Ureters Slender tubes attaching the kidney to the bladder Continuous with the renal pelvis Enter...
-
Upload
matilda-thornton -
Category
Documents
-
view
218 -
download
5
Transcript of Ureters Slender tubes attaching the kidney to the bladder Continuous with the renal pelvis Enter...

Ureters Slender tubes attaching the
kidney to the bladder
• Continuous with the renal pelvis
• Enter the posterior aspect of the bladder
Runs behind the peritoneum
Peristalsis aids gravity in urine transport

Urinary Bladder Function
• Smooth, collapsible, muscular sac
• Temporarily stores urine
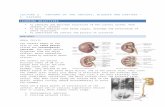
Trigone Structure
Bladder Wall
• Three layers of smooth muscle (detrusor muscle)
• Mucosa made of transitional epithelium
• Walls are thick and folded in an empty bladder
• Bladder can expand significantly without increasing internal pressure
• Internal and external sphincters
Figure 15.6

Urethra Thin-walled tube that carries urine from the bladder to
the outside of the body by peristalsis
Release of urine is controlled by two sphincters
• Internal urethral sphincter (involuntary)
• External urethral sphincter (voluntary)
Length and Location
• Females – 3–4 cm (1 inch), along wall of the vagina
• Males – 20 cm (8 inches) through the prostate and penis
Function
• Females – only carries urine
• Males – carries urine and is a passageway

Micturition (Voiding) Both sphincter muscles must open to allow
voiding
• The internal urethral sphincter is relaxed after stretching of the bladder
• Activation is from an impulse sent to the spinal cord and then back via the pelvic splanchnic nerves
• The external urethral sphincter must be voluntarily relaxed

Urinary System I: Kidneys and Urine Formation Functions of the Urinary System
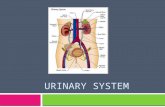
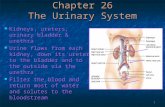
Organs of the Urinary System
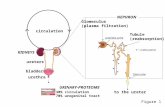
The Kidney
• Coverings and Regions
• Blood Flow
• Nephrons: Glomeruli and Renal Tubules
• Urine Formation
Urinalysis
Ureters, Bladder, and Urethra

Characteristics of Urine Used for Medical Diagnosis
Colored somewhat yellow due to the pigment urochrome (from the destruction of hemoglobin) and solutes; darker if patient dehydrated, lighter if over hydrated.
Sterile
Slightly aromatic
Normal pH of around 6
Specific gravity of 1.001 to 1.035; higher if concentrated, lower if dilute.
Checking for
• Glycosuria (excessive sugary food intake or diabetes)
• Proteinuria (intense exercise, pregnancy, hypertension)
• Pyuria (pus from urinary tract infections)
• Hemoglobinuria (from transfusion reactions or hemolytic anemia)
• Bilirubinuria (hepatitis)
• Pyelonephritis (high specific gravity)

Urinary System II: Fluid, Electrolyte, and Acid/Base Balance Distribution of Body Fluid
Maintaining Water Balance
Hormornal Regulation of Water and Salt
Acid-Base Balance
• Blood Buffers
• Regulation by Lung Respiration
• Regulation by Kidney on Bicarbonate
Developmental Aspects of the Urinary System

Most Body Fluid is Within Cells Intracellular fluid (inside
cells)
Extracellular fluid (outside cells)
• Interstitial fluid
• Blood plasma
Normal amount of water in the human body
• Young adult females – 50%
• Young adult males – 60%
• Babies – 75%
• Old age – 45%
•Low Na+ and Cl–
•Major cation: K+
•Major anion HPO42–

Maintaining Water Balance Water intake must equal water output
• Sources for water intake
o Ingested foods and fluids
o Water produced from metabolic processes
• Sources for water output
o Vaporization out of the lungs
o Lost in perspiration
o Leaves the body in the feces
o Urine production
Urine Output
• Dilute urine is produced if water intake is excessive
• Less urine (concentrated) is produced if large amounts of water are lost
• Proper concentrations of various electrolytes must be present

Maintaining Water and Electrolyte Balance

Maintaining Acid-Base Balance in Blood Blood pH must remain between 7.35 and 7.45 to maintain
homeostasis
• Alkalosis – pH above 7.45
• Acidosis – pH below 7.35
Most ions originate as byproducts of cellular metabolism
Acid-base control
• Blood buffers (immediate, first line regulator of pH)
• Respiration rate (reacts in 1-3 minutes)
• Renal/Kidney mechanisms exert strongest effect but slow (hours-days)

Chemical Buffer Systems of the Body
1. Bicarbonate buffer system
o Major buffer for the extracellular fluid, also intracellular fluid
o H2O + CO2 <--> H2CO3 <--> HCO3- + H+
2. Phosphate buffer system
o Effective buffer in urine and ICF, where phosphate concentrations are high
o (H3PO4 <--> H2PO4– + H+ <--> HPO4
2– + H+),
3. Protein buffer system
o Mostly active within cells, some effects in plasma
o Amino groups bind H+ (-NH2 + H+ <--> NH3+)
o Carboxyl groups remove OH- (-COOH + OH- <--> -COO- + H2O
Buffers react to prevent dramatic changes in hydrogen ion (H+) concentrations
• Bind to H+ when pH drops
• Release H+ (or bind OH-) when pH rises

The Bicarbonate Buffer System

Renal Mechanisms of Acid-Base Balance Excrete bicarbonate ions if needed
Conserve or generate new bicarbonate ions if needed
• Bicarbonate conservation or production causes rise in blood pH
• Bicarbonate excretion causes fall in blood pH
• H+ excretion in the urine
Urine pH varies from 4.5 to 8.0-+
2 2 2 3 3CO + H O H CO H + HCO

Acidosis and Alkalosis: Why It Matters Acidosis
• Blood pH below 7 depression of CNS coma death
• Enzymes denature
Alkalosis
• Blood pH above 7.8 excitation of nervous system muscle tetany, extreme nervousness, convulsions, respiratory arrest
• Enzymes denature

Metabolic Acidosis and Alkalosis Any pH imbalance not caused by abnormal blood CO2 levels;
indicated by abnormal HCO3– levels
Metabolic Acidosis
• Caused by ingestion of too much alcohol ( acetic acid), excessive loss of HCO3
– (e.g., persistent diarrhea)
• Causes by accumulation of lactic acid, shock, ketosis in diabetic crisis, starvation, and kidney failure
Metabolic Alkalosis (much less common than metabolic acidosis)
• Indicated by rising blood pH and HCO3–
• Caused by vomiting of the acid contents of the stomach or by intake of excess base (e.g., antacids)

Developmental Aspects of the Urinary System Fetal Development and Newborns
• Functional kidneys are developed by the third month
• Urinary system of a newborn
o Bladder is small
o Urine cannot be concentrated
• Control of the voluntary urethral sphincter does not start until age 18 months
• Urinary infections are the only common problems before old age
Effects of Aging on Urinary System
• There is a progressive decline in urinary function
• The bladder shrinks with aging
• Urinary retention is common in males
Congenital Abnormalities of the Urinary System
• Polycystic kidney
• Hypospadias
Hypospadias

Urinary System II: Fluid, Electrolyte, and Acid/Base Balance Distribution of Body Fluid
Maintaining Water Balance
Hormornal Regulation of Water and Salt
Acid-Base Balance
• Blood Buffers
• Regulation by Lung Respiration
• Regulation by Kidney on Bicarbonate
Developmental Aspects of the Urinary System