Respiratory System
description
Transcript of Respiratory System

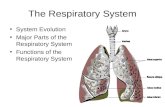
Respiratory System
Lecture 1

Functions• gas exchange
–between air & blood• sound production• sends olfactory sensations to CNS
from olfactory epithelium• helps to control blood pH• moves air to & from exchange surfaces• filters air• helps rid some water and heat in
exhaled air

Structural Anatomy • upper respiratory
system
–nose, nasal cavity & pharynx
• lower respiratory system
–larynx, trachea, bronchi & lungs

Functional Anatomy• conducting zone
– respiratory paths from nasal cavity through bronchioles
– consists of rigid conduits for air to reach sites of gas exchange
• respiratory zone– actual site of gas
exchange– includes respiratory
bronchioles, alveolar ducts & alveoli

Epithelium• changes along tract
• pharynx-stratifed squamous
• lower-pseudostratified ciliated columnar
• bronchioles-cuboidal
• exchange surfaces-simple squamous

Respiratory Mucosa• conducting path lined with respiratory mucosa• conditions air• by time air reaches alveoli, foreign particles &
pathogens have been removed• humidity & temperature are acceptable limits• pseudostratified ciliated columnar epithelium,
goblet cells & underlying alveolar tissue• Goblet cells
– secrete mucous containing lyzozymes-antibacterial enzymes & defensins-antibodies that help rid body of microbes
• Mucous– intercepts & excludes solid matter in air
such as dust, pollen, bacteria & viruses• particles hit side wall-trapped in mucus• once particles are sidelined by mucus• carried out by cilia
– tiny hair-like structures which undulate 1200 movements/minute
– undulation keeps mucous moving either up toward pharynx or down toward stomach
– upward & downward movement is termed- mucociliary escalator

Respiratory System Anatomy• nose
– primary passage for air to enter through external nares-nostrils
– warms, cleanses & humidify inhaled air
• extends from external nares to posterior or internal nares
• nose empties into nasal cavityvestibule– space just inside nose containing hair
follicles-vibrissae – filters particles out of air
• nasal cavity is divided by nasal septum• Roof
– made of ethmoid & sphenoid bones• Floor
– palate• in each bone surrounding nasal cavity
there are holes-paranasal sinuses• lighten skull

Pharynx• nasal cavity leads into pharynx• consists of 3 regions• Nasopharynx
– posterior to nasal cavity– extends to soft palate– air passage only
• Oropharynx– posterior to oral cavity– extends from soft palate to
hyoid bone– air & food passage
• Laryngopharynx– begins at hyoid opens into
esophagus posteriorly & larynx anteriorly
– common passage for air & food – air & food passage


Larynx• voice box• opens into
laryngopharynx• continuous with
trachea inferiorly• provides open airway
& switching mechanism to route air & food into proper channels
• functions in voice production
• consists of 9 cartilages

Larynx Cartilages• thyroid
– large, shield shaped cartilage
– fusion-laryngeal prominence
• Adam’s Apple• cricoid cartilage
– inferior to thyroid cartilage– ring-like
• arytenoid• cuneiform• corniculate• epiglottis
– flexible elastic cartilage

Trachea• below larynx• patent or open
– kept so by rings of C or tracheal cartilages
• descends from larynx into mediastium
• divides into right & left primary bronchi
• enters lungs at hilus• right & left primary bronchi
are paired but of unequal length & diameter
• right-wider, shorter & more vertical

Bronchi• primary bronchi subdivide into
secondary or lobar bronchi– 3 on right & 2 on left
• lobar bronchitertiary or segmental bronchidivide into smaller & smaller bronchioles
• air passages<1mm in diameter-bronchioles
• smallest<0.5mm-terminal bronchioles
• arborizing branching pattern is respiratory or bronchial tree
• conducting zone

Label the Parts of the Respiratory Tree

Alveoli• each terminal bronchiole feeds into
respiratory bronchiole– beginning of respiratory division
• each respiratory bronchiole divides into 2 to 10 long, thin passages- alveolar ducts
• ducts end in spongy, air-filled sacs-alveolar sacs
• each cluster-made of alveoli– comprise most of volume of lung– responsible for spongy look– provide tremendous surface area
for gas exchange• surrounded by capillaries & elastic
tissue– can recoil to help push out air
• inhaled O2 passes into alveoli, diffuses through capillaries & then into arterial blood

Respiratory Membrane• walls of alveoli are simple squamous-type I
alveolar cells• main sites of gas exchange• type II alveolar cells-Septal cells• secrete pulmonary surfactant• alveolar macrophages-dust cells
– phagocytize dust & other particles. • external surface of each alveolus is covered
with capillaries• barrier between alveolar air & blood-
respiratory membrane consists of only squamous alveolar cells, squamous endothelial cells of capillary walls and shared basement membrane
• gas on one side• blood on other• gas exchange occurs by simple diffusion-
from higher to lower concentration• diffusion is rapid because:• distances are small• O2 & CO2 are lipid soluble • can pass through surfactant layer
O2 CO2
Alveolus
CapillaryType II
Macrophage
Type I

Surfactant• mixture of phospholipids &
lipoproteins• prevents alveoli from collapsing• detergent like properties• coats alveolar surfacesreduces
surface tension– attraction between water
molecules at air-water boundary. • molecules of liquids are more
strongly attached to each other than gasproduces tension at surface
• creates barrier keeping small objects from entering & causes small bubbles to collapse
• interferes with cohesiveness of water moleculesreduces surface tension less energy needed to overcome force to expand lungs

Respiratory Physiology• gas exchange-respiration has 3 steps
• pulmonary ventilation-breathing
• external respiration
–exchange of gases between blood & lungs
• internal respiration– exchange of gases between capillary
blood & tissues

Breathing• Pulmonary
ventilation– physical movement
of air into & out of respiratory tract
• consists of• inspiration-taking air
into lungs• expiration-gas
exiting lungs• mechanical

Pressure & Volume Changes• air moves into & out of respiratory tract as air
in lungs cycles between below atmospheric & above atmospheric pressure
• depends on volume changes in thoracic cavity
• volume changespressure changesgases flowpressure equalizes
• to understand need to understand physical principles of gases-gas laws

Boyle’s Law-Ideal Gas Law• relationship between pressure &
volume • at constant temperature pressure of
gas varies inversely with its volume• P1V1=P2V2
– P = pressure of gas-mm Hg– V = volume-cubic mm
• gases conform to shape of container in which they are contained– always fill container
• large volumesgas molecules far apart don’t bump into each other much pressure low
• reduced volumes gas molecules compress & bump into each other more often pressure rises
• when volume of gas decreases pressure increases
• when volume of gas increases pressure decreases
• relationship can be stated in formula– P = 1/V

Boyle’s Law & Breathing• inhalation & exhalation
involve changes in lung volumes creates pressure changes moves air into & out of lungs
• think of thoracic cavity as gas filled box with one opening
• each lung enclosed in box bounded below by diaphragm
• on sides by chest wall & mediastinum

Boyle’s Law & Breathing• parietal & visceral pleurae of pleural
cavity are separated by thin layer of pleural fluid
• allows them to slide past one another but still be held together by fluid between
• tension makes surface of lungs stick to inner chest wall & to diaphragm
• movement of chest wall or diaphragm changes volume of lungs
• breathing makes box bigger• as rib cage moves updepth &
width of thoracic cavity increases• contraction of diaphragmmoves
diaphragm inferiorlyincreases volume of thoracic cavityalveolar pressure decreases– Pinside <P outsideair rushes in

Inhale-Quiet Inspiration• diaphragm & external
intercostals contract
• ribs lift & pulled outward
• diaphragm moves downward chest cavity enlargeslung expands to fill space pressure inside lung lowers air enters respiratory tract
• P inside < pressure outside
• air moves in until P inside = P outside

Exhalation• diaphragm &
intercostals relax• thoracic cavity
decreases in volume• ribs return to position• P inside decreases
air forced out

Inhalation & Exhalation

Pressure Changes during Inhalation & Exhalation
• respiratory pressures are given relative to atmospheric pressure
• Atmospheric pressure-Patm– measured in mm Hg– pressure exerted by air
surrounding body• sea level = 760mm Hg or 1
atm• pressure in respiratory system
– measured in air spaces of lungs-alveolar pressure or intrapulmonary pressure
– measured in pleural fluid between parietal & visceral pleurae-intrapleural pressure

Inhalation• air continues to flow into alveolipressure increases until thoracic cage stops
expanding• air movement continues until pressure inside equalizes with atmospheric
pressure• during this time intrapleural pressure drops to -6mm Hg• pressure averages –4mm Hg below atmospheric pressure at all times due to
relationship of lungs & body wall

Exhalation

Intrapleural Pressure• opposing forces at lungs produce
negative pressure at all times• alveolar fluid surface tension pulls
visceral pleura away from parietal pleura producing strong fluid bond
– force keeps pleurae together– opposed by elasticity of chest wall
• elastic components gives lung natural tendency to recoil
– cannot overcome fluid bond• elastic fibers stay stretched even
after full exhalationpressure remains negative negative intrapleural pressure
• amount of fluid in pleural cavity must be minimal to maintain negative pressure
• negative pressure is important because anytime intrapleural pressure equalizes with intrapulmonary pressure-lung collapses

Muscles of Breathing• air moves due to pressure
changes
• direct result of volume changes
• due to muscle contractions• main muscles-quiet inspiration-
diaphragm & external intercostals
• diaphragm-responsible for 75% of air flow
• external intercostals-25%• deep or forced breathing is
aided by• Sternocleidomastoids• Scalenes• Pectoralis minor

Mechanics of Expiration• Quiet expiration due to
muscle relaxation• passive• muscle contraction is not
required• depends on natural
elasticity or elastic recoil of lungs
• Forced expiration• active process• requires contraction of
accessory muscles • transversus abdominus• rectus abdominus


Other Factors Influencing Air Flow• surface tension
– must be overcome to expand lungs– surfactant– reduces surface tension
• compliance of lungs– effort required to stretch lung & chest wall
• lower compliancegreater force needed to fill & empty lungs
• greater compliancelungs easier to fill & empty
– surfactant increases compliance– Decreased mobility of thoracic
cagedecreases compliance
• airway resistance – resistance to air flow– walls of bronchioles offer some resistance to
flow– larger diameters have less resistance– any condition that narrows walls increases
resistance

Respiratory Cycle• one cycle consists of one
inhalation & one exhalation• Tidal volume
– amount of air brought into & taken out of lungs in one respiratory cycle
• beginning of respiratory cycle intrapulmonary & atmospheric pressures are equalno air movement
• Inhalation beginsintrapleural pressure drops due to expansion of thoracic cavity to –6mm Hg-intrapulmonary pressure drops to –1mm Hg
• Exhalation– intraplueral & intrapulmonary
pressures riseair forced out of lungs
• End of respiratory cycle– atmospheric & intrapulmonary
pressures become equal again

Respiratory Rates• respiratory system adapts to meet
O2 demands of body
• does so by varying number of breaths per minutes or BPM
• number of breaths taken each minute = respiratory rate
• 12-18 bpm-normal range

Respiratory Rates• MV-minute volume• total volume of air inhaled &exhaled each
minute• MV = F (bpm) X VT (tidal volume)
– 12 X 500 = 6000ml/minute• may not indicate how much air reaches
alveoli– not all air reaches alveoli-remains in
conducting airways & does not exchange gases with blood
• anatomical dead space-150ml

Respiratory Rates• during one inhalation 500 mls of fresh air (tidal
volume) is brought into respiratory system• displaces 150ml of stale air in dead
spaceleaving 350ml of fresh air to go to alveoli• Tidal Volume – Dead Space = 500ml- 150ml =
350ml– 350 ml of air is involved in alveolar ventilation
• Alveolar ventilation rate-VA– amount of air reaching alveoli each min
• VA = f X (TV – VD). 12 breaths/min X (500ml/breath – 150ml/breath) = 4200ml/min or 4.2L/min
• better indicator of ventilation because determines rate of O2 delivery to alveoli

Respiratory Rates• minute volume can be increased by
increasing tidal volume or respiratory rate
• O2 demands increaseTV & respiratory rate must increase
• rate of breathing or depth of breathing changes alveolar ventilation

Respiratory Volumes• total volume of lungs can be divided into volumes &
capacities• Volumes:• tidal volume
– amount of air moving during quiet inspiration & expiration; 500 mls
• inspiratory reserve volume– amount of air that can be inspired beyond tidal inspiration– differs significantly by gender; lungs of males are larger
• expiratory reserve volume– amount of air that can be exhaled after normal expiration
• residual volume– amount of air left after strenuous expiration– cannot be directly measured– keeps alveoli open & prevents lung collapse– part is minimal volume
• volume of air remaining when lung collapse

Respiratory Capacities• sum of 2 or more lung volumes• IC-inspiratory capacity
– total amount of air that can be inspired after tidal expiration = TV + IRV
• FRC-functional residual capacity = RV + ERV– amount of air remaining after tidal expiration
• VC-vital capacity– total amount of exchangeable air = TV + IRV + ERV– amount of air that can be moved into or out of respiratory system with
one breath
• TLC-total lung capacity – sum of all lung volumes = VC + RV
• FVC-forced vital capacity – amount of gas expelled when deep breath is taken & then forcibly
exhaled as maximally as possible






![Respiratory System [โหมดความเข้ากันได้] · PATHOLOGY OF RESPIRATORY SYSTEM นพ. อรรณพ นาคะป ท Respiratory system U it](https://static.fdocuments.us/doc/165x107/5fa578efd4e80f055f6b3401/respiratory-system-aaaaaaaaaaaaaaaaaa-pathology.jpg)



![Anatomy and Physiology Respiratory System [Tab 2] Respiratory System.](https://static.fdocuments.us/doc/165x107/56649ebd5503460f94bc631f/anatomy-and-physiology-respiratory-system-tab-2-respiratory-system.jpg)









![Respiratory system roadmap.pptx [Repaired] - Loginanatomical-sciences.health.wits.ac.za/roadmaps/Respiratory system... · DIVISION OF THE RESPIRATORY SYSTEM CONDUCTING PORTION Nasal](https://static.fdocuments.us/doc/165x107/5a78c3d87f8b9ae6228c9db0/respiratory-system-repaired-loginanatomical-scienceshealthwitsaczaroadmapsrespiratory.jpg)