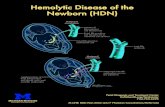
Rh negative pregnancy
-
Upload
obgymgmcri -
Category
Healthcare
-
view
841 -
download
1
Transcript of Rh negative pregnancy

Rh NEGATIVE PREGNANCYDr shweta

Contents
Introduction. Pathophysiology. Isoimmunisation. Diagnosis. Management. Effect on fetus.

INTRODUCTION Rh factor discovered by Landsteiner in
1937. Protein antigen of red cell membrane. 5% of pregnancies are Rh-ve. Inherited as Mendelian dominant. common cause of perinatal mortality in
babies of Rh-ve mothers.

PATHOPHYSIOLOGY Mother is Rh-ve with a Rh+ve foetus. Mother is having anti Rh antibodies. Antibodies cross placenta to foetus. Foetal Rh+ve red blood cells get
hemolysed. Foetus suffers from severe anaemia
leading to cardiac failure,oedema and death.

CAUSES FOR ISOIMMUNISATION OF THE
MOTHER
Previous Rh+ve fetus with isoimmunisation due to foeto-maternal haemorrhage.
May be full term delivery, abortion, ectopic or partial mole.
Previous Rh+ve blood transfusion.

ISOIMMUNISATION
Cause-foetomaternal haemorrhage.
Maternal blood produces large number of antibodies in response to small amount of foetal blood.
Amount of foetal blood required to cause isoimmunisation-0.1ml.
Antibodies thus formed in maternal blood stays lifelong.

contd Usual fetomaternal Hge- <4ml.
If no prophylaxis- sensitization in next pregnancy-16%.

DIAGNOSIS Routine blood grouping and typing for
all antenatal mothers on 1st visit.
If Rh-ve-, husband’s blood group.
If negative-normal pregnancy.
If positive-indirect Coomb’s test to look for isoimmunisation at 24 weeks.
If negative for antibodies-treat as nonisoimmunised Rh-ve pregnancy.

INDIRECT COOMB’S TEST(ICT)
Done in Rh-ve antenatal mothers with a Rh+ve husband.
Timing-24 weeks.
Detects incomplete IgG antibodies which can cross placenta.
Done with Coomb’s serum containing antiglobulin antibodies.

MANAGEMENT OF ICT-VE Anti D prophylaxis-at 28 weeks. After delivery if needed. Prevent anaemia. Arrange donors before delivery. Ensuring availability of blood in bank. Quick clamping of cord. Send cord blood for testing. Neonatal care facility.

CORD BLOOD TESTS Blood grouping and typing. Direct Coomb’s test. Bilirubin,Hb and haematocrit to detect
haemolysis,anaemia and jaundice.

ANTI D PROPHYLAXIS Anti D immunoglobulin is administered to
neutralise the Rh+ve blood which enters maternal circulation.
Sensitisation in next reduced to 1.6% compared to 16% if not given.
These antibodies disappear from blood within some time.

TIMING Within 72 hours of delivery if baby blood
group is Rh+ve and DCT-ve. After 1st trimester pregnancy loss. After invasive procedures-
amniocentesis,chorionic villus sampling,cordocentesis.
Antenatal-at 28 weeks. Also in 2nd,3rd trimester APH,ECV.

DOSE AND ROUTE Route-intramuscular injection. Dose-300µgm of anti D immunoglubulin. Neutralises 15ml of foetal RBC or 30ml
of blood. Higher dose required for larger FMH. Assessed by Kleihauer Betke test.

LARGE FMH Traumatic delivery. Abruption. Manual removal of placenta. Stillbirth,IUD. Twins. Hydrops fetalis.

KLEIHAUER BETKE TEST
To assess amount of FMH. Acid elution test which detects foetal
haemoglobin. Amount of foetal blood in ml= maternal blood vol x maternal hct X KB
cells/ fetal hct.

NONRESPONSE Immunologic nonresponder. Co-existing ABO incompatibility. Insufficient sensitising volume.

FOETAL EFFECT Mild effect-haemolytic anaemia of the
newborn. Moderate-effect-icterus gravis
neonatorum. Severe effect-hydrops foetalis.

CONGENITAL HAEMOLYTIC ANAEMIA
Anaemia develops slowly in first few weeks.
Jaundice is not evident. Haemolysis continues for 6 weeks after
which antibodies cease to exist.

ICTERUS GRAVIS NEONATORUM
Baby not jaundiced at birth. Develops so within 24 hours. Effect starts after cord clamping as
excretion through placenta stops and premature liver enzymes.
If serum bilirubin >20mg/dl-crosses blood brain barrier-kernicterus(damage of basal ganglia).

HYDROPS FOETALIS Severe haemolysis. Anaemia causes heart failure. Compensatory placental hyperplasia. Liver damage causing hypoprotinemia Oedema,hydrothorax,ascites. Stillborn or dies soon after. USG-Buddha foetus-for scalp edema.

MANAGEMENT OF ISOIMMUNISED PREGNANCY
Critical titer of Ab-1:16 to 1:32. If ICT +ve-titer at 1st visit-monthly. If below critical level-deliver at term. If >CL-if mature lungs-delivery. If immature lungs-glucocorticoids. If below 36weeks-amniocentesis and
bilirubin estimation.

Contd High titer or multiple isoimmunised
pregnancy or previous history of EF- amniocentesis,bilirubin estimation at OD450.
Plot it in Liley’s graph as zones 1,2 or 3 with zone 3 as most severe.
Zone1-deliver at term. Zone 2-repeat titer after 2 weeks. Zone 3-cordocentesis and IUT.

CORDOCENTESIS Under USG guidance. 0.5 to 2 ml collected from umbilical
vein. Risk of abortion,preterm labour,IUD. Test for foetal haematocrit and bilirubin.

FOETAL MONITORING USG-polyhydramnios/foetal hyrops
though a late finding. Amniocentesis and Liley graph plotting-
from 26 weeks. Middle cerebral artery peak systolic
velocity-18 weeks onwards.

INTRAUTERINE TRANSFUSION
Based on –Hct,amniocentesis or MCA-PCV.
Route-intravascular(portal/umbilical vein),intraperitoneal.
Blood-fresh O-ve packed cells. Amount based on gestational age or
Nicolaide’s formula.

TREATMENT OF BABY Phototherapy-with blue light with
protection of eye and genitalia from exposure.
Phenobarbitone. Exchange transfusion.

EXCHANGE TRANSFUSION INDICATIONS-cord Hb<10gm/dl cord bil>5mg/dl rising rate>1mg/dl/hr Aim –to correct anaemia,to remove
antibodies and bilirubin. Route-umbilical vein by push and pull
technique. Watch for hypoglycemia,
hypocalcimea,metabolic acidosis.

Conclusion
Rh negative pregnancy should be thoroughly investigated to rule out adverse effects on the mother and the fetus.

THANK YOU