Tissues: Living Communities Chapter 4. Introduction Since cells are differentiated, they have lost...
Transcript of Tissues: Living Communities Chapter 4. Introduction Since cells are differentiated, they have lost...

Tissues: Living Communities
Chapter 4

Introduction• Since cells are differentiated, they have
lost ability to perform all metabolic functions required to sustain life as an isolated entity.
• Cells exist in cooperative communities in multicellular organisms
• Cells of similar type and function cluster together to form tissues.


Classification of Tissues• Epithelial tissue
• Covers and lines• Connective tissue
• Provides support• Muscle tissue
• Enables movement• Nervous tissue
• Controls work


Classification continued• Most organs contain all 4 tissue types.• The study of microscopic structures of
tissues and organs is called histology or microscopic anatomy.
• What is gross anatomy?

Epithelial Tissue• Composed of sheets of cells that cover
and line other tissues.• Bladder, mouth, blood vessels, thorax,
etc.• Have an exposed surface that affords
access to the surrounding environment or to the inner openings of chambers and ducts.
• Acts as interface layer that separates and defines the beginning and ending of different types of tissues.

Epithelial functions• Acts as protection for underlying tissues• Filter of biochemical substances• May be absorptive• May play an important role in sensory
input• Secretion and excretion of biochemical
substances• Epithelia that do this are called
glandular epithelia• Individual glandular epithelia are goblet
cells.

Characteristics of Epithelia• Organized into tightly packed groups that form
sheets of tissue.• Can be composed of single layer or multiple layers
depending on location.• Epithelial cells share the following characteristics:
• Polar - Each epithelial cell has an apical surface and a basal surface
• Apical surface faces the lumen or body cavity
• Basal surface faces the underlying connective tissue
• Lateral surfaces are connected to neighboring cells by junctional complexes
• Epithelial cells are avascular• Most epithelial cells are innervated

Epithelial Tissue: Cellular Attachments• Epithelial cells are held together in many ways• Between the cell membranes of adjacent cells are channels that carry
nutrients to the cells and waste away• Junctional Complexes – specialized attachments between epithelial cells
• 3 major types:• Desmosomes
• Welded plaque• Tough, resist tension and stretching (like Velcro)• Skin, heart, uterus
• Gap junctions• Cytoplasm continuous• Exchange ions, nutrients – quickly transmit signals through
connexons• Cardiac, smooth muscles
• Tight junctions• Nothing can penetrate• Prevent leakage• Bladder, GI tract


Epithelial Cells: Basement Membrane• Foundation of epithelial cells• Meshwork of fibers that cements epithelial cell to
underlying connective tissue (CT)• Also called basal lamina• Varies in thickness
• Where might thickness vary?• Helps prevent cell from being torn off by intraluminal
pressures• Acts as a partial barrier between epithelial cell and
underlying CT – substances have to travel through basement membrane to get in and out of epithelial cells.


Surface Specialization• Surfaces vary depending on location in body and
function• May be smooth or contain microvilli-fingerlike
projections, or cilia-hairs• If the cell contains microvilli, it is said to have a
brush border.• Brush border helps to increase surface
area, which aids in absorption. (can add up to 20 times of surface area).
• Skin may have keratin-waterproof substance• Keratin may accumulate as cell matures and
moves from basal layer to superficial layer of integument.




Classifications of Epithelia• Characterized by 3 characteristics
• Number of layers of cells• Single layer is called simple
• Found in protected parts of body because provide minimal protection to underlying structures
• More than one layer is called stratified.• Thicker and stronger and are on parts of
body that are subjected to mechanical or chemical stress.
• Shape of cells• Based on shape that is on exposed or luminal
surface• Squamous, cuboidal, and columnar
• Presence of surface specializations• Keratinized, ciliated, etc.


Simple Squamous Epithelium• Fragile and thin • Found lining surfaces involved
in the passage of either gas or liquid (lining of lungs, kidneys)
• Flat and smooth• Mesothelium – lining of chest
(pleura), abdomen (peritoneum), and pericardium
• Endothelium – lining of bloodvessels


Simple Cuboidal Epithelium• Single layer of cube-shaped
cells • Round, dark-staining nuclei
aligned in a single row • Occurs in areas of the body
where secretion and absorptiontake place• Surface of ovaries, glands, lining
of ducts of liver, kidneys, pancreas



Simple Columnar Epithelium• Elongated and closely packed
together - thicker• Nuclei aligned in a row at the
base of the cell near the basement membrane
• Line the GI tract from stomach to rectum• absorptive cell- apical surface is blanketed by
dense microvilli that maximize absorption by increasing surface contact with nutrient-filled lumen.
• goblet cell- manufacture and store mucus for lubrication
• Found in many excretory ducts



Stratified Squamous Epithelium
• Multilayered • Occur in areas of the body
subject to mechanical and chemical stresses• Mouth, esophagus, vagina,
rectum
• Continually being wornaway or sheared off
• Replaced by cells from a deeper layer


Stratified Cuboidal Epithelium
• Usually two layers of cuboidal cells
• Found primarily along large excretory ducts• Salivary glands,
mammary glands, sweat glands


Stratified Columnar Epithelium
• Found only in select parts of the respiratory, digestive, reproductive systems and along some excretory ducts
• Rare• Function in secretion and
protection


Pseudostratified Columnar Epithelium• “False” stratified – truly simple• Cell nuclei are found at different levels
across the length of the tissue• Some cells do not reach luminal
surface but all attach to basement membrane.
• Usually ciliated• Found in respiratory tract and in
portions of male reproductive tract• trachea



Transitional Epithelium• Stratified epithelium
• basal layer of cuboidal or columnar cells • superficial layer of cuboidal or squamous
cells• Ability to stretch - found in areas
where changes in volume occur• Bladder, ureters, urethra
• As epithelia stretches, layers often thin depending on how much volume is present
• Also form a leak-proof barrier



Glandular Epithelia• Gland- a cell or group of cells that have ability to manufacture
and discharge a secretion.• Secretions- specialized protein molecules that are produced
in the RER, packaged by the golgi and discharged from the cell.
• Glands can be organized by factors:• Presence or absence of ducts
• Endocrine vs. Exocrine • Number of cells that compose them
• Unicellular vs multicellular• Shape of secreting ducts
• Simple or compound• Complexity of glandular structure
• Tubular, acinar, tubuloacinar• Type of secretion made
• Mucoid or serous• Manner in which secretion is stored and discharged
• Merocrine, apocrine, or holocrine

Endocrine GlandsEndocrine Glands• No ducts• Blood stream delivers secretions to entire body• Secrete hormones
• Regulate body functions (growth, maturity, sex cycle)• Part of Endocrine System


Exocrine GlandsExocrine Glands
• Contain ducts (except for Goblet cells)• Have local effect
• Salivary• Pancreas, liver (digestive enzymes)• Musk (scent)• Sweat• Anal (scent glands)



Unicellular Exocrine Gland:Unicellular Exocrine Gland: Goblet Cell Goblet Cell
• Ductless• Opens into GI, respiratory
tracts, conjunctiva• Composed of modified
columnar epithelial cell • Secretes mucin: mixed with
water → mucus

Multicellular Exocrine Glands
• Contains:• 1) secretory unit
• Secretory unit usually surrounded by connective tissue rich in blood vessels and nerve fibers
• 2) a duct • May be surrounded by
myoepithelial cells that assist with the discharge of secretions into the glandular duct

Classification of Multicellular Exocrine Glands: Shape• Based on shape and number of tubes

Classification of Exocrine Glands: Manner of secretion• Merocrine
• glands package their secretions and release them via exocytosis as they are manufactured
• Majority of glands• (ex: pancreas, sweat, salivary)
• Apocrine • glands store their secretions and then release
the top part (apex) of the cell into the duct system
• (ex: mammary, some sweat)
• Holocrine • glands store their secretions and then release
the entire contents of the cell • (ex: sebaceous)





Classification of Exocrine Glands:Type of Secretions Produced
Type of secretion produced• Serous secretions
• Watery • Contain a high concentration of enzymes
• Pancreatic secretion• Mucous secretions
• Thick, viscous• Mucus membranes (GI, resp)
• Composed of glycoproteins
• Mixed exocrine glands contain both mucous and serous components

Connective Tissue• Found everywhere in the body and represents most abundant tissue
by weight.• Some systems are almost exclusively composed of connective tissue
• Skeletal, integumentary• Appearance varies.
• Is derived from mesoderm, and composed of nonliving extracellular matrix- matrix surrounds and separates the cells providing important structural and nutritional support to epithelial cells. Is combination of extracellular fibers and ground substance.
• Form and function may be different.• Reserve for energy• Protection• Provides framework of structural support
• Is vascularized.• Level of vascularity varies among connective tissue type.

Connective Tissue Components• All connective tissue is composed of distinct components
• 1. Extracellular fibers• Collagenous• Reticular• Elastic
• 2. Ground substance• 3. Cells
• Fixed cells• Fibroblasts• Adipocytes (fat cells)• Reticular cells
• Wandering cells• Mast cells• Leukocytes (white blood cells)• Macrophages (fixed and wandering)

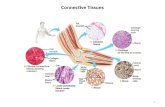
Connective Tissue Components

Connective Tissue Components: Ground Substance• An amorphous, homogenous material that
ranges from liquid to gel to solid.• Composed of glycoproteins called
glycosaminolglycans (GAGs)• Is medium through which cells exchange
nutrients and waste with the bloodstream.• Acts as shock absorbing cushion and
helps to protect underlying delicate cells.• Serves as obstacle for invading
microorganisms.


Fibers of Connective Tissue• Collagenous:
• Strong and thick.• Composed of collagen.• Organized into bundles• Found in tendons and ligaments that
are continuously being pulled and stretched.
• Sometimes called white fibers• Density and arrangement can vary.
• Loose to dense.


Fibers of Connective Tissue• Reticular:
• Composed of collagen, but are not thick• Thin and delicate and branched into
complicated networks.• Form support for around other cellular organs
like endocrine glands.• Elastic:
• Composed primarily of elastin.• Are branched to form networks• Lack tensile strength of collagenous fibers.• Can stretch and contract.• Found in vocal cords, lungs, blood vessles.• May be referred to as yellow fibers.


Major Cell Types of Connective Tissue• Fixed Cells:
• Remain in the connective tissue• Fibroblast: secrete fibers and ground substance
of particular matrix.• Can reproduce and are metabolically active.• Called based on location
• Chondroblast, osteoblast, etc.• As mature, cells are less active and are
called –cytes. Can revert back though if more matrix is needed.
• Chondrocyte, osteocyte, fibrocyte

• Fixed cells continued.• Adipose cells/Adipocytes:
• Found throughout connective tissue• Form adipose tissue.• Filled with lipid or fat.
• Reticular Cells:• Form net-like connections through
cells• Involved in immune response and
manufacture of reticular fibers.

• Transient or Wandering Cells• Move in and out of connective tissue as
needed. • Leukoctyes: white blood cells
• Found in blood and move into connective tissue during periods of infection.
• Important in immune function.• Mast cells: carry histamine and heparin which
initiate inflammatory response when released into tissue
• Usually found near blood stream where can mount response.


• Wandering cells continued..• Macrophages: phagocytotic scavengers
that may be either fixed or transient in connective tissue.
• Engulf microbes, dead cells and debris
• What digests the cell?• Given different names depending on
locatons• Kupffer cells, microglial cells,
histiocytes.


Types of Connective Tissue• Categorized as:
• Loose• Areolar• Adipose• Reticular
• Dense• Regular• Dense irregular• Elastic

Areolar Tissue• Most common type of connective tissue• Found everywhere in body• Acts to support and cushion organs and other
delicate structures.• Moderately elastic but tears easily compared to
other connective tissue.• Has “open” spaces
• Filling of spaces during trauma is called edema• Pitting edema- when tissue leaves pits in tissue
after being compressed.• Viscous ground substance


Adipose Tissue• Commonly known as fat.• Part of areolar tissue in which adipocytes dominate.• Highly vascularized• Cells expand based on amount of lipid being
stored.• Important energy store.• May be classified as:
• White:• Found throughout body
• Brown:• Found in newborns and hibernating animals• Specialized form plays role in temperature
regulation


Reticular Connective Tissue• Resembles areolar connective tissue but
only contains reticular fibers• Found in limited sites of body

Dense Regular Connective Tissue• Tightly paced, parallel collagen fibers• Tremendous tensile strength in one
direction.• Makes up tendons and ligaments

Dense Irregular Connective Tissue
• Collagen fibers in thicker bundles than those in regular connective tissue.
• Can withstand force from many different directions.• Found in dermis and fibrous coverings.• Forms tough capsule of joints.

Elastic Connective Tissue• High concentration of elastic fibers that is
extremely flexible.• Found in few regions of body.
• Stomach, large airways, bladder, etc.

Specialized Connective Tissues• Cartilage
• Hyaline Cartilage• Elastic Cartilage• Fibrocartilage
• Bone• Blood

Cartilage• Tough, specialized connective tissue.• May be called gristle. • More rigid than dense connective tissue, more
flexible than bone.• Does not contain nerves.• Can take a great deal of compression.• Composed of cells (chondrocytes) and matrix.• 3 types of cartilage:
• Hyaline cartilage• Elastic Cartilage• Fibrocartilage

Types of Cartilage• Hyaline Cartilage
• Most common type of cartilage found in body.• Found as articular cartilage at end of long
bones and joints and connects ribs to the sternum.
• Most rigid type of cartilage.• Elastic Cartilage
• Similar to hyaline cartilage but contains elastic fibers
• Can withstand repeated bending.• Found in pinnae

Types of cartilage continued• Fibrocartilage
• Found merged with hyaline cartilage and dense connective tissue.
• Found between vertebrae and spine

Bone• Also called osseous connective tissue• Hardest and most rigid type of connective
tissue• Is well vascularized• Provides protection.• Structure
• Ground matrix - osteoid – calcium phosphate and collagen fibers
• Haversian canals – channels in bone that carry blood supply and nerves
• Periosteum – fibrous membrane that covers the bone

Blood• Most atypical type of connective
tissue.• Composed of specialized cells:
• Erythrocytes (red blood cells)• Leukocytes (white blood cells)• Thrombocytes (platelets)

Membranes• Epithelial and connective tissue may be
linked to form membranes.• Are thin, protective layers that line body
cavities, separate organs and cover surfaces.
• Four common epithelial membranes are:• Mucous• Serous• Cutaneous• Synovial

Mucous Membranes• Always found lining organs that have connection to
outside environment.• Esophagus, mouth, colon, etc.
• Produces protective and lubricating mucous• Play role in monitoring and controlling what enters
into body and form barrier.• How are mucous membranes important to us?
• CRT• Are very absorptive
• Buprenex


Serous Membranes• Also called Serosa• Line walls and cover organs that fill closed body
cavities• Characterized by continous sheet that is doubled
over to form two layers with a narrow space.• Remember parietal vs. visceral?• Fluid is thin and watery (a transudate).
• Large amount of fluid is called effusion.• Fluid in abdomen is termed ascites.• Adhesions are connections between parietal
and visceral layers.



Cutaneous Membranes• The integument
• What else is this called?• Perpetually exposed to environment.• Composed of keratinized stratified
squamous epithelium called epidermis• Epidermis is attached to underlying
Dermis.

Synovial Membranes• Line the cavities of joints• Contain no epithelium• Manufacture synovial fluid that fills the joint
spaces and reduces friction and abrasion at the ends of bones.

Muscle Tissue• Uniquely designed for contraction.• Composed of myosin and actin• Three types of muscle tissue:
• Skeletal• Smooth• Cardiac


Skeletal Muscle• Large and numerous cells• Usually controlled by conscience thought
therefore is voluntary.• Are striated or striped• Held together by loose connective tissue.

Smooth Muscle• Composed of small spindle-shape cells
that lack striation or bands and appear smooth.
• Can not be consciously controlled.• Found in walls of hollow organs

Cardiac Muscle• Possesses ability to contract even when
neural input has been altered.• Exists only in the heart.• Completely involuntary.• Cells are smooth and only contain one
nucleus• Branches to form complex network.• Are striated and connected to other cells
via an intercalated disk• Contract at set rate.



Nervous Tissue• Neural tissue is designed to send and receive electrical
and chemical signals.• Found in brain, spinal cord, and peripheral nerves• Composed of two cell types
• Neurons• Longest cells in body.• Composed of three parts
• Cell body (perikaryon)• Cytoplasmic extensions (dendrites)• Long single extension (axon)
• Forms connections with many other tissues• Sensitive to electrical and chemical changes
• Neuroglial cells• Found in greater numbers than neurons• Do not transmit impulses• Are supportive to the neurons


Tissue Healing and Repair• Body’s initial response to injury is inflammation.• Repair includes organization of granulation tissue
and regeneration of lost tissue or formation of scar tissue
• Inflammation:• Area generally becomes swollen, red and hot.• Sometimes is decreased function in that part.• This isolates area to prevent further damage• Inflammation is not same as infection.

Steps in the Process of Inflammation• 1. Inflammation begins and then
vasodilation. Blood flow and oxygen and nutrient supply is increased to area.
• 2. Swelling occurs• 3. Clot formation takes place• 4. Debris is removed by phagocytic cells• 5. Histamine and Heparin help to reduce
swelling and heat.

Organization: The formation of Granulation Tissue• New tissue is formed called granulation
tissue• Composed of collagen fibers that has
been manufactured by fibroblasts.• If granulation tissue becomes too thick, will
be called proud flesh.• Granulation tissue is slowly replaced by
fibrous scar tissue• Helps to pull wound closed.• Is less flexible than normal tissue



Proud FleshProud Flesh

Classifications of Wound Healing• First intention:
• Wound edges are held closed• Usually by sutures
• Skin forms a primary union without formation of granulation tissue or significant scarring
• Second Intention:• Edges of wound separated• Granulation tissue forms to close gap; scarring
results• Third Intention:
• Contaminated wound left open until contamination is reduced and inflammation subsides; later closed by first intention; also called delayed primary closure


• http://www.youtube.com/watch?v=CjTQy6WJFOs
• http://www.youtube.com/watch?v=6wFIVnleDgk&feature=related