CGI INITIATIVE FOR COLLABORATIVE GOVERNMENT’S · digital white paper, capturing best practices,...
Transcript of CGI INITIATIVE FOR COLLABORATIVE GOVERNMENT’S · digital white paper, capturing best practices,...

CGI INITIATIVE FOR COLLABORATIVE GOVERNMENT’S
spring 2013

Leadership Interviews
The CGI Initiative for Collaborative Government’s Leadership executive journal gives voice to top senior executives who are addressing the most important issues confronting the United States and the globe. These interviews feature practical management approaches and insights that are applicable across the government, private and nonprofit sectors.
Reports
Together with leading academic experts, the CGI Initiative publishes reports and Q&As to provide practical, actionable ideas about top-of-mind challenges for government executives on topics ranging from job creation to large IT
project management. EventsThe CGI Initiative brings together leaders from government, academia and associations
for executive dialogues on critical issues, including budget savings, information
security, data sharing, transparency, health IT and more.
Webinars and Digital White Papers
The CGI Initiative has hosted webinars
featuring leaders spanning the U.S. Army, Recovery Board, Energy Department and the Environmental Protection
Agency. From these webinars, the initiative produces online Executive Guides, a form of digital white paper, capturing best practices, lessons learned and carefully chosen links.
Videos, E-Newsletters
Evolving continuously to connect most effectively with government executives, the CGI Initiative uses video to deliver expert analysis quickly and directly on the Web. Using cutting-edge publishing technology, the initiative creates and delivers a daily e-newsletter, Collaborative Government Today.
We focus on helping government leaders collaborate effectively while retaining
strategic alignment, control and accountability. Products, including leadership
interviews, reports, in-person events, webinars, e-newsletters, videos, blog posts
and digital white papers, bring together the initiative’s mission and expert analysis to
provide thoughtful, incisive, ready-to-use information.
www.collaborativegov.org
The CGI Initiative for Collaborative Government

NoteEditor’s
Welcome to the Winter 2013 issue of Leadership, the CGI
Initiative for Collaborative Government’s executive journal.
Leadership gives voice to thoughtful executives who are
creatively and effectively addressing the most important
issues confronting the United States and the world. Each
edition focuses on a theme that challenges leaders of
diverse organizations and features profiles of executives
whose practical insights and observations are borne of
success and are applicable across the government, private
and nonprofit sectors.
This edition of Leadership examines health care, one
of the country’s biggest challenges. Specifically, we look
at how big data and data analytics are key parts of the
future of health care. To illustrate that, we gathered the
perspectives of leaders across domestic and foreign
government, industry and academia. To set the stage, we
start with a candid Q&A with Brig. Robin Cordell, head
of medical strategy and policy for the United Kingdom’s
Defence Medical Services. Other thought leaders include:
• Dr. Mark Chassay, deputy executive commissioner for
the Office of Health Policy and Clinical Services, Texas
Health and Human Services Commission.
• David Cordani, president and chief executive officer,
Cigna.
• Dr. Robert Jesse, principal deputy undersecretary for
health, Veterans Health Administration.
• Tony Trenkle, director and chief information officer,
Centers for Medicare and Medicaid Services.
• Dr. Michael Wagner, president and CEO, Tufts Medical
Center.
I want to thank them for taking time out of their difficult
schedules to share with us their ideas on data-driven
health care. Thank you to each of you for the insight and
dedication to mission that you shared with us.
This issue also includes analysis on our theme from CGI
Initiative Fellows Dr. James Peake and Dr. John Loonsk,
who have served as advisers on this project. Dr. Peake was
secretary of the Department of Veterans Affairs from 2007
to 2009 and U.S. Army surgeon general from 2000 to 2004.
He retired from military service with a rank of lieutenant
general. Dr. Loonsk is the former director of interoperability
and standards at the Office of the National Coordinator for
Health Information Technology. He also was the associate
director for informatics at the Centers for Disease Control
and Prevention.
Finally, a special thank you to CGI Initiative staff
members Andrew McLauchlin, Sarah Lindenau and
John Adams for managing and guiding this project
to completion. Andrew’s leadership from starting this
publication through this latest edition has been an
important contribution. Also thank you to our editorial
partner, 1105 Media.
Molly O’Neill
Senior Fellow
CGI Initiative for Collaborative Government
S p r i n g 2 0 13 | COLLABOrATiVEgOV.Org/LEAD | Leadership 1

Leadership
4 Thinking BigDecoding big data’s health care potential depends on leadership, technology, and collaboration.
SPRING 2013
In This Issue
12 Carrying the Torch Dr. Mark Chassay Texas Health and Human Services
Commission Dr. Mark Chassay teams data with
policy for Texas health care delivery
8 Global Collaboration Brigadier Robin Cordell
Defence Medical Services, UK Brigadier Robin Cordell instills a
spirit of collaboration within the UK’s Defence Medical Services
2 Leadership | CGI INITIATIVE FOR COLLABORATIVE GOVERNMENT | S P R I N G 2 0 13

20 Setting the Pace David Cordani
Cigna Partnerships and embracing
uncertainty underscore Cigna CEO’s accountable care approach
4 Thinking BigDecoding big data’s health care potential depends on leadership, technology, and collaboration.
In This Issue
36 On a Mission Tony Trenkle,
Centers for Medicare and Medicaid Services
Tony Trenkle advances health reform through technology modernization
28 Tools of the Trade Dr. Robert Jesse Veterans Health Administration Dr. Robert Jesse focuses VHA
health care fixes on patient needs
44 Making the Grade Dr. Michael Wagner
Tufts Medical Center Dr. Michael Wagner helps Tufts
Medical Center deliver on health care promises
S P R I N G 2 0 13 | COLLABORATIVEGOV.ORG/LEAD | Leadership 3

The health technology community is buzzing about big data — and for good reason: with this emerging technology come big promises of being able to access, integrate and apply different types of data to establish the full picture of a patient and then mesh that context with health system data to create more efficient, patient-friendly outcomes.
Volume is a hallmark of big data, with criti-cal information carved from terabytes and pet-abytes of data. But in health, big data is also big because it documents and manages com-plex and vast health concepts. It is big when it begins to describe intricate parts of a living en-tity, such as a human genome. It is big when it begins to document the comprehensive clinical state of an individual. It is big when it articulates the research lessons that person holds for the broader population.
With these advancements come big challenges, which, while frustrating, also have the potential to foster creative solutions and provide an op-portunity to rethink and renovate the health care experience for everyone involved, from individual patients to entire populations and from doctors to major medical health care providers.
Imagine the Possibilities Big data-enabled capabilities are rapidly becom-ing ingrained in health care. Doctors use digitized radiologic images, microscopic sections, free-text operative notes and discharge summaries. Data characterizing the full patient status can help protect against drug and allergic reactions, for example, or adjust medication dosage for ge-netic ability to metabolize. Big data can make for more efficient scheduling of operating rooms by
Thinking Big Decoding big data’s health care potential
By Drs. John Loonsk anD James Peake
4 Leadership | CGI INITIATIVE FOR COLLABORATIVE GOVERNMENT | s p R I N G 2 0 13

sequencing cases and ensuring the right instru-ments are available. For recovering patients, it can predict the date of hospital release and coor-dinate people involved in discharge: pharmacies, rehab services and caregiver pickup.
But big data can do more than give a better view of the status quo. Predictive analytics use big data to paint a picture of what could be. Big data is central to describing, managing and mea-suring the road between the two. It underlies our ability to improve patients’ safety, maximize hos-pital resources, optimize hospital stays and de-crease the likelihood of readmission. Data used to provide individual feedback can even mod-ify patients’ behavior and guide them toward a healthier lifestyle. At the same time, big data can boost efficiency and cut costs.
Breaking Down Walls
This new realm of data possibilities requires a greater integration of data inside hospital walls and beyond and new ways of thinking. It’s not enough to implement electronic health records (EHRs) that convert existing health processes. Workflows and processes must change to take advantage of the new capabilities.
Big data is eroding some traditional barriers to data sharing, but this reform is also about chang-ing mind-sets, which is never simple. It is still easier to follow the traditional course and defer to proprietary business concerns, legal postures and distrust among health care constituencies. Incentives are only slowly being realigned to hold providers and health systems accountable for care outcomes, but expectations and policy are advancing rapidly.
EHR Spending 2009-2015
10
8
6
4
2
0
(in b
illio
ns)
2009 20152010 2011 2012 2013 2014
$2.18 billion
$6.05 billion
EStimatEd compound annual gRowtH RatE of 18.1 pERcEnt
Source: University of Illinois at Chicago
s p R I N G 2 0 13 | COLLABORATIVEGOV.ORG/LEAD | Leadership 5

Most health-related data is still in paper form and even when it has been digitized, it often lacks a high level of structure, making meaningful and consistent aggregation difficult. Technology con-tinues to advance, however, providing new tools to deal with these new data problems. Big data tools offer ways to store and process greater quantities of data faster than ever. They can also help set standards. In a big data construct, ap-plying analytics to both structured and unstruc-tured data is promising.
Navigating ObstaclesFrom a technical standpoint, sharing data can be challenging. Specifically, no standards exist for digital data, health information technology incen-tives vary and most existing systems were set up to stand alone.
Standardizing data is difficult because dif-ferent health specialties have different require-ments. For instance, a medical center might have specialists in endocrinology and anesthesiology with different workflows and information needs.
A commercial solution doesn’t cut it, and open-source software is not a panacea, either. Instead, standardization requires management and inte-gration into the ecosystem.
Beyond technology, the medical community must broaden its perspective to embrace the idea that big data means health care is about more than caring for individual patients. It’s about tak-ing care of populations. Because data gleaned from one person can be applied to others through predictive analytics, health professionals can re-verse it and use population data to help individual patients. To do this, different data sources, stor-ing and managing large amounts, must be linked in new ways to deliver new information. This also means recognizing that bringing together large data sets is an important step in improving health care — but it is not the solution. Solutions and improvements will be made when we begin using this data to rethink fundamental elements of health care.
If we can surmount these technical and behav-ioral challenges to unleash the data, make it avail-
Dr. Loonsk
John Loonsk, M.D., FACMI,
is a CGI Initiative for Collab-
orative Govern-
ment Fellow with
experience in
health information
technology span-
ning government,
commercial and
academic environ-
ments. In 2009,
Loonsk was appointed chief
medical officer at CGI.
Previously, he held the
position of director of in-
teroperability and standards
at the Office of the
National Coordinator
for Health IT. In this
role, Loonsk led the
architecture of the
Nationwide Health
Information Network
and advanced the
interoperability pro-
cesses of the American Health
Information Community.
Loonsk also was associate
director for informatics at the
Centers for Disease Control
and Prevention. There, he
led the creation of the Public
Health Information Network.
He was also instrumental in
designing the National Elec-
tronic Disease Surveillance
System and initiating the
BioSense program.
6 Leadership | CGI INITIATIVE FOR COLLABORATIVE GOVERNMENT | s p R I N G 2 0 13

able in electronic formats and begin the analysis process, health care outcomes will improve and costs will diminish.
The Path ForwardAchieving the potential of big data will take big leadership. Although interoperability will be elusive for many health systems and programs in the near term, bringing together unstructured data, connect-ing it with existing structured data and analyzing all of that information with big data tools will allow for quick, significant patient and population benefits. The push for EHRs and the combination of clinical and payment data mean organizations are going to have a lot of data to deal with. The biggest prob-lem they face is how to harness the capability of big data to push health care forward faster.
The proper approach is a combination of actions focused on the justified concerns of people and businesses. We must apply new big data tech-nology options incrementally, acknowledging the need for an extended — perhaps perpetual — pe-riod when organizations will operate with a hybrid
of older and new data sources and systems. The key is creating a convergence model to pull all the pieces together.
Another point to consider is cloud technology, which can efficiently process large amounts of data at commodity pricing. We also need to encourage mobile communication and website redesign to ef-fectively deliver information in a way that consumers want to see it and use it — and can understand it. This might include a hosted analytical tool by which individuals can model the effects of their behaviors.
IT solutions can join data and analytics, but a suc-cessful health care environment requires improve-ment in collaboration and partnership among all stakeholders. As we begin to gain more access to these large data sets, we must remember that avail-ability and storage are not the end game. We will fall short if we do not use the data to ask questions that will improve health care. The promise of big data and emerging analytic tools is here now, and the American health care system needs to com-mit to using this new wealth of data in new ways to achieve significant improvements in health care. n
Dr. Peake
James Peake, M.D., is a CGI Ini-
tiative for Collaborative Govern-
ment Fellow. In December 2009,
Peake was appointed senior
vice-president for the health
industry at CGI.
Prior to joining CGI, Peake was
nominated by President George
W. Bush to be secretary of the
Veterans Affairs Department on
Oct. 30, 2007, and unanimously
confirmed by the Senate on
Dec. 14 of that year. He served
from December 2007 through
January 2009. Peake was the
principal advocate for veterans in
the U.S. government
and directed the na-
tion’s second largest
Cabinet department,
responsible for a
nationwide system of
health care services,
benefits programs
and national cemeter-
ies for America’s veterans and
dependents.
He previously was U.S. Army
Surgeon General from 2000 to
2004. As such, he commanded
50,000 medical per-
sonnel and 187 Army
medical facilities
worldwide. Before
that, he served as
commanding gen-
eral of the U.S. Army
Medical Department
Center and School,
one of the largest medical train-
ing facilities in the world with
30,000 students annually.
s p R I N G 2 0 13 | COLLABORATIVEGOV.ORG/LEAD | Leadership 7

Brigadier Robin Cordell is responsible to the
Surgeon General for Defence Medical Ser-
vices (DMS) strategy and medical policy, in-
cluding the DMS Information Strategy, and
is co-chair of the US-UK Task Force working
group on mental health. He is also the mili-
tary representative on the Royal British Le-
gion chaired Medical Advisory Group.
The DMS is staffed by nearly 7,000 uni-
formed medical and dental personnel from
the Naval Service, British Army and Royal
Air Force. It provides health care to approxi-
mately 196,000 servicemen and women en-
suring they are medically fit for duty.
Cordell was previously Allied Command
Operations Medical Advisor where he was
responsible for the medical direction for all
NATO operations, the International Secu-
rity Assistance Force (ISAF) mission in Af-
ghanistan being the main focus. He was first
commissioned as an infantry officer in 1977,
serving in Belize prior to medical school.
Brigadier Robin Cordell
Head of Medical Strategy and Policy, Headquarters
Surgeon General, Defence Medical Services, UK
PersPectives from
8 Leadership | CGI INITIATIVE FOR COLLABORATIVE GOVERNMENT | s p R I N G 2 0 13

Q. the Defence Medical services
moved from a provisional model by
the Army, Navy and Air Force inde-
pendently, to a unified model, and
providing an electronic medical re-
cord for its patients. What are some
of the hurdles you are facing?
A. The main challenge has been a cul-
tural one. moving away from a Service
“stovepipe” system required a change
in emphasis. We moved from using
electronic information systems that
were different in each Service, con-
nected as local networks within each
primary health care center and used al-
most exclusively for health care record
management, to a Defence medical
Services - wide system that allows data
capture to improve health care delivery.
At the same time, it still supports record
keeping and clinical decision making.
The challenge was to move people
from the independent provider way of
thinking, entering data in the way that
suited their individual preference, to a
system where we would require them to
enter data in a standard coded way that
is easily analyzed. By actually looking
at the codings from consultations, you
can build a picture of the health issues
that affect our people and how we can
prevent ill health.
This single electronic medical record
is the central spine for our health infor-
mation system. This allows the health
care provider access to those records
from anywhere in the world, in perma-
nent bases and on military operations.
Q. How did you convince providers
to move from a medical model to a
public health model?
A. It was difficult at first. What worked
was forming user groups so that we
were able to show the benefits to our
patients without having to take a top-
down approach. Providers found it use-
ful to have additional health information,
particularly in the military context. Hav-
ing that detailed information allows us
to advise commanders on how to pre-
vent illness and injury, which is better
than having to manage the injury after it
occurs. We therefore got the message
across: “This is the way you can best
help our patients. We can provide in-
formation that you can then use to help
prevent illness and injury, but this all de-
pends on you using coding in consulta-
tions in a consistent way.”
The other benefit is improved health
care quality. Within the UK’s National
Health Service we have a number of
measures, called quality framework in-
dicators. If civilian doctors make those
targets they get additional payments as
an incentive. The motivation for military
doctors is to demonstrate the quality of
the health care they provide is just as
good or better. The psychology of this
is that professional pride takes over
and they want to do better. Being one
of the best performers is motivational.
Q. As head of medical strategy and
policy for the Defence Medical ser-
vices, you play a significant role
in transformation and managing
change. What would you consider
some of your major achievements
in this area? What would you say are
the biggest challenges?
A. As in the United States, each of the
UK Armed Services is proud of their
traditions and is accustomed to oper-
ating a certain way. We are in the pro-
cess of implementing the new Defence
Primary Health care structure, which
will bring together uniformed and ci-
vilian medical staff delivering primary
health care in the UK and in the firm
Base overseas. This brings benefits
of scale, and therefore efficiency, but
does mean a change in approach to
some degree. from our experience on
deployed operations which are almost
all jointly delivered, and have delivered
truly excellent results, this unified ap-
proach will deliver primary health care
more effectively and more consistently
across Defence.
The key to successful transformation
is two-fold. The first is for all those who
need to make this happen to agree and
strive toward a vision that all provid-
ers can buy into. This is to deliver the
best possible health care wherever our
people are. The second is to build a new
culture that embodies the vision.
Q. You talk about collecting and
analyzing more data to deliver bet-
ter care to the patients. How is this
progressing?
A. It is happening now through the De-
fence medical Information Capability
Program (DmICP). We have introduced
templates which automatically code the
diagnosis and treatments given to pa-
tients. It has taken some time, but we
are now getting some good information
out so we can compare practices with
each other from a quality point of view.
Q. the Defence Medical services
provides a range of services in many
s p R I N G 2 0 13 | COLLABORATIVEGOV.ORG/LEAD | Leadership 9

different facilities inside and outside
the UK. it’s a very collaborative en-
vironment. What is your approach
to collaboration? How do you coor-
dinate care and share data with the
various stakeholders?
A. Placing the focus on our core outputs
allows the Defence medical Services
and its stakeholders to share a common
purpose and vision. These include ad-
vice to commanders on health threats
and how the risk of ill health and injury
might be managed, and the provision of
world-class military health care focused
on optimal patient outcome.
Shared values are important. In the
Cold War era, where large numbers of
casualties were expected, the empha-
sis of the military medical services was
on preventing ill health. In regard to
health care in the field, the need was to
provide a system that had the resilience
to withstand damage to the health care
infrastructure itself, and this necessar-
ily led to a ’do the greatest good for the
greatest number’ philosophy.
our values now are rooted in excel-
lence in care provided for every casu-
alty. Perhaps with the exception of the
US, no nation can realistically provide
excellence in health care everywhere
in the modern military operational en-
vironment and so greater collaboration
with a small number of allies is neces-
sary, usually within the North Atlantic
Treaty organization (NATo) of which
we and the US are key contributors.
The learning we get from collaborating
with other nations is highly beneficial.
In terms of sharing data, there is al-
ways a tension between protecting in-
formation that might harm one’s own
troops through exposing vulnerabilities,
and the need to share information for
the protection of troops. Achieving data
sharing is difficult due to the under-
standable security concerns, and also
because the effectiveness of preventive
activities (and so the benefit of sharing
information) can be difficult to prove. In
addition to excellent work that is already
undertaken within NATo, a recent initia-
tive that the UK is contributing to is the
Deployment Health Surveillance Capa-
bility in munich. This is a branch of the
NATo military medical Centre of Excel-
lence based in Budapest.
Q. How do you agree on a common
standard to exchange and share
data?
A. It’s a really big job and it isn’t just a
medical issue. The technical issues in-
clude information systems being able to
talk to each other. In terms of hard prog-
ress what we do have is the Defence
Health Surveillance Capability. We are
starting to put the structures in place
to better understand what the health
threats are on the ground and react to
them as they arrive.
Another area we have made some
progress is the NATo trauma registry,
which is compatible with the US Joint
Theatre Trauma registry. There is now
a single repository on the outcome of
various injuries, interventions and a
mechanism for learning how to make
continual improvement. There is a lot
of emphasis on sharing information and
experience, but there is still a way to go
in terms of a comprehensive approach
to this.
Q. sounds like you are doing inter-
esting things with information al-
ready. What is possible down the
road?
A. We have gained a better under-
standing of why we need the informa-
tion and what we are going to use the
information for. We use this information
for the benefit of patients in preventing
ill health, and also to improve the qual-
ity of the care we give. In terms of what
will happen in the future, I think there
will be greater collaboration between
nations. The way we deliver health
Brig. Robin Cordell, as ACO Medical Advisor, led one of three working groups assembled to discuss strategic, operational, and tactical-based information management during the NATO Medical Conference in Istanbul, Turkey April 2010.
10 Leadership | CGI INITIATIVE FOR COLLABORATIVE GOVERNMENT | s p R I N G 2 0 13

care on operations now is very much
on a multinational basis. We need to
not only share information but also im-
prove the interoperability and connec-
tivity between our nations.
Q. You have had significant inter-
national experience, including your
job as the Allied command Opera-
tions Medical Advisor. How do you
approach this type of environment
and what are the challenges in pro-
viding health care in a multinational
environment?
A. The essence of it is to understand
the culture- the national, military and
medical culture. once you start to
understand culture you can start to
engage those who really are the key
influencers – and these may not nec-
essarily be the most senior in rank. Un-
derstanding them is the key to effective
leadership.
People are a product of their upbring-
ing and specific environment. Under-
standing the values people hold helps
to predict how people will react. Even
though medical staff across the world
have a common set of values in terms
of the Hippocratic oath, there are some
differences in how people approach
providing care in the complex environ-
ments in which we operate.
In the case of the UK, our military
medical services are largely embed-
ded in the National Health Service,
where our hospital specialists work
between deployments. our casualties
from Afghanistan and elsewhere return
to the National Health Service, spe-
cifically the Queen Elizabeth University
Hospital in Birmingham.
We have had a few challenges to
introducing some common ways
of working. one example was the
timelines for reaching casualties on
the battlefield. There were two per-
spectives: there was a slightly more
pragmatic approach and a more pre-
scriptive approach. By speaking with
the key stakeholders, we were able to
get a satisfactory agreement and now
have something in place that works re-
ally well.
Language is also important. misun-
derstandings can arise even between
native English speakers from differ-
ent nations. There is unique language
used within the military culture, which
can vary between the individual Armed
Services and between the military and
civilians.
The key lesson is to use all your
senses to ensure that people really
understand you --even if they are na-
tive English speakers--listen carefully
to what they say, observe their reac-
tion and feel the atmospherics. This is
why videoconferencing is useful, but to
be really effective needs to have been
founded on face-to-face meeting be-
forehand.
Q. How much training do you need
to provide those working on the
ground?
A. The key point is not only individual
training, but team training. What has
been highly successful in regard to the
UK-led hospital at Camp Bastion in
Afghanistan is having US doctors and
nurses that form a significant part of
the hospital staff to come to our Army
medical Services Training Center and
work with the people they will work
with in Afghanistan. We look at how
we will manage casualty loads, how
we will treat host nation civilians and
detainees. It also enables people to
understand how they relate to one an-
other and how they work as a team. As
a result of our experience we have rec-
ommended that it makes sense to con-
tinue training with our US colleagues
to prepare for any future missions after
the end of the current operation in Af-
ghanistan.
Q. Are there changes in strategy,
approach or technology that will
make this easier today than it was
five years ago?
A. We will examine how we can best le-
verage emerging technology to inform
the health advice we provide and to
support health care delivery. At pres-
ent our system is based on a server
model, but opportunities presented
by cloud technology could be useful.
Deploying cloud technology would
help us enhance the linkages between
command, aviation, military medical
and civil health care systems within our
own nation, and also between our in-
ternational partners.
We are likely to see collaboration in
the provision of medical support be-
tween nations as the norm for future
operations; transferring information
will be enhanced between medical
Evacuation (mEDEVAC) helicopters
and the receiving hospitals, between
field hospitals within the operational
theater, between the field hospital and
the strategic aeromedical evacuation
assets, and with the receiving home
base hospital.
Better information in regard to each
step in the pathway provides opportu-
nities to improve. We are providing an
excellent standard of health care on
operations. Continued improvement in
information support will allow us pro-
vide better advice we give regarding the
promotion and protection of health, and
excellence in restoring the health of the
sick or injured soldier, sailor, airman and
marine - and others we look after. n
s p R I N G 2 0 13 | COLLABORATIVEGOV.ORG/LEAD | Leadership 11

12 Leadership | CGI INITIATIVE FOR COLLABORATIVE GOVERNMENT | s p R I N G 2 0 13

Dr. Mark Chassay teams data with policy
for Texas health care delivery
Dr. Mark Chassay has always been a planner
with a vision. Soon after finishing medical school,
he applied to become a volunteer physician for
Team USA. Although the wait was more than
five years, he figured by that time he would have
enough experience to land the job.
Carrying the Torch
By John STein Monroe
PhotograPhy by Lance rosenfieLd
s p R I N G 2 0 13 | COLLABORATIVEGOV.ORG/LEAD | Leadership 13

in the end, his persistence paid off, and in 2003, he was accepted into the U.s. olym-pic committee’s volunteer training program in california. he worked as a medical officer at the 2008 summer olympics in beijing and more recently was appointed team Usa’s chief medical officer for the 2012 London Paralympics.
chassay has always enjoyed sports — he played varsity football and baseball in high school — and always wanted to be a doctor, but it wasn’t until he was in medical school that he decided to combine his love of both.
a friend tipped him off to fellowships in sports medicine that he could apply for when he was finished with his residency. “the goal, after my fellowship in california, was to go back to where i grew up in the houston sub-urb of sagemont and treat my friends and my friends’ kids.”
he returned to his roots in texas, where he co-founded a private practice focusing on family and sports medicine. “along the way, i got a job as the head team physician” for intercollegiate athletics at the University of texas at austin.
recently, he decided to take on a new chal-lenge: health care policy. in January 2012, he became the deputy executive commissioner for the office of health Policy and clinical services at the texas health and human ser-vices commission (hhsc).
“i decided this would be a good way to continue doing some policy work and get in-volved in the complexities of health care,” he said. “at the same time, it allows me to get a little out of my comfort zone since i had been doing the same thing for a while.”
Whether in athletics or health care, leaders know that good data is indispensable when it comes to training. “it’s all about being pre-pared,” chassay said, “and in order to be pre-pared, you need data.”
There are a lot of times you are successful, but the winners are always the ones who learn from their mistakes, changing things up just a little bit.
14 Leadership | CGI INITIATIVE FOR COLLABORATIVE GOVERNMENT | s p R I N G 2 0 13

it’s important to constantly review past perfor-mance and assess what works, what doesn’t and what can be done differently the next time around, he said. “in athletics, you make mistakes,” chas-say said. “there are a lot of times you are suc-cessful, but the winners are always the ones who learn from their mistakes, changing things up just a little bit.”
the same holds true in health care, he said. “if we see that things, either through claims or qual-ity, are going a little bit awry or are not up to the standards that we would like, we can make more interventions, whether it’s education or advocacy for certain items.”
health care providers, insurance companies and state agencies collect a vast array of health-related data: on the quality of care, the cost of care and the outcomes. the key is to analyze the information and get it into the right hands, where it can be used to make changes in health care ser-vices, chassay said.
Jump-starting innovationin one of his first tasks, chassay is helping lead an effort to improve the exchange of information in texas between state agencies and between the public and private sectors. the goal is not new, but it was given new impetus after the state leg-islature created the texas institute of health care Quality and efficiency in 2011 to study how to im-prove health care.
chassay envisions creating a life cycle of health data, where data is transformed into information, information into knowledge and knowledge into wisdom. “once we get data to flow, people can get more information to be more knowledgeable about different areas,” he said. “and ultimately, the wisdom is giving managed care organizations information that might help them improve the quality of their care.”
the institute got off to a fast start, by necessity. the legislation that created the institute, senate bill 7, directed it to develop a report by dec. 1,
2012, recommending how data could be more ef-fectively collected and used to improve the quality and efficiency of health services in the state. the institute is run by a board of directors and is sup-ported by chassay and his team.
senate bill 7 was a comprehensive piece of leg-islation aimed at revamping the state’s health care infrastructure, with provisions to expand man-aged care, streamline Medicaid, foster new health care collaboratives, and move Medicaid and the children’s health insurance Program (chiP) to reimbursement models tied to innovation, cost-efficiency and performance.
chassay and his staff needed to coordinate their work with several related committees and numerous hhsc departments. the key to this co-ordination, chassay said, was having a clear guid-ing objective — sharing data — and then breaking that down into manageable pieces. “if you tackle the challenge a little bit at a time, it works out,” he said.
before the first meeting concluded, the board broke into groups to develop action plans around four specific issues: make full use of existing health care data, collect and use a broader range of data, make information on the quality and cost of health services available to consumers, and recognize health facilities for outstanding quality and efficiency.
the institute’s task was feasible because its objectives were clear and compelling, with many parties in both the public and private sectors hav-ing a vested interest in improving health care ser-vices.
being a physician, chassay said, has helped him put some of the things he is trying to do in perspective. “When someone says, ‘We need a provider to do this’, i say, ‘Let’s focus on the most important issues.’ We have to take little steps for people to evolve the position.” Like in sports, it’s going to take a group effort, “teamwork and col-laboration.”
the board ended up making 25 recommenda-
s p R I N G 2 0 13 | COLLABORATIVEGOV.ORG/LEAD | Leadership 15

tions in its report, drawing on the research of the first three groups. the fourth group concluded that the market did not need any more awards or recognition programs. the institute is now waiting on direction from the state legislature.
data sharing and deliveryhhsc, which has an annual budget of $16 bil-lion and 9,300 employees, is the result of a con-solidation of a number of state agencies in 2003. it also administers more than half a dozen pro-grams, such as Medicaid, chiP and the texas Women’s health Program.
although all fall under the purview of hhsc,
chassay acknowledges that each group has been accustomed to owning its own data rather than sharing it. Whatever direction the institute goes, the commission now understands the im-portance of breaking down its own information silos.
“there are a lot of organizations that have come together over time,” he said. “We are try-ing to make sure that we can map out all the in-formation sources and what data we can share with whom.”
figuring out who can share data “is one of our biggest challenges internally and externally,” chassay said. “there are other agencies outside
the board of directors of the institute
of health care Quality and efficiency
provided the texas legislature with 25
recommendations in four categories.
here is a sampling in each.
Improving Public Policy and Decision-making
• Expand public reporting of health out-
comes measures at the facility level,
beginning with a small set of patient
safety indicators.
• Expand data collection in high-priori-
ty areas, such as hospital emergency
department claims.
• Reduce barriers to data sharing
among state agencies and speed
the availability of data in the public
domain.
• Publicly share data on health care
facilities regarding potentially pre-
ventable readmissions and potentially
preventable complications.
• Encourage (but do not mandate)
public/private-sector collabora-
tion to expand information available
on health services utilization and
reimbursement for the commercially
insured population.
• Ensure the protection of any sensi-
tive personal information that might
be included in any future centralized
health care database.
• Identify and eliminate any data collec-
tion requirements that provide little or
no public purpose.
Improving Transparency and Aiding Consumer Purchasing
• Develop and offer a high-deductible
health plan with a health savings
account (i.e., a consumer-directed
health plan) to state employees.
• Provide participants in the state’s Em-
ployees retirement system and the
teacher retirement system of texas
with price and quality transparency
tools.
• Improve access to information
regarding consumers’ out-of-pocket
financial obligations for health care
services.
• Generally promote efforts in the
private sector to increase the public
availability of information on health
care quality, costs to the consumer,
outcomes of care and patient safety.
Improving the Use of Quality-related Data
• Develop a consumer-friendly website
offering health care quality infor-
mation to consumers, including a
dashboard of publicly reported health
outcome measures.
• Conduct a comprehensive study of
consumer behaviors, preferences and
the best ways to maximize consum-
ers’ use of health care information.
Recognizing Exemplary Performance by Health Care Facilities
• The board determined that no new
recognition program was needed.
data-driven health care: options to consider
16 Leadership | CGI INITIATIVE FOR COLLABORATIVE GOVERNMENT | s p R I N G 2 0 13

our hhsc enterprise that we would like to ex-change information with,” chassay said, adding that privacy, security and confidentiality policies must be in place first.
access to more information makes people “more knowledgeable about different areas,” chassay said. but the data is only useful if it is accurate, and data collection, even automated, is not a perfect science. the challenge is for agencies to scrub data as quickly as possible and deliver it to health care providers who need it, chassay said.
“there is so much data coming in and out. the biggest concern for government entities is making sure the data is correct, that it has been scrubbed, that it’s as accurate as possible,” chassay said. “because if people outside gov-
ernment are going to make decisions based on non-scrubbed data, it could lead to incorrect suppositions.”
technology can help, thanks to increasingly sophisticated business intelligence software that can sort through and analyze large amounts of information. in this era of big data, it is possible to create exponentially larger data stores that can be mined for intelligence.
a Local approachone recommendation the institute made in its ini-tial report is to collect, analyze and deliver health care information back to providers in a particular region rather than on a statewide basis. although such an approach involves smaller samples, it also provides a more efficient feedback loop. the
Dr. Chassay served Team USA at the summer Olympics in Bejing
s p R I N G 2 0 13 | COLLABORATIVEGOV.ORG/LEAD | Leadership 17

regional perspective also has the benefit of reflect-ing how care is actually provided. a person under-going treatment for a cardiac condition is likely to visit other health care providers in the same area.
although each regional collaborative will have its own approach for assessing the effectiveness of its services, the groups might also find it useful to share data with one another, “so they get a better idea of how they are performing compared to oth-ers,” chassay said.
one model for such an approach is the dallas-fort Worth hospital council foundation, a non-profit public/private partnership involving more than 80 organizations, including hospitals, clinics, insurance providers and government agencies.
the foundation has created a regional database that can give partner organizations insight into
It’s all about being prepared, and in order to be prepared, you need data.
Dr. Chassay at the baseball College World Series with the University of Texas
18 Leadership | CGI INITIATIVE FOR COLLABORATIVE GOVERNMENT | s p R I N G 2 0 13

their operations. hospitals identify prevention quality indicators for tracking outpatient care, or they can drill into admissions records to help de-cide where to establish new clinics.
for chassay, the collaborative approach helps doctors avoid costly errors. What a medical checklist often reveals, chassay said, is how players are involved in providing care. “the more folks you have involved in checking and double-checking [processes], the more collaborative it is and the safer the environment is going to be,” he said.
already texas is encouraging regional ar-rangements by testing innovative approaches to services that might improve the quality or cost-efficiency of the chiP or Medicaid programs.
“it’s important to know this is very local,” chas-say said. “We want to be able to get the informa-tion out to our regional health care partnerships as quickly as possible, give them some feedback and help them understand their local areas. our goal is to push data down to the local areas so they can make the decisions about what they need the most help with.”
the institute could go in any number of direc-tions with its data-sharing initiatives, depending on what it hears back from the legislature. in the meantime, there are smaller changes it can make to improve health care delivery, such as using readily accessible metrics that suggest new ways to improve the quality or cost-effectiveness of care. Potential fields include diabetes, asthma and medications used to treat psychiatric con-ditions — “things that could affect our patients pretty deeply,” chassay said.
it’s like an athlete preparing for a competition, chassay said. “it’s just being proactive about trying to think about what you do: What are the intended or unintended consequences and how do you measure those?” he said. “you need to balance all the information all the time. you need to look at where you are going.”
the good news is that data sharing will get
easier over time. “Just as in sports,” chassay said, “the more you play and the more you work with the athletes, the more the teamwork [and] the camaraderie develop in order to move that team forward.”
despite his full-time policy job, chassay said he still works as the assistant team physician at the University of texas, filling in where needed, and practices medicine in the community, providing care to children from lower-income families.
chassay would enjoy an opportunity to work at the olympics again. “i feel like this is a good way to volunteer for our country,” he said. “it’s excit-ing. at any point, anything could happen. and what i love is the interaction with the athletes and learning about what it took them to get there.” n
Texas State Capitol in Austin
Dr. Chassay at the baseball College World Series with the University of Texas
s p R I N G 2 0 13 | COLLABORATIVEGOV.ORG/LEAD | Leadership 19

20 Leadership | CGI INITIATIVE FOR COLLABORATIVE GOVERNMENT | s p R I N G 2 0 13

Partnerships and embracing uncertainty
underscore Cigna CEO’s accountable care
approach
By Stephanie Kanowitz
PhotograPhy by gale Zucker
In many ways, David Cordani’s job running
Cigna is a lot like training for his upcoming half
marathon. Both require the ability to exist in a
comfort zone that embraces change — and a
little bit of pain.
Setting the Pace
s p R I N G 2 0 13 | COLLABORATIVEGOV.ORG/LEAD | Leadership 21

cordani, the 46-year-old president and ceo of cigna, said change has always been a key job re-quirement, even before he took the helm at cigna. and it’s the evolution of the business that has kept him in it for 20-plus years. cigna is a global health service approaching $30 billion in annual revenue, reaching 30 countries and serving 75 million cus-tomers.
When it comes to handling the changes occur-ring in the health care industry, it helps that cordani is comfortable with being uncomfortable. Perhaps he owes some of this to his dedication to athletics. he is a longtime runner and an avid biker who has completed numerous bike rides for charity.
although he didn’t start his career in the health care industry, cordani said he initially was attracted to its goal of providing programs “that are trying to help people at a variety of life points.” beyond that, cordani said he wanted “an industry that I thought was going to go through significant change. little did I know what I was asking for.”
Fortunately, leading through change is what cordani does well. he decided in 2008 that cigna would shift its focus from treating ailments at high costs to preventing and managing them through holistic care over time. as a result, he became a leader in promoting and establishing collaborative accountable care partnerships (cacs).
cacs are cigna’s version of accountable care organizations (acos). they are collaborations be-tween cigna and groups of health care profession-als that are accountable for the people they serve. as with acos, cacs aim to improve health care, lower health care costs and increase patient satis-faction. Pay is based on how well providers do in meeting these goals.
cigna set up its first cac in 2008 with Dart-mouth-hitchcock, a physician group that practices in New hampshire. today cigna has more than 50 cac initiatives in 22 states, encompassing more than 510,000 customers. by 2014, cordani aims to have 100 programs reaching 1 million individuals.
“historically, insurance is a way to try to take un-
certainty and project some level of certainty. that’s why we flipped our company around and said, ‘We’re no longer an insurance company. We’re a health service company, dedicated to helping the people we serve improve their health, well-being and sense of security,’” he said.
In some ways, the change was organic. the ma-jority of new programs and services that cigna was developing were less focused on insurance and financing vehicles and more on keeping peo-ple healthy. “of course, there was an insurance feature to it,” he said, “but that became a piece of the puzzle as opposed to the totality of it.”
Success through Partnerships collaboration is so crucial to the vision of global health service that cordani first reached out to form partnerships within the company and with his own employees. after establishing the new mission — the focus on health, well-being and a sense of se-curity for the insured — he gathered about 150 unit executives and presented his case for revamping the company.
“We gave people a choice of whether or not they wanted to pursue that path,” he said. “We started to identify the fact that things were going to change: processes, structures, rewards, mea-surements.” People had to decide whether they were comfortable with making that change or not, he said.
the decision to ask the leaders for their buy-in “turned out to be a pretty powerful process,” cor-
We’re a health service company, dedicated to helping the people we serve improve their health, well-being and sense of security.
22 Leadership | CGI INITIATIVE FOR COLLABORATIVE GOVERNMENT | s p R I N G 2 0 13

dani said. “Individuals first and foremost were in-formed, they were brought into the thinking, they understood why this case for change was being put forward, and very importantly, they understood what was in it for our customers.”
It also challenged the employees to embrace change rather than accept the status quo.
“If you need certainty,” cordani told his employ-ees, “this is not going to be the right place for you. everything around us is going to change — regula-tion, legislation, competitor behaviors, hospital and physician partners, and the needs of customers.”
outside cigna’s walls, cordani reached out to health care providers. again, the partnerships start-ed with a conversation, this time with the leaders of a physician group or hospital system to find out if their goals align with cigna’s.
“If there’s enough shared space, then you move forward. If there’s not enough shared space, there’s going to be way too much friction and you’re never going to move forward,” he said. “that doesn’t
make it right or wrong. It just makes it different and not on target.”
the reach extends beyond u.S. borders, with cordani traveling to england, belgium, turkey, South korea, taiwan and china to broker deals. and it even extends beyond the company itself, with cigna acquiring other firms to bolster its growth. For example, in october 2011, it purchased health-Spring for $3.8 billion to reinforce its Medicare ad-vantage business.
collaborating on Data, Not Just MissionInherent to collaborative care is an astonishing amount of information that needs to be captured, stored and shared. cigna’s approach to managing it is by now familiar: through partnerships.
but collecting data for data’s sake is not the objective, cordani said. “It’s the right information on the right person to a physician at the point of interaction. It’s understanding how physicians
If we’re only fixing people when they’re sick,we’re missing it.
s p R I N G 2 0 13 | COLLABORATIVEGOV.ORG/LEAD | Leadership 23

work, understanding the work protocols and being able to supplement those protocols with the information to help them provide a higher-quality, more predictable outcome for the ben-efit of the customers.”
For example, cigna developed proprietary technology to create a set of workflows and tools so that a clinician could see details on an indi-vidual and understand everything about that per-son — including lab data; biometric indicators; and information on behavioral, lifestyle and family history— and could add information as it came in.
“It’s a very powerful tool because you need to see and understand these people clearly when they’re not in the physician’s office,” he said. “If we’re only fixing people when they’re sick, we’re missing it.”
cigna doesn’t demand that physicians use
If you need certainty, this is not going to be the right place for you. Everything around us is going to change.
24 Leadership | CGI INITIATIVE FOR COLLABORATIVE GOVERNMENT | s p R I N G 2 0 13

specific technologies and methods. to be success-ful, cordani said, health care providers must be comfortable with the information technology they’re using. “then that flywheel starts spinning faster, and you’ll start getting physicians pinpointing the kind of information that would be most helpful to them,” he said.
to become part of cigna’s cacs, doctors’ offices and hospitals must demonstrate either that they have the technology in place needed for the envi-ronment or that they are willing to get it. It is essen-tial that an organization commit to data, electronic medical records and modernization or demonstrate that it is moving in that direction, cordani said. “be-cause what this is all about is evidence-based care, practice pattern variability and providing the best-quality outcomes.”
taking the leadushering in this new era of health care demands strong leadership. that’s where cordani slides com-fortably into place. he tries to apply many of the les-
sons he’s learned through athletic competition to the business challenges he confronts.
“It’s like any other business problem,” cordani said of the triathlons, marathons and long-distance bike rides he’s participated in for more than 20 years. “you have to set a goal, [and] you have to have disci-pline in your execution and training to prepare for it. a race is a test that gives you immediate feedback, and you always have the ability to get better.”
and there are other benefits. “It’s very much a clearing of the mind and a stress reliever,” he added. “a lot of people think that working out is about fit-ness. I think it’s mental fitness first, physical fitness second.”
cordani applied that attitude to earning an un-dergraduate degree from texas a&M in 1988 and an M.b.a. from the university of hartford in 1994 before going to work at coopers and lybrand, an accounting firm where he focused on health care and financial services. cigna, based in bloomfield, conn., was the only company he considered when he was ready for something new.
How Many Are There?
the five-year-old program today has more than 50 cacs in 22 states covering more than
510,000 customers and 14,000 doctors — 6,500 primary care physicians and 7,500 specialists.
the company aims to have 100 initiatives for 1 million customers by the end of 2014.
What Are they?
cacs are cigna’s version of
accountable care organizations.
they are collaborations between
cigna and health care profession-
als who are accountable for the
people they serve in a given lo-
cale. cacs have a three-pronged
approach: improve the quality
of health care, make it more af-
fordable and increase patient
satisfaction. the medical group
is rewarded through a pay-for-
performance structure if it meets
certain improvement thresholds.
cigna’s collaborative accountable care Partnerships
Source: Cigna
s p R I N G 2 0 13 | COLLABORATIVEGOV.ORG/LEAD | Leadership 25

“ultimately, what I wanted to do is be in a position where I could have an impact, and that gave way to a whole variety of different opportunities here over al-most 21 years now, whether it was classic financial roles, operational roles within our investment opera-tion or field operations,” cordani said.
cordani credits his professional success to fear.“boredom scares me,” he said. “the recipe that
seems to work for me is challenge, impact and fun. you need to be challenged, and change consists of that.”
before he was named president and ceo in Decem-ber 2009, cordani was president and chief operating officer at cigna, and president of cigna healthcare.
I view that my job is to enable the team to be successful, not vice versa.
26 Leadership | CGI INITIATIVE FOR COLLABORATIVE GOVERNMENT | s p R I N G 2 0 13

he joined the cigna board of Directors in october 2009 and also serves on the boards of the National association of Manufacturers and the cigna Foun-dation.
cordani draws on his penchant for racing in his leadership style, too, recognizing that although he’s out in front, many people are working hard to win.
“I view that my job is to enable the team to be suc-cessful, not vice versa,” he said. that begins with “making sure we have a shared agreement on what we’re trying to accomplish and a way in which to measure that as a team. “
cordani also spends a lot of time in the field, talk-ing with cigna’s physician partners, its customers
and health care regulators. by getting out of the home office, “you have the ability to firsthand listen and understand and then demonstrate to your team that you’re there to help to move things along,” he said.
“It’s an attitude of enablement,” he added. “you get the right person in place, and my job is to take barriers out of the way and give them the resources to be successful, and sometimes in part doing it with them in the field and having the shared experience.”
changing Mind-setbut cordani’s interest in change is more than just a matter of personal style. as he sees it, the ameri-can health care system’s overhaul depends on changing our mind-set. reframing the approach to health care means reframing the way people feel about insuring it, providing it and receiving it.
“how do you engage individuals throughout the course of their life in a way that they want to be engaged and help them?” he said, adding that waiting until illness or injury strikes is a poor option. “that’s really the attitudinal shift from sick care to health care.”
and although technology and information flows play major roles in this transformation, they’re not the heart of it, cordani insisted. too often, people go in search of a “technology silver bullet” rather than realizing that health care, ultimately, is local. “It’s one person at a time, one interaction at a time,” he said.
that possibility of change is what keeps cordani going, whether it’s pounding the pavement dur-ing early morning runs or leading his organization along the rough road that is the health care indus-try today.
“I get up every day saying, ‘Wow.’ you look at the size of that opportunity and the impact it has on people’s lives and the impact it could have on the viability and the vibrancy of the country,” he said. “that’s what gets our team up every day.” n
s p R I N G 2 0 13 | COLLABORATIVEGOV.ORG/LEAD | Leadership 27

By Colleen o’Hara
PhotograPhy by DaVID WEIgoLD
Dr. Robert Jesse, principal deputy
undersecretary for health in the Veterans
Affairs (VA) Department, is someone who
likes to fix things, whether it’s a broken car
or a health problem that can have life or
death consequences.
Toolsof theTrade
Dr. Robert Jesse focuses VHA health
care fixes on patient needsPhotograPhy by DaVID WEIgoLD
28 Leadership | CGI INITIATIVE FOR COLLABORATIVE GOVERNMENT |

Toolsof theTrade
s p R I N G 2 0 13 | COLLABORATIVEGOV.ORG/LEAD | Leadership 29

“I don’t like things that don’t work well,” Jesse said. “I always encourage people to figure out the real problem and solve that. It takes longer, but it delivers a better result in the end. this is what we do in health care. We’re trained to find a cure, not just to treat the symptoms.”
It’s this approach that has gotten Jesse to where he is today: helping manage the nation’s largest in-tegrated health care system. the Veterans health administration (Vha) cares for more than 8.3 mil-lion veterans and their family members each year at more than 1,400 sites, including hospitals, clinics and nursing homes.
as a practicing cardiologist who sees patients in his clinic on Friday afternoons, Jesse is an ideal judge of what works in health care and what doesn’t. his clinic is in his hometown of richmond, Va., but many of his patients know he works for Va in Washington, D.C.
“a lot of conversation goes on that brings a dif-ferent perspective to things,” he said. “We talk a lot about patients under care, but it’s a different issue when you’re doing it.” and he is applying this first-
I always encourage people to figure out the real problem and solve that. It takes longer, but it delivers a better result in the end. This is what we do in health care. We’re trained to find a cure, not just to treat the symptoms.
30 Leadership | CGI INITIATIVE FOR COLLABORATIVE GOVERNMENT |

hand perspective of patients and doctors, and the systems that support them, in leading Va’s push to create a new health management platform.
the goal, he said, is to share information across the full care cycle of a patient, empower patients with their own health information in a context they can understand and act on, deliver the data to care-givers so they can make the best possible decisions as part of their natural workflow, and ultimately achieve what Jesse called “connected health.”
The Jesse Manifestothere are three faces to this health It effort — the provider, patient and system — that must work to-gether to enable Va to look across patient data, identify trends and improve approaches to care, Jesse said.
Several management principles — dubbed the “Jesse Manifesto” by Dr. Madhulika agarwal, depu-ty undersecretary for health for policy and services at Va — guide the effort: health data must be ac-quired as part of the workflow process; technology must support workflow, not encumber it; users must have real-time access and visibility into the system; delivery of effective health care must have sound business practices and principles of systems engi-neering; new capabilities must be easy to use; and complexity must be managed.
Jesse is up for the challenge, he said. “the reason I am in the position I am in is because I have always taken the approach of understanding and fixing the root source of the problem.”
Whatever changes are made, though, they must deliver better patient care, Jesse said. “I operate under the premise that you can’t have healthy pa-tients without a healthy health care system,” he said. “So it’s our job to make sure that the system is as healthy as possible.”
already, Vha has begun reorganizing its health care teams, technology and knowledge around pa-tient needs to achieve the goal of accountable care.
Under its patient aligned care team (PaCt) pro-gram, a team of people, led by a primary care phy-
sician, with the involvement of other staff such as nurses and mental health providers, supports a patient. the goal is to make it easier for patients to make appointments, receive care, get lab or test results, communicate with their doctors, and be more involved in their health care. It also lets providers share data on their patients and integrate various levels of specialty care back into the pri-mary care environment.
In addition to involving technology, such as elec-tronic medical records (EMrs) and secure messag-ing, the PaCt approach is also a philosophy. “there are multiple ways to engage a patient,” Jesse said. “Fundamentally, we are trying to change the health care dynamic. If we can change it from being about an encounter to being more about a sustained rela-tionship, you change the whole meaning of access.”
Under PaCt everybody brings certain skills to the table to deliver a much more holistic, personalized approach. Nearly one-third of Vha employees have gone through formal PaCt training so far. “We are trying to move to a more personalized, preventative and patient-driven model of care,” Jesse said. “that means you ask different questions and communi-cate with patients in very different ways.”
technology must support this team-based ap-proach, he added. he is a regular user of the Vet-erans health Information Systems and technology architecture (Vista), which allows health care provid-ers to review and update a patient’s EMr, order pro-cedures and medicine, and track treatment.
as good as Vista is, Jesse said, it does not sup-port the ultimate goal of team-based care, which re-
I operate under the premise that you can’t have healthy patients without a healthy health care system.
s p R I N G 2 0 13 | COLLABORATIVEGOV.ORG/LEAD | Leadership 31

quires information sharing, coordination and patient involvement in health care decisions. “We don’t need another electronic medical record. We have a great one,” Jesse said. “but that construct is not sufficient to manage the health care system we are striving to be. We are moving toward what we call the health Management Platform.”
Va recently announced plans to turn to the pri-vate sector and open-source software to improve Vista, including making it more configurable based on who is using it and where, and making data more accessible and a shared resource depart-mentwide.
there is also continuing progress on the Virtual
Lifetime Electronic record (VLEr) which allows health information on members of the military to flow among Va, the Defense Department and pri-vate providers. VLEr creates a seamless way for service members and veterans to access and manage benefits and care from the day they enter military service and throughout their lives.
VLEr is a business and technical redesign initiative that doesn’t create a new patient record, but makes it possible for DoD, Va and other public and private partners to securely exchange that information.
So far, VLEr supports the exchange of health care information among DoD, Va and private health care providers in 12 sites around the coun-
the Veterans affairs
Department is using several
new tools, and developing
others, to make collecting
and sharing patient data
easier, and to deliver
information to providers.
the Surgery Quality
Workflow Manager (SQWM)
creates an end-to-end shared
workflow system that collects
patient data starting when
the patient is first referred for
surgery through long-term
follow-up appointments.
It automates many related
tasks along the way such as
scheduling, accessing patient
information and ordering
tests.
Similarly, the Emergency
Department Informatics
System (EDIS) is a workflow
system for emergency
departments that tracks
patients and automates
order entry, charting and
other procedures. the bed
Management System (bMS),
which manages inpatient
beds, is also being deployed
across Va. and work is under
way on Consolidated Flow
Management (CFM), which
will link SQWM, EDIS and
bMS in a way that allows for
operational insight to optimize
inpatient resources.
the Cardiovascular,
assessment, reporting
and tracking System for
Cath Labs (Cart-CL)
system creates a nationwide
repository for catheterization
lab data, including software
for data entry and report
generation. In the cath labs,
for instance, at the end of
every day, Va knows how
many catheterizations were
done across the entire
enterprise, how many
patients had complications
— including major ones
— and the success of the
procedures. and, because
this occurs in real-time, it
allows for very precise quality
management.
Va is developing new
Cart modules and
analytics for peripheral
cardiovascular interventions,
electrophysiology and in-
hospital cardiac arrest.
Tool Time
32 Leadership | CGI INITIATIVE FOR COLLABORATIVE GOVERNMENT |

try with plans to expand the capability to addi-tional regions by the end of 2013.
VLEr and the expansion of the ebenefits portal will give veterans and service members access to health care records, benefit applications, ben-efits information and other personal information through a web portal.
‘No Pain For the Gain’ another critical step toward accountable care, Jesse noted, is for providers to collect and use data as part of their daily routines and workflow.
“one of my principles is if data is important enough that you need to manage the patient or the system, then it needs to be acquired through the workflow process, not as a secondary opera-tion,” Jesse said. “Principle No. 2 is no pain for the gain. People won’t adopt things that create more work for them.”
Primary care providers generally have about 1,200 patients, Jesse said. “they ought to be able to sit down every Friday afternoon and see how their diabetics are doing, how their patients with heart failure are doing, how patients with spe-cific knee or hip implants are doing. and looking all across those records is essential because it’s often the variance that highlights where the prob-lems really are.”
the analytics group, which is part of Vha, is al-ready moving in this direction. It has developed a risk model that flags the highest-risk patients. the model predicts for doctors the probability of these higher-risk patients being hospitalized within 30 or 60 days. the ability to do this allows the provid-ers to focus on those patients who will benefit the most from the right interventions, Jesse said. Vha plans to launch a pilot program that will use this capability to monitor a group of high-risk outpa-tients along the lines of an “ambulatory ICU” to improve outcomes.
there are several new tools – and some in de-velopment – that Va is using to make collecting and sharing patient data easier and to deliver in-
“One of my principles is if data is important enough that you need to manage the patient or the system, then it needs to be acquired through the workflow process, not as a secondary operation.”
s p R I N G 2 0 13 | COLLABORATIVEGOV.ORG/LEAD | Leadership 33

formation to providers as part of daily workflow, which ultimately leads to better decision-making. (See sidebar).
the technology and tools allow doctors to build a better relationship with their patients. “the real key is to get the data back to people,” Jesse said. “true quality improvement gets done in rapid cycle models at the workflow level. If you’re only reporting data at a macro level, that gets re-freshed every month. It doesn’t help people doing that work. So they are spending all their time col-lecting data and not improving on it.”
The Big Data WaveVa is also working on mining that data for valuable information that will improve the health care it pro-vides to patients.
Jesse noted that being able to share data, look across patient records, glean information on trends, identify areas of care and prevention with potential high impact on quality, and apply that insight to im-prove care is essential.
“our term is ‘population health,’” he said. “by looking at what works across an organization allows you to then go and substantiate the things that are successful.”
Jesse also noted that Va is actively pursuing use of the vast new types of data emerging in the health field to help achieve connected health.
the Va Informatics and Computing Infrastructure (VINCI) is expanding the knowledge base of medical records, Jesse said, by creating a data warehouse that lets researchers look across and analyze Va data. It encourages collaborative research and pro-vides cognitive support to physicians and a deeper and richer capability to understanding the impact of a specific action on a specific patient, he said.
For instance, VINCI would allow a researcher to enter data terms associated with prostate biopsies in natural language and then, using a recognition engine, would establish relationships among data related to that topic. It’s possible to use VINCI to create sce-narios that would show, for example, that eight out of
10 doctors took a specific action related to prostate biopsies. “When you have the ability to access mil-lions of medical records, you can start to change the dynamics of clinical research,” Jesse said.
other programs, such as Va’s Million Veteran Pro-gram, which will collect health data to study genes’ role in health, and the genomic Information System for Integrated Science, which will create a reposito-ry of genomic information, represent ways to apply new types of data to improve health.
Patient-centric Viewhealth care transformation at Va couldn’t happen without technology. however, technology is just a means to an end. as Jesse reminds us, it’s always about the patient.
“When we talk about patient-centered care, it’s not about plants in lobbies and artwork. It’s about getting patients to be able to articulate what’s really important to them,” he said. “When you take care of people for 20 years, that clearly changes across those periods of time, but if you don’t have the con-versations, then you don’t know; you’re just treating the disease.”
Jesse said he is happiest when he can learn new things and make a difference. he has won awards for his work in cardiac care and for teaching, but the achievement he is most proud of is seeing systems that work flawlessly. “When the systems work well, the art of medicine can flourish and the precious time we spend with patients becomes most valu-able,” he said.
Jesse said he has taken the approach “that I work for the people below me because it is my job to make them successful. and I am accountable to the people above me. and if you can build in the organi-zation a sense of empowerment and determination, then that’s how things are successful. they aren’t successful because I said they have to happen.”
People should feel empowered to make deci-sions. If they don’t, the decisions get “escalated up” and are made by executives who have “little insight into operational nuances,” he added.
34 Leadership | CGI INITIATIVE FOR COLLABORATIVE GOVERNMENT |

a leader’s job is to provide intent and direction, Jesse said. “operational success is predicated on having talented people who are trained to follow up on a vision. you can put all the performance mea-sures out there, but the best judge of success is if decisions are being made at the appropriate level.”
Measuring and establishing performance mea-sures can help improve health care delivery, but they have their limitations. “really what we want is to drive a system on value,” he said.
Jesse says he will continue working toward what he calls “true health care reform,” which will come when patients own their health. “they must own their medical record and control access to it,” he said. “Medical systems of the future will allow that to happen, but we have to be operating on that premise.” n
When the systems work well, the art of medicine can flour ish and the precious time we spend with patients becomes most valuable.
Department of Veterans Affairs at a Glance
Number of VA Facilities VA Benefits and Health Care Utilization
VA Community-Based Outpatient Clinics
VA Vocational Rehabilitation Trainees
Veterans Receiving VA Pension
VA Education Beneficiaries
Active VA Home Loan Participants
Veterans Receiving VA Disability
Compensation
Life Insurance Policies Supervised and
Administered by VA
Total Enrollees in VA Health Care System817 8.57*
7.02
3.53
1.73
0.95
0.31
0.06
300
152
131
56
VA Vet Centers
VA Hospitals
VA National Cemeteries
VA Benefits Administration
Regional Offices
Numbers in Millions
Source: Department of Veterans Affairs, Office of the Actuary, Veteran Population Projection Model (VetPop) 2011; Veterans Benefits Administration; Veterans Health Administration, Office of the Assistant Deputy Under Secretary for Health for Policy and Planning.
s p R I N G 2 0 13 | COLLABORATIVEGOV.ORG/LEAD | Leadership 35

On a Mission
Tony Trenkle advances health reform
through technology modernization
Throughout his career in public service, Tony
Trenkle has never shied away from high-profile
technology projects, whether the assignment
was to establish electronic commerce programs
or design online services for his fellow citizens.
Trenkle’s current position at the Department of
Health and Human Services’ Centers for Medi-
care and Medicaid Services (CMS) underscores
his penchant for programs that affect and im-
prove government services, in this case the U.S.
health care system.
By Colleen o’Hara
PHoTograPHy by DaVID WEIgoLD
PHoTograPHy by DaVID WEIgoLD
36 Leadership | CGI INITIATIVE FOR COLLABORATIVE GOVERNMENT | s p R I N G 2 0 13

s p R I N G 2 0 13 | COLLABORATIVEGOV.ORG/LEAD | Leadership 37

Trenkle, who is the chief information officer and director of the office of Information Services (oIS) at CMS, said he enjoys jobs that allow him to use the agency mission to help improve how govern-ment works. “I’ve liked working at agencies with big levers that can be used to create real change,” he said.
His first job in government was as an intern at NaSa working on telecommunications programs. although he was there after the apollo program had successfully landed a man on the moon, the excitement of the endeavor still resonated with him.
It was that strong sense of mission that motivat-ed Trenkle to spend most of his career in govern-ment. “What has always brought me to work in the public sector is the idea that I can make a differ-ence,” he said. “My career wasn’t a defined path as much as it was trying to get things done and lead in various ways.”
Trenkle has worked on many major federal infor-mation technology initiatives during his career, but
there has been one constant, he said: “I have al-ways spent my time at the intersection of technol-ogy and business.”
That’s true of his job at CMS, where Trenkle has worked for seven years, the past two in his current position. He oversees a $1 billion annual IT budget and directs a national operational infrastructure that supports CMS claims processing and other business services.
CMS is one of the largest purchasers of health care in the world, running Medicare, Medicaid and the Children’s Health Insurance Program.
Health care reform has been an impetus for CMS to make changes to its IT infrastructure and im-prove how it processes rapidly increasing amounts of data. Trenkle has helped lay the foundation for the agency to “take advantage of all these trends and have them work for us and not get over-whelmed by them.”
This requires not only new technology, but also a new way of thinking. Traditionally, CMS’ IT infra-structure has been decentralized and funded on
Stages of Shared Services
FY 2012Foundation work FY 2013
Supporting major programs
FY 2014Showing real ROI for programs
Source: Centers for Medicare and Medicaid Services
38 Leadership | CGI INITIATIVE FOR COLLABORATIVE GOVERNMENT | s p R I N G 2 0 13

a mostly programmatic basis, Trenkle said, but in a time of tight budgets, that wasn’t a practical approach.
Under the umbrella of health reform, CMS “is bringing together different funding sources and business requirements to produce shared ser-vices,” Trenkle said. “Even with the funding that we get, there is no way we could support building all these program-specific IT processes.”
There are four enterprise shared services that Trenkle has chosen to launch first: enterprise identity management, an enterprise portal, master data management and a business rules engine. His three-year plan, which began last year, set his shared-services strategy in motion. “This year we are beginning to implement it in terms of real ap-plications,” he said. by fiscal 2014, Trenkle said, CMS will start to consolidate systems, and shared services will begin to show some real results.
None of this could happen without establish-ing a security strategy, Trenkle said, noting that people can connect to systems anytime from
anywhere. “as you move to more sharing of data to produce better health care coordination and reduce costs, the old security and privacy re-quirements need to be reviewed,” he said.
A Doubling of Big Data Measuring the success of health reform focuses on data, Trenkle said, and CMS will be inundat-ed with new types of information as that reform gains momentum. “For health reform to succeed, we need good data to make better decisions — whether you are changing how you make pay-ments, measure quality or improve health care coordination.”
Currently, CMS stores and maintains about half a terabyte of data each month. That is expected to double by 2015, with Medicare claims data growing to 700 terabytes from 370 terabytes, and Medicaid data growing to 100 terabytes from 30 terabytes.
The growth is attributed to more beneficiaries enrolling in the Medicare and Medicaid programs,
What has always brought me to work in the public sector is the idea that I can make a difference. My career wasn’t a defined path as much as it was trying to get things done and lead in various ways.
s p R I N G 2 0 13 | COLLABORATIVEGOV.ORG/LEAD | Leadership 39

states creating insurance exchanges, and provid-ers moving away from a traditional fee-for-service pay model to one based on performance, quality and shared savings. The nature of the facts and figures will change, too, as CMS collects more unstructured data that will require more analytics.
Data analytics puts power in end users’ hands, Trenkle said. “Someone with an mobile device can access this information to make quick decisions.”
This means CMS must adjust how it receives and analyzes the information it collects, so that changes to health care policy will happen faster.
“It’s dependent on having a data infrastructure that can support that,” Trenkle said. The afford-able Care act “gave us some strong business imperatives that have forced us to step back and think about how we are doing data management here at the agency.”
one vision is to create an enterprise data ware-house. Trenkle said this would allow CMS to com-bine new information, such as quality and clinical data with traditional claims, beneficiary and pro-
vider records. CMS is an information clearing house, he said, that can support external re-searchers doing sophisticated analytics.
Last year, CMS partnered with oak ridge Na-tional Laboratory to test better methods of data management. The lab, which works with the Defense Department and the National Weather Service on big data issues, introduced CMS to Hadoop open-source software. That “caused us to think about how we can look at data manage-ment differently,” Trenkle said.
Data center consolidation is another effort under way at CMS. Under a multibillion-dollar virtual data center procurement awarded last year, the agency will consolidate a number of its dozens of data centers to eliminate redundant spending and solutions and make the most of shared resources.
Collaboration Lessons LearnedThroughout his career Trenkle has played a cen-tral role in developing IT standards for govern-ment, which underscored for him the importance
• More than 98 million beneficiaries (not counting additional potential 30+ million Americans that will be added through health care reform).
• CMS expends approximately 1 trillion dollars annually on Medicare, Medicaid, and CHIP programs.
• More than 900 million Medicare fee-for-service claims.
• More than 1.6 billion claims for Medicaid beneficiaries.
• More than 111 million home health assessment records.
• More than 13 million nursing home assessment records.
CMS Operations
Source: Centers for Medicare and Medicaid Services
40 Leadership | CGI INITIATIVE FOR COLLABORATIVE GOVERNMENT | s p R I N G 2 0 13

of collaborating with others. “all that experience has helped me understand both sides of the equation,” he said. “Standards are a compromise. They are a way of bringing different industry needs together to form something we can all utilize.”
before becoming CIo, Trenkle headed CMS’ of-fice of E-Health Standards and Services (oESS), where he coordinated policy and standards re-lated to “meaningful use” under the Medicare and Medicaid Electronic Health records (EHr) Incentives Programs. Meaningful use establishes certain thresholds for EHr programs that, if met, result in financial incentives to providers.
“I heard from the health plans, from the provider community and other parts of industry,” Trenkle said. “Now being on the user side with oIS, I can better understand where those groups were com-ing from. at the same time, from my oESS experi-ence I also know how policies developed and how we work with the standards organization in imple-menting the EHr incentive program.”
Standards are crucial to making various elec-tronic processes work, Trenkle said, including insurance exchanges and Health Insurance Porta-bility and accountability act standards for claims data and information. “If you don’t have good standards in place or implementation guides that help you, then you create more problems on both ends,” he said. “I think they are the glue that holds a lot of the work we do together.”
Compromise is important in other areas besides standards, Trenkle said. “In the IT area, we are a service provider, but we are also a partner with the business side, industry and others. We have to support them, but it is a partnership with re-sponsibilities on both sides.”
Trenkle has spent much of his career building relationships between business and government. He worked for eight years in the private sector after leaving his internship at NaSa. as a result, he is familiar with IT mandates that the business side must adhere to and some of the frustrations IT workers have with missing or undeveloped
“We are a service provider, but we are also a partner with the business side, industry and others. We have to sup-port them, but it is a partnership with responsibilities on both sides.
s p R I N G 2 0 13 | COLLABORATIVEGOV.ORG/LEAD | Leadership 41

business requirements, he said.Keys to health reform include payment reform
and health care coordination, which require working with other organizations, Trenkle said. The rise of multi-payer databases, data analyt-ics tools, new sources of personal data and the collection of more clinical data emphasize the need for cooperation and agreement on stan-dards.
“We have to look at standards from a larger perspective, thinking about how you can do business with each other,” he said.
Several techniques work well when it comes to collaboration, Trenkle said. “None of us have perfect knowledge. Even as we get more information, we get less knowledge,” he said. “So you have to be willing to listen and to meet the other person where they are. but you also have to educate them on your point of view and why you are proposing a certain way of doing business.”
building strong relationships within the ven-
dor and government communities is important to making progress, Trenkle said. “The key is to keep a sense of perspective, calm and humor,” he said. “over time, you find people who want to have a collaborative relationship. So even if you are not on the same side of the fence on every issue, you can at least work toward a common goal.” but in the end, “sometimes you have to take a stand and be willing to support a position that they might not agree with.”
Trenkle thinks strategically when it comes to making changes in government IT. His work has helped develop groundbreaking programs, in-cluding e-commerce programs at the general Services administration and online services at the Social Security administration.
“I’ve enjoyed being part of some major changes in how government conducts business over the past couple decades,” he said. “In the early 1990s we looked at how we could use technology to im-prove services to the public. Here we are a couple decades later still fighting the good fight.”
The Centers for Medicare and
Medicaid Services is instituting
an enterprise shared-services
approach that will deliver
scalable, reusable technical
solutions that serve multiple
business processes. The agency
will start with four areas:
• Enterpriseidentity
management. This will give
individuals a single identity for
engaging in business with CMS
that meets federal security
requirements. This program
can support health insurance
exchanges and will reduce CMS’
access management costs.
• Enterpriseportal.Thiswill
provide a single face to providers,
beneficiaries and organizations
to receive CMS information,
products and services, and
will provide integrated access
to multiple CMS websites and
portals.
• Masterdatamanagement.
This will create a suite of data
records and services that allows
CMS to link and synchronize
beneficiary, provider and
organization data with multiple
disparate sources. It will also
make provider and beneficiary
profiles available through a
trusted data service.
• Businessrulesengine.This
software tool will execute one
or more business rules within
CMS’ information technology
application code and will manage
enterprise rules and define the
relationship among different rules.
Shared Approach
42 Leadership | CGI INITIATIVE FOR COLLABORATIVE GOVERNMENT | s p R I N G 2 0 13

Trenkle understands that progress and change aren’t easy, but leading by example and taking a measured approach are important — whether it’s in IT or life. In his office, he displays a famous quote from gandhi: “We must become the change we want to see.”
Even before he joined NaSa, Trenkle said, he saw how the government “could create change for this country, whether it was the space program, civil rights or providing opportunities for people.” That idea was reinforced by a college professor
who suggested a career in government because it presented the opportunity to do great things.
Trenkle clearly remembers the excitement of his NaSa internship and meeting people who helped put a man on the moon. It’s the same excitement he feels about being at CMS, which is at the cen-ter of change in U.S. health care.
“I’ve worked at different places with different missions,” he said.” but they all make you want to come into work and do what you can to make the world a better place.” n
Sometimes you have to take a stand and be willing to support a position that they might not agree with.
s p R I N G 2 0 13 | COLLABORATIVEGOV.ORG/LEAD | Leadership 43

44 Leadership | CGI INITIATIVE FOR COLLABORATIVE GOVERNMENT | s p R I N G 2 0 13

Dr. Michael Wagner helps Tufts Medical Center
deliver on health care promises
By Colleen o’Hara
PhotograPhy by Matt tEUtEN
Dr. Michael Wagner was director of the internal
medicine residency program at St. Mary’s Hospi-
tal and a member of the Department of Medicine
faculty at the University of Rochester’s School of
Medicine years ago when he thought it would be
interesting to pursue an MBA at the same time.
Making theGrade
s p R I N G 2 0 13 | COLLABORATIVEGOV.ORG/LEAD | Leadership 45

While trudging to class one wintry evening, Wagner realized he could direct his career development more effectively if he chan-neled his time and energy into projects at the hospital rather than pursue another de-gree. “I said to myself, ‘What are the issues confronting a hospital and how can I help an organization work on those issues?’”
the 53-year-old has always been a prob-lem-solver, analytically oriented and com-fortable sifting through a large amount of data and correlating that with clinical infor-mation. “Early on I got that piece, and that was valuable to the organization,” Wagner said. “So as we looked at managed care data and clinical practices of primary care physicians, I could understand how the two were related to each other.”
a facilitator and clarifier who makes things
We develop practices in the community in order to bring high-level specialty care in collaboration with our referring physicians but not in competition with them.
tufts Medical Center in boston
46 Leadership | CGI INITIATIVE FOR COLLABORATIVE GOVERNMENT | s p R I N G 2 0 13

happen, Wagner believes that “people come to the table sincerely, to do the right thing. My goal is to listen carefully, to understand where they are coming from, how they look at the world, and use that in a way that is a win-win for both par-ties.”
his skills have proved valuable, particularly at the 550-member, boston-based tufts Medical Center Physicians organization, where he held various positions before becoming president and chief executive in September 2012. tufts Medi-cal Center, which counts Paul revere and Sam-uel adams among its founders, is a nonprofit academic medical center home to two boston teaching hospitals, one serving adults, the other children. It is also the principal teaching hospital for tufts University School of Medicine.
Step by step, Wagner has helped pursue a sustainable health care model that is working for tufts Medical Center — one that is based on operating an efficient organization that depends on strong relationships with the community and a network of partners to provide the health care people need.
Staying Nimble tufts Medical Center is relatively small com-pared with its competitors in boston — with 260 to 330 beds occupied on any given day — but it is as big as it wants to be, Wagner said. “We are happy with that bed size because we think in the future world of health care delivery, it will be ef-ficient, relatively smaller tertiary medical centers that have a high degree of expertise in specific areas that can deliver ... value to the community.”
Despite demonstrating quality and efficiency that match or exceed its larger competitors, tufts Medical Center’s reimbursements have histori-cally been less, “so we have to have a very cost-competitive structure,” Wagner said. but so far, the results have been positive. the center’s cost data, reviewed by the University health System Consortium, is consistently in the top 10 range
nationwide, he said. “that means we have fig-ured out how to efficiently take care of patients. at the same time, our quality scores are as good as or better than many of our local competitors. We think that structure is very important going into the future of health care delivery.”
another important piece of tufts Medical Cen-ter’s philosophy is the relationships it establish-es with its employees, other physicians and the community it serves. Wagner understands first-hand the power of those connections.
he started his career at tufts Medical Center as a general internist, a position he held from 1990 to 1992. he returned to the hospital in 1999 as chief of general medicine and held that role until 2003. he left for five years and returned as chief of internal medicine and adult primary care in 2008.
he credits familiarity for his returns. Like the “title song from the boston-based television show ‘Cheers,’ everybody knows your name,” he said. “that’s how many of us feel about tufts Medical Center — we know our patients, and they know us.”
that friendly environment extends beyond tufts Medical Center. “our physicians understand that in order for us to be successful we have to extend that friendliness to our referring network,” Wag-ner said. that involves calling people and treat-ing them with respect. It also involves a strategy called Distributed academic Medical Center, “where we develop practices in the community in order to bring high-level specialty care in col-laboration with our referring physicians but not in competition with them,” he said. “this is some-thing that tufts Medical Center Physicians or-ganization has done for decades to build strong and respectful physician relationships.”
“We know that providers in the community have choices,” he added. “For them to stay with us means we must constantly keep an eye on value. I think a lot of primary care doctors and specialty physicians in the community ultimately
s p R I N G 2 0 13 | COLLABORATIVEGOV.ORG/LEAD | Leadership 47

want respect. they want to be part of a network that is highly effec-tive.”
the efforts have resulted in good relationships with physicians in the community and a good rela-tionship with tufts Medical Cen-ter’s own physicians network, the New England Quality Care alliance (NEQCa). Last September, tufts Medical Center, NEQCa and Van-guard health Systems announced they were forming a joint venture to improve patient health care de-livery.
over the years, the NEQCa re-lationship has gone beyond con-tracting with insurers to include care management, patient tech-nology implementation, health registries “and a whole culture of physicians working together under a single banner to provide commu-nity-based care, population-based care and also integration with aca-demic and tertiary care,” Wagner said.
Strategically, Wagner said, the combination of tufts Medical Cen-ter, the Physicians organization and NEQCa provides the ability to execute the “triple aim” of account-able care: improving population care, improving health outcomes for individuals and doing both cost effectively.
When it comes to partnering, it isn’t a one-size-fits-all approach, Wagner said, and the organization is always exploring new approach-es. tufts Medical Center negotiat-ed an alternative Quality Contract with blue Cross blue Shield of
If we remain a traditional medical center where all we care about is the admission, we won’t survive.
48 Leadership | CGI INITIATIVE FOR COLLABORATIVE GOVERNMENT | s p R I N G 2 0 13

Massachusetts, which is part of the NEQCa net-work. the contract focuses on quality and use management to help keep health care spending in check.
“I think this is a fundamental piece,” Wagner said. “We all know that we are going through a transition in health care delivery. the problem is if we do not effectively manage the transition from fee-for-service to payment based on value, we could financially harm the organization. by performing well on risk-based contracts while in this transition phase, we can make the appropri-ate investments.”
readmissions are one example. by reducing readmissions and meeting other significant qual-ity goals, tufts Medical Center has been able to gain some additional reimbursement that it is investing in health information technology in-frastructure to help achieve the “triple aim” goal, Wagner said.
tufts Medical Center’s agreements with other insurance providers have followed a more tradi-tional path, Wagner said, since not everyone is able to enter into a risk-based contract. “We are interested in moving ahead with a contract struc-ture that allows us to take measured risk, focus on quality and be able to manage utilization in a reasonable way,” he said.
tufts Medical Center’s approach is due part-ly to its small size and its reliance on referrals from outside its community, Wagner said. “the number of patients we have that would be able to be in a shared savings program is just over the threshold. So we haven’t seen a shared savings program opportunity for tufts Medical Center.”
a shared savings contract is one type of risk-based contract that gives a physician practice a percentage of savings if the cost of the care it provides is less than what it budgeted. risk-based contracts make sense with large pools of beneficiaries.
Wagner said tufts Medical Center officials are evaluating whether the concept of a bundled
payment option proposed by the Center for Medicare and Medicaid Innovation would work for them. the concept would allow the center to suggest a single price for managing care starting when the patient enters the hospital through 90 days after the patient has been discharged.
then, assuming there are savings, tufts Medi-
Partnerships play a central role in how
tufts Medical Center delivers health care
to patients in an increasingly changing
health care industry. In one such deal,
the hospital and its physicians network
teamed with Vanguard health Systems
to sponsor a new health plan. In august
2012, the Centers for Medicare and Med-
icaid Services approved tufts Medical
Center’s application for an $88.5 million
loan to launch what the center calls a
consumer-governed health plan.
the goal for this new type of health
plan is to give doctors easier access to
patient data, make real-time health care
decisions, establish a nimbler adminis-
trative and information systems structure,
provide streamlined provider payment
rules and processes, and allow physi-
cians to help design workforce wellness
plans.
The Road to Accountable Care
s p R I N G 2 0 13 | COLLABORATIVEGOV.ORG/LEAD | Leadership 49

-cal Center would have additional revenue to in-vest in other areas. the center needs to “move its care beyond the four walls of the organiza-tion,” which is why this bundling option makes sense, Wagner said. “If we remain a traditional medical center where all we care about is the admission, we won’t survive.” the bundling proj-ect would allow tufts Medical Center to expand its reach, and at the same time, help it to defray some of the cost.
technology and People ChallengesUnder debate is what approach will work best to sharing data: a big database that acts as a reposi-tory and allows you to sync your data with it or mul-tiple point-to-point systems that require the right interfaces. Currently, tufts Medical Center uses the latter. “I am sending that information from my hospital-centric system to your electronic medical
record and you can consume it,” Wagner said. however, patients today can interact with multi-
ple providers, each with their own health It system, which requires data sharing. tufts Medical Center is completing an implementation of a single elec-tronic medical record (EMr) for the majority of its ambulatory clinics. however, several clinics require specialized EMrs due to their unique care and management requirements. the tension between a single system and multiple systems optimized for specific clinical areas creates data integration chal-lenges, Wagner said. In a perfect world, a single system shared by tufts Medical Center and all the physicians in its network would be nice, but the re-ality is “we will have multiple different systems.”
health information exchanges, which allow or-ganizations to share health-related data electroni-cally, will go a long way to establishing standards, including how data is structured in a way that it
Health care is ripe for that disruptive change. I think there will be some 23-year-old who will come up with some major initiative and it will blow the socks off of everybody.
50 Leadership | CGI INITIATIVE FOR COLLABORATIVE GOVERNMENT | s p R I N G 2 0 13

can be distributed and consumed. “these point-to-point solutions have been figured out in banking and finance, why not in health care?” he said. “For-tunately, that is changing.”
Making sure the right technology is in place and teaching doctors how to use and incorporate it in their jobs are important pieces of the puzzle. and because tufts Medical Center is a teaching hos-pital, Wagner has the opportunity to do this every day. he likes to remind medical students not to for-get the basics of clinical evaluations, even though much patient health data is readily available elec-tronically. “I worry that students and residents will take shortcuts,” he said. “they look at a prior prob-lem list or medicine list and take it as truth. that’s a concern.”
More change is anticipated, and Wagner thinks that today’s young doctors will help usher it in with new ideas.
“Some of our students and young residents will be part of a disruptive change that will occur in the way we manage patient flow data and how we manage the care of the case,” Wagner said. “health care is ripe for that disruptive change. I think there will be some 23-year-old who will come up with some major initiative and it will blow the socks off of everybody.”
Leading by ExampleWagner, who enjoys spending time with his wife and four kids, said it was his older brother — also a doctor — who helped convince him to pursue a career in medicine. “he said, ‘be a doctor and you will have doors that will open for you your entire life.’”
Wagner remembers his parents dealing with life-threatening illnesses when he was a child. “Medicine helped extend their lives by decades,”
Health Information Exchange
Sharing electronic health care information among individuals,
organizations, communities and hospitals
Hospital
Local public health department
Local public health department
State public health department
Laboratory
Out-patient RX
Physician officeAmbulatory center
Source: Regenstrief Institute
s p R I N G 2 0 13 | COLLABORATIVEGOV.ORG/LEAD | Leadership 51

he said. “Surgical interventions and ongoing medical care really were a testimony to modern medicine and the impact it has on people living long, productive lives.”
Wagner also credits his own drive and other early mentors who influenced his leadership style.
one such mentor was Edmund Pellegrino, for-mer president of Catholic University and founder of the Center for Clinical bioethics at georgetown University, when Wagner was attending medical school at georgetown.
“Pellegrino was the consummate internist,” Wag-ner said. “In a lecture, he would talk about medi-cine, ethics and then he would quote Cicero. and I said, ‘I want to be like him.’”
During his career, Wagner said he interacted with many general internists who have been great role models “because they can speak broadly and they think deeply about issues. It was a natural fit for me.”
For instance, a chief resident he worked with
taught him to be a good listener. “because half of leadership is just listening, a quarter is just reflecting that back and the other quarter is re-ally having a strategic vision of where you want to go.”
In the future, Wagner said, there is a lot more that he wants to accomplish. he sees a lot of po-tential in further developing patient-related medi-cal home initiatives, which coordinate patient care through a primary care physician.
he also is interested in improving the concept of care integration, which helps manage patients as they move from the emergency department to the inpatient unit and back home.
Wagner said he likes where he is — on the pro-vider side, helping solve problems. “I feel that everyone who participates in the conversation is coming with their minds and hearts in the right place,” he said. “by working as a shared collec-tive, we can arrive at the best solution for our patients and organization.” n
By working as a shared collective, we can arrive at the best solution for our patients and organization.
52 Leadership | CGI INITIATIVE FOR COLLABORATIVE GOVERNMENT | s p R I N G 2 0 13

The CGI Initiative for
Collaborative Government
is a joint public policy
project of CGI in partnership
with leading academic
institutions. Launched in
January 2008, the initiative’s
mission is to analyze
models of government’s
collaboration with the
private and nonprofit
sectors in order to identify
best practices in using
collaboration to achieve
mission results.
Today, government
partners with the private
and nonprofit sectors to
accomplish a broad range
of mission-related and
administrative functions.
The question is not whether
collaboration will occur, but
rather how agencies will
collaborate most effectively
while retaining strategic
alignment, control and
accountability.
The CGI Initiative for
Collaborative Government
is focused on helping
government answer this
challenge. We focus our
analysis in special focus
areas, seeking to provide
practical management
approaches that executives
can apply to take strategy
into action.
About the Initiative
Special Focus Areas for 2013

www.collaborativegov.org
12601 Fair Lakes Circle Fairfax, VA 22033
This issue of the CGI Initiative for Collaborative Government’s Leadership is printed using
soy-based inks on FSC®-certified Flo Gloss paper. This paper contains 10% post con-
sumer recycled fiber from well-managed forests, independently certified according to the
standards of the Forest Stewardship Council™.











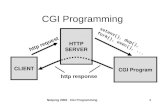


![Cgi animation[2]](https://static.fdocuments.us/doc/165x107/55ce5208bb61eb1c0f8b45f2/cgi-animation2.jpg)




