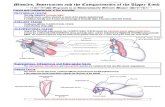
Upper Limb Cases- Case 4
description
Transcript of Upper Limb Cases- Case 4

UPPER LIMB CASES- CASE 4
Group 4David Folt, Stephen Smith, Valerie
Allen, Amanda Foley

PATIENT PROFILE A 17 year-old male student athlete Chief complaint: complains of a “bad shoulder”Vital signs: Blood Pressure: 125/75 Pulse: 58 bpm Rhythm: Regular Temperature: 97.6oF Respiratory rate: 13 bpm Height: 6’0” Weight: 200 lbs. General: No cutaneous sensory changes were found.
No swelling or changes in perfusion were noted. All other systems: Normal

HISTORY OF PRESENT ILLNESS He was performing bench press without a spotter
when his left upper limb and shoulder were pushed posteriorily past the bench by the shifting weight.
He states that he felt “an electric shock” inside his left shoulder.
When he was free from the weight bar and was able to stand up, he found that could not raise his left arm away from his body.
Following the incident he went home, took some “pain medicine”, and went to bed.
During the next several days he experienced pain and “stiffness”, especially in his chest and left upper limb.

MUSCULOSKELETAL EXAMINATION Left shoulder:
a decrease of muscular tone (firmness) on the posterior scapula
The glenohumeral joint allows a greater degree of manual movement Flexion/extension, medial/lateral rotation present
but not smooth Inability to voluntarily abduct the left arm
from anatomical position to 90 degrees Ability to maintain the position of 90 degree
abduction if the limb is placed in that position

QUESTION 1 1) Which bone(s) and or ligament(s),
if any, have been directly damaged?

ANSWER 1 Bones:
Probably none involvedWhy?
Ligaments: If any, fibrous joint capsule involved in
glenohumeral jointHeavily involved in glenohumeral
stability, possible compromised stability

QUESTION 2 The function of which muscle/tendon
unit(s), if any, has been altered by this event? How has the function been altered?

ANSWER 2 Possible muscles involved:
Supraspinatus Cannot abduct from anatomical position to 30 degrees
Infraspinatus Weakened lateral rotation Quick! What nerve innervates supra/infraspinatus?
Deltoid Possible strain, no innervations affected Clavicle Deltoid tuberosity connection affected in the
incident Flexion/Extension, lateral/medial rotation are not smooth
movements Pectoralis major
Pain/stiffness, swelling in chest Hyperextension of muscle during the incident

QUESTION 3 The function of which peripheral
nerve(s), if any, has been altered by this event? How has the function been altered?

ANSWER 3ANerves Involved: Suprascapular
Supraspinatus and infraspinatus
Where does the suprascapular n. come from?
NOT axillary Deltoid maintains functionality

ANSWER 3BHow has nerve function been
altered? No sensory changes, therefore not
severed Other nerves that are continuous with
the upper trunk are not affected (i.e. musculocutaneous, and he has no problems with anterior compartment muscles of arm)

QUESTION 4 With a working assumption (hypothesis)
that a tendon has been torn, when might the patient expect to have a return of function or elimination of symptoms related to his injury?

ANSWER 4 Although we have not discussed the
specific surgical techniques for repairing tendons, it is our understanding that the tendon will not regain original function unless appropriate medical interventions are used
Depending on the length of time the muscle remains inactive due to the injury, some sort of physical rehabilitation would be necessary

QUESTION 5 If a nerve were injured (crushed), when
might the patient expect to have a return of function or elimination of symptoms related to his injury?

ANSWER 5 The patient would require conservative
therapy consisting of rest, anti-inflammatory medication, and physical therapy designed to increase muscular tone and strength. (Safran MR: Nerve injury about the shoulder in athletes, part 1: Suprascapular nerve and axillary nerve. Am J Sports Med 2004;32:803.)
Surgical intervention is used if the initial non-invasive treatment is ineffective(Cummins, CA, Schneider DS. Peripheral Nerve Injuries in Baseball Players. Neurologic Clinics 2008; 26:1)