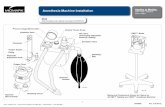
Anesthesia Machine
-
Upload
allredgreg -
Category
Documents
-
view
32 -
download
5
description
Transcript of Anesthesia Machine
KNOW YOUR MACHINE
Why it’s important What it does All its parts All its safety features How to check it
Equipment Misuse
Equipment misuse > Equipment failure ◦ Lack of familiarity ◦ Not checking machine ◦ Only 2% ASA closed claims database ◦ Breathing circuit #1 (39%) Disconnects or misconnects
What does it do?
Gas Supply
Machine Controls flow
Reduces pressure
Vaporizes Agents
Mixes final gas
mixture Delivers to circuit
Circuit attached to patient and
the ventilator
(removable)
Pipeline Inlets
Safety features ◦ Color designation Green = ? Yellow = ? Blue = ?
◦ Diameter-Index Safety System Non-interchangeable Prevents incorrect hose attachment at machine
◦ Filter Traps debris
◦ One-way check valve Prevents retrograde flow
E Cylinders
Attach via Hanger-yoke assemblies ◦ Pin Index Safety System Only O2 cylinder will connect to O2
◦ Washer ◦ Gas filter ◦ Check valve
High-Pressure ◦ Backup for pipeline failure
Handle ◦ Should not be left on at all times ◦ Always check tank volume each morning O2 full = 1800-2200 psi = 625-700L N2O full = 745 psi = 1590 L (have to weigh) Air full = 1800-2200 psi = 625-700L
Flow Control Circuits
Pressure Regulator ◦ Reduces E-cylinder pressure to 45-47 psig ◦ Less than pipeline, so pipeline used preferentially
High Pressure Relief Valve Datex-Ohmeda ◦ Second regulator to drop pipeline and cylinder pressure further O2 20psig N20 38psig
Most machines 45-55 psig
O2 Failure Detection Devices
O2 directly to flow control valve N2O and Air (except Aestiva) ◦ Safety devices first ◦ Allows other gases to flow only if certain pressure of O2 available ◦ Decreases risk of hypoxic mixture
O2 ◦ Pressurizes safety devices ◦ O2 flush valves ◦ Ventilator power
O2 Failure Detection Devices
Datex-Ohmeda ◦ Balance regulator Reduces gases (not air) in proportionate to O2 reduction Shuts off gases below preset O2 pressure ◦ N2O when O2 0.5psig ◦ Other gases when O2 10psig
O2 supply low pressure alarm ◦ Alarm when O2 inlet pressure less than 20-35 psig ◦ Can still get hypoxic mixtures
Flow Valves and Meters
High Pressure System ◦ Proximal to flow valves
Low pressure System ◦ Between flow valves to CGO
Flow valves ◦ Barrier to gas entering vaporizer ◦ Controlled by flowmeters
Flow control valve Knobs
• Turn Counterclockwise • Knobs color-coded • O2 safety features
• farthest to the right • fluted • sticks out the farthest
Flowmeters
Contstant Pressure Variable Orifice ◦ Old Datex (main hospital) ◦ Ball, bobbin or float ◦ Supported by flow of gas ◦ Tube tapered Widens at the top Requires higher flows to keep bobbin afloat
◦ Calibrated for specific gases Depends on viscosity at low flows Depends on density at high flows
◦ Flowmeter malfunction Dirt Vertical tube misalignment Sticking of float at the top
◦ Hypoxic mixture If leak within or downstream from O2 flowmeter
Electronic Flowmeters
• Backup O2 flowmeter • Each gas has a separate flow measurement device before being mixed
Minimum O2 flow
Minimum flow typically 150ml/min ◦ Can be as low as 50ml/min
Some designed to delver < 1L/min
Nitrous –Oxygen link
N20 flow linked to 02 ◦ Ensures minimum 02 of 2l or 25% ◦ Ration controller Mechanically Pneumatically Electronically (our machines)
Vaporizers
All gases must be vaporized Dial in amount added to gas flow from
flowmeters Located between flowmeters and CGO Interlocking exclusion device ◦ One agent at a time
Variable Flow Vaporizer
Concentration dial
Pressure compensator
Wick
Vaporizing Chamber Anesthetic Agent
Concentrating Cone
Temperature Compensating bypass
Outlet port
On/off switch
Vaporizers
Agent Specific Most have agent specific keyed filling ports Can overdose if fill with an agent with higher vapor pressure ◦ i.e. isoflurane in sevoflurane
Tilting ◦ Floods the bypass area = high concentration of anesthetic
Ambient pressure ◦ Vaporizers compensate for altitude changes
Desflurane Vaporizer
Vapor pressure so high = boils at room temperature Problems with delivery ◦ Nml vaporizer can’t deal with cooling from vaporization ◦ Needs high flows to dilute
Tec 6 ◦ Reservoir heated to 39 deg C ◦ No fresh gas flows through reservoir ◦ Vapor released depending on what you dial in and
fresh gas flow Tec 6 plus ◦ Partial pressure of desflurane decreases at
increased altitude = have to increase conc delivered
Common Fresh Gas Outlet
CGO ◦ Only way to get gas to the patient ◦ Adds new gas to circle system
O2 flush valve ◦ High flow ◦ 35-55L/min ◦ Directly to CGO (no gas) ◦ Pressure of 45-55 psig
Breathing Circuit
Circle System ◦ VA conc effected by Lung uptake MV Total FGF Circuit volume Gas leaks
◦ High flows diminishes discrepancies
Extra Components
Oxygen Analyzers ◦ Polarographic, galvanic and paramagnetic ◦ In insp or exp limb Exp lower from oxygen consumption
Spirometers ◦ Measure exhaled TV
Circuit Pressure ◦ Measure between insp and exp limb ◦ Most accurate from Y limb
Extra Components
APL valve ◦ “pop-off” valve ◦ Fully open for spont vent ◦ Partially closed for manual ventilation ◦ Can cause barotrauma if closed too much ◦ Never completely closed
Humidifiers
Intubation prevents normal mechanism of gas humidification ◦ Dehydration of mucosa ◦ Altered ciliary function ◦ Atelectasis ◦ v/q mismatch ◦ Causes loss of heat ◦ Not significant for short cases
Humidifiers
•Passive Humidifiers •Heat and Moisture Exchangers •Added to circuit •Trap heat and moisture from exhaled gas •Increase circuit resistance •Increase dead space
•More of an issue in peds •Active Humidifiers
•Add water to gas via a water chamber or wick •Potential for thermal injuries •We don’t use these
Ventilators
Basic Concepts ◦ Flow generated by pressure gradient between prox airway and alveoli = Positive Pressure Ventilation
Trigger
Trigger = what initiates inspiration Flow trigger (patient) Pressure trigger (patient) Time trigger (Machine)
REGARDLESS of trigger ◦ Machine generates flow along a pressure gradient to reach a predetermined Volume pressure
Cycle
Cycle = what switches from inspiration to expiration ◦ Flow cycle (pressure support) ◦ Time cycle (pressure control) ◦ Volume cycle (volume control)
Insp:Exp Ratio ◦ Determines how long inspiration and expiration are ◦ Usually 1:2 ◦ If RR is 10, each breath = 6s Inspiration 2s and expiration 4s
Exhalation
Exhalation is always passive Airway pressure reduced to Atm pressure or PEEP Effected by ◦ Airway resistance ◦ Lung compliance
PEEP ◦ Positive End Expiratory Pressure Helps prevent de-recruitment ◦ Obese patients ◦ Gravid patients ◦ Pulmonary pts
Ventilator Circuit Design
Double-Circuit System ◦ TV delivered by bellow
Ascending Bellow ◦ Easier to detect leak or circuit disconnect ◦ Pressurized by O2 (45-50psig) ◦ May have higher inspired O2 if leak in bellow
Free breathing valve ◦ Bellows go down with spont ventilation
Piston Ventilator ◦ More accurate with small TV and low lung compliance
APL ◦ Closed during inspiration
Volume and Pressure Monitoring
Peak Inspiratory Pressure ◦ Highest circuit pressure during inspiration ◦ Indication of dynamic compliance
Plateau Pressure ◦ Measured during inspiratory pause (no flow) ◦ Indication of static compliance
Airway Pressures
• PIP and Ppl normally close in value • Increase in both PIP and Ppl
• dec compliance •Edema •Obesity •Packing •insufflation
• increase TV • Increase in PIP only
• increase airway resistance •Bronchospasm •Kinked tube •secretions
• increase in airway flow
Ventilator Alarms
Machine Must Have Alarms!!!!!!!! Disconnect Alarms (at least 3) ◦ Low PIP ◦ Low exhaled TV ◦ Low ETCO2
High PIP High PEEP High sustained airway pressure Negative pressure Low O2 supply pressure
Problems with Anesthesia Ventilators
Fresh Gas Coupling FGF = 6l/min or (100ml/s) I:E = 1:2 and RR = 10 (I=2s and E=4s) Extra TV of 200ml with each breath Increases PIP Increases MV
Positive Pressure ◦ Can cause barotrauma ◦ Avoid O2 flush during inspiration ◦ Many machines have built in APL valves
Problems with Anesthesia Ventilators
Tidal Volume Discrepancies ◦ FGF coupling ◦ Circuit compliance 5ml/cmH2O (if PIP 20 then 100ml lost)
◦ Gas Compression in bellows 3% loss normally
◦ Sampling lines CO2 and volatile agents
◦ Must measure at Y connector to get accurate data ◦ New Machines compensate
Scavenging Systems
Waste gas = Health Hazard NIOSH limits ◦ N20=25ppm ◦ VA= 2ppm (0.5ppm w/ N20)
Gas vented through APL valve and spill valve ◦ Both valves connected to scavenging interface ◦ Open Interface – open to outside w/o pressure relief
valves ◦ Closed Interface – requires neg and pos pressure relief
valves to protect the patient Passive vs Active ◦ Vacuum system is active ◦ Vacuum is full = waste reservoir ◦ Vacuum control 10-15l/min Adequate for high flow and low flow
Machine Checkout
The more you check it the better you’ll understand it i.e. you will remember it for boards