Bacterial Skin Infection (Staph & Strep) - Lecture Notes - TIU · 2021. 1. 20. · Skin diseases...
Transcript of Bacterial Skin Infection (Staph & Strep) - Lecture Notes - TIU · 2021. 1. 20. · Skin diseases...

Bacterial Skin Infection (Staph & Strep)
Dr. Shler Ghafour RaheemBSc., MSc., PhD Medical Microbiology

Structure of the skin
The skin is divided into three distinct layers:
The epidermis is made up of layeredsquamous epithelium. Hair follicles, sebaceousglands (oil-producing), and sweat glands open to theskin surface through the epidermis.
The dermis is composed of dense connectivetissue rich in blood and nerve endings, andthis is where some hair follicles andsebaceous glands originate.
Diagram of skin

The subcutaneous tissue contains loose connective tissue and isrich in fat. Deeper hair follicles and sweat gland originate in this layer.Below the subcutaneous layer are thin fascial membranes (sheets or bands offibrous tissue) covering muscles, ligaments, and other connective tissues.
Normal Microbiota of the Skin
• Diphtheroids
• Staphylococcus epidermidis
• Other coagulase-negative staphylococci
• Propionibacterium acnes

FUNCTION OF THE SKIN
• The skin is the body’s largest and thinnest organ. It forms a self-repairing and
protective boundary between the body’s internal environment and the external
environment.
• Skin plays a crucial role in the control of body temperature, excretion of water and
salts, synthesis of important chemicals and hormones, and as a sensory organ.
• The skin has an important protective function because of the composition of the
outermost layer of the epidermis, which is composed of cells containing keratin, a
water-repellent protein.
• The skin’s normal microbial flora, pH, and chemical defenses (high salt and acidic
environment) also help prevent colonization by many pathogens.

There are huge numbers of microorganisms.After the gut, there are more microorganisms on the skinthan any where else in the body.
Traditionally swabs are taken of suspected bodysites although tissue or biopsy specimen results moreefficient recovery of these bacteria.
Most of the common infection are caused byStaphylococcus aureus and Streptococcuspyogenes

Staphylococcus spp.
Genus Features
• Gram-positive cocci in
clusters
• Catalase positive
(streptococci are catalase
negative)

Medically important species
Staphylococcus aureus
Staphylococcus epidermidis
Staphylococcus saprophyticus
Staphylococcus aureus is the most virulent member among the genus

Staphylococcus aureus

Staphylococcus aureus
Distinguishing features
• Small, yellow colonies on blood agar.
• Β-hemolytic
• Coagulase-positive (all other staphylococcus are negatve).
• Ferments mannitol on mannitol salt agar.

Virulence factors & pathogenicity
Pathogenicity results from three features
A- Structural components
B-Production of toxins
C- Production of enzymes

A- Structural components
1- Protein A (major protein in the cell wall) binds Fc component of IgG, inhibits phagocytosis.
2- Teichoic acids are polymers of ribitol phosphate. They mediate adherence of the staphylococci to mucosal cells.
3- Polysaccharide capsule. There are 11 serotypes based on the antigenicity of the capsular polysaccharide, but types 5 and 8 cause 85% of infections.

B- Production of toxins
S. aureus causes disease both by producing toxins and by inducing pyogenic inflammation.
Important toxins produced by S. aureus.
1- Enterotoxin
2- Toxic shock syndrome toxin (TSST)
3- Exfoliatin
4- Exotoxins (alpha toxin and Panton-Valentine toxin).

Exotoxins
• Alpha toxin causes marked necrosis of the skin and hemolysis. The cytotoxic effect of alpha toxin is attributed to the formation of holes in the cell membrane
• Panton-Valentine toxin (P-V) is a pore-forming toxin that kills cells, especially WBC, by damaging cell membranes.
• The two subunits of the toxin assemble in the cell membrane to form a pore through which cell contents leak out.
• P-V leukocidin as a virulence factor is indicated by the severe skin and soft tissue infection caused by MRSA strains that produce this leukocidin.

C- Production of enzymes
Coagulase: Converts fibrinogen to fibrin clot.
Fibrinolysin: Dissolves fibrin clots
Hyaluronidase: Breaks down hyaluronic acid and enables the bacteria to spread between cells
Proteases; Hydrolyzes proteines
Nucleases: Degrades DNA in exudates or necrotic tissue.
Lipases: Hydrolyzes lipids

meddic.jp
Skin diseases caused by S. aureus
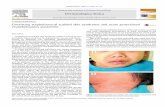
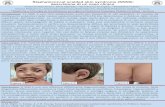
1- Scalded skin syndrome Is a skin infection in which the skin becomes damaged
and sheds.
Exfoliatin causes “scalded skin” syndrome in young children.
Superficial infection that mostly affects young
childrenFace
Limbs
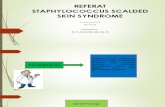
2- Impetigo

3- Folliculitis, Furuncles (boils) and Carbuncles
Folliculitis is a pyogenic infection in the hair follicles
Furuncles is an extension of folliculitis with large, painful
raised nodules that have an underlying collection of dead
and necrotic tissue
Carbuncles occur when furuncles extend to the deeper
subcutaneous tissue

Treatment & Prevention
• Nafcillin/oxacillin are drugs of choice because of widespread antibiotic resistance.
• Vancomycin for methicillin-resistant Staphylococcus aureus(MRSA)
Hand antisepsis important to prevent nosocomial infections

Genus: Streptococcus
• Gram-positive cocciarranged in chains
• Catalase negative

Medically important species
• Streptococcus pyogenes (Group A streptococci; GAS)
• Streptococcus agalactiae (group B streptococci; GBS)
• Streptococcus pneumoniae
• Viridance streptococci
• Enterococcus faecalis, Enterococcus faecium

Streptococci can be classified according to
1- Hemolytic patterns on blood agar:
(A)- α-Hemolytic streptococci (incomplete lysis of red blood cells)
(B)- β-Hemolytic streptococci (complete lysis of the red cells).
(C) - γ-hemolysis: Some streptococci are nonhemolytic.
2- Serologically on presence of C substance
C substance is located in the cell wall, and its specificity is determined by an amino sugar. β-Hemolytic Streptococci are arranged into groups A–U (known as Lancefield groups) on the basis of antigenic differences in C carbohydrate.
A, B and D are more frequent.

Streptococcus pyogenes

Group A Streptococcus (Streptococcus pyogenes)
Distinguishing features
• Β-hemolytic
• Bacitracin sensitive
• Pyrrolidonyl arylamidase (PYR) positive.
Reservoir
- Human throat
- Skin
Transmission
• Human contact
• Respiratory droplets

Virulence Factors & pathogenesis
• M protein (antiphagocytic)
• Capsule (composed of hyaluronic acid) is also antiphagocytic.
Antibodies are not formed against the capsule because hyaluronic acid is a normal component of the body and humans are tolerant to it.

Group A streptococci produce three important inflammation-related enzymes:
(1)Hyaluronidase degrades hyaluronic acid, it facilitates the rapid spread of S. pyogenes in skin infections (cellulitis).
(2) Streptokinase (fibrinolysin) activates plasminogen to form plasmin, which dissolves fibrin in clots, thrombi, and emboli.
(3) DNase (streptodornase) degrades DNA in exudates or necrotic tissue.

Group A streptococci produce five important toxins and hemolysins:
(1) Erythrogenic toxin causes the rash of scarlet fever
(2) Streptolysin O: Hemolysin inactivated by oxidation. It is antigenic.
(3) Streptolysin S: Hemolysin that is not inactivated by oxygen.It is not antigenic.
(4) Pyrogenic exotoxin A: Responsible for most cases of streptococcal toxic shock syndrome.
(5) Exotoxin B is a protease: Rapidly destroys tissue and is produced in large amounts by the strains of S. pyogenes, the so-called “flesh-eating” streptococci that cause necrotizing fasciitis.

Skin diseases caused by S. pyogenes
Erysipelas
Acute infection and imflammation of the dermal layer of skin.

Necrotizing fasciitis
This infection involves the fascia and overlying fat.
It progresses rapidly, having greater risk of developing in the immunocompromised due to conditions such as diabetes or cancer.
microbewiki.kenyon.edu

Impetigo
• S. aureus causes about 80% of cases, and 20% of cases involves S. pyogenesalone or in conjugation with S. aureus
howdoeslooklike.com

Skin diseases caused by S. aureus & S. pyogenes
Cellulitis
• cellulitis is an infection that also involves the skin's deeper layers: the dermis and subcutaneous tissue.
• The main bacteria responsible for cellulitis are streptococcus & Staphylococcus.

Treatment
• Penicillin G or amoxicillin
• Erythromycin or one of its long-acting derivatives (e.g., azithromycin) can be used in penicillin-allergic patients.
• S. pyogenes is not resistant to penicillins.

References
• Patricia M. Tille. Bailey & Scott’s Diagnostic Microbiology. 2017. Fourteenth edition. ISBN: 978-0-323-35482-0. St. Louis, Missouri : Elsevier.
• Robert W. Bauman, Todd P. Primm. Microbiology with Diseases by Body System. 2018. Fifth edition, Pearson.
• Patrick R. Murray, Ken S. Rosenthal, Michael A. Pfaller. 2020. Medical Microbiology. Elsevier