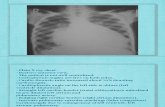
Xray of Bones in Osteomyelitis
-
Upload
bukola-ajoke -
Category
Documents
-
view
279 -
download
0
Transcript of Xray of Bones in Osteomyelitis

ROENTGENOGRAPHY AS DIAGNOSTIC TECHINIQUE
MORONIKE OLUBUKOLA AJOKEGROUP: 501
FACULTY: IMFDEPARTMENT: RADIOLOGICAL
MEDICINE

Defining Osteomyelitis
What’s in a Name?
Osteomyelitis (Osteo- bone, Myelo- Marrow, and –itis -Inflammation)

Defining Osteomyelitis
What is it?
It is an infection of the of the bone or bone marrow which leads to a subsequent
Inflammatory process.

TYPES OF OSTEOMYELITIS
Acute, subacute and chronicPediatric and adulthoodHematogenous, by direct spread, contigous,
associated with diseaseTraumatic and post traumatic


Acute Osteomyelitis
Types of Acute Osteomyelitis
I. Hematogenous Osteomyelitis
II.Direct Inoculation Osteomyelitis

Acute Osteomyelitis
Hematogenous Osteomyelitis:
Bacterial seeding from the blood.
Seen primarily in Children.
The most common site is the Metaphysis at the growing end of Long Bones in Children, and The Vertebrae and pelvic in Adults.

Acute Osteomyelitis
Direct Inoculation Osteomyelitis
Direct contact of the tissue and bacteria as a result of an Open Fracture or Trauma.
Tend to involve multiple organisms.

Acute Osteomyelitis
Causative Organisms: Staphylococcus aureus (Mainly)
Streptoccous pyogens or pneumoniae. (Less)
H.Influenzae (Young Children)
Salmonella (Sickle-Cell)

Acute Osteomyelitis
Imaging: First 10 days X-Rays Show No Abnormality. By the end of the 2nd Week signs of
rarefaction of Metaphysis and New Bone Formation.
With Healing there is Sclerosis and thickening of Cortex.
MRI may help to distinguish between Bone and Soft-Tissue Infection.

Joint involvement common Septic arthritis X-ray findings Initial radiographs often normal for as long as 7-10 days Localized soft-tissue swelling adjacent to metaphysis
with obliteration of usual fat planes (after 3-10 days) Area of bone destruction (lags 7-14 days behind
pathologic changes) Involucrum = cloak of laminated /spiculated periosteal
reaction (develops after 20 days) Sequestrum = detached necrotic cortical bone (develops
after 30 days) Cloaca formation = space in which dead bone resides

Radiological studiesX-Ray:
First sign is soft-tissue edema at 3-5 days after infection.
Bony changes are not evident for 14-21 days:
1. early radiographic signs of rarefraction (thining of bony tissue sufficient to cause decreased density of bone) of the metaphysis and periosteal new bone formation
2. increasing ragged if treatment is delayed
3. sclerosis and thickening of the bone at healing
Approximately 40-50% focal bone loss is necessary to cause detectable lucency on plain films.

Plain-film radiograph showing osteomyelitis of the second metacarpal (arrow). Periosteal elevation, cortical disruption and medullary involvement are present.

Osteomyelitis of index finger metacarpal head secondary to clenched fist
injury

Osteomyelitis of elbow

Septic arthritis of right hip

The above X-ray of the right ankle of a 10-year-old boy shows lucency in the tibial metaphysis secondary to acute hematogenous osteomyelitis (AHO).
The above X-ray of the left ankle of a 10-year-old boy shows lucency in the tibial metaphysis secondary to acute hematogenous osteomyelitis (AHO).

Here is an X-ray of an AHO lesion extending into the growth plate.

Streptococcal osteomyelitis in a 3-year-old patient presenting with periosteal new-bone formation of the tibia



Subacute Osteomyelitis
Results from a less virulent Microorganism, or a patient with an elevated resistance.
Occurs Mostly at the Distal Femur or Proximal Tibia
On X-Ray we See Brodie’s Abcess:
Small and Oval in shape
It is surrounded by sclerotic bone
May be mistaken for Ostieoid Osteoma

A Brodie abscess is a subacute osteomyelitis with a predilection
for the ends of long bones and the carpus and tarsus. Plain radiographic findings include the following: (1) a central area of radiolucency with a surrounding thick rim of reactive bone sclerosis, which may persist for months; (2) pathognomonic tortuous parallel lucent channels extending toward the growth plate; (3) a variable degree of periosteal new-bone formation; and (4) associated soft-tissue swelling.

Brodie’s abscess, a localised radiolucency usually seen in the metaphyses of long bones. It is sometimes difficult
Treatment of Brodie’s abscess in the metaphysis includes surgical curettage

Subacute Osteomyelitis An image depicting subacute osteomyelitis

Chronic Osteomyelitis

Chronic osteomyelitis is a severe, persistent, and sometimes
incapacitating infection of bone and bone marrow. It is often a recurring condition because it is difficult to treat definitively.

This disease may result from
(1) inadequately treated acute OSM (2) a hematogenous type of osteomyelitis; (3) trauma, (4) iatrogenic causes such as joint replacements and the internal fixation of fractures; (5) compound fractures; (6) infection with organisms, such as Mycobacterium tuberculosis and Treponema species (syphilis); and (7) contiguous spread from soft tissues, as in diabetic ulcers or ulcers in peripheral vascular disease

RadiographyFindingsPlain radiographic findings in acute or sub acute osteomyelitis are deep soft-tissue
swelling, a periosteal reaction, cortical irregularity, and demineralization. The chronic phase of the disease is characterized by thick, irregular, sclerotic bone interspersed with radiolucency, an elevated periosteum, and chronic draining sinuses.
Sclerosing osteomyelitis of Garré most commonly affects the mandible and appears with a focal sclerosing periosteal reaction on radiologic studies.
Chronic recurrent osteomyelitis is benign self-limiting condition that primarily affects long bones in children and adolescents. The metaphysis of long bones are usually affected, and changes may be symmetrical. The appearances are those of confluent areas of bone lysis.
.False Positives/NegativesStress fractures, osteoid osteomas, and other causes of periosteitis may
mimic acute or chronic osteomyelitis.

Osteomyelitis, chronic. Sequestrum of the lower tibia


Osteomyelitis, chronic. Sclerosing osteomyelitis of the lower tibia. Note the bone expansion and marked sclerosis.

Sequelae of Osteomyelitis:Chronic
•Sinus –Intermittent drainage
•Sequestrum –Dead bone
(sclerotic) –Failure to resorb
•Involucrum –New bone envelope •Pathologic fracture

Tuberculous osteomyelitis of sternum

References American Diabetes Association, Consensus Reports
http://care.diabetesjournals.org/content/vol28/suppl_1/
Reese RE, Belts RF: A Practical Approach to Infectious Diseases, 3rd Ed.,Boston: Little, Brown and Company;1991:464-498
Resnick D: Diagnosis of Bone and Joint Disorders, 3rd Ed., Philadelphia:W.B. Saunders Company;1995:Vol. 4,2323-2558.
Weinstein SL, Buckwalter JA: Turk’s Orthopedics Principles and their Application,5th Ed.,Philadelphia:J.B.Lippincott Company;1994.
http://emedicine.medscape.com/article/785020-workup#a0720