndrome following total body perfusion. Surg Gynecol Obstet,
1960. 111: p. 317-21.
51. Warren, J.B., A.J. Brady, and G.W. Taylor, Vascular smooth muscle influences
the release of endothelium-derived relaxing factor. Proc Biol Sci, 1990.
241(1301): p. 127-31.
52. Kilbridge, P.M., et al., Induction of intercellular adhesion molecule-1 and E-
selectin mRNA in heart and skeletal muscle of pediatric patients undergoing
cardiopulmonary bypass. J Thorac Cardiovasc Surg, 1994. 107(5): p. 1183-92.
53. Wilson, I., et al., Inhibition of neutrophil adherence improves postischemic
ventricular performance of the neonatal heart. Circulation, 1993. 88(5 Pt 2): p.
II372-9.

92
54. Haslett, C., et al., The pulmonary vascular sequestration of neutrophils in
endotoxemia is initiated by an effect of endotoxin on the neutrophil in the rabbit.
Am Rev Respir Dis, 1987. 136(1): p. 9-18.
55. Ratliff, N.B., et al., Pulmonary injury secondary to extracorporeal circulation. An
ultrastructural study. J Thorac Cardiovasc Surg, 1973. 65(3): p. 425-32.
56. Till, G.O., et al., Intravascular activation of complement and acute lung injury.
Dependency on neutrophils and toxic oxygen metabolites. J Clin Invest, 1982.
69(5): p. 1126-35.
57. Smith, P.L., et al., Cerebral consequences of cardiopulmonary bypass. Lancet,
1986. 1(8485): p. 823-5.
58. Sasaki, S., et al., Partial cardiopulmonary bypass in rats for evaluating ischemia-
reperfusion injury. ASAIO J, 1996. 42(6): p. 1027-30.
59. Dodds, A.W. and R.B. Sim, Complement : a practical approach. Practical
approach series. 1997, Oxford: IRL Press at Oxford University Press. xxi, 274 p.
60. Mondino, B.J., Y. Sidikaro, and H. Sumner, Anaphylatoxin levels in human
vitreous humor. Invest Ophthalmol Vis Sci, 1988. 29(7): p. 1195-8.
61. Schleuning, M., et al., Complement activation during storage of blood under
normal blood bank conditions. Effects of proteinase inhibitors and leukocyte
depletion. Blood, 1992. 79(11): p. 3071-5.
62. Hed, J., M. Johansson, and M. Lindroth, Complement activation according to the
alternate pathway by glass and plastic surfaces and its role in neutrophil
adhesion. Immunol Lett, 1984. 8(6): p. 295-9.
63. Webster, J.G., Encyclopedia of medical devices and instrumentation, Wiley-
Interscience: Hoboken, N.J.
64. Chaurasia, C.S., et al., AAPS-FDA Workshop White Paper: microdialysis
principles, application, and regulatory perspectives. J Clin Pharmacol, 2007.
47(5): p. 589-603.
65. Clough, G.F., Microdialysis of large molecules. AAPS J, 2005. 7(3): p. E686-92.
66. Schutte, R.J., S.A. Oshodi, and W.M. Reichert, In vitro characterization of
microdialysis sampling of macromolecules. Anal Chem, 2004. 76(20): p. 6058-63.
67. Plock, N. and C. Kloft, Microdialysis--theoretical background and recent
implementation in applied life-sciences. Eur J Pharm Sci, 2005. 25(1): p. 1-24.
68. Groth, L. and A. Jørgensen, In vitro microdialysis of hydrophilic and lipophilic
compounds. Analytica Chimica Acta, 1997. 355(1): p. 75-83.
69. Mary, S., et al., Assessment of the recovery of three lipophilic psoralens by
microdialysis: an in vitro study. International Journal of Pharmaceutics, 1998.
161(1): p. 7-13.
70. Patterson, S.L., K.A. Sluka, and M.A. Arnold, A novel transverse push-pull
microprobe: in vitro characterization and in vivo demonstration of the enzymatic
production of adenosine in the spinal cord dorsal horn. J Neurochem, 2001.
76(1): p. 234-46.
71. Huang, Q., B. Seibig, and D. Paul, Polycarbonate hollow fiber membranes by
melt extrusion. Journal of Membrane Science, 1999. 161(1-2): p. 287-291.
72. Bungay, P.M., P.F. Morrison, and R.L. Dedrick, Steady-state theory for
quantitative microdialysis of solutes and water in vivo and in vitro. Life Sci,
1990. 46(2): p. 105-19.

93
73. Bungay, P.M., et al., Microdialysis of dopamine interpreted with quantitative
model incorporating probe implantation trauma. J Neurochem, 2003. 86(4): p.
932-46.
74. Jacobson, I., M. Sandberg, and A. Hamberger, Mass transfer in brain dialysis
devices--a new method for the estimation of extracellular amino acids
concentration. J Neurosci Methods, 1985. 15(3): p. 263-8.
75. Ao, X. and J.A. Stenken, Microdialysis sampling of cytokines. Methods, 2006.
38(4): p. 331-41.
76. Lonnroth, P., P.A. Jansson, and U. Smith, A microdialysis method allowing
characterization of intercellular water space in humans. Am J Physiol, 1987.
253(2 Pt 1): p. E228-31.
77. Chefer, V.I., et al., Overview of brain microdialysis. Curr Protoc Neurosci, 2009.
Chapter 7: p. Unit7 1.
78. Larsson, C.I., The use of an "internal standard" for control of the recovery in
microdialysis. Life Sci, 1991. 49(13): p. PL73-8.
79. Scheller, D. and J. Kolb, The internal reference technique in microdialysis: a
practical approach to monitoring dialysis efficiency and to calculating tissue
concentration from dialysate samples. J Neurosci Methods, 1991. 40(1): p. 31-8.
80. Le Quellec, A., et al., Microdialysis probes calibration: gradient and tissue
dependent changes in no net flux and reverse dialysis methods. J Pharmacol
Toxicol Methods, 1995. 33(1): p. 11-6.
81. Lonnroth, P. and L. Strindberg, Validation of the 'internal reference technique' for
calibrating microdialysis catheters in situ. Acta Physiol Scand, 1995. 153(4): p.
375-80.
82. Janasek, D., J. Franzke, and A. Manz, Scaling and the design of miniaturized
chemical-analysis systems. Nature, 2006. 442(7101): p. 374-80.
83. Shuichi, S., Micro total analysis system (&mgr;TAS). Electronics and
Communications in Japan (Part II: Electronics), 1999. 82(2): p. 21-29.
84. de Jong, J., R.G. Lammertink, and M. Wessling, Membranes and microfluidics: a
review. Lab Chip, 2006. 6(9): p. 1125-39.
85. Tjerkstra, R.W., et al., Multi-walled microchannels: free-standing porous silicon
membranes for use in μTAS. Microelectromechanical Systems, Journal of,
2000. 9(4): p. 495-501.
86. Gielens, F.C., et al., Microsystem technology for high-flux hydrogen separation
membranes. Journal of Membrane Science, 2004. 243(1-2): p. 203-213.
87. Metz, S., et al., Polyimide microfluidic devices with integrated nanoporous
filtration areas manufactured by micromachining and ion track technology.
JOURNAL OF MICROMECHANICS AND MICROENGINEERING, 2004.
14(3): p. 324-331.
88. Song, S., A.K. Singh, and B.J. Kirby, Electrophoretic concentration of proteins at
laser-patterned nanoporous membranes in microchips. Anal Chem, 2004. 76(15):
p. 4589-92.
89. Hisamoto, H., et al., Chemicofunctional membrane for integrated chemical
processes on a microchip. Anal Chem, 2003. 75(2): p. 350-4.
90. Gao, J., et al., Integrated microfluidic system enabling protein digestion, peptide
separation, and protein identification. Anal Chem, 2001. 73(11): p. 2648-55.

94
91. Wang, P.C., J. Gao, and C.S. Lee, High-resolution chiral separation using
microfluidics-based membrane chromatography. J Chromatogr A, 2002. 942(1-
2): p. 115-22.
92. Duffy, D.C., et al., Rapid Prototyping of Microfluidic Systems in
Poly(dimethylsiloxane). Analytical Chemistry, 1998. 70(23): p. 4974-4984.
93. Whatman.
94. Chueh, B.H., et al., Leakage-free bonding of porous membranes into layered
microfluidic array systems. Anal Chem, 2007. 79(9): p. 3504-8.
95. Daniel, K.D., et al., Multi-reservoir device for detecting a soluble cancer
biomarker. Lab Chip, 2007. 7(10): p. 1288-93.
96. Trickler, W.J. and D.W. Miller, Use of osmotic agents in microdialysis studies to
improve the recovery of macromolecules. J Pharm Sci, 2003. 92(7): p. 1419-27.
97. Yang, S., Microfluidic Devices for On-line Monitoring of Clinically Relevant
Proteins During Cardiopulmonary Bypass Procedures, in Department of
Bioengineering. 2006, Pennsylvania State University.
98. Sasso, L., Zahn, J.D. Continuous microfluidic biosensing with conjugated
paramagnetic beads. in 2008 ASME IMECE. Boston, Mass.
99. Sasso, L., Zahn, J.D. Continuous microfluidic immunosensing with antibody
conjugated paramagnetic beads. in MicroTAS 2008, The Twelth International
Conference on Miniaturized Systems for Chemistry and Life Sciences. San Diego,
CA.
100. Sasso, L., Zahn, J.D., Undar, A. A microfluidic immunosensor to monitor systemic
inflamation during CPB. in Fifth International Conference on Pediactric
Mechanical Circulatory Support Systems and Pediactric Cardiopulmonary
Perfusion. 2009. Dallas, Texas.

95
Appendix A: Preliminary Experiments
Preliminary experiments were conducted using channels with simple single-
channel devices. These were done as proof-of-concept tests of various bonding methods
and as practice for sample collection and analysis techniques. The PDMS device
consisted of a single channel, 2 mm wide, 12 mm long, and 100 µm deep, for both the
reservoir and perfusion sides. A polycarbonate membrane with 100 nm pore sizes were
used. A syringe pump was used to control each of the channel’s flowrate.
Figure A. 1: Various orientations of the channels: (left) reservoir channel is directly over perfusion
channel; (middle) reservoir channel is perpendicular to perfusion channel; and (right) the two
channels are offset laterally by one-half the channel width. Arrows denote direction of flow.

96
First, the “parallel” configuration was used, as shown in Fig. A.1, where both
channels are aligned directly over one another. The reservoir solution consisted of a 1.27
g/l glucose/PBS mixture and pumped at a flowrate 40 µl/min while the perfusate solution
was pumped at various flowrates, as shown in Fig. A.2.
0
10
20
30
40
50
60
70
80
90
100
0 1 2 3 4 5 6 7 8 9
Perfusion Flowrate (uL/min)
Relative Recovery %
Experimental
Theoretical
Equilibrium
Figure A. 2: Glucose recovery at the perfusion outlet shown in Fig. A.1 (left), “parallel”
configuration.
The theoretical relative recovery values in Fig. A.2 were computed using the
membrane permeability value, K0, determined by KaleidaGraph’s (Synergy Software,
Reading, PA) regression analysis of the experimental data itself. Thus, the resulting K0
value is assumed to be only relevant to each own respective data set. The result clearly
shows that the change in perfusion flowrate has little effect on the relative recovery,
perhaps signifying that the two solutions are crossing through the membrane from their
respective channels and mixing with one another. However, the two concentrations do
not reach the theoretical equilibrium concentration value (shown in Fig. A.2), which

97
assumes that both solutions have infinite time for analytes to cross the membrane. One
should also note that, under this configuration, the membrane does not remain flat and
parallel to the plane where the two PDMS layers come in contact. In fact, it bows in the
shape of a “U” due to the relatively wide and unsupported width of the channel. This
results in an unexpected change in effective channel depth, thereby affecting the
hydraulic pressure within the channel. This configuration also places the inlet and outlet
holes of each channel, directly over the other channel. This does not allow the flow to
stabilize first, before diffusion across the membrane is supposed to occur. In order to
remedy these two problems, alternative alignment configurations were used, such as the
“cross” and “shifted parallel” configurations shown in Fig. A.1 (middle and right).
In the cross configuration, the two channels are oriented perpendicular from one
another, thereby decreasing the diffusion area, but also limiting the amount of bowing of
the membrane. This setup also allows the flow to stabilize in its respective channel before
the fluid reaches the diffusion area. The theoretical and experimental values were
calculated using the same method as in the parallel configuration and shown in Fig. A.3.
As one can see, the relative recovery values are significantly lower than that of the
parallel configuration due to the decreased diffusion area. However, the experimental
values do follow an exponential trend, as noted by the agreement with the expected
values in Fig. A.3. The plot also demonstrates that bulk mixing is not occurring or is
negligible.

98
0
10
20
30
40
50
60
70
80
90
100
0 1 2 3 4 5 6 7
Perfusion Flowrate (uL/min)
Relative Recovery %
Experimental
Theoretical
Equilibrium
Figure A. 3: Glucose recovery at the perfusion outlet shown in Fig. A.1 (middle), “cross”
configuration.
Finally, the shifted parallel configuration was used also to limit bowing across the
width of the membrane, by shortening the width of the diffusion area, and to limit the
deleterious effects of the inlet and outlet holes in the PDMS channel to be so close to the
diffusion area. Once again, the experimental values are shown to follow an exponential
trend and does not seem to experience mixing between the two channels, as shown in Fig.
A.4.

99
0
20
40
60
80
100
120
0 2 4 6 8 10
Recovery %
Perfusion Flowrate (uL/min)
Experimental
Theoretical
Equilibrium
Figure A. 4: Glucose recovery at the perfusion outlet shown in Fig. A.1 (right), “shifted parallel”
configuration.

100
Appendix B: Matlab Code
clear all; display(' '); display(' '); display(' ');display(' '); display(' '); display(' '); display('********************************************************** '); % display(datestr(now)); display('********************************************************** '); display(' '); Width_Blood_um = input('Width of blood channel (um): '); Width_Blood_m = Width_Blood_um .* 10^-6; length_Width_Blood = length(Width_Blood_m); Height_Blood_um = input('Height of blood channel (um): '); Height_Blood_m = Height_Blood_um .* 10^-6; length_Height_Blood = length(Height_Blood_m); Width_Perfus_um = input('Width of perfus channel (um): '); Width_Perfus_m = Width_Perfus_um .* 10^-6; length_Width_Perfus = length(Width_Perfus_m); Height_Perfus_um = input('Height of perfus channel (um): '); Height_Perfus_m = Height_Perfus_um .* 10^-6; length_Height_Perfus = length(Height_Perfus_m); Length_mm = input('Length of channel (mm): '); Length_m = Length_mm .* 10^-3; N = input('Number of channels: '); Tube_rsrv_inlet_in = input('What is the length of PE-10 tubing for the Reservoir Inlet (in): '); Tube_rsrv_inlet_m = Tube_rsrv_inlet_in.*.0254; % convert in to meters length_Tube = length(Tube_rsrv_inlet_m); display(' '); Q_perf_uLmin = input('What is perfusion flowrate (uL/min): '); Q_perf_in = sym(Q_perf_uLmin.*1.667e-11); length_Q_perf = length(Q_perf_in);

101
P_CPB_mmHg = input('What is the CPB pump pressure into reservoir (mmHg): '); P_CPB_Pa = sym(P_CPB_mmHg.*133.3); length_P_CPB = length(P_CPB_Pa); Pore_diam_um = input('Pore size (um): (0.05, 0.08, 0.1, 0.2, 0.4, 0.6, or 0.8) = '); length_Pore = length(Pore_diam_um); % FOR LOOP in order of importance for analysis % Pore Size >> Blood Height >> Blood Width >> Perfus Height >> Perfus Width >> % Tube L >> CPB Press >> Q_perfus % END string_varying_variables = input('Note: ','s'); for index_Pore = 1:length_Pore for index_Height_Blood = 1:length_Height_Blood for index_Width_Blood = 1:length_Width_Blood for index_Height_Perfus = 1:length_Height_Perfus for index_Width_Perfus = 1:length_Width_Perfus for index_Tube = 1:length_Tube for index_CPB = 1:length_P_CPB for index_Q_perfus = 1:length_Q_perf
ResistCalc_AUTO(Width_Blood_m(index_Width_Blood),... Height_Blood_m(index_Height_Blood),... Width_Perfus_m(index_Width_Perfus),... Height_Perfus_m(index_Height_Perfus),... Tube_rsrv_inlet_m(index_Tube),... Q_perf_in(index_Q_perfus),... P_CPB_Pa(index_CPB),... Pore_diam_um(index_Pore),... Length_m, N, string_varying_variables);
end end end end end end end end display(' '); display('Data has been written to Excel file'); display('^^^^^^^^^^^^ E N D ^^^^^^^^^^^^'); display('==============================='); display(' ');display(' ');display(' '); clear all

102
function [] = ResistCalc_AUTO(Width_Blood_m_fun, Height_Blood_m_fun, Width_Perfus_m_fun, Height_Perfus_m_fun, Tube_rsrv_inlet_m_fun, Q_perf_in_fun, P_CPB_Pa_fun, Pore_diam_um_fun, Length_m_fun, N_fun, string_varying_variables_fun) % Declare Symbolic Variables syms P_rsrv Resist_rsrv Q_rsrv_in Q_pore P_perf Resist_perf Resist_pores syms Resist_tube dyn_visc_blood = 3.5e-3; %N-s/m^2 at 35C dyn_visc_perf = 1e-3; %N-s/m^2 dyn_visc_plasma = 1.6e-3; % Calculate Pore Resistance pore_boolean = 0; while (pore_boolean == 0) if Pore_diam_um_fun == .05 Pore_density = 6e8*(100)^2; Pore_thk = 6e-6; pore_boolean = 1; elseif Pore_diam_um_fun == .08 Pore_density = 6e8*(100)^2; Pore_thk = 6e-6; pore_boolean = 1; elseif Pore_diam_um_fun == .1 Pore_density = 3e8*(100)^2; % converts from per cm^2, to per m^2 Pore_thk = 6e-6; % [m] pore_boolean = 1; elseif Pore_diam_um_fun == .2 Pore_density = 3e8*(100)^2; Pore_thk = 10e-6; pore_boolean = 1; elseif Pore_diam_um_fun == .4 Pore_density = 1e8*(100)^2; % converts from per cm^2, to
per m^2 Pore_thk = 10e-6; % [m] pore_boolean = 1; elseif Pore_diam_um_fun == .6 Pore_density = 3e7*(100)^2; Pore_thk = 10e-6; pore_boolean = 1; elseif Pore_diam_um_fun == .8 Pore_density = 3e7*(100)^2; % converts from per cm^2, to

103
per m^2 Pore_thk = 9e-6; % [m] pore_boolean = 1; else display(' '); display('Please enter correct pore size') display(' '); display(' '); end %if statement end % while statement Pore_diam_m = Pore_diam_um_fun*10^-6; % converts pore size diameter
from [um] to [m] Diff_Area_m2 = N_fun*Length_m_fun*min(Width_Perfus_m_fun,
Width_Blood_m_fun); % area is based on whichever width dimension is smallest
Num_Pores = Pore_density*Diff_Area_m2; Num_Pores; Fudge_rsrv_sumseries = 0; Fudge_perf_sumseries = 0; %%% additional fudge factor for Rectangular Duct Resistances %%% (simplified equation does not apply due to low aspect ratio
for ii=1:2:13 Fudge_rsrv_sumseries = Fudge_rsrv_sumseries +
(1/ii^5)*tanh(ii*pi*Width_Blood_m_fun/(2*Height_Blood_m_fun));
Fudge_perf_sumseries = Fudge_perf_sumseries + (1/ii^5)*tanh(ii*pi*Width_Perfus_m_fun/(2*Height_Perfus_m_fun));
end Fudge_rsrv = (1 - Height_Blood_m_fun/Width_Blood_m_fun *
(192/pi^5*Fudge_rsrv_sumseries))^-1; Fudge_perf = (1 - Height_Perfus_m_fun/Width_Perfus_m_fun *
(192/pi^5*Fudge_perf_sumseries))^-1; % Fudge_rsrv = 1; % Fudge_perf = 1;
%>>>>>>>>>>>>> SYMBOLIC EQUATIONS <<<<<<<<<<<<<<<<< eq1 = (P_CPB_Pa_fun-P_rsrv)/Resist_tube - P_rsrv/Resist_rsrv –
Q_pore; eq2 = Q_perf_in_fun + Q_pore - P_perf/Resist_perf;
eq3 = Q_pore - (P_rsrv/2-P_perf/2)/Resist_pores;
eq4 = Resist_rsrv - (12*dyn_visc_blood*Length_m_fun/
(Width_Blood_m_fun*Height_Blood_m_fun^3)/N_fun)*Fudge_rsrv;

104
eq5 = Resist_perf – 12 * dyn_visc_perf*Length_m_fun/
(Width_Perfus_m_fun*Height_Perfus_m_fun^3)/N_fun* Fudge_perf;
eq6 = Resist_pores - 8*dyn_visc_plasma*Pore_thk/(pi*
(Pore_diam_m/2)^4) / Num_Pores; eq7 = Resist_tube - 8*dyn_visc_blood*Tube_rsrv_inlet_m_fun/
(pi*(0.28e-3/2)^4);
eq8 = Q_rsrv_in - (P_CPB_Pa_fun-P_rsrv)/Resist_tube; S = solve(eq1, eq2, eq3, eq4, eq5, eq6, eq7, eq8); %>>>>>>>>>>>>> SYMBOLIC EQUATIONS <<<<<<<<<<<<<<<<< format short eng P_rsrv = single(S.P_rsrv); % Pa P_perf = single(S.P_perf); % Pa Resist_rsrv = single(S.Resist_rsrv); Resist_perf = single(S.Resist_perf); Resist_pores = single(S.Resist_pores); Resist_tube = single(S.Resist_tube); Q_rsrv_in = single(S.Q_rsrv_in)/1.667e-11; % uL/min Q_perf_in_fun = single(Q_perf_in_fun)/1.667e-11; % uL/min Q_pore = single(S.Q_pore)/1.667e-11; % uL/min Q_rsrv_out = single(S.P_rsrv/S.Resist_rsrv)/1.667e-11; % uL/min Q_perf_out = single(S.P_perf/S.Resist_perf)/1.667e-11; % uL/min P_CPB_mmHg_fun = single(P_CPB_Pa_fun)/133.3; note = string_varying_variables_fun;
% % % % % % % % % % % % % % % % % % % % % % % % % % % % % % % % % % % % % S T O R I N G D A T A I N E X C E L % %
% % % % % % % % % % % % % % % % % % % % % % % % % % % % % % % % %
Header_title = {'0','Note','Reservoir Channel Width (um)','Reservoir Channel Height (um)',... 'Perfusion Channel Width (um)','Perfusion Channel Height (um)','Channel Length (mm)',... 'Number of Channels','Reservoir Tubing Length (in)','Pore Size (um)',... 'Perfusion Flow Rate (uL/min)','CPB Inline Pressure (mmHg)',...

105
'Reservoir Pressure (Pa)','Perfusion Pressure (Pa)','Reservoir Channel Resistance',... 'Perfusion Channel Resistance','Pore Resistance','Reservoir Tubing Resistance',... 'Reservoir Flowrate-In (uL/min)',... 'Pore Flowrate (uL/min)','Reservoir Flowrate-Out (uL/min)',... 'Perfusion Flowrate-Out (uL/min)', 'Perf Flowrate Rec%'}; xlswrite('VolumeCalc_AUTO',Header_title,'Sheet1'); % % targetSheet = worksheets.Item('Sheet1'); % targetSheet.Activate; % % Check Excel sheet to make sure where data was last written, prevents % % writing over previous data [numrow, numcol] = size(xlsread('VolumeCalc_AUTO','Sheet1')); row = num2str(numrow + 1); col = 'A'; location = [col row]; write_excel = {0,note, Width_Blood_m_fun*1e6,
Height_Blood_m_fun*1e6, Width_Perfus_m_fun*1e6,... Height_Perfus_m_fun*1e6, Length_m_fun*1e3, N_fun,
Tube_rsrv_inlet_m_fun/.0254, Pore_diam_um_fun,... Q_perf_in_fun, P_CPB_mmHg_fun, P_rsrv, P_perf, Resist_rsrv, Resist_perf, Resist_pores, Resist_tube, Q_rsrv_in, Q_pore, Q_rsrv_out, Q_perf_out, Q_perf_out/Q_perf_in_fun*100};
xlswrite('VolumeCalc_AUTO',write_excel,'Sheet1',location); % display(' '); % display('Data has been written to Excel file'); % display('^^^^^^^^^^^^ E N D ^^^^^^^^^^^^'); % display('==============================='); % display(' ');display(' ');display(' '); % clear all; end % function







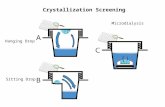



![Improvement of the Mechanical Stability of Microdialysis Catheters · 2016-02-09 · The next step in the development of microdialysis was when Urban Ungerstedt [3] introduced a hollow](https://static.fdocuments.us/doc/165x107/5f2bf162a4336743450d5a4a/improvement-of-the-mechanical-stability-of-microdialysis-2016-02-09-the-next-step.jpg)







