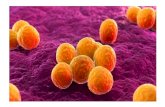
Susceptibility of MRSA biofilms to denture-cleansing agents
Transcript of Susceptibility of MRSA biofilms to denture-cleansing agents

R E S E A R C H L E T T E R
SusceptibilityofMRSAbio¢lms todenture-cleansingagentsDiana Lee1, Julie Howlett1, Jonathan Pratten1, Nicola Mordan1, Ailbhe McDonald1, Michael Wilson1 &Derren Ready2
1UCL Eastman Dental Institute, London, UK; and 2Microbial Diseases, Eastman Dental Hospital, UCLH NHS Foundation Trust, London, UK
Correspondence: D. Ready, Microbial
Diseases, Eastman Dental Hospital, UCLH
NHS Foundation Trust, 256 Gray’s Inn Road,
London WC1X 8LD, UK. Tel.: 144 20 7915
1050; fax: 144 20 7915 1127; e-mail:
Received 18 July 2008; accepted 21 November
2008.
First published online 22 December 2008.
DOI:10.1111/j.1574-6968.2008.01463.x
Editor: William Wade
Keywords
MRSA; denture; disinfection; oral cavity;
biofilm; antimicrobial susceptibility.
Abstract
Methicillin-resistant Staphylococcus aureus (MRSA) is an important nosocomial
pathogen, which is responsible for considerable morbidity and mortality in
the United Kingdom. The major reservoir of this organism is thought to be the
anterior nares, but there is increasing evidence that this pathogen is present in the
oral cavity, particularly in denture wearers. The purpose of this study was to
determine whether MRSA, grown as biofilms on denture acrylic resin, could be
eradicated using commercially available agents. EMRSA-15 or EMRSA-16 was
grown in a model system on the surface of denture acrylic resin for 4, 24 or 120 h
before the samples were exposed to a range of disinfectants for time intervals of 1, 5
and 10 min. All of the agents reduced the number of cultivable MRSA bacteria
present on the acrylic resin surface at 4 h, with 2% sodium hypochlorite (NaOCl)
eliminating MRSA below the level of detection after an exposure of 1 min.
However, the established MRSA biofilms (24 and 120 h) were more resistant to
killing by the agents, although 2% NaOCl was still able to eradicate all ages of
MRSA biofilms within 1 min of exposure.
Introduction
Staphylococcus aureus, particularly methicillin-resistant
strains of the organism (MRSA), are important nosocomial
pathogens. MRSA infection occurs mainly in people aged
65 or older (Maudsley et al., 2004) and poses a serious
challenge to healthcare providers. Although the importance
of methicillin-sensitive S. aureus (MSSA) and MRSA as
pathogens has long been recognized, the significance of their
presence within the oral cavity has only been highlighted in
the literature in the last decade (Rossi et al., 1997; Smith
et al., 2001, 2003a, b; Maeda et al., 2007). A number of oral
infections are caused at least in part by S. aureus, for
example, angular cheilitis, parotitis and staphylococcal mu-
cositis (Smith et al., 2003a, b), and it has been confirmed
that MSSA and MRSA can be isolated from the oral cavity
(Smith et al., 2001, 2003a, b). Furthermore, there has been
an increase in the number of reports suggesting that
S. aureus from the oral cavity can cause infection at distant
sites (Smith et al., 2001, 2003a, b).
The major reservoir of S. aureus is thought to be the anterior
nares, but there is increasing evidence that the organism is
present in the oral cavity, particularly in denture wearers
(Ayliffe et al., 1998; Smith et al., 2001). Staphylococcus aureus
has been isolated from 24% to 36% of healthy oral cavities,
but the incidence has been reported to rise to 48% in denture-
wearing patients (Dahlen et al., 1982; Ohman et al., 1995). In
one UK study carried out over a 3-year period, 5% of oral
specimens containing S. aureus were shown to be MRSA
strains (Smith et al., 2003b). In a separate study, MRSA was
recovered from 10% of unselected denture-wearing patients
in Japan (Tawara et al., 1996) and from 19% of the mouths
of an elderly institutionalized group (Owen, 1994).
The suggestion that prosthetic devices in the oral cavity,
including dentures, may encourage colonization of MRSA
and indeed, act as a source of cross-infection or recoloniza-
tion, is of growing concern (Rossi et al., 1997; Smith et al.,
2001, 2003a, b; Maeda et al., 2007). This may be especially
problematic in institutional settings, including hospitals,
where denture cleaning is often undertaken by carers,
potentiating horizontal transmission to other vulnerable
hosts. Additionally, there is a risk of cross-infection to and
from the dental and medical team in any setting. A recent
survey of MRSA prevalence in intensive care units showed
that 16% of patients were either colonized or infected with
MRSA (Hails et al., 2003).
FEMS Microbiol Lett 291 (2009) 241–246 c� 2008 Federation of European Microbiological SocietiesPublished by Blackwell Publishing Ltd. All rights reserved

Denture cleaning and disinfection procedures rely on a
range of antimicrobial agents; however their ability to
eradicate MRSA, growing as a biofilm i.e. the natural state
of the organism in denture-associated plaque, has not been
fully assessed. The aim of this work was to determine
whether current procedures for chemical decontamination
of dentures are sufficient to eradicate planktonic, early
attached cells, and established and mature MRSA biofilms
present on denture acrylic resin.
Materials and methods
Minimum inhibitory concentration (MIC) ofdenture cleansers
Susceptibility testing was performed by a broth dilution
method (CLSI, 2006). Antimicrobial agents were double
diluted in Mueller Hinton broth. A standardized bacterial
inoculum was prepared of either EMRSA-15 (NCTC 13142)
or EMRSA-16 (NCTC 13143), added to the diluted anti-
microbial agents and incubated for 18 h at 37 1C. The agents
tested were 2% sodium hypochlorite (NaOCl) (Miltons
Sterilising Fluid, Milton Pharmaceutical Ltd, Nantes,
France); 2% w/v aldehyde-free, oxygen-releasing disinfec-
tant solution recommended for disinfection of prosthetic
material and dental impressions (Performs-ID, Schulke &
Mayr UK Ltd, Sheffield, UK) and a 1.5% w/v alkaline
peroxide denture cleanser solution [Steradent Active plus,
Reckitt Benckiser (UK) Ltd, Swindon, UK]. Miltons Ster-
ilising Fluid was used as supplied by the manufacturer;
Performs-ID and Steradent Active plus were prepared as
per the manufacturer’s instruction in sterile water. The MIC
was defined as the lowest concentration of the agent that
inhibited visible growth.
Testing of denture cleansers against sessileorganisms
Biofilms were grown on denture acrylic resin in a Constant
Depth Film Fermenter (CDFF), which is an artificial mouth
model able to generate large numbers of identical biofilms.
A 10-mL volume from an overnight culture of EMRSA-15 or
EMRSA-16 was added to 500 mL of nutrient broth, mixed
and pumped into the fermenter over an 8-h period to
provide the bacterial inoculum. The inoculation vessel was
disconnected and a medium reservoir containing sterile
nutrient broth was connected and delivered via a peristaltic
pump at a rate of 0.5 mL min�1. Five millimeter denture
acrylic resin discs were prepared by firstly making a mould by
pouring addition-cured silicone (Shera Duo-Sil H, Addition-
cure Silicone duplicating system, Shera GmbH & Co. KG,
Lemforde, Germany) over blank Perspex rods with a dia-
meter of 5 mm. A self-curing acrylic resin was then prepared
by mixing the polymer powder (Rapid Repair Polymer,
shade pink, Chaperlin & Jacobs Ltd, Sutton, UK) and
monomer liquid (Rapid Repair Monomer, Chaperlin &
Jacobs Ltd) according to the manufacturer’s instructions.
The mixture was packed into the mould and the whole setup
then placed into a pressure pot for a curing cycle of 15 min
at room temperature. The prepared acrylic resin rod (5 mm
in diameter) was removed from the mould and cut into
sections with a depth of 8.0–10.0 mm, the samples were
polished to standardize the surface area. All samples were
then soaked in plain water for two 24-h cycles before use.
Discs were aseptically removed from the fermenter at 4,
24 and 120 h. Triplicate samples were placed into 1 mL of
each test agent or sterile phosphate-buffered saline and kept
for 1, 5 or 10 min before being removed, placed into 1 mL of
neutralizing buffer (Becton Dickinson, Detroit, MI) and
then vortexed for 1 min to disrupt the biofilm. The samples
were serially diluted and bacterial survival was determined
by spread plating in duplicate onto Columbia Blood Agar
plates (Oxoid Ltd, Basingstoke, UK) containing 5% defibri-
nated horse blood (E & O Laboratories, Bonnybridge, UK).
After 24-h incubation, colonies were counted, allowing the
number and percentage of isolates killed by the different
regimes to be calculated.
Scanning electron microscopy (SEM)
To carry out SEM, samples were fixed in 3% glutaraldehyde
in 0.1 M sodium cacodylate buffer at 4 1C overnight. The
specimens were dehydrated in a graded series of alcohol
(20%, 50%, 70%, 90% and 100%� three 10-min applica-
tion time). The samples were then transferred into hexam-
ethyldisilazane (TABB Laboratories Ltd, Reading, UK) for
1–2 min before drying on filter paper in a fume cupboard.
Once dry, the specimens were placed on aluminium stereo-
scan stubs with adhesive carbon tags (Agar Scientific,
Stansted, UK). The samples were coated with a metallic
layer of gold/palladium in a Polaron E5000 sputter coater
(Quorum technology Ltd, Newhaven, UK) and viewed in a
Cambridge Stereoscan 90B Electron Microscope (Zeiss,
Cambridge, UK).
Statistical analysis
Analysis of the viable counts before and after exposure to the
different agents was carried out using the Mann–Whitney
U-test. Data were analysed using SPSS software, and the 5%
level of significance was used throughout these analyses.
Results
MIC of EMRSA-15 and EMRSA-16
All three agents inhibited planktonic EMRSA-15 and EMR-
SA-16. NaOCl was the most effective with an MIC of 0.03%
FEMS Microbiol Lett 291 (2009) 241–246c� 2008 Federation of European Microbiological SocietiesPublished by Blackwell Publishing Ltd. All rights reserved
242 D. Lee et al.

(1 : 64 dilution) when tested against EMRSA-15 or EMRSA-
16. The MIC of Performs-ID when tested against either
strain of MRSA was 0.12% (1 : 16 dilution). Steradent was
also able to inhibit the growth of both MRSA strains,
although EMRSA-16 appeared to be less susceptible to this
agent with a 0.38% w/v (1 : 4 dilution) being required to
inhibit growth of this bacterium compared with EMRSA-15,
which was inhibited at a concentration of 0.09% (1 : 16
dilution).
EMRSA-16 and EMRSA-16 biofilms
The number of bacteria present on the surface of the denture
acrylic resin increased over the 120-h time period (Fig. 1).
At 4 h, an average of 3.5� 104 CFU mm�2 of EMRSA-15 and
7.6� 103 CFU mm�2 of EMRSA-16 were recovered from
the denture acrylic resin disks. This number increased after
24 h with 4.1� 105 CFU mm�2 of EMRSA-15 and 9.7�105 CFU mm�2 of EMRSA-16 attached to the denture acrylic
resin surface. The average total viable count of the mature
biofilm at 120 h had increased further to 1.1� 107 CFU mm�2
for EMRSA-15 and 2.4� 107 CFU mm�2 for EMRSA-16.
Susceptibility of EMRSA-15 and EMRSA-16biofilms
Four-hour sessile EMRSA-15 or EMRSA-16 were rapidly
killed by Miltons at all three time intervals (Figs 2 and 3). A
10-min exposure time to Steradent led to elimination of 4-h
sessile EMRSA-15 and EMRSA-16 below the level of detec-
tion (2.7 CFU mm�2). Exposure to Steradent for 1 min was
the least effective regime and achieved a 38.6% and 91.1%
reduction in the number of viable EMRSA-15 and EMRSA-
16 cells, respectively. A 10-min exposure time to Performs-
ID was sufficient to eliminate EMRSA-16 below the level of
detection; however, total elimination of EMRSA-15 was
not achieved with 7.1� 102 CFU mm�2 surviving these
conditions.
The 24-h established EMRSA-15 and EMRSA-16 biofilms
were rapidly killed by Milton, with bacterial numbers below
the level of detection even after an exposure period of only
1.0E+00
1.0E+01
1.0E+02
1.0E+03
1.0E+04
1.0E+05
1.0E+06
1.0E+07
1.0E+08
Contro
l
Milto
n 1
min
Stera
dent
1 m
in
Perfo
rm 1
min
Milto
n 5
min
Stera
dent
5 m
in
Perfo
rm 5
min
Milto
n 10
min
Stera
dent
10
min
Perfo
rm 1
0 m
in
Agent / exposure time
CF
U m
m−2
Fig. 2. Survival of a 4-, 24- and 120-h EMRSA-15
after exposure to Miltons, Performs-ID and
Steradent for 1, 5 and 10 min. White bars represent
4-h sessile biofilms, grey bars represent 24-h
established biofilms and black bars represent 120-h
mature biofilms. Error bars represent SDs.
Fig. 1. SEM images of MRSA deposition and biofilm development on
denture acrylic resin after 4 h (a), 24 h (b) and 120 h (c).
FEMS Microbiol Lett 291 (2009) 241–246 c� 2008 Federation of European Microbiological SocietiesPublished by Blackwell Publishing Ltd. All rights reserved
243Susceptibility of MRSA denture biofilms

1 min (Figs 2 and 3). A 1-min exposure to Steradent was the
least effective regime when tested against EMRSA-15 with
only 16.9% of the viable cells killed; however, a 10-min
exposure to Steradent did result in a significant reduction in
the viable numbers of EMRSA-15 (99.7% kill; Po 0.05) and
EMRSA-16 (98.4% kill; Po 0.05). Exposure to Performs-
ID for 1 min significantly reduced the viable numbers of the
established 24 h EMRSA-16 biofilms from 9.7� 105 to
2.2� 103 CFU mm�2 (99.8% kill; Po 0.05) and EMRSA-15
biofilms from 4.1� 105 to 2.0� 104 CFU mm�2 (95.1% kill;
Po 0.05).
The results obtained using the mature 120-h EMRSA-15
or EMRSA-16 biofilms showed that these two pathogens
were again rapidly killed by Miltons with a 1-min exposure
time being sufficient to eliminate these bacteria below the
level of detection (Figs 2 and 3). Mature EMRSA-15 or
EMRSA-16 biofilms could not be eradicated below the level
of detection with a 10-min exposure to either Performs-ID
or Steradent, as demonstrated by a 100% survival rate for
EMRSA-16 after exposure to Steradent for this time period.
A 10-min exposure to Performs-ID, however, did lead to a
significant reduction in the total viable numbers of mature
120 h biofilms of EMRSA-15 (4 99.99% kill; Po 0.05) and
EMRSA-16 (96.83% kill; Po 0.05).
Discussion
The two epidemic strains, EMRSA-15 and EMRSA-16, are
the dominant forms of MRSA in the United Kingdom. The
possibility that dentures may act as a reservoir of MRSA is
becoming increasingly acknowledged (Rossi et al., 1997;
Maeda et al., 2007) and, therefore, the aim of this study was
to establish whether current disinfection cleansers are effec-
tive in killing MRSA when growing as biofilms on denture
acrylic resin.
Four phases of MRSA growth were used in this study:
planktonic, sessile (4 h), established biofilms (24 h) and
mature biofilms (120 h). Studying biofilm development
and perturbation requires the use of a reproducible model
system. The CDFF has previously been used to produce
in vitro denture plaque biofilms with similar compositions
to those seen in vivo (Lamfon et al., 2005). Furthermore,
using this model, longitudinal analysis can be carried out.
Indeed, it has previously been shown that the susceptibility
of biofilms to antimicrobial agents changes throughout
biofilm development (Lamfon et al., 2004).
Our results suggest that the only agent that was able to
consistently eradicate EMRSA-15 and EMRSA-16 when
grown in all four phases was Miltons Sterilising Fluid. This
agent eliminated bacterial numbers below the level of
detection even with an exposure time of only 1 min.
Previous studies have shown that NaOCl not only kills
viable bacterial cells but also is able to remove the biofilm
from the surface (Clegg et al., 2006). Furthermore, in
addition to its antimicrobial activity, NaOCl also may
remove stains and dissolve mucin and other organic sub-
stances (Jagger & Harrison, 1995). However, as NaOCl has
previously been shown to cause bleaching of denture acrylic
resin and corrosion of the metal parts of dentures, dentists
may be apprehensive to use it for this application; however,
the short immersion times, seen in this study, required to
eliminate MRSA biofilms may avoid or minimize this
complication (Jagger & Harrison, 1995).
Bacteria in the planktonic phase of growth are routinely
used to determine the susceptibility to antimicrobial agents.
The MIC data for Performs-ID and Steradent demon-
strated that planktonic EMRSA-15 and EMRSA-16 were
susceptible to these two agents. However, the biofilm data
showed that these two agents had less ability to reduce the
24- and 120-h biofilms, to viable counts below the level of
1.0E+00
1.0E+01
1.0E+02
1.0E+03
1.0E+04
1.0E+05
1.0E+06
1.0E+07
1.0E+08C
FU
mm
−2
Contro
l
Milto
n 1
min
Stera
dent
1 m
in
Perfo
rm 1
min
Milto
n 5
min
Stera
dent
5 m
in
Perfo
rm 5
min
Milto
n 10
min
Stera
dent
10
min
Perfo
rm 1
0 m
in
Agent / exposure time
Fig. 3. Survival of a 4-, 24- and 120-h EMRSA-16
after exposure to Miltons, Performs-ID and
Steradent for 1, 5 and 10 min. White bars
represent 4-h sessile biofilms, grey bars represent
24-h established biofilms and black bars represent
120-h mature biofilms. Error bars represent SDs.
FEMS Microbiol Lett 291 (2009) 241–246c� 2008 Federation of European Microbiological SocietiesPublished by Blackwell Publishing Ltd. All rights reserved
244 D. Lee et al.

detection. Biofilm communities are known to be far more
resistant to antimicrobial agents than their planktonic
counterparts and for many years it has been obvious that
standardized tests such as MIC are no longer appropriate on
their own (Ready et al., 2002). This study was carried out
using monospecies biofilms of MRSA, and as MRSA on
denture materials in vivo would be present in multispecies
biofilms, their susceptibility profile may be further altered.
The ability of antimicrobial agents to eradicate the carriage
of multispecies biofilms harbouring EMRSA requires
further investigation.
Performs-ID significantly reduced EMRSA-15 and
EMRA-16 at all four phases of growth. Performs-ID is a
product that is currently used in both dental clinics and
hospital environments and, as it is not NaOCl based, its use
avoids complications such as bleaching. Although this
product did not eliminate MRSA below the level of detec-
tion at each time point, a 10-min exposure with this product
significantly reduced the microbial burden of the established
120-h MRSA biofilms. Steradent also demonstrated a high
level of anti-MRSA activity, especially against 4-h early-
attached cells, with MRSA eliminated below the level of
detection after a 10-min exposure time.
If in-patients are identified as MRSA carriers in a hospital
or nursing home setting, then disinfection for time periods
4 10 min would be possible. Therefore the ability to eradi-
cate mature MRSA denture biofilms after extended period of
exposure (including overnight soaking) to antimicrobial
agents, combined with the potential beneficial antibiofilm
activity of other antimicrobial agents used for denture disin-
fection such as chlorhexidine, glutaraldehyde, acetic acid,
hydrogen peroxide and sodium perborate (Buergers et al.,
2008; Da Silva et al., 2008) requires further investigation.
This study has demonstrated that planktonic MRSA are
rapidly killed using these three antimicrobial agents, which
correlates with the findings from a study by Maeda et al.
(2007). However, established (120 h) MRSA biofilms are
difficult to eradicate unless 2% NaOCl is used. Currently,
eradication of this organism from patients with high MRSA
carriage rates (elderly patients either hospitalized or in
nursing homes) may be significantly hindered if one possi-
ble source of reinfection, the patient’s own dentures, is either
ignored or inadequately disinfected.
Acknowledgement
This work was undertaken at UCLH/UCL, which received a
proportion of funding from the Department of Health’s
NIHR Biomedical Research Centres Funding Scheme, UK.
References
Ayliffe GAJ, Buckles A, Casewell MW et al. (1998) Revised
guidelines for the control of methicillin-resistant
Staphylococcus aureus infection in hospitals. J Hosp Infect 39:
253–290.
Buergers R, Rosentritt M, Schneider-Brachert W, Behr M, Handel
G & Hahnel S (2008) Efficacy of denture disinfection methods
in controlling Candida albicans colonization in vitro. Acta
Odontol Scand 66: 174–180.
Clegg MS, Vertucci FJ, Walker C, Belanger M & Britto LR (2006)
The effect of exposure to irrigant solutions on apical dentin
biofilms in vitro. J Endodont 32: 434–437.
Clinical and Laboratory Standard Institute (CLSI) (2006)
Methods for Dilution Antimicrobial Susceptibility Tests for
Bacteria that Grow Aerobically. Approved Standard. Document
M7-A7, 7th edn. Clinical and Laboratory Standard Institute
(CLSI), Wayne, PA.
Dahlen G, Lindhe A, Moller AJR & Ohman A (1982) A
retrospective study of microbiologic samples from oral
mucosal lesions. Oral Surg Oral Med O 53: 250–255.
Da Silva FC, Kimpara ET, Mancini MN, Balducci I, Jorge AO &
Koga-Ito CY (2008) Effectiveness of six different disinfectants
on removing five microbial species and effects on the
topographic characteristics of acrylic resin. J Prosthodont 17:
627–633.
Hails J, Kwaku F, Wilson AP, Bellingan G & Singer M (2003) Large
variation in MRSA policies, procedures and prevalence in
English intensive care units: a questionnaire analysis. Intens
Care Med 29: 481–483.
Jagger DC & Harrison A (1995) Denture cleansing-the best
approach. Brit Dent J 178: 413–417.
Lamfon H, Porter SR, McCullough M & Pratten J (2004) The
susceptibility of Candida albicans biofilms grown in a constant
depth film fermentor to chlorhexidine, fluconazole and
miconazole: a longitudinal study. J Antimicrob Chemoth 53:
383–385.
Lamfon H, Al-Karaawi Z, McCullough M, Porter SR & Pratten J
(2005) Composition of in vitro denture plaque biofilms and
susceptibility to antifungals. FEMS Microbiol Lett 242:
345–351.
Maeda Y, Kenny F, Coulter WA et al. (2007) Bactericidal activity
of denture-cleaning formulations against planktonic health
care-associated and community-associated methicillin-
resistant Staphylococcus aureus. Am J Infect Control 35:
619–622.
Maudsley J, Stone SP, Kibbler CC, Iliffe SR, Conaty SJ, Cookson
BD, Duckworth GJ, Johnson A & Wallace PG (2004) The
community prevalence of methicillin-resistant Staphylococcus
aureus (MRSA) in older people living in their own homes:
implications for treatment, screening and surveillance in the
UK. J Hosp Infect 57: 258–262.
Ohman SC, Osterberg T, Dahlen G & Landahl S (1995) The
prevalence of Staphylococcus aureus, Enterobacteriaceae
species, and Candida species and their relation to oral mucosal
lesions in a group of 79-year-olds in Goteborg. Acta Odontol
Scand 53: 49–54.
FEMS Microbiol Lett 291 (2009) 241–246 c� 2008 Federation of European Microbiological SocietiesPublished by Blackwell Publishing Ltd. All rights reserved
245Susceptibility of MRSA denture biofilms

Owen MK (1994) Prevalence of oral methicillin resistant
Staphylococcus aureus in an institutionalized veterans
population. Spec Care Dent 14: 75–79.
Ready D, Roberts AP, Pratten J, Spratt DA, Wilson M & Mullany P
(2002) Composition and antibiotic resistance profile of
microcosm dental plaques before and after exposure to
tetracycline. J Antimicrob Chemoth 49: 769–775.
Rossi T, Peltonen R, Laine J, Eerola E, Vuopio-Varkila J &
Kotilainen P (1997) Eradication of the long-term carriage
of methicillin-resistant Staphylococcus aureus in patients
wearing dentures: a follow-up of 10 patients. J Hosp Infect 34:
311–320.
Smith AJ, Jackson MS & Bagg J (2001) The ecology of
staphylococci in the oral cavity. J Med Microbiol 50: 940–946.
Smith AJ, Brewer A, Kirkpatrick P, Jackon MS, Young J, Watson S
& Thakker B (2003a) Staphylococcal species in the oral cavity
from patients in a regional burns unit. J Hosp Infect 55: 184–189.
Smith AJ, Robertson D, Tang MK, Jackson MS, MacKenzie D &
Bagg J (2003b) Staphylococcus aureus in the oral cavity: a three-
year retrospective analysis of clinical laboratory data. Brit Dent
J 195: 701–703.
Tawara Y, Honma K & Naito Y (1996) Methicillin resistant
Staphylococcus aureus and Candida albicans on denture
surfaces. Bull Tokyo Dent Coll 37: 119–128.
FEMS Microbiol Lett 291 (2009) 241–246c� 2008 Federation of European Microbiological SocietiesPublished by Blackwell Publishing Ltd. All rights reserved
246 D. Lee et al.