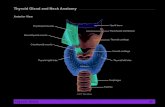
THYROID GLAND SURGERY. THYROID GLAND ANATOMY Detailed Thyroid Anatomy.
THE THYROID GLAND
description
Transcript of THE THYROID GLAND

THE THYROID THE THYROID GLANDGLAND
HYPOTHYROIDISMHYPOTHYROIDISM

MEASUREMENT OF THYROID HORMONESMEASUREMENT OF THYROID HORMONES
DIRECT METHODSDIRECT METHODS Circulating levels of total Circulating levels of total
hormoneshormones total thyroxine (TTtotal thyroxine (TT44))
total triiodothyronine (TTtotal triiodothyronine (TT33)) protein bound iodine (PBI)protein bound iodine (PBI)
Circulating levels of free Circulating levels of free hormoneshormones
free thyroxine (fTfree thyroxine (fT44))
free triiodothyronine (fTfree triiodothyronine (fT33))
Thyroid hormone binding Thyroid hormone binding proteinsproteins
Thyroxine binding globulin (TBG)Thyroxine binding globulin (TBG)
INDIRECT METHODSINDIRECT METHODS Thyroid hormone binding Thyroid hormone binding
teststests resin uptake of resin uptake of 125125I-TI-T33
Free thyroxine index (FTI)Free thyroxine index (FTI)
FTI=FTI=TT4 4 x patient x patient 125125I-TI-T3 3 resin uptakeresin uptake
Control Control 125125I-TI-T33 resin uptake resin uptake

OTHER TESTS OF THYROID FUNCTIONOTHER TESTS OF THYROID FUNCTION
Dynamic tests of thyroid Dynamic tests of thyroid
activityactivity Thyroid uptake of Thyroid uptake of 123123I or I or 131131I I
(and scan)(and scan)
Thyroid uptake of Thyroid uptake of 9999mTcmTc T3 suppression testT3 suppression test
TSH stmulationTSH stmulation test test
Tests of the thyroid-Tests of the thyroid-
pituitary axispituitary axis Basal serum TSHBasal serum TSH
Serum TSH response to Serum TSH response to
exogenous TRHexogenous TRH
impaired response - hyperthyroid
exaggerated response - hypothyroid
normal response - euthyroid

HYPOTHYROIDISMHYPOTHYROIDISM
Hypothyroidism is a disease caused by a Hypothyroidism is a disease caused by a
level of thyroid hormone insufficient for level of thyroid hormone insufficient for
normal body function.normal body function.
It affects every cell of human body.It affects every cell of human body.
An enlarged thyroid gland is the An enlarged thyroid gland is the
abnormality present in most cases.abnormality present in most cases.

HYPOTHYROIDISMHYPOTHYROIDISM
Causes of hypothyroidismCauses of hypothyroidism
PRIMARYPRIMARY
/thyroid gland//thyroid gland/
SECONDARYSECONDARY
/pituitary//pituitary/
TERTIARYTERTIARY
/hypothalamus//hypothalamus/

Primary hypothyroidismPrimary hypothyroidism
CONGENITALCONGENITAL AthyreosisAthyreosis
Ectopic thyroidEctopic thyroid DyshormonogenesisDyshormonogenesis
Iodide deficiencyIodide deficiency Antithyroid immunity Antithyroid immunity
(transient due to illness)(transient due to illness)
ACQUIREDACQUIRED Iodine deficiencyIodine deficiency
AutoimmunityAutoimmunity Post-radioactive iodine Post-radioactive iodine
therapytherapy Post-thyroidectomyPost-thyroidectomy Antithyroid drugs Antithyroid drugs
(e.g. Carbimazole)(e.g. Carbimazole) Iodine excessIodine excess
Subacute thyroiditisSubacute thyroiditis Thyroid irradiationThyroid irradiation

Secondary hypothyroidismSecondary hypothyroidism pituitary tumourspituitary tumours
pituitary granulomas (e.g. sarcoid) or injurypituitary granulomas (e.g. sarcoid) or injury „„empty sella” syndromeempty sella” syndrome
Tertiary hypothyroidismTertiary hypothyroidism hypothalamic disorders (e.g. craniopharyngioma)hypothalamic disorders (e.g. craniopharyngioma)
Isolated TRH deficiencyIsolated TRH deficiency

CAUSES OF HYPOTHYROIDISMCAUSES OF HYPOTHYROIDISM
Iodine deficiency is the most common Iodine deficiency is the most common cause of goitre and bordeline cause of goitre and bordeline hypothyroidism worldwide.hypothyroidism worldwide.
In noniodine-deficient areas In noniodine-deficient areas autoimmunity is the common cause of autoimmunity is the common cause of
hypothyroidismhypothyroidism

EFFECTS OF IODINEEFFECTS OF IODINE
Goitre, rarely hypothyroidismGoitre, rarely hypothyroidismDEFICIENCYDEFICIENCY
Temporary inhibition Temporary inhibition of thyroid hormone synthesisof thyroid hormone synthesis
(Wolff-Chaikoff effect)(Wolff-Chaikoff effect)Induction of thyrotoxicosisInduction of thyrotoxicosis
(Jod-Basedow phenomenon)(Jod-Basedow phenomenon)
EXCESS,EXCESS,ACUTEACUTE
Goitre, hypothyroidismGoitre, hypothyroidismEXCESS,EXCESS,CHRONICCHRONIC

IODINE DEFICIENCYIODINE DEFICIENCY
REDUCTION OF DIETARY IODINE INTAKEREDUCTION OF DIETARY IODINE INTAKE
thyroid hormone production thyroid hormone production
(preferential secretion of T(preferential secretion of T33 rather than T rather than T44))
compensatory compensatory TSH secretion TSH secretion

IODINE DEFICIENCYIODINE DEFICIENCY
MODERATE MODERATE Urinary iodide Urinary iodide
excretion:excretion:25 -5025 -50μμ/g creatinine/g creatinine
Prevalence of Prevalence of goitre:goitre:
20 -50%20 -50%
Hypothyroidism:Hypothyroidism:rarelyrarely
SEVERESEVERE Urinary iodide Urinary iodide
excretion:excretion:
<25<25μμ/g creatinine/g creatinine
Prevalence of Prevalence of goitre:goitre:>50%>50%
Hypothyroidism:Hypothyroidism:frequentlyfrequently

EXCESS OF IODINEEXCESS OF IODINE
Acute increase in intracellular iodine Acute increase in intracellular iodine concentrationsconcentrations
Temporal inhibition of thyroid hormone Temporal inhibition of thyroid hormone
synthesis and release synthesis and release (Wolff-Chaikoff effect)(Wolff-Chaikoff effect)
Decrease in intracellular iodine concentrationDecrease in intracellular iodine concentration
(escape from Wolff-Chaikoff effect)(escape from Wolff-Chaikoff effect)

EXCESS OF IODINEEXCESS OF IODINE
Introduction of iodine therapy in areas of Introduction of iodine therapy in areas of iodine deficiencyiodine deficiency
Increase in the frequency of Increase in the frequency of
thyrotoxicosisthyrotoxicosis(Jod-Basedow phenomenon)(Jod-Basedow phenomenon)
unmasking thyroid autonomy unmasking thyroid autonomy (previously protected by iodine deficiency)(previously protected by iodine deficiency)

EXCESS OF IODINEEXCESS OF IODINEProlonged iodine ingestion in patients with Prolonged iodine ingestion in patients with
autoimmune thyroiditis autoimmune thyroiditis (Hashimoto’s (Hashimoto’s disease)disease) and in fetal and neonatal period and in fetal and neonatal period
(maternal ingestion of excess iodine)(maternal ingestion of excess iodine)
Permanent hypothyroidism Permanent hypothyroidism
and goitre formationand goitre formation
No excape from Wolff-Chaikoff effectNo excape from Wolff-Chaikoff effect

CLINICAL PICTURE OF CLINICAL PICTURE OF
HYPOTHYROIDISM DEPENDS ON TIME HYPOTHYROIDISM DEPENDS ON TIME
OF THE ONSET OF DISEASEOF THE ONSET OF DISEASE

CONGENITAL HYPOTHYROIDISMCONGENITAL HYPOTHYROIDISM
The prevalence:The prevalence:
1 : ~4,000 live births1 : ~4,000 live births Usually no signs at birthUsually no signs at birth
Untreated congenital hypothyroidismUntreated congenital hypothyroidism
Non-reversible retardation of physical Non-reversible retardation of physical
and mental developmentand mental development

Clinical features of congenital Clinical features of congenital hypothyroidismhypothyroidism
Typical faceTypical face MacroglossiaMacroglossia
Enlarged posterior Enlarged posterior fontanelle (>0.5 cm) fontanelle (>0.5 cm) NN
HypotoniaHypotonia HypoactivityHypoactivity Mottled skinMottled skin
Cold extremitiesCold extremities Dry skinDry skin
Umbilical hernia (>0.5cm) Umbilical hernia (>0.5cm) NN
Delayed passage of Delayed passage of meconium meconium NN
ConstipationConstipation Feeding problemsFeeding problems Prolonged icterus Prolonged icterus NN Hoarse, grunting cryHoarse, grunting cry
GoiterGoiter Placidity, lethargyPlacidity, lethargy
Growth retardation and Growth retardation and immature body proportionsimmature body proportions Mental retardationMental retardation
N – symptoms only observed in the neonatal periodN – symptoms only observed in the neonatal period
All signs are facultative and frequently are not seen in All signs are facultative and frequently are not seen in the neonatal phase.the neonatal phase.

CONGENITAL HYPOTHYROIDISMCONGENITAL HYPOTHYROIDISM
May be detected biochemically by screening May be detected biochemically by screening all neonates 3 – 5 days after birth.all neonates 3 – 5 days after birth.
T4 screening TSH screening
False positive
False negative
PrematurityPrematurity
Low TBGLow TBG
Laboratory errorLaboratory errorLaboratory errorLaboratory error
Ectopic thyroidEctopic thyroid
Laboratory errorLaboratory error
HypopituitarismHypopituitarism
Laboratory errorLaboratory error

ACQUIRED HYPOTHYROIDISMACQUIRED HYPOTHYROIDISM
In noniodine-deficient areasIn noniodine-deficient areas
primary hypothyroidism primary hypothyroidism
women : men = 10 : 1women : men = 10 : 1
The prevalence in women of all ages:The prevalence in women of all ages:
2 - 4%2 - 4%
(one-third of this cases (one-third of this cases iatrogenic hypothyroidism) iatrogenic hypothyroidism)

ACQUIRED HYPOTHYROIDISMACQUIRED HYPOTHYROIDISM
CLINICAL FEATURES IN HYPOTHYROIDISMCLINICAL FEATURES IN HYPOTHYROIDISM
The symptoms of hypothyroidism are The symptoms of hypothyroidism are
nonspecific and may be attributed by both nonspecific and may be attributed by both
patient and doctor to ageing, the onset patient and doctor to ageing, the onset
usually being insidious.usually being insidious.

Symptoms of hypothyroidismSymptoms of hypothyroidismUSUALUSUAL
LethargyLethargy Increased sleepIncreased sleep
ConstipationConstipation Mild weight gain Mild weight gain Cold intoleranceCold intolerance Facial puffinessFacial puffiness
Dry skinDry skin Hair lossHair loss
HoarsensessHoarsensess Abnormal mensesAbnormal menses AcroparaesthesiaeAcroparaesthesiae
Snoring Snoring
RARERARE
DeafnessDeafness
PsychosisPsychosis
Cerebellar disturbanceCerebellar disturbance
MyotoniaMyotonia

SIGNS OF HYPOTHYROIDISMSIGNS OF HYPOTHYROIDISM
Change in appearance Change in appearance (e.g. face puffy and (e.g. face puffy and
pale)pale) Periorbital oedemaPeriorbital oedema
Dry, flaking, cool, pasty Dry, flaking, cool, pasty skinskin
Diffuse hair lossDiffuse hair loss BradycardiaBradycardia
Signs of median nerve Signs of median nerve compressioncompression
(carpal tunnel syndrome)(carpal tunnel syndrome)
Effusions in body Effusions in body
cavities cavities
(e.g. ascites, pericardial (e.g. ascites, pericardial
effusion)effusion)
Delayed relaxation of Delayed relaxation of
reflexesreflexes
Croaky voiceCroaky voice
GoitreGoitre
Rarely stupor or comaRarely stupor or coma

MYXOEDEMAMYXOEDEMAMyxoedema is a severe form of hypothyroidism Myxoedema is a severe form of hypothyroidism
causing complete exhaustion of all bodily causing complete exhaustion of all bodily functions.functions.
All the organs are infiltrated with All the organs are infiltrated with mucopolysaccharides that interfere with mucopolysaccharides that interfere with
proper cell metabolism.proper cell metabolism.Myxoedema patients have all the symptoms and Myxoedema patients have all the symptoms and
signs described for hypothyroidism, as well as signs described for hypothyroidism, as well as low brain center reserve, low cardiac reserve, low brain center reserve, low cardiac reserve, low respiratory reserve, low adrenal reserve, low respiratory reserve, low adrenal reserve,
and low thermoregulatory reserve. In addition, and low thermoregulatory reserve. In addition, they may show hyponatremia, hypercapnia, they may show hyponatremia, hypercapnia,
hypoxia, and anemia.hypoxia, and anemia.

HYPOTHYROIDISM- HYPOTHYROIDISM- DIAGNOSTIC PROCEDURESDIAGNOSTIC PROCEDURES
TSH levelTSH level
(second or third generation assays = the lower (second or third generation assays = the lower detection limit: 0.05-0.005 -0.002 mU/l)detection limit: 0.05-0.005 -0.002 mU/l)
FTFT44 level level
(the measurement of T(the measurement of T33 is not a good is not a good
diagnostic test for hypothyroidism)diagnostic test for hypothyroidism) TSH response to exogenous TRHTSH response to exogenous TRH
(secondary and tertiary hypothyroidism; (secondary and tertiary hypothyroidism; subclinical hypothyroidism)subclinical hypothyroidism)

Hypothyroidism- summary of Hypothyroidism- summary of diagnostic testsdiagnostic tests
PrimaryPrimary
HypothyroidismHypothyroidism
Secondary Secondary
HypothyroidismHypothyroidism
Tertiary Tertiary
HypothyroidismHypothyroidism
Non-thyroid Non-thyroid
illnessillness
Basal Basal
TSHTSH
raisedraised
low or normallow or normal
low, normallow, normal
or elevatedor elevated
normal or lownormal or low
TT44
lowlow
lowlow
lowlow
lowlow
TRHTRHresponseresponse
exaggeratedexaggerated
reducedreducedor absentor absent
sluggish sluggish or delayedor delayed
normal or lownormal or low

Subclinical hypothyroidismSubclinical hypothyroidism(diminished thyroid reserve)(diminished thyroid reserve)
Serum TSerum T44 : normal (lower half of the normal range) : normal (lower half of the normal range)
Serum TSerum T33: normal or sometimes even slightly elevated: normal or sometimes even slightly elevated
Basal TSHBasal TSH: slightly raised : slightly raised
TSH/TRHTSH/TRH: exaggerated: exaggerated
Definition: „subclinical” Definition: „subclinical” no symptoms and signs (?) no symptoms and signs (?)
Patients with subclinical hypothyroidism are at Patients with subclinical hypothyroidism are at increased risk for coronary heart diseaseincreased risk for coronary heart disease
HOWEVERHOWEVER

IMAGING STUDIESIMAGING STUDIES
Rapidly growing large goiter; Rapidly growing large goiter; Goiter with a dominant nodule;Goiter with a dominant nodule;
Hashimoto’s diseaseHashimoto’s disease
ultrasonography examination and fine ultrasonography examination and fine
needle aspiration biopsyneedle aspiration biopsy

IMAGING STUDIESIMAGING STUDIES
Cardiac function shoud be assessed Cardiac function shoud be assessed
before treatment is started.before treatment is started.
The presence of other associated The presence of other associated
autoimmune endocrinopathies must be autoimmune endocrinopathies must be
ascertained.ascertained.

HYPOTHYROIDISM –HYPOTHYROIDISM –TREATMENTTREATMENT
Hypothyroidismis treated with replacement Hypothyroidismis treated with replacement TT44 therapy therapy (sodium L-thyroxine)(sodium L-thyroxine)
Replacement doses usually start at 50 Replacement doses usually start at 50 μμg/d g/d being increased in a stepwise fashion at being increased in a stepwise fashion at monthly intervals to 100 - 150 monthly intervals to 100 - 150 μμg/d as the g/d as the
response is assessed clinically and response is assessed clinically and biochemically.biochemically.

HYPOTHYROIDISM –HYPOTHYROIDISM –TREATMENTTREATMENT
There is considerable variation in patient There is considerable variation in patient
response to Tresponse to T44 because of differential thyroid because of differential thyroid
hormone receptor isoform tissue hormone receptor isoform tissue
concentration.concentration.

HYPOTHYROIDISM –HYPOTHYROIDISM –TREATMENTTREATMENT
During TDuring T44 therapy: therapy:
Serum TSerum T33 concentration must be in the concentration must be in the
normal range, as should that of TSHnormal range, as should that of TSH
Serum TSerum T44 may exceed the upper limit of may exceed the upper limit of
normal.normal.

HYPOTHYROIDISM –HYPOTHYROIDISM –TREATMENTTREATMENT
During TDuring T44 therapy: therapy:
Clinically satisfactory response:Clinically satisfactory response:
normal pulse rate normal pulse rate
and complete resolution of presenting symptoms and complete resolution of presenting symptoms
and signs.and signs.
Occasionally cardiac symptoms such as palpitations Occasionally cardiac symptoms such as palpitations
may occur; in this case a may occur; in this case a ββ-adrenergic blocker drug -adrenergic blocker drug
is indicatedis indicated..

HYPOTHYROIDISM –HYPOTHYROIDISM –TREATMENTTREATMENT
In patients with ischemic heart disease:In patients with ischemic heart disease:
Replacement therapy should be introduced Replacement therapy should be introduced
cautiously, with started doses of 25cautiously, with started doses of 25μμg/d; g/d;
increments should also be smallincrements should also be small..

Protocol for the management of Protocol for the management of myxoedema comamyxoedema coma
Take blood for diagnostic tests: TTake blood for diagnostic tests: T44, ,
TSH and plasma cortisolTSH and plasma cortisol
Give 300 Give 300 μμg Tg T44 i.v. and repeat i.v. and repeat
approximately 100 approximately 100 μμg q.d; give via g q.d; give via
nasogastric tube if i.v. preparation nasogastric tube if i.v. preparation
is unaviableis unaviable
Treat hypothermia with gradual Treat hypothermia with gradual
rewarming using blanketsrewarming using blankets
Give i.m. hydrocortisone 75 mg Give i.m. hydrocortisone 75 mg
immediately and repeat 25-50 mg 8-immediately and repeat 25-50 mg 8-
hourlyhourly
Give TGive T33 20 20 μμg i.v., i.m. or by g i.v., i.m. or by
nasogastric tube 12-hourly, if nasogastric tube 12-hourly, if
possible possible
Treat any heart failure with Treat any heart failure with
diureticsdiuretics
Correct any electrolyte Correct any electrolyte
disturbancesdisturbances
Carefully exclude or treat Carefully exclude or treat
infectioninfection
Use sedative drugs and fluids Use sedative drugs and fluids
sparingly sparingly
Measure serum TMeasure serum T44, T, T33 and TSH and TSH
frequentlyfrequently