Pharmaco2 asthma
-
Upload
lim-wee-yi -
Category
Documents
-
view
1.041 -
download
5
Transcript of Pharmaco2 asthma

MANAGEMENT A&E

9:30 am
• BP 140/83, HR 87bpm, spO2 95%, T 36.4⁰C
• Generalised rhonchi• Plan– IV HCT 200mg stat given @ 9:35am.– Neb. Combivent– PEFR

10:10am
• Speak in full sentence• PEFR 300L/min, RR 30/min, O2 sat 98%
• Generalized rhonchi • Plan– ABG– CXR– Cont neb

10:26am• VBG?
– pH: 7.377– pCO2: 42.0mmHg– pO2: 30.6mmHg– Base: -0.4 – HCO3: 22.9mmol/L
• WBC: 8.8x109/L• Lymph#: 3.2x109/L• Gran#: 4.8x109/L• Lymph%: 35.8%• Gran%: 54.1%• Hb: 16.5 g/dL• RBC: 5.13x1012/L• HCT: 47%• MCV: 91.8fL• MCH: 32.1pg• MCHC: 35.1 g/dL• Plt: 252x109/L



11:30am• BP 140/83; HR 87bpm; T 37⁰C; spO2 95%↓RA, 98% ↓
NPO2 3L/min• O/E generalized rhochi• Plan – Admit 7S– Cont a/b (h/o admission for similar problem 10 days ago)
• T azithromycin 500mg od• IV claforan 1g tds
– NPO2 3L/min– Neb combivent 4hourly– IV HCT 100mg qid– ABG ↓ RA

11:30am• ABG
– pH 7.498– pCO2: 29.4mmHg– pO2: 147mmHg– HCO3: 25.2mmol/L– Base: -0.3mmol/L
• CXR– Hyperinflated lungs– Bilateral lung hazziness
• Coagulation profile– PT: 13.2s (11.9 – 13.9)– INR: 1.01 (0.86 – 1.14)– aPTT: 40.5s (control 37.9)
• BUSE/creat– Na: 139mmo/L– K: 4.1mmol/L– Creat: 106umol/L– Urea: 2.7mmol/L– Cl: 108mmol/L

MANAGEMENTMedical ward

3:20pm
• Assessment: infective exarcebation COPD– Partially treated pneumonia– Haemodynamically stable– Not in respiratory failure
• Investigations: FBC, BUSE/creat, LFT, aPTT/INR, ESR, ECG, sputum C+S, sputum AFB (D/S x3, C+S)

Plan • Strict I/O, encourage orally• IVD 2Ѳ NS/24hrs• Antibiotic
– IV claforan 2g stat & 1g tds– T azithromycin 500mg stat & OD
• Acute reliever– Neb combivent hourly x2 then 2hourly x2 then 6hourly– Monitor BUSE/creat on neb combivent– PEFR
• Controller– IV HCT 200mg stat & 100mg qid
• Chest physiotherapy• Stop smoking education

11:40pm
• Plan– Refer quit smoking clinic– Increase neb combivent 4hourly– Continue a/b– Continue IV hydrocort– Inhaler technique– MDI becotide 2puffs bd– MDI combivent 2puffs tds

PEFR chartL/min
Time
Day 1 Day 2 day3 day4

DIAGNOSING ASTHMA

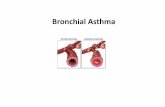
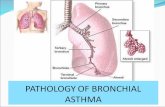
• Asthma is a chronic inflammatory disorder of the airways. Chronically inflamed airways are hyperresponsive; they become obstructed and airflow is limited (by bronchoconstriction, mucus plugs, and increased inflammation) when airways are exposed to various risk factors.

• Symptoms & medical history• Lung function– Spirometry– PEF
• Additional diagnostic tests– Airway responsiveness– Skin tests with allergens or measurement of
specific IgE in serum

MANAGEMENTExacerbations





Prompt tx
• Inhaled rapid-acting β2-agonists in adequate doses are essential. – begin with 2 to 4 puffs every 20 minutes for 1st hour; – then mild exacerbations will require 2 to 4 puffs every 3 to
4 hours, and – moderate exacerbations 6 to 10 puffs every 1 to 2 hours.
• Oral glucocorticoids (0.5 to 1 mg of prednisolone/kg or equivalent during a 24 hr period) introduced early in the course of a moderate or severe attack.
• O2 is given if patient is hypoxemic (achieve O2 saturation of 95%).

Prompt tx
• Combination β2-agonist/anticholinergic therapy is associated with lower hospitalization rates.
• Methylxanthines are not recommended if used in addition to high doses on inhaled β2-agonists.

• Monitor response to tx– Evaluate symptoms, peak flow, O2 saturation
• After exacerbations is resolved– Identify precipitating factors – Implement avoidance strategies– Review pt’s medication

MANAGEMENTWard

• Continue oxygen > 40%• IV HCT 100-200 mg 6 hourly or prednisolone 30-60 mg daily.• Neb β2-agonist 2-4 hourly preferably in combination with
anticholinergic.• If patient is still not improving, commence aminophylline infusion
(0.5-0.9 mg/kg/hour); monitor blood levels if aminophylline infusion is continued for more than 24 hours.
• Terbutaline or salbutamol infusion at 3-20 mcg/min after an initial IV bolus dose of 250 mcg over 10 mins can be given as an alternative.
• In cases where response to the above treatment is inadequate, IV MgSO4 2 g in 50 ml NS infused over 10-20 mins may be given.

Monitoring the response to treatment
• Repeat measurement of PEF 15-30 minutes after starting treatment.
• Aim to maintain arterial oxygen saturation above 92%.• Repeat arterial blood gas measurements if initial
results are abnormal or if patient deteriorate.• Monitor PEF at least 4 times daily throughout the
hospital stay.• Other I(x):– BUSE– ECG if indicated

Transfer pt to ICU or prepare to intubate if there is:
• Deteriorating PEF• Worsening hypoxaemia, or hypercapnia• Exhaustion or feeble respiration• Confusion or drowsiness• Coma or respiratory arrest

MANAGEMENTICU

• Cont O2
• Cont IV HCT• If the patient is mechanically ventilated,
administer neb β2- agonist with anticholinergic via the ETT. This can be given up to every 15-30 min.
• IVI aminophylline or terbutaline or salbutamol should be continued
• IVI MgSO4 may be added.

DISCHARGE PLAN FOR HOSPITALISED PATIENT
• Before discharge, the patient should be:– started on inhaled steroids for at least 48 hours in addition to a short
course of oral prednisolone and bronchodilators– Stable on the medications he is going to take outside the hospital for at
least 24 hours– Having PEF of > 75% of predicted or best value and PEF diurnal variability of
< 20%– Able to use the inhaler correctly and if necessary, alternative inhaler
devices could be prescribed– Educated on the discharge medication, home peak flow monitoring and self– Management plan (for selected, motivated patients), and the importance
of regular follow up– Given an early follow-up appointment within 2-4 weeks for reassessment
of the condition and for adjustment of the medicines

MANAGEMENTChronic asthma

Assessing asthma control

Mx approach based on control (>5 y/o)

Tx steps

Monitoring
• At each visit:– Control– Technique– Compliance & avoiding risk factors– Concerns
• Adjusting medication:– Not controlled → step up, TCA 1/12– Partly controlled → consider step up– Control at least 3 months → step down

CONTROLLERS Medications




RELIEVERMedications




Per inhalation Ipratropium Br monohydrate 21 mcg, salbutamol sulphate 120 mcg
Per UDV Ipratropium Br 0.5 mg, salbutamol sulfate 2.5 mg

• Seretide 50/100 Accuhaler Salmeterol 50 mcg, fluticasone propionate 100 mcg.
• Seretide 50/250 Accuhaler. • Seretide 50/500 Accuhaler
•Seretide 25/50 Evohaler •Seretide 25/125 Evohaler•Seretide 25/250 Evohaler

Per 160/4.5 mcg inhalationBudesonide 160 mcg, formoterol 4.5 mcg

Identify & reduce exposure to risk factors
• Tobacco smoke• Drugs, foods, and additives• Occupational sensitizers• House dust mites• Animals with fur• Cockroaches• Outdoor pollens and mold• Indoor mold