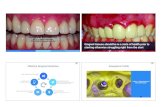
Acute gingival infrections
-
Upload
saeed-bajafar -
Category
Education
-
view
3.337 -
download
4
description
Transcript of Acute gingival infrections


Necrotizing Ulcerative Gingivitis (NUG)
Trench Mouth.Vincent Infection.Acute Ulceromenbranous Gingivitis.Fusospirochetal GingivitisAcute Ulcerative Gingivitis

Necrotizing Ulcerative Gingivitis (NUG)
It is a painful, inflammatory destructive disease which affect marginal and papillary gingiva
and less frequently the attached gingiva.

Classification
Acute Subacute
A single tooth A group of the teeth May be wide-spread
throughout the mouth.

Oral Signs
Craterlike depressions at the crest of the interdental papilla
Oral SignsOral Signs
Sudden onset


Sometimes the lesions are denuded of the surface pseudomembrane, exposing the gingival margin which is red, shiny and hemorrhagic.

Other Signs Gingival hemorrhage
Fetid odor (Halitosis).
Increased of salivation.
The disease can occur in otherwise disease- free mouth or can be superimposed on chronic gingivitis or periodontal pockets.
Other SignsOther Signs

The gingiva is extremely sensitive to touch.
Constant, radiating, gnawing pain.
Metallic unpleasant taste.
Excessive amount of “pasty” saliva.
Oral Symptoms Oral Symptoms

Patients are usually ambulatory and have a minimum of systemic complications.
Local lymphadenotathy and slight elevation of the temperature.
Insomnia, fatigue, anorexia, gastrointestinal disorders, headache and mental depression (sometimes).
Extraoral and Systemic Signs and Symptoms Extraoral and Systemic Signs and Symptoms

Predominantly spirochetes and fusiform bacilli.
EtiologyEtiology
Bacterial Flora

Local Predisposing Systemic Predisposing Factors Factors
Preexisting chronical gingivitis and periodontal pocket.
Predominance of Spirochetes, Bacteroides and Fusiform bacteria in the plaque.
Plaque retentive areas and areas of the gingiva traumatized.
Smoking
Nutritional Deficiencies.
Debilitating Diseases:
Psychosomatic Factors

DiagnosisBased on clinical findings of gingiva.
Epidemiology and Prevalence An epidemic pattern. Occurs at all age. It is not common in children.
CommunicabilityIt has not been shown to be communicable or contagious.

. First Visit. History of the Chief Complaint.
Extraoral and Intraoral Examination.
Isolated with cotton rolls and dried.
Apply topical anesthesia
The areas are swabbed by a cotton pellet with normal saline or hydrogen peroxide 3%.
TreatmentTreatment

Remove supra gingival calculus.
All procedures such as extractions or periodontal surgery are postponed until the patient has been symptom free for a period of 4 weeks.
The patient is instructed to rinse the mouth every 2 hours with a glassful of an equal mixture of warm water and 3% hydrogen peroxide or twice daily rinse with 0.12% chlorhexidine.
TreatmentTreatment

Antibiotic treatment in moderate or severe NUG and local lymphadenopathy or other systemic symptoms (penicillin, 500mg orally every 6 hours or erythromycin in the same way).
Metronidazole (500 mg twice times daily for 7 days).
TreatmentTreatment

Instructions to the patient
1.Avoid tobacco, alcohol and condiments.
2. Avoid excessive physical exertion.
3. Confine tooth brushing to the removal of surface debris with a bland dentifrice.
TreatmentTreatment

Second Visit: (1 or 2 days ago)
Scaling, if sensitivity permits. Shrinkage of the gingival may expose the
previously covered calculus, which is gently removed.
The instructions to the patient are the same.
TreatmentTreatment

Third visit: (1 or 2 days after the second)
TreatmentTreatment
Scaling and root planning are repeated. The patient is instructed in plaque control procedures. The hydrogen peroxide rinses are discontinued. Maintain chlorhexidine rinses for 2 or 3 weeks.

Subsequent Visits The tooth surfaces in the involved areas are
scaled and smoothed. Plaque control by the patient is checked and
corrected if is necessary. Comprehensive treatment of the patient's
chronic periodontal problem should start (chronic gingivitis, periodontal pockets, etc)
Additional Treatment (Gingivectomy)

Primary Herpetic Gingivostomatitis
Is an infection of the oral cavity caused by herpes simplex virus type 1 (HSV -1)

Oral SignsOral Signs Diffuse, erythematous and shiny gingiva and the
adjacent oral mucosa.
Varying degrees of edema and gingival bleeding.
Presence of discrete, spherical gray vesicles which may occur on the gingiva, labial and buccal mucosa, soft palate, pharynx, sublingual mucosa and tongue.

Oral SignsOral Signs
A painful, small ulcers with red, elevated, halolike margin and a depressed, yellowish or gray-wite central portion

Occasionally may occur without overt vesiculation.
The course of the disease is limited from 7 to 10 days.
The diffuse gingival edema and erythema may persist for several days.
Scarring does not occurs in the areas of healed ulcerations.
Oral SignsOral Signs

Generalized “soreness” of the oral cavity, which interferes with eating and drinking.
The rupture vesicles are the focal sites of pain.
Oral Symptoms Oral Symptoms

Cervical adenitis, fever as high 101 to 1050 F (38.3 to 40.60 C) and general malaise are common.
Extraoral and Systemic Signs and Symptoms Extraoral and Systemic Signs and Symptoms

History:Recent acute infection is a common feature of the
history of the patient.
Diagnosis:
The diagnosis is usually established from the patient’s history and the clinical findings.
Communicability:This disease is contagious. Most adults have
developed immunity to HSV as the result of infection during childhood.

Topical local anesthetic .
Orabase compounded with high-potency topical steroids (e.g., clobetasol).
Clorhexidine mouthwash.
Acyclovir preparations (antiviral agents) may be prescribe for topical and systemic.
TreatmentTreatment It is directed to alleviates the symptoms

Supportive Treatment Panadol or nonestoroidal anti-
inflammatory agent for the relieve of pain. Copious fluid intake. Systemic antibiotic therapy for the
management of toxic systemic complications in severe cases. No penicillin (may aggravate the herpetic lesions).
The patient should be informed that the disease is contagious at certain stages such as when vesicles are present. All individuals exposed to an infected patient should take precautions.

RECURRENT APHTOUS STOMATITIS
It is a disorder characterized by recurring painful ulcersin the oral mucosa, which vary in shape, number and size.It is a disorder characterized by recurring painful ulcersin the oral mucosa, which vary in shape, number and size.

RAS affects 20% of the general population.
Can affects both sex, women are more susceptible.
It is classified according to clinical characteristics as Minor ulcers, Major ulcers and Herpetiform ulcers.

ETIOLOGYETIOLOGY Hereditary factors. Immunologic Disorders. Psychosomatic Disorders. Gastrointestinal Diseases. Trauma. Endocrine Factors. Allergy. Hematological and Nutritional Deficiencies. Smoking.

Minor ulcers, comprise more than 80% of RAS cases, are less than 1 cm in diameter and heal without scars.
Major ulcers are over 1 cm in diameter, take longer to heal and often scar on healing.
Herpetiform ulcers are considered a distinct clinical
entity that manifests as recurrent crops of dozens of small ulcers (2- 3 mm) throughout the oral mucosa.

Topical Therapy
Medication prescribed to treat RAS should relate to the severity of the disease.
In mild cases, use of topical coating agents such as Orabase or Zilactin is appropriate.
Pain relief can be obtained with the use of a topical anesthetic agent, such as benzocaine in Orabase.
TREATMENT

In more severe cases, the use of a high potency topical steroid.
Other topical preparations that have been shown to decrease the healing time of minor RAS lesions include topical tetracycline

Gingival Abscess
Is a lesion of the marginal or interdental gingiva, usually produced by an impacted foreign object.

CLINICAL CHARACTERISTICS Sudden onset, painful.
Red, rounded swelling localized to the papilla and marginal gingiva with smooth and shinny surface.
The adjacent teeth may be sensible during percussion.

TreatmentTreatment
Under topical and local infiltrative anesthesia, the fluctuant area of the lesion is incised with # 15 blade, and the incision is gently widened to permit the drainage. The area is cleansed with warm water and covered with a gauze pad.

After bleeding stops, the patient is dismissed for 24 hours and instructed to rinse every 2 hours with a glassful of warm water.
When the patient returns, the lesion generally is reduced in size and free of symptoms.
Apply topical anesthesia and make the scaling of the involved area.
TreatmentTreatment

Bibliography Carranza´s. Clinical Periodontology. 9th
ed. 2003. pg:15-55. Gururaja R. Textbook of Periodontology.
2nd ed. pg: 6. Klaus H. Color Atlas of Dental Medicine.
Periodontology. Vol 1. 1989. pg: 1- 10.