Physiotherapy Mgt of Infection in UL(160313) · sling suspension 8 Acute Phase Intervention –...
-
Upload
nguyenkhue -
Category
Documents
-
view
219 -
download
1
Transcript of Physiotherapy Mgt of Infection in UL(160313) · sling suspension 8 Acute Phase Intervention –...

Physiotherapy Management of Infection in Upper Limb
Raymond Tsang
13 March 2016
2
Hand Infection
In general, 3 phases for Assessment & Intervention for Physiotherapist:
• Acute Phase – acute inflammation & infection
• Post-Acute Phase – resolving inflammation & infection
• Post-Infection Phase – infection under control
3
Acute Phase
Assessment1. Acute Inflammation• Redness• Swelling• Temperature increase• Pain• Loss of function
4
Acute Phase
Assessment2. Wound Condition• 3-colour concept – red, yellow & black
wound• Any pus or abscess collection

5
Acute Phase
Intervention – Aims & Methods1. To minimize exacerbation of
inflammation & infection• Rest/immobilization (boxing glove
bandaging)• Compression (boxing glove
bandaging)• Elevation
6
Boxing Glove Bandaging
• Compression– venous return & oedema
• Reduction of inflammatory changes– rest– pain
• Facilitation of wound drainage
7
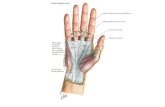
Elevation with sling suspension
8
Acute Phase
Intervention – Aims & Methods2. To prevent joint contracture• Rest/immobilization in intrinsic plus
position (position of immobilization)3. To drain pus and clean wound• Hibitane bath

9
Acute Phase
Intervention – Aims & Methods3. To drain pus and clean wound• Saline irrigation for deep wound• Whirlpool therapy (past)
10
Post-Acute Phase
Assessment1. Inflammation• Redness• Swelling• Temperature increase• Pain
11
Post-Acute Phase
Assessment2. Wound Condition• More healthy wound condition (with
the use of antibiotics debridement)• Pus or abscess collection
3. Joint ROM & Soft Tissue Adhesions
12
Post-Acute Phase
Intervention – Aims & Methods
1. To prevent/improve finger joint stiffness & soft tissue contracture
• Gentle active passive finger mobilization exercises

13
Post-Acute Phase
Intervention – Aims & Methods2. To prevent tendon adhesions &
improve tendon gliding• Tendon gliding exercises
14
Post-Acute PhaseIntervention – Aims &
Methods3. To reduce residual
swelling• Pneumatic compression
therapy• Massage• Bandaging; Coban wrap• Advice on continuing &
appropriate elevation
15
Intermittent Pneumatic Compression
(Lowe et al, 2005)16
Post-Infection Phase
Assessment1. Joint ROM & Joint Stiffness2. Soft Tissue Adhesions/Scars3. Residual Swelling4. Muscle Strength5. Pain6. Function

17
Post-Infection Phase
Intervention – Aims & Methods1. To improve finger joint ROM, stiffness
& soft tissue contracture• Active passive finger mobilization
exercises• Stretching
18
Post-Infection PhaseIntervention – Aims & Methods2. To improve soft tissue adhesions/Scars• Massage• Ultrasound therapy3. To improve tendon gliding• Tendon gliding exercises4. To muscle strength• Muscle strengthening exercises
19
Post-Infection Phase
Intervention – Aims & Methods5. To improve functions• Dexterity training• Work conditioning/simulation
programme
20
Common Infection Cases• Paronychia – infection of space surrounding
eponychial fold

21
Common Infection Cases• Felon – infection of closed space of volar
digital pulp
Septa22
Common Infection Cases• Felon
Treatment – Incision and drainage; appropriate antibiotics; open drainage of wound – saline gauze packing
23
Common Infection Cases• Infective Tenosynovitis
(Tubiana et al, 1996) Incision & Continuous Drainage
24
Common Infection Cases• Infective Tenosynovitis

25
Special Infection Cases
• Mycobacterial Infections– Typical: Mycobacterium Tuberculosis– Atypical:
(Bhambri et al, 2009)
26
M. Marinum
(Bhambri et al, 2009)
27(Cheung et al, 2010)
M. Marinum
28
Postoperative immobilization in boxing glove bandaging for 3 weeks
(Cheung et al, 2010)

M. Marinum
Drug Treatment (QMH)(1) Standard regimen for previously untreated patient.• Ethambutol and rifampicin(2) For patient with relapse after treatment• Clarithromycin and minocycline and ethambutolDuration of treatment• 6 month in total or at least 2 more months after definite clinical
improvementDosage• Ethambutol 15mg/kg QD daily• Rifampicin 450mg (for BW ≤ 50kg) or 600mg (for BW > 50kg) QD
daily• Clarithromycin 500mg BD daily• Minocycline 100mg BD daily
29 30
Other Mycobacterial Infections
• Drug Treatment – multi-drug therapy, e.g.:– Isoniazid– Pyrazinamide– Rifampicin– Ethambutol (risk of blurred vision, red / green
colour blindness)– Clarithromycin– Minocycline (risk of pigmentation)– Amikacin (risk of vestibular & auditory damage)
• Monitoring of drug compliance and side effects by physiotherapist
31
Mycobacterial Infections
• Monitoring of liver and renal functions, haemotological status (platelet, WBC, RBC counts)
32
Special Infection Cases
• Fungal Infections• Necrotising Fasciitis

33
Fungal Infection• Scedosporium apiospermum infection
34
Fungal Infection
35
Fungal Infection
Management• Multiple surgical debridements + bone
graft + percutaneous K-wire fixation• Prolonged drug treatment –
Itraconazole• Physiotherapy & Occupational Therapy
36
Necrotising Fasciitis• Type I – anaerobic bacteria and
streptococci other than serogroup A• Type II – group A Streptococci• Usually occurred in patients with
chronic debilitating diseases – diabetes, alcohol abuse, or renal insufficiency
(Cheung et al, 2009)

37
Necrotising FasciitisManagement• Prompt diagnosis with radical
debridement amputation• Appropriate antibiotics• Rehabilitation – management of
sequelae
38
Case 1
History• 88 year-old man• Slip & fell with sprained (R) Index
Finger• Consulted bonesetter• Developed swelling & pain for 3-4 days
before admission
39
Case - Preop
40
Case - Preop

41
Case – I & D - Postop D4
C/ST: E. Coli, Streptococci; Bacteroides 42
Case - Physiotherapy
43
Case – Postop D7(Osteolytic change at tuft of distal phalanx)
44
Case – Post-Amputation D1

45
Case – Post-Amputation D20
46
Case – Post-Amputation D29
AROM: (R) IF MPJ: 00-800; PIPJ: 00-500 (700)
Hand Grip: (R) 5kgf; (L) 9kgf
47
Case 2• Infection in an immunocompromised patient
48
Case 2• Infection in an immunocompromised patient

49
Case 2• Infection in an immunocompromised patient
6 weeks later 50
Application ofBoxing Glove Bandaging
51
•Wrist in neutral or slight extension
•MPJ ~ 900
•IPJ ~ 00
•Thumb in palmar abduction
Position of Immobilization
52
Position of Immobilization
MPJs
– Collateral ligaments taut in flexion
- Joint capsule & volar plate loose
(Tubiana et al, 1996)

53
Position of Immobilization
IPJs – Joint capsule & volar plate are tight
(Tubiana et al, 1996)
54
Video on Boxing Glove Bandaging
55
Re-assessment after Application
• Check any subjective discomfort, e.g. too tight, throbbing sensation
• Observe capillary refill of nail bed or pulp
• Feel the resilience of bandaging for even pressure
56
Re-assessment when Boxing Glove Bandaging is removed
• Revise boxing glove bandaging when it is loosened
• Check any local pressure points (especially at PIPJs, wrist)
• Check any reduction in swelling or oedema– Wrinkles or creases
• Check position of finger joints

57
References• Bhambri S, Bhambri A, Del Rosso JQ (2009) Atypical
mycobacterial cutaneous infections. Dermatologic Clinics 27: 63-73.
• Cheung JPY, Fung B, Tang WM, Ip WY (2009) A review of necrotising fasciitis in the extremities. Hong Kong Medical Journal 15: 44-52.
• Cheung JPY, Fung BKK, Ip WY (2010) Mycobacterium marinuminfection of the deep structures of the hand and wrist: 25 years of experience. Hong Kong Medical Journal 15: 211-216.
• Lowe E, Smith , Nolan TP (2005) Mechanical modalities: traction and intermittent pneumatic compression. In: Michlovitz SL, Nolan TP (Eds) Modalities for Therapeutic Interventions, Philadelphia: F.A. Davis, 165-181.
• To MKT, Ho PL, Ip WY (2005) Scedosporium apiospermumcausing septic arthritis of the hand in an immunocompetent patient. Hong Kong Journal of Orthopaedic Surgery 9: 73-78.
• Tubiana R, Thomine J-M, Mackin E (1996) Examination of the Hand and Wrist, 2nd ed, London: Martin Dunitz.