The Changing Face of Addiction Health Care Moving Forward
description
Transcript of The Changing Face of Addiction Health Care Moving Forward

The Changing Face ofAddiction Health Care
Moving ForwardArthur Schut
Arapahoe House, IncColorado
Texas Initiative for Program Success and Sustainability Leadership Summit
Association of Substance Abuse ProgramsAustin, Texas
January 10, 2011

How to Avoid Being a Dinosaur:
Thoughts related to preventing the potential extinction of stand-alone substance-use
illness treatment providers in the course of health reform
OR

Brief overview of “Where are we going?”
Thoughts on being strategic with the goal of survival – avoid being a dinosaur
Practical operational issuesYou leave with one approach or idea that has practical value
Goals of breakout

There will be some type of universal health coverage and payment mechanism.
There will be a health care delivery system
that functions in an integrated manner (even if there is no universal health coverage).
Primary care providers will be the “hub” of
the health care delivery system that is integrated.
Moving Forward

We will have to provide an integrated continuum of substance-use illness care that at the minimum: includes essential levels of care; addresses co-occurring conditions; includes an emphasis upon recovery management; and engages meaningfully with primary care and health homes.
Moving Forward

Prevention will be viewed as essential to health system outcomes.
We will be part of, or intimately connected to, the mainstream health care delivery system or cease to exist.
Moving Forward

We must connect clients to health systems.
We must connect our services to health systems.
We need to be aware of quality and performance measures (e.g., NQF, IOM).
It is time for us as a field to do a self-critical
inventory, and make major changes.
Moving Forward

Significant changes include…
Moving back into the medical system
The majority of substance-use illness services will be provided through primary care settings (as is currently true for depression and anxiety disorders)
Some of us will be the substance-use illness specialty providers for the transformed system
Moving Forward

….the trends we see as having a transformative effect on addiction services … are among the subjects that are informing treatment or challenging treatment orthodoxy.
Trends that are transforming the fieldNew information is altering many old assumptions about treatment by Gary A. Enos, Editor and David Raths, {Addiction Professional - Used and edited with permission}

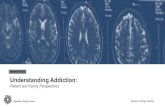
The images … healthy and drug-affected brains … bring the promise of more effective treatments to be generated from the various discoveries in the lab.
What areas of the brain are associated with craving?
Science fiction may be close to fact

“As health care reform moves forward, it will require a proactive approach that includes early detection, screening and interventions”
“Physicians have a key role to play in this effort.”
[Larry M. Gentilello, MD, professor of surgery at the University of Texas Southwestern Medical Center, Dallas]
Physicians become a significant influence

Automation is “among the most important strategic decisions organizations such as ours have to make.” [David T. Smith, New Beginnings in Waverly, Minnesota and St. Cloud State University]
… addiction treatment facilities … continue to lag behind both mental health and general health facilities in technology adoption
Wider implementation of electronic health records

“There's absolutely no question that providers who aren't able to address multi-service needs are not going to be in service much longer”
[Linda Grove-Paul, MSW, Centerstone of Indiana]
Competencies in multiple services

Both the stand-alone addiction treatment organization and the mental health only agency appear to be moving toward extinction.
Competencies in multiple services

…. people in treatment for alcohol and drug addiction have better outcomes if they quit tobacco use….
Some studies show that more than 50 percent of the deaths in substance abuse treatment populations result from tobacco-related disease.
State governments commit funding and pass legislation regarding smoking cessation in addiction treatment facilities
Tobacco becoming an enemy of recovery

Patients use a smart phone system with an opt-in GPS tracking feature which monitors their movements and triggers a peer call when they go near high risk situations (marked liquor stores, for example).
University of Wisconsin (with support from NIAAA) has launched the Innovations for Recovery Model (http://www.innovationforrecovery.com)
Taking treatment services online

The days when addiction treatment programs would ignore clients' other health habits as long as they weren't drinking or using seem to be numbered. Treatment centers are experiencing a nutrition and fitness boom…
Emphasizing diet and exercise

“Since no one behavioral approach has better overall outcomes than others, clients should have a choice of available, effective treatments,” [Mark L. Willenbring, Director, Treatment and Recovery Research Division NIAAA]
Embracing blended treatment approaches

National Quality Forum (NQF)National Voluntary Consensus Standards
Institute of Medicine (IOM) of the National Academies
Crossing the Quality Chasm The Six Aims of High-Quality Health Care
The Quality of Care We Must Provide

NQF
National Voluntary Consensus Standards for the Treatment of Substance Use Conditions: Evidence-Based Treatment Practices (2007)
“… performance measures for the treatment of substance use conditions.”

NQF Standards Impact
“… conducted according to the NQF Consensus Development Process, … the 11 endorsed practices and their specifications have legal status as national voluntary consensus standards for the treatment of substance use conditions.”

Safe - avoiding injuries to patients from the care that is intended to help them.
Effective - providing services based on scientific knowledge to all who could benefit and refraining from providing services to those not likely to benefit (avoiding underuse and overuse, respectively).
The Six Aims of High-Quality Health Care (IOM)

Patient-centered - providing care that is respectful of and responsive to individual patient preferences, needs, and values and ensuring that patient values guide all clinical decisions.
Timely - reducing waits and sometimes harmful delays for both those who receive and those who give care.
The Six Aims of High-Quality Health Care (IOM)

Efficient - avoiding waste, including waste of equipment, supplies, ideas, and energy.
Equitable - providing care that does not vary in quality because of personal characteristics such as gender, ethnicity, geographic location, and socioeconomic status.
SOURCE: IOM, 2001:5–6. [Italics added]
The Six Aims of High-Quality Health Care (IOM)

For many clients there are “consequences” for not cooperating with treatment
Clients now may be pushed to one provider (or group of providers) because it is the only source of services with financial assistance. This will change.
Do we have as the foundation of our service delivery model an implicit assumption that most clients have to come to us?
Challenges

What happens when everyone has the ability to pay with universal coverage?
There will be more options for services.
Challenges

In the new delivery system we will need to be engaging in a different way to assist clients to voluntarily manage their own care
Evidence-Based Practices (EBP) need to be implemented with reportable fidelity measurement
Brief interventions and case management alone are treatment
Challenges

Enhance Handoffs to and from “the health system/primary care”
Organize services around episodes and a full continuum of care, rather than discrete levels of care or locations
Increase skill diversity of professional staff to address major co-occurring conditions
Challenges

Our tradition of consumer involvement – persons in recovery – gives us the illusion we know what it is like to be a customer.
Need high quality customer service – NIATx process improvement techniques are a very effective tool.
“Be a customer”.
Improve Customer Service

Apply for services at your own organization.
Be admitted.
Ask a customer.
Become active in NIATx.
Improve Customer Service

Evidence-based “Practices” as well as “Programs”
Incomplete adoption and too little fidelity
TIPS, TAPS
National Quality Forum (NQF)
IOM Crossing the Quality Chasm
Evidence-Based Practices and Programs

NREPP – National Registry of Evidence-based Programs and Practices
Medication assisted treatment
Training to, and tracking fidelity of, implementation of EBPs
Without FIDELITY there is no evidence-based practice
Need executive leadership support for implementation with fidelity measures
Evidence-Based Practices and Programs

Experience vs. education - No longer a “real” separate choice
Need and can find both experience and education in one
Payers will not pay for experience absent education
Human ResourcesQualified professional clinical staff

Need significant numbers of staff dual-credentialed at a level, and in a way, that is acceptable as a health professional
Clinical master’s degree prepared
Licensure both as mental health professional and upper level certified addictions counselor
Human ResourcesQualified professional clinical staff

A high school diploma and certification as an addictions counselor will not be acceptable as a primary provider nor as a clinical supervisor of services for substance use illness treatment.
Bachelor’s or Master’s degree minimum for primary service delivery
Human ResourcesQualified professional clinical staff

Recovery coachRecovery mentorAddictions tech (psychiatric tech)Detox technicianOutreach workerOther?
Meaningful roles for those existing staff without at least a BA/BS

Hire clinical staff with at least a BA.
Inventory existing clinical staff: degree(s); college or university (accredited? really?); program of study/major; eligible for licensure/certification? (substance-use illness; mental health); supervision requirements (what kind, by whom, in what amounts, for what duration).
Action from this point forward:

support non-degreed staff to become degreed
support BA level staff to obtain MA, MSW, etc.
support existing MA level staff to become licensed MH professionals
train substance-use illness staff to mental health competence
train mental health staff to substance-use illness competence
Train all professional staff to work with primary care
Develop concrete plan with support to assist staff to upgrade:

flex time for external classes
tuition assistance ($$)
clinical supervision for licensure and/or certification (internal or hired consultants) ($)
multiply supervision over time as develop own licensed/certified professionals
salary differentials for licensure and certification ($)
Develop concrete plan with support to assist staff to upgrade:

Credential with third party payersorganization with payers when
possibleindividual clinicians as necessary
Engage clinical staff in pre-
authorizations, continuing stay reviews, billing documentation – they usually produce what is billed or reported.
Finance

Analyze business processes particularly as they relate to services delivered which could be billed or are currently billed.
Coding services delivered – need to be correct to result in payment
Claims-based billing systems
Finance

Electronic tie from services recording to billing [There are advantages to services being recorded in a way that is sufficiently disaggregated that most billing options are open].
Bundling and unbundling services at the billing end of the process.
Electronic claims processing
Finance

Appeal claim denials
Advocate for single case agreements
Contracting vs care management
Appeal claim denials
Finance

IT is part of the essential foundation for service delivery.
Sophisticated does not have to be complicated.
Develop business processes anticipating Electronic Health Record (EHR).
Ability to export to other systems is important.
Information Technology

Ability of other systems to import information from you is important
Single entry data (efficient & reduces errors)
Customer friendly information collection (unduplicated is efficient)
Information Technology

Effective, timely information sharing between clinicians, systems of care, and different provider organizations.
Thoroughly inventory both internal and external electronic communication.
Information Technology

State and payer reporting requirements should be an output, not the design structure.
Challenges in conceptualizing data reporting in a way that facilitates an “episode of care”, rather than discrete admissions and discharges (“opens and closes”?)
Providers should not allow data reporting to structure clinical services (also see regulation).
Information Technology

Initiate business practices that begin to approach electronic communication
Closed internal email system
Scan and email (closed system)
Scan and fax
Photocopy and send with the patient
e-Communication without a lot of "e"

Integrated with physical location services
Target is to ultimately provide patient electronic access integrated with all clinical services
Secure login where clients can complete initial information
e-Treatment

Smart phone, text messages, access to part of client’s clinical record, etc.
The substance-use illness field could be a leader in the development of e-solutions.
e-Treatment

Most providers have multiple audits by multiple funders and regulators – at times with conflicting requirements.
High degree of variability in regulation.
Historically some regulation assumes provider is a paraprofessional requiring significant oversight of a “clinical supervisor” (mental health professional).
Regulation

Will regulation and documentation requirements change as the delivery system changes?
Required documentation often drives the structure of the delivery system.
Regulation

Requirements to collect way too much information “up front” – how difficult can we make initial engagement and entry into treatment?
Regulation by convenience for external record audit – regulatory or payer audit staff suggestions regarding how to make audits easier for them.
Regulation

How much of what we think is “regulation” is provider self-inflicted?
Providers should not allow regulation and auditing to structure clinical services (also see IT).
Providers should partner with states to modify regulation – including self-inflicted regulation.
Regulation

e.g., client must be “discharged” after 30 (or 45 or 60 or 90) days of no face-to-face contact.
Letter to client “if we don’t hear from you by xx/xx/xxxx we are going to discharge you.” “Failure to xyz will result in your discharge ….”
How many letters like this have you received from your health care provider?
Do not confuse payer requirements with how you think of clients’
relationships with you as a provider.

Evaluation of business processesOrganizing data around business
management requirements, rather than external reporting requirements [still need to accommodate external reporting]
Performance measurement – process and outcome
Reliable accurate data (internal)
Metrics

Reliable accurate data is more important than a lot of data.
Reliable external data is a challenge at the minimum.
Benchmarking – where is the thermometer by which we compare our organization’s performance – what is normal?
Metrics

Fidelity – do we do what we say we do? Need for formal mechanisms to measure
Results driven service delivery – what does the customer want as deliverables?
Who are the customers? Pay for health outcomes!
Metrics

Join NIATx process improvement - “mini metrics”
Join a benchmarking initiative –Benchmarking for Organizational Excellence in Addiction Treatment initiative, sponsored by SAAS, NIATx and Behavioral Pathway Systems
Using data to make decisions – actually using data.
Metrics

We are experts at dealing with difficult to reach patients
We are experts at engaging patients that are seen as disruptive in other systems
We are experts at de-escalation
We have affection for people who are addicted, even when they are not at their best
Strengths = New and Diverse Opportunities

We know how to manage a complex illness over a lifetime. We know recovery.
We understand what’s going on with the family in relation to the illness.
We understand how a range of external systems impact and can support a patient and family e.g., child welfare, employment, law enforcement, corrections, etc
Strengths = New and Diverse Opportunities

Who are our health system customers?
Where can we add value in the places we “touch”
What do we do that creates value for primary care and health systems?
Is there a thorn in the paw that we can remove?
Strengths = New and Diverse Opportunities

Inventory - What we SAY we do well
Inventory – What DO we do well (outside view needed?)
Inventory - Where do we currently “touch” health services? Just “touch” anywhere - primary care, health systems, clinics.
Strengths = New and Diverse Opportunities

“Fast Forward” – skip ahead to primary care integration
Connecting our clients to primary care
How many SUD specialty providers know (or ask) if client has a primary care provider?
Improved Partnership with Primary Care

How many SUD specialty providers contact clients’ existing primary care providers at admission?
At discharge?
How many arrange for a primary care “home” before discharge?
Improved Partnership with Primary Care

Provide consultation to primary care health professionals (need immediate access)
Increase qualifications of professional staff to dual credentialed, professionally licensed
Brief patient consult - 15 to 20 minutes sessions
Improved Partnership with Primary Care

Intervening to help patients participate in the management of their illness to shorten hospital stays
Partner around shared challenges – healthy babies, outreach, over-utilization, disruptive behavior, prescription medication addiction (pain management challenges), illness management
Partnership Opportunities

Networks with other substance-use illness providers, mental health and behavioral health providers – create a continuum of care
Joint efforts/ventures
Behavioral health managed care entities, managed service organizations, private payers
Partnership Opportunities

Co-locate/integrate in primary care clinics
Co-locate/integrate in emergency departments
Co-located/integrated services need to be seamless to the client
Partnership Opportunities

Emergency departments (EDs) and intoxicated patients
Reducing over-utilization of services
Managing chronic illnesses
Partnership Opportunities

Community health clinics,
OB/GYN clinics
EAPs
HMOs/MCOs/Integrated MCOs e.g., Kaiser Permanente
Partnership Opportunities

Can all this be done in the next few years?
Start with “low hanging fruit” – trite but true
Business process
Where to start

Clinical efficiency
IT support
Inventory & enhance clinical staff
Where to start

We must connect clients to health systems.
We must connect our services to health systems.
We need to be aware of quality and performance measures (e.g., NQF, IOM)
Where to start

One change at a time – avoid contingent linking.
Measure change (quick, brief, & targeted).
Adjust – Move Forward.
Where to start

Benchmarking SAAS, NIATx, and Behavioral Pathway Systems are
partnering to sponsor an addiction-specific national benchmarking initiative: Benchmarking for Organizational Excellence in Addiction Treatment
A thermometer would not be a very helpful measure of your health if you didn’t know that 98.6° were normal. Similarly, in the absence of a relevant context, your organization’s measures of performance are of limited value. The Addiction Benchmarking Initiative provides that vital context as well as a vehicle for ongoing organizational improvement.
RESOURCES

BenchmarkingBenchmarking for Organizational Excellence in Addiction
TreatmentBehavioral Pathway Systems
877-330-9870 (Toll-Free)[email protected]
If at least 10 agencies from your state participate, your reports will also include state-wide norms in addition to national norms.
RESOURCES

Moving Forward: Preparing for the Future of Addiction Services
Implementing Healthcare Reform: First Steps to Transforming Your Organization, A Practical Guide for Leaders
http://www.saasnet.org/PDF/Implementing_Healthcare_Reform-First_Steps.pdf

NIATx – Network for the Improvement of Addiction Treatment
www.NIATx.org
NREPP – National Registry of Evidence-based Programs and Practices
http://www.nrepp.samhsa.gov/
CSAT Inventory of Effective Substance Abuse Treatment Practices
http://csat.samhsa.gov/treatment.aspx
Dennis McCarthy The Realities of Evidence-Based Practices for Addiction Treatment
http://www.attcnetwork.org/find/news/attcnews/epubs/v1i2_article04.asp

National Quality Forum
http://www.qualityforum.org/National Quality Forum (2007). National Voluntary
Consensus Standards for the Treatment of Substance Use Conditions: Evidence-Based Treatment Practices. Washington, DC: National Quality Forum.
http://www.qualityforum.org/Publications/2007/09/National_Voluntary_Consensus_Standards_for_the_Treatment_of_Substance_Use_Conditions__Evidence-Based_Treatment_Practices.aspx http://www.qualityforum.org/Publications/2005/10/Evidence-Based_Treatment_Practices_for_Substance_Use_Disorders.aspx

Institute of Medicine of the National AcademiesImproving the Quality of Health Care for Mental and
Substance-Use Conditions: Quality Chasm Serieshttp://www.iom.eduInstitute of Medicine (2001). Crossing the Quality Chasm:
A New Health System for the 21st Century. Washington, DC: National Academy Press.
Institute of Medicine (2006). Improving the Quality of Health Care for Mental and Substance-Use Disorders: Quality Chasm Series. Washington, DC: National Academy Press.
http://www.iom.edu/Reports/2005/Improving-the-Quality-of-Health-Care-for-Mental-and-Substance-Use-Conditions-Quality-Chasm-Series.aspx

Bridging the Gap Between Practice and Researchhttp://www.iom.eduInstitute of Medicine (1998). Bridging the Gap Between
Practice and Research: Forging Partnerships with Community-Based Drug and Alcohol Treatment. Washington, DC: National
http://www.iom.edu/Reports/2003/Bridging-the-Gap-Between-Practice-and-Research-Forging-Partnerships-with-Community-Based-Drug-and-Alcohol-Treatment.aspx