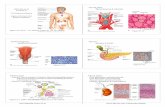
Thyroid and parathyroid glands - Julie Cornish
-
Upload
welshbarbers -
Category
Health & Medicine
-
view
437 -
download
1
Transcript of Thyroid and parathyroid glands - Julie Cornish

Thyroid and Parathyroid
Julie CornishGeneral Surgical SpR


Location of Thyroid Gland•Located just below thyroid cartilage • Isthmus is midway between apex of thyroid cartilage (“Adams apple”) and suprasternal notch



origin of the thyroid gland?
• originates from the floor of the pharynx
• outpouching which grows downward in front of trachea (Thyroglossal duct)
• bifurcates and forms a series of cellular cords which in turn form follicles and the lateral lobe
• remnants of the thyroglossal duct can be seen in the adult as cysts (mucus-filled, lined with squamous epithelium) or in the pyramidal lobe

Thyroid development


function of thyroid gland
• hormone production– Thyroxine (T4)
– Tri-iodothyronine (T3)
• produced in lumen of thyroid follicle• synthesis and release – controlled by TSH• TSH released from ant. pituitary• controlled by TRH from hypothalamus


hyperthyroidism
• incidence = 20/1000 females• 5 x less common in men• causes
– Graves disease– multinodular goitre– thyroiditis– iodide induced– TSH induced


clinical features
• goitre• D+V• weight loss• palpitations / AF / sinus tachycardia• tremor• proximal myopathy• pretibial myxoedema• eye signs – lid lag, exomphalos

classification -hypothyroidism
• Goitrous– Hashimotos thyroiditis– Drug induced (lithium, iodine)
– Iodide deficiency – Dyshormonogenesis - rare
• Post ablative• Transient (e.g. post subtotal thyroidectomy)
• Subclinical• Congenital


clinical features
• tiredness• weight gain• cold intolerance• goitre• hoarseness• depression• alopecia• myxoedema

classification - thyroid cancer
• <1% of all malignancies• Follicular cells
– Papillary carcinoma (70%) – Follicular carcinoma (10%)– Anaplastic carcinoma (undifferentiated) (5%)
• Parafollicular C cells– Medullary carcinoma (5-10%)
• Lymphocytes– Lymphoma (5-10%)

investigation
• FNA• USS +/- guided biopsy• CT• Radio-isotope imaging• Larygoscopy

Mx thyroid nodule disease
• Indications for surgery– cytological features of follicular lesion/medullary
Ca/ papillary Ca– clinical suspicion of malignancy (despite –ve bx)– pressure symptoms/ tracheal compression– thyroid toxicity– size goitre– patient preference

Mx of Graves Disease• MDT• treatment options
– anti-thyroid drugs (carbimazole)– beta blockers– radioactive iodine ablation– surgery
• indications for surgery– when other treatments failed– patient preference– pregnancy / planning pregnancy

Surgical Access
• Supine patient, neck extended• Transverse incision (2 finger breadths above clavicle)
• Deepen incision through platysma• Down to lateral border of sternomastoid• Identify anterior jugular veins• Incise along midline raphe between strap muscles• Create tissue plane between strap muscles and
thyroid



total thyroidectomy
• aim to preserve at least 1 parathyroid gland• if in doubt – remove a damaged gland, mince
it and implant pieces into sternomastoid /forearm muscle
• but not in malignant disease• following implantation – function takes 3
months to recover

Postop Mx
• Serum calcium to be checked
• Hypocalcaemia– Trousseau’s sign– Chvostek’s sign
• Mx of hypocalcaemia

complications of thyroidectomy
• recurrent laryngeal nerve damage– national incidence 5%
• Hoarseness (if > 2-3 days =external laryngeal nerve damage)
• postoperative haemorrhage• keloid scar• thyroid crisis • temporary/permanent hypoparathyroidism
– 30% transient hypocalcaemia• Tracheomalacia - rare

Parathyroid gland
• At least 4 glands in the region of the thyroid gland
• 3 cell types– adipose cells– chief cells– oxyphil cells
• Parathyroid hormone (PTH)– peptide that raises serum calcium– produced by Chief cells



Regulation of blood levels of calcium
• Thyroid C cells or parafollicular cells • lie outside follicles either in clusters, or singly • produce the peptide hormone, calcitonin • protein synthesizing organelles prominent
• Calcitonin– inhibits calcium resorption from bones– lowers blood calcium – regulated by calcium levels – high calcium will stimulate its release

Parafollicular or C cells
C Cells labeled immunocytochemically for calcitonin
Thyroid follicle
C-Cells

Parathyroid hormone functions
• stimulates osteoclasts • resorption of bone • stimulates kidney proximal tubule • reabsorption of calcium • promotes absorption of calcium from the
small intestine • raises calcium levels; regulated by calcium
itself

Regulation and feedback
Calcium levels
Calcium levels
Parathyroid hormone levels
Parathyroid hormone levels

parathyroidectomy• primary hyperparathyroidism
– PTH secreted from parathyroid adenoma (90%)– Multiple adenomata (4%)– Nodular hyperplasia (5%)– carcinoma (1%)
• clinical features:– anorexia, wt loss, N+V, constipation, weakness
• Ix: – serum Ca 2+, PTH – USS/ CT scan + radio-isotope injection to isolate gland