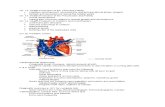
Peds Fluid Mx Dn
Transcript of Peds Fluid Mx Dn
-
8/18/2019 Peds Fluid Mx Dn
1/41
Policy Directive
Department of Health, NSW73 Miller Street North Sydney NSW 2060
Locked Mail Bag 961 North Sydney NSW 2059Telephone (02) 9391 9000 Fax (02) 9391 9101
http://www.health.nsw.gov.au/policies/
spacespace
Children and Infants with Gastroenteritis - Acute Management
space
Document Number PD2010_009
Publication date 03-Feb-2010
Functional Sub group Clinical/ Patient Services - Baby and child
Summary Clinical Practice Guidelines for the treatment of infants and children withgastroenteritis.
Replaces Doc. No. Children and Infants with Gastroenteritis - Acute Management[PD2009_064]
Author Branch Statewide Services Development
Branch contact Trish Boss 9424 5706
Applies to Area Health Services/Chief Executive Governed Statutory HealthCorporation, Board Governed Statutory Health Corporations, AffiliatedHealth Organisations - Non Declared, Affiliated Health Organisations -Declared, Public Health System Support Division, Community Health
Centres, NSW Ambulance Service, Public HospitalsAudience Emergency Departments, Paediatric Units
Distributed to Public Health System, Divisions of General Practice, NSW AmbulanceService, Private Hospitals and Day Procedure Centres, TertiaryEducation Institutes
Review date 03-Feb-2013
Policy Manual Patient Matters
File No. 06/3557
Status Active
Director-GeneralspaceThis Policy Directive may be varied, withdrawn or replaced at any time. Compliance with this directive is mandatory
for NSW Health and is a condition of subsidy for public health organisations.
-
8/18/2019 Peds Fluid Mx Dn
2/41
POLICY STATEMENT
PD2010_009 Issue date: February 2010 Page 1 of 1
INFANTS AND CHILDREN:ACUTE MANAGEMENT OF GASTROENTERITIS
PURPOSE
The infants and children: acute management of gastroenteritis clinical practice guideline(attached) has been developed to provide direction to clinicians and is aimed at achievingthe best possible paediatric care in all parts of the state.
The clinical practice guideline was prepared for the NSW Department of Health by anexpert clinical reference group under the auspice of the state wide Paediatric ClinicalPractice Guideline Steering Group.
MANDATORY REQUIREMENTS
This policy applies to all facilities where paediatric patients are managed. It requires all
Health Services to have local guidelines/protocols based on the attached clinical practiceguideline in place in all hospitals and facilities likely to be required to assess or managechildren with gastroenteritis.
The clinical practice guideline reflects what is currently regarded as a safe andappropriate approach to the acute management of gastroenteritis in infants and children.However, as in any clinical situation there may be factors which cannot be covered by asingle set of guidelines. This document should be used as a guide, rather than as acomplete authoritative statement of procedures to be followed in respect of eachindividual presentation. It does not replace the need for the application of cl inical judgement to each indiv idual presentat ion.
IMPLEMENTATION
Chief Executives must ensure:
Local protocols are developed based on the infants and children: acutemanagement of gastroenteritis clinical practice guideline.
Local protocols are in place in all hospitals and facilities likely to be required toassess or manage paediatric patients with gastroenteritis.
Ensure that all staff treating paediatric patients are educated in the use of thelocally developed paediatric protocols.
Directors of Clinical Governance are required to inform relevant clinical staff treatingpaediatric patients of the revised protocols.
REVISION HISTORY
Version Approved by Amendment notes
December 2004(PD2005_238)
Director-General New policy
October 2009(PD2009_064)
Deputy Director-GeneralPopulation Health
Second edition
February 2010(PD2010_009)
Deputy Director-GeneralPopulation Health
Third edition. Corrects table on page 8.
ATTACHMENT1. Infants and Children: Acute Management of Gastroenteritis – Clinical Practice
Guideline.
-
8/18/2019 Peds Fluid Mx Dn
3/41
Infants and children:
A cute M anagem ent of G astroenteritis
third edition
CLINICAL PRACTICE GUIDELINES
-
8/18/2019 Peds Fluid Mx Dn
4/41
N SW D EPA RTM EN T O F H EA LTH
73 M iller Street
N orth Sydney N SW 2060
Tel. (02) 9391 9000
Fax. (02) 9391 9101
w w w .health.nsw .gov.au
This w ork is copyright. It m ay be reproduced in w hole or part for study or training
purposes subject to the inclusion of an acknow ledgem ent of the source. It m ay not be
reproduced for com m ercial usage or sale. Reproduction for purposes other than those
indicated above requires w ritten perm ission from the N SW D epartm ent of H ealth.
N SW D epartm ent of H ealth 2009
SH PN: (SSD) 090178
ISBN : 978-1-74187-453-2
For further copies of this docum ent please contact:
Better H ealth C entre –Publications W arehouse
PO Box 672
N orth Ryde BC , N SW 2113
Tel. (02) 9887 5450
Fax. (02) 9887 5452
Inform ation Production and D istribution
Tel. (02) 9391 9186
Fax. (02) 9391 9580
E-m ail: bhc@ nsccahs.nsw .gov.au
Further copies of this docum ent can be dow nloaded from the
N SW H ealth w ebsite: w w w .health.nsw .gov.au
A revision of this docum ent is due in 2011.
N ovem ber 2009 - third edition
-
8/18/2019 Peds Fluid Mx Dn
5/41
NSW HEALTH Infa nts and Children — Acute Mana geme nt of Ga stroenteritis PAGE 1
C ontents
Introduction ...............................................................................................3
Summary .....................................................................................................4
Significant C hanges from 2002 C PG Version .........................................................4
Gastroenteritis in Infancy and Childhood ..................................................5
Principles of Fluid M anagem ent .............................................................................6
M edications ...........................................................................................................6
D ifferential D iagnoses ............................................................................................7
Table 1: Clinical A ssessm ent of D ehydration and Initial Treatm ent ..........................8
M anagem ent A lgorithm ........................................................................................9
Enteral Rehydration Therapy ...................................................................10
O ral Rehydration Solutions (O RS) .........................................................................10M ethod of G iving O ral Fluids ...............................................................................12
D ischarge C riteria ..............................................................................................12
Nasogastric Rehydration Therapy ...........................................................13
Intravenous Fluid Therapy .......................................................................15
Introductory N otes ..............................................................................................15
Resuscitation ..............................................................................................15
Rapid IV Rehydration ...........................................................................................16
Standard IV Rehydration ......................................................................................17
H ypernatraem ia ..............................................................................................19
H yponatraem ia ..............................................................................................19
Investigations and Observations .............................................................20
Reintroduction of D iet .........................................................................................21
-
8/18/2019 Peds Fluid Mx Dn
6/41
PAGE 2 NSW HEALTH Infa nts and Children — Acute Mana gemen t of Ga stroente ritis
References ................................................................................................22
Bibliography .............................................................................................24
Appendices .............................................................................................29
A ppendix O ne –Glossary .....................................................................................29
Appendix Tw o –IVT Com position ....................................................................................30
A ppendix Three –Parent O ral Rehydration D ocum entation Form .........................31
A ppendix Four –Parent Inform ation ....................................................................33
A ppendix Five –Resources ...................................................................................34
A ppendix Six –Significant C hanges From 2002 C PG Version ...............................35
A ppendix Seven –A lternative C alculation for M aintenance Fluids ........................35A ppendix Eight –W orking Party M em bers ...........................................................36
-
8/18/2019 Peds Fluid Mx Dn
7/41
NSW HEALTH Infa nts and Children — Acute Mana geme nt of Ga stroenteritis PAGE 3
Introduction
These G uidelines are aim ed at achieving the
best possible paediatric care in all parts of the
State. The docum ent should not be seen as a
stringent set of rules to be applied w ithout
the clinical input and discretion of the
m anaging professionals. Each patient should
be individually evaluated and a decision m ade
as to appropriate m anagem ent in order to
achieve the best clinical outcom e.
The form al definition of clinical practice
guidelines com es from the N ational H ealth
and M edical Research C ouncil:
‘System atically developed statem ents toassist practitioner and patient decisions
about appropriate health care for specific
clinical circum stances.’
(Nat ional Health and Medical Research
Council ‘A Guide to the Development,
implementation and evaluation of
Clinical Practice Guidelines’, Endorsed
16 November 1998, available from
www.nhmrc.gov.au/publications/
synopses/cp30syn.htm)
It should be noted that this docum ent
reflects w hat is currently regarded as a
safe and appropriate approach to care.
H ow ever, as in any clinical situation there
m ay be factors w hich cannot be covered bya single set of guidelines. This docum ent
should be used as a guide, rather than as
a com plete authoritative statem ent of
procedures to be follow ed in respect of each
individual presentation. It does not replace
the need for the application of clinical
judgm ent to each individual presentation.
This docum ent represents basic clinical
practice guidelines for the acute
m anagem ent of gastroenteritis in children
and infants. Further inform ation m ay be
required in practice; suitable w idely available
resources are included as Appendix Five.
Each A rea H ealth Service is responsible forensuring that local protocols based on these
guidelines are developed. A rea H ealth
Services are also responsible for ensuring
that all staff treating paediatric patients are
educated in the use of the locally developed
paediatric guidelines and protocols.
In the interests of patient care it is critical
that contem poraneous, accurate and
com plete docum entation is m aintained
during the course of patient m anagem ent
from arrival to discharge.
Parental anxiety should not be
discounted: it is often of significance
even if the child does not appear
especially unwell.
-
8/18/2019 Peds Fluid Mx Dn
8/41
PAGE 4 NSW HEALTH Infa nts and Children — Acute Mana gemen t of Ga stroente ritis
Sum m ary
G astroenteritis is a com m on paediatric
condition. A ppropriate m anagem ent
attem pts to avoid dehydration, but w hen
this occurs appropriate fluid m anagem ent
is essential.For rehydration the enteral
route is preferred, but if intravenous
fluids are used then low sodiumcontaining fluids m ust be avoided. For
intravenous rehydration 0.9% N orm al
Saline (N aC l) + 2.5% G lucose is preferred.
0.9% N orm al Saline (N aC l) + 5% G lucose
m ay also be used. If rehydrating over 24
hours then 0.45% N aC l + 2.5% G lucose is
an acceptable alternative. O ral rehydration
solutions m ay be offered orally oradm inistered nasogastrically.
In cases of severe dehydration or clinical
deterioration after adm ission or despite
treatm ent, the A dm itting M edical O fficer
in charge or consulting paediatrician
should be notified and should personally
review the patient as soon as possible. W hereother m edical staff act as a delegate for
the A dm itting M edical O fficer, the hospital
m ust have clear w ritten protocols defining
this arrangem ent.
For hospitals em ploying junior m edical staff:
The Admitting Medical Officer MUST be
notified within an hour of the decision
to admit the child. Details of the physical
findings and proposed fluid therapy should
be discussed. Hospitals should have an
internal policy that defines roles if senior
registrars act as a delegate for the A M O .
These C linical Practice G uidelines should
be read in conjunction w ith other relevant
C linical Practice G uidelines (e.g. the
Recognit ion of a Sick Child in Emergency
Departments , and Acute Management of
Infants and Children with Acute Abdom inal
Pain ). W hen dealing w ith children
suspected of having gastroenteritis,it is
essential that infection control
measures be implemented to prevent
cross-contam ination and spread.
-
8/18/2019 Peds Fluid Mx Dn
9/41
NSW HEALTH Infa nts and Children — Acute Mana geme nt of Ga stroenteritis PAGE 5
G astroenteritis in Infancy
and C hildhood
This com m on acute intestinal
com m unicable infection causes
vom iting, diarrhoea and fever. It is
usually viral, but som etim es bacterial
or parasitic. C om m unity outbreaks are
sporadic and seasonal.
A sm all proportion of those affected
w ill suffer severe dehydration and
electrolyte disturbance. U ntreated or
poorly treated dehydration m ay
progress to shock and death. There are
also risks from over-hydration and/or
inappropriate electrolyte replacem ent,
including death from cerebral oedem a.
Som e other serious illnesses are
som etim es incorrectly diagnosed as
gastroenteritis.Warning signs of
other diagnoses must be recognised
and investigated(see page 7).
Suggested hospital requirements
for management of children withgastroenteritis
24-hour availability of nurses and
m edical practitioners experienced in
the m anagem ent of sick children.
A ccess to 24-hour standard
biochem istry for inpatient
m anagem ent. This m ay include point
of care testing.
A vailability of standard resuscitation
intravenous fluids, including 0.9%
N aC l (w ithout added glucose) or
H artm ann’s solution (w ithout added
glucose).
A vailability of rehydration intravenous
fluids, including 0.9% N aC l + 2.5%
G lucose, 0.45% N aCl + 2.5% G lucose.
Intravenous paediatric giving sets w ith
burettes, appropriate infusion pum ps.
A ppropriate O ral Rehydration Solutions
such as G astrolyte® , G astrolyte-R® ,
Repalyte® , H ydralyte®
A ppropriate giving sets and enteralinfusion pum ps (e.g. Kangaroo® pum p).
Availability of assistance when
treating severely ill children
The treatm ent of children w ith severe
dehydration should be discussed w ith
a paediatrician and consideration be
given to transfer to a facility w ith a
paediatric intensive care unit.
For advice regarding the m anagem ent
of seriously ill children or to arrange
their transfer to any of the children’s
hospitals contact N SW N ew born and
Paediatric Em ergency Transport Service
(NETS) Hotline number:1300 36 2500.
-
8/18/2019 Peds Fluid Mx Dn
10/41
PAGE 6 NSW HEALTH Infa nts and Children — Acute Mana gemen t of Ga stroente ritis
C alls to N ETS are voice recorded and
form part of the N ETS m edical record
for the patient.
Principles of FluidManagement
Infants and children w ith gastro-
enteritis require additional fluids to
prevent dehydration, or for
rehydration.
The enteral route is preferred for
rehydration of children w ith m ild or
m oderate dehydration. This is w ith anO ral Rehydration Solution (O RS) either by
m outh or via nasogastric tube.
Suitable fluids should be offered, for
oral rehydration
– Babies w ho are breastfed should
receive sm all frequent breastfeeds
to ensure norm al urine output. This
m ay be supplem ented w ith an O RS.
– For all other children, offer an
O RS. Those requiring m ixing m ust
follow the m anufacturer’s
instructions.Do not add flavouring
or sweet drinks to an ORS.
– If an O RS is unavailable, or refused,
dilute juice/lem onade (m ixed as 1part juice/lem onade w ith 4 parts
w ater) can be used only if a child
is not dehydrated.These are less
desirable fluid opt ions .
– Do not use ‘sports drinks’as they
are not an appropriate rehydration
fluid for children w ith gastroenteritis.
– Do not use low -calorie or diet drinks.
Suitable volum es should be offered: try
to give about 0.5m L/kg every 5 m inutes.
A chieving successful oral rehydration
dem ands constant attention and
persistence, usually by parents.
The principles and practice of oral
replacem ent therapy are described on
page 10.
Intravenous rehydration is often a
reasonable alternative for m oderate
dehydration (see Table 1 on page 8)
and is essential w here severe
dehydration and/or shock are present. C hildren receiving fluid rehydration
require regular tim ely reassessm ent.
The principles and practice of
intravenous replacem ent therapy are
described on page 15.
NB: Careful calculations of fluid
volume and rate are requiredregardless of route of administration.
Medications
There are no indications for using
anti-m otility or anti-diarrhoeal agents in
the m anagem ent of acute gastroenteritis
in infants or children.
M any antiem etic m edications have a risk
of significant side effects, like dystonic
reactions and sedation, and should be
avoided [e.g. prom ethazine,
prochlorperazine]. M edications such as
5H T-3 receptor antagonists, such as
ondansetron, m ay have som e clinical
benefit, how ever the evidence is notconclusive. Experienced clinicians choosing
-
8/18/2019 Peds Fluid Mx Dn
11/41
NSW HEALTH Infa nts and Children — Acute Mana geme nt of Ga stroenteritis PAGE 7
to use that m edication generally should
lim it the use to a single dose.
Pro-biotics and Zinc m ay have som e
clinical benefits in the m anagem ent of
gastroenteritis, and m ay be available in
som e com m ercially available products such
as yoghurts. These can be given to children
w hen a norm al diet is reintroduced.
A ntibiotics are rarely required in
gastroenteritis, even w hen bacterial in
aetiology. If unsure, consult a paediatrician
or paediatric infectious disease specialist.
Rotavirus vaccines are available and have a
significant benefit in the prevention of
gastroenteritis in young infants. A dditional
inform ation is available at the N ational
C entre for Im m unisation Research and
Surveillance of Vaccine Preventable
D iseases w ebsite
ht t p://w w w .ncirs.usyd.e d u.a u/fa cts/rotavirus_vaccine_for_children_
june_2007.pdf
Differential Diagnoses
A lw ays keep in m ind the possibility that
the diagnosis of gastroenteritis could be
incorrect.Gastroenterit is consists of the
tr iad of vomit ing, diarrhoea and fever. Be
cautious of evaluating the child w ith
vom iting alone. The follow ing list is not
exclusive. C onsider also:
A cute appendicitis
Strangulated hernia
Intussusception or other causes of
bow el obstruction
U rinary tract infection
M eningitis and other types of sepsis
A ny cause of raised intracranial
pressure
D iabetic ketoacidosisInborn errors of m etabolism
Inflam m atory bow el disease
H aem olytic uraem ic syndrom e
A lw ays consider another diagnosis if
there is:
A bdom inal distension Bile-stained vom iting
Fever >39ºC
Blood in vom itus or stool
Severe abdom inal pain
Vom iting in the absence of diarrhoea
H eadache
Beware! The very young infant and
the malnourished child are more likely
to suffer severe disease, or to have
another diagnosis.
Table 1 on page 8 gives an overview of
dehydration definition, signs and sym ptom s,
along w ith initial enteral or parenteral fluid
therapy. W herever 0.9% N aCl + 2.5%
G lucose is advised, 0.9% N aC l + 5%
G lucose w ould be an acceptable alternative.
The flow chart on page 9 outlines a
treatm ent overview and highlights decision
points in regard to the initial m anagem ent
of an infant or child w ith gastroenteritis.
-
8/18/2019 Peds Fluid Mx Dn
12/41
PAGE 8 NSW HEALTH Infa nts and Children — Acute Mana gemen t of Ga stroente ritis
T a b l e 1
: C l i n i c a l A s s e s s m e n t o f D e h y d r a t i o n a n d I n i t i a l T r e
a t m e n t
N o s i n g
l e s y m p
t o m o r c l
i n i c a
l s i g n r e
l i a b l y p r e
d i c t s t h e
d e g r e e
o f d e
h y d r a
t i o n
D e s c r
i p t i o n o f
d e h y d
r a t i o n
D e h y d r a t i o n
( % o
f B o d y
W e i g h t )
S
i g n s a n d S y m p t o m s
R e p l a c e m e n t
F l u i d R o u t e
R e p
l a c e m e n t F l u i d T y p e
N o
C l i n i c a
l
S i g n s o
f
D e
h y d
r a t i o n
R
e d u c e
d u r i n e o u
t p u
t
T
h i r s t
N
o p
h y s
i c a
l s i g n s
O r a
l
I n o
r d e r o
f p r e
f e r e n c e
1 . F r e q u e n
t b r e a s t
f e e
d s w
h e r e a p
p r o p r i a
t e / p o s s
i b l e
2 . O r a
l R e
h y d r a
t i o n
S o
l u t i o n
( s e e p a g e
1 0 )
3 . 1 / 5 s t r e n g
t h c l e a r
f l u
i d s
i . e . : 4
p a r t s w a
t e r a n
d 1
p a r t
j u i c e
/ l e m o n a
d e ( i f a n
O R
S r e f u s e d )
M i l d
3 %
R
e d u c e
d u r i n e o u
t p u
t
T
h i r s t
D
r y m u c o u s m e m
b r a n e s
M
i l d T a c h y c a r d
i a
O r a
l
I n o
r d e r o
f p r e
f e r e n c e
1 . F r e q u e n
t b r e a s t
f e e
d s w
h e r e p o
s s i b l e / a p p r o p r i a
t e
m a y
b e s u p p
l e m e n
t e d w
i t h a n
O R S
2 . O r a
l R e
h y d r a
t i o n
S o
l u t i o n
( s e e p a g e
1 0 )
N a s o g a s t r i c
O r a l R e
h y d r a
t i o n
S o
l u t i o n e . g .
G a s t r o
l y t e ® ( s e e p .
1 0 )
I n t r a v e n o u s
– R a p
i d
– S t a n
d a r d
0 . 9 %
N a
C l + 2 . 5
% G
l u c o s e
0 . 9 %
N a
C l + 2 . 5
% G
l u c o s e o r 0
. 4 5 %
N a
C l +
2 . 5 %
G l u c o s e
M o
d e r a
t e
5 %
D
r y m u c o u s m e m
b r a n e s
T
a c h y c a r d
i a
A
b n o r m a
l r e s p
i r a
t o r y p a
t t e r n
L
e t h a r g y
R
e d u c e
d s k
i n t u r g o r
S
u n
k e n e y e s
N a s o g a s t r i c
1 . O r a
l R e
h y d r a
t i o n
S o
l u t i o n e . g
. G a s t r o
l y t e ®
( s e e p a g e
1 0 )
I n t r a v e n o u s
– R a p
i d
– S t a n
d a r d
0 . 9 %
N a
C l + 2 . 5
% G
l u c o s e
0 . 9 %
N a
C l + 2 . 5
% G
l u c o s e o r 0
. 4 5 %
N a
C l +
2 . 5 %
G l u c o s e
S e v e r e
1 0 %
A
b o v e s i g n s
P
o o r
P e r f u s i o n
: M o
t t l e d , c o o l
l i m b s /
S l o w c a p
i l l a r y r e
f i l l / A l t e r e
d
c
o n s c
i o u s n e s s
S
h o c k
: t h r e a
d y p e r i p
h e r a
l p u l s e s
w
i t h m a r k e
d t a c h y c a r d
i a a n d
o t h e r
s
i g n s
o f p o o r p e r f u s i o n s t a t e d a
b o v e
I n t r a v e n o u s o r
i n t r a o s s e o u s
2 0 m
L / k g s t a
t
a n
d r e a s s e s s
f l u
i d n e e
d s
U s e
e i t h e r :
0 . 9 %
N a
C l o r
H a r t m a n n
’ s s o
l u t i o
n f o r
r e s u
s c i t a
t i o n a n
d t h e n r e a s s e s s t
h e c h
i l d .
O n g
o i n g
f l u
i d r e p
l a c e m e n
t s h o u
l d b e w
i t h
e i t h
e r :
0 . 9
% N
a C l + 2 . 5
% G
l u c o
s e o r
0 . 4 5 %
N a
C l + 2 . 5
% G
l u c o s e
-
8/18/2019 Peds Fluid Mx Dn
13/41
NSW HEALTH Infa nts and Children — Acute Mana geme nt of Ga stroenteritis PAGE 9
Management Algorithm
H istory and exam ination results in provisional diagnosis of gastroenteritis. C linical assessm ent of
degree of dehydration (see table on page 8). If no sign of dehydration, continue frequent sm all
volum es of oral fluids increasing volum e and reducing frequency as fluids are tolerated.
Mild dehydration
O ffer frequent, sm all volum es
O RS (achieving about
0.5m L/kg every 5 m inutes).
Moderate dehydrationC hild not shocked
Severe dehydration
C hild shocked
Reassess frequent ly
Tolerating oral fluids and
clinical/fam ily status
satisfactory:
•Educate fam ily & provide
Fact Sheet.
•Discharge hom e.
•A dvise about planned
m edical follow -up and need
for earlier review .
Not tolerating oral fluids:
•Continue to encourage oral
fluids.
•Adm it to hospital if
dehydration progressing and oral intake is inadequate.
•C onsider nasogastric
rehydration or intravenous
rehydration.
•Consider the need for EU C .
4 options
1. “Aggressive” and diligentoral rehydration.
2. Rapid NG rehydration:Ensure the nasogastric tubeis inserted in the stom ach, e.g. aspirating fluid and testingacid by pH tape. C om m enceG astrolyte® via an enteralinfusion pum p e.g. Kangaroo® at 10m L/kg/hr for 4 hours.
3. Rapid IV rehydration: TakeEUC , check BG L. C om m ence10m L/kg/hr for 4 hours using 0.9% N aCl + 2.5% G lucose.
4. Standard IV rehydration:Take EU C , check BG L.C om m ence 0.9% N aC l +2.5% G lucose or 0.45%N aCl + 2.5% G lucose.
If contemplating IV rehydra-tion and there is difficultygaining vascular accesscommence oral/nasogastricrehydration.
O r if:
•D eteriorating clinical status
•W orrying signs/sym ptom s (see page 8)
Seek urgent medical advice/review.
Further consultation may be necessary.
Local hospital policy should define theappropriate consultation m echanism .
C om m ence/continue oral intake.
It is expected that the clinical status of an infant or child who is receiving rehydration therapy
for gastroenteritis should gradually improve.
Reassess clinically and consider EU C w ithin 6–8 hours.
•G ive oxygen until signs ofshock are reversed.
•G ain vascular accessurgently.
•If IV difficult, use theintraosseous route.
•Take EU C , BG L (if possible)but do not delay in givingbolus of 20m L/kg 0.9%N aC l or H artm anns stat.
•Reassess for signs of shock.
•Repeat bolus if necessaryuntil signs of shock arereversed.
•Reassess hydration status.Based on this assessm entadm inister IV fluidreplacem ent over 24 hours.Reassess fluid balancefrequently.
•M onitor continuously andclinically reassessfrequently.
Requires admission to hospital
for prompt management
and constant supervision
N O T IM PRO VIN G IM PRO VIN G
-
8/18/2019 Peds Fluid Mx Dn
14/41
PAGE 10 NSW HEALTH Infa nts and Children — Acute Mana gemen t of Ga stroent eritis
M ost children w ith gastroenteritis and
m ild- m oderate dehydration can be
successfully rehydrated w ith oral
rehydration solutions either by m outh or
nasogastric tube.
Oral Rehydration SolutionsO ral rehydration solutions (O RS) are
specifically designed fluids that contain an
appropriate am ount of sodium , glucose
and other electrolytes and are of the
appropriate osm olality, to m axim ise w ater
absorption from the gut. They use the
principle of glucose-facilitated sodium
transport w hereby glucose enhancessodium and secondarily w ater transport
across the m ucosa of the upper intestine.
The sodium and glucose concentrations
and the osm olality are of vital im portance.
The W orld H ealth O rganisation (W H O )
recom m ends an O RS that has a sodium
concentration of 90m m ol/L. In developedcountries w ith non-cholera diarrhoea, it is
generally thought that 90m m ol/L is a little
high, as non-cholera gastroenteritis does
not result in the sam e sodium losses that
are seen in cholera.
M any different O RS w ith varying sodium
concentrations have been developed. It
has been show n that w ater absorption
across the lum en of the hum an intestine is
m axim al using solutions w ith a sodium
concentration of 60m m ol/L1 (such as
G astrolyte® ) and this is the concentration
recom m ended by the European Society of
Paediatric G astro-enterology and
N utrition.2 H ow ever som e children w ho
are not particularly dehydrated w ill refuseto drink such an O RS because of its salty
taste. O RS w ith slightly less sodium such
as Hydralyte® m ay be m ore palatable,
particularly as this com es in an iceblock
form .
O RS w ith sim ilar com positions to
H ydralyte® are safe and effective. These
hypo-osm olar solutions (such as
G astrolyte® and H ydralyte® ) are m ore
effective at prom oting w ater absorption
than isotonic or hypertonic solutions.3,4,5
The com position of various O RS and other
fluids is show n in Tables 2 and 3. Fruit
juices and soft drinks are inappropriate
because of the m inim al sodium contentand the excessive glucose content and
hence excessive osm olality, w hich w ill
w orsen diarrhoea. A lthough diluting juices
and soft drinks reduces glucose
concentration, the fluid has insufficient
sodium to act as a rehydration fluid.
Sports drinks have varying sodium andcarbohydrate levels, and are considered
inappropriate as rehydration solutions.
Enteral Rehydration Therapy
-
8/18/2019 Peds Fluid Mx Dn
15/41
NSW HEALTH Infa nts and Children — Acute Mana gemen t of Ga stroent eritis PAGE 11
Table 3: Composition of Oral Fluids
Comparisons of Oral Fluids
N a+ C arbohydrate O sm olality(m m ol/L) (m m ol/L) (m O sm /L)
A pple Juice 3 690 730
Soft drinks ~2 ~700 ~750
Sports drinks ~20 ~255 ~330
Table 2: Composit ion of Oral Rehydration Solutions
Comparisons of ORS
N a C arbohydrate O sm olality(m m ol/L) (m m ol/L) (% ) (m O sm /L)
W H O 90 G 111 (2% ) 331
G astrolyte® 60 G 90 (2% ) 240
G astrolyte-R® 60 RSS 6g/L (2.5% ) 226
Repalyte® 60 G 90 (2% ) 240
Terry W hite/C hem -m art® 60 G 90 (2% ) 240
H ydralyte® 45 G 90 (2.5% ) 240
G = glucose, RSS = rice syrup solids
-
8/18/2019 Peds Fluid Mx Dn
16/41
PAGE 12 NSW HEALTH Infa nts and Children — Acute Mana gemen t of Ga stroent eritis
Discharge Criteria
C hildren w ith gastroenteritis can be dis-
charged, even if they still have som e
vom iting, if the follow ing discharge criteria
are m et:
1. D iagnosis of gastroenteritis
2. C hild is rehydrated or only m ildly
dehydrated
3. G astrointestinal losses not profuse
4. C hild has passed urine in ED or w ithin
the last 4 hours
5. Parent has dem onstrated the ability togive an O RS appropriately
6. C linical staff confident parent w ill take
child to G P for review w ithin 48hrs
and represent for m edical review if
child’s condition deteriorates.
7. If a child w ith gastroenteritis and
dehydration does not fulfil the
discharge criteria, they w ill need to be
adm itted for ongoing m anagem ent.
Method of Giving Oral Fluids
It is im portant to give sm all am ounts of
fluid frequently, for exam ple 0.5m L/kg
every five m inutes. The fluid can be
m easured in a syringe and given to the
child either by syringe, teaspoon or cup.The child is far m ore likely to tolerate
these sm all am ounts of fluid than if he/she
drinks a large am ount at once.
O bviously if the child tolerates this fluid
the parent can gradually increase the
volum e and decrease the frequency of the
fluid offered. Success can be optim ised in
the Em ergency D epartm ent setting by
giving the parents a docum entation chart
(see A ppendix 3) to record the fluid given
and any vom its, diarrhoea or urine passed.
It is im portant to educate the parents that
seeing a doctor w ill not cure their child of
his/her vom iting and diarrhoea. Sm all,
frequent am ounts of fluid w ill hopefully
m inim ise the vom iting, but w ill not reduce
the diarrhoea. The aim is for the input to
exceed the output by enough to rehydrate
and then m aintain hydration.
Occasional vomiting alone should not
be considered as failure of oral
rehydration therapy.
-
8/18/2019 Peds Fluid Mx Dn
17/41
NSW HEALTH Infa nts and Children — Acute Mana gemen t of Ga stroent eritis PAGE 13
Increasing num bers of hospitals in
developed countries are using an O RS via
continuous nasogastric (N G ) infusion.8,9
This has been show n to be as effective as
intravenous rehydration,8-15 less
expensive8,15 and reduces lengths of
hospital stay8 w hen com pared w ithstandard intravenous rehydration. It is
usually unnecessary to perform EU C for
children being rehydrated w ith nasogastric
O RS.
N asogastric rehydration is w here an O RS is
infused continuously via a nasogastric tube
w ith a pum p such as a Kangaroo® pum p.
Choose an ORS with a sod ium
concentration of 60mmol/L such as
Gastrolyte®, as this is the optimal
concentration and taste is not an issue
when using an NG tube. H ydralyte® has
only 45 m m ol/L of sodium , and is not the
preferred nasogastric solution (but w hen
given orally often has better com pliance
due to taste). N asogastric rehydration is
often successful even in children w ith
frequent vom iting. Staff need to be
com petent in placing nasogastric tubes in
children and babies and follow local
protocols and training/accreditation
procedures. Facilities need to be equipped
to deliver N G rehydration in regards to
equipm ent and education before this form
of rehydration should be introduced.
Do not use nasogastric rehydration if
the child has:
an ileus (check for bow el sounds)
significantly reduced level of
consciousness
Do not use ‘rapid’ nasogastric
rehydration if child:
is younger than 6 m onths old
has a m edical condition w hich
increases the risk of fluid overload
D ifferent regim ens are used for
continuous nasogastric rehydration. O ne
sim ple m ethod is described below :
Perform observations –tem perature
(T), pulse (P), respiratory rate (R), blood
pressure (BP) and m ental state –before
com m encing, then repeat T, P, and R
at least hourly.
Establish N G access
G ive 10m L/kg/hour of G astrolyte®
over four hours for all m ild-m oderately
dehydrated children,after which the
infusion is ceased.
D o not take blood for EU C and BG L as
a routine.
A fter com pletion, the child is then
re-exam ined by the m edical officer and
a re-trial of oral fluids is com m enced.
N asogastric Rehydration Therapy
-
8/18/2019 Peds Fluid Mx Dn
18/41
PAGE 14 NSW HEALTH Infa nts and Children — Acute Mana gemen t of Ga stroent eritis
A fter 1–2 hours of com pleting rehydration
the child is reassessed and if he/she fulfils
the discharge criteria (page 12), m ay be
discharged w ith appropriate advice and
follow -up.
If the child does not tolerate N G
rehydration, (N B: 1 or 2 sm all vom its does
not necessarily m ean N G rehydration has
failed), IV rehydration w ill probably need
to be com m enced.This should be over
24 hours i.e. do not give rapid IV
rehydration after the child has already
received ‘rapid’ NG rehydration (see
page 16 for calculation).
Som e clinicians m ay choose to use a low er
N G infusion rate, either initially or over a
longer period of tim e; sim ilar to the
standard IV rehydration rate (see page 17).
If the child tolerated the N G rehydration
but fails the subsequent trial of oral fluids,the child w ill usually need to stay in
hospital. If further fluid in addition to that
taken orally is required after reassessm ent,
this can be given via the nasogastric tube.
A second administration of ‘rapid’ NG
rehydration should not be given (see
page 18 for calculation). A t this point,
EU C and BG L should be checked to ensure
that an electrolyte abnorm ality is not the
cause for failure of rehydration.
N G rehydration is m ost suitable for infants
and young children. From a practical
view point, older children w ould be m ore
suitable to be rehydrated orally or
intravenously.
-
8/18/2019 Peds Fluid Mx Dn
19/41
NSW HEALTH Infa nts and Children — Acute Mana gemen t of Ga stroent eritis PAGE 15
Introductory notes
W hen IV fluid therapy is com m enced,
the first decision is w hether the child is
severely dehydrated and needs
resuscitation (see below ).
W hen resuscitation fluid (a bolus) hasbeen given for shock, and the signs of
shock corrected, then the next phase of
treatm ent is to provide standard IV
rehydration.
If a bolus has not been needed, the
next phase of treatm ent is to provide
either rapid IV rehydration or standard
IV rehydration.
In this G uideline, 0.9% N aC l + 2.5%
G lucose is considered to be an isotonic
solution, as the glucose is rapidly
m etabolised after infusion.
W henever an IV cannula is inserted for
the provision of IV fluids, blood should
be w ithdraw n and sent for EU C andBG L.
C hildren w ith gastroenteritis and
dehydration are at risk of
hypoglycaem ia; any fluid used for
rehydration should contain som e
glucose. For hypoglycaem ic children
(i.e. BG L
-
8/18/2019 Peds Fluid Mx Dn
20/41
PAGE 16 NSW HEALTH Infa nts and Children — Acute Mana gemen t of Ga stroent eritis
established. If neither is possible
com m ence nasogastric rehydration
w hile aw aiting assistance. These
adm inistration routes do not negate
the need for an IV line.
0.9% N aC l or H artm ann’s solution, 20m L/kg, should be given IV/IO initially
over 10–20 m inutes. These fluids
should N O T contain G lucose.
For hypoglycaem ic children (i.e. BG L
-
8/18/2019 Peds Fluid Mx Dn
21/41
NSW HEALTH Infa nts and Children — Acute Mana gemen t of Ga stroent eritis PAGE 17
Sm all am ounts of oral fluids m ay be
com m enced earlier, during IV
rehydration, if appropriate. Intravenous
fluids should only be recom m enced if
on review the child still has signs of
dehydration, or if there are significant
ongoing losses.
If the rapid rehydration has been
com pleted late at night, and the child
has no signs of dehydration, the child
m ay safely be allow ed to sleep w ith
the IV capped, w ith a trial of oral fluids
to com m ence w hen the child w akes.
It is expected that the clinical status
(e.g. heart rate, perfusion and m ental
state) of the child receiving rapid IV
rehydration for gastroenteritis should
gradually im prove. Failure to im prove,
any deterioration, or the developm ent
of unexpected signs or sym ptom s
should lead to a reconsideration of the
diagnosis and m anagem ent, and
discussion w ith a Paediatrician.
Standard IV Rehydration
Standard rehydration refers to the
provision of m aintenance fluids, and
the correction of dehydration, usually
over 24 hours.
W hen the IV cannula is inserted, sendblood for EUC and BG L.
It is acceptable to com m ence fluid
therapy w ith either 0.9% N aC l + 2.5%
G lucose or 0.45% N aCl + 2.5%
G lucose for standard IV rehydration,
pending EUC results. 0.9% N aCl + 5%
G lucose and 0.45% N aC l + 5%
G lucose are acceptable alternatives.
Calculate the total volum e of IV fluids
likely to be needed for the next 24
hours, being m aintenance and deficit.
Do not include fluids already given for
resuscitation. If resuscitation has been
required, reassess dehydration state
now and calculate fluid requirem ent
from now . N ote that this calculation is
a ‘starting point’w hich w ill be review ed
according to progress, including
assessm ent of general appearance,
heart rate, urine output, ongoing losses
(vom iting, diarrhoea), or fever, at
intervals of not m ore than 6 hours.
Body Weight Fluid requirement mL/ day Fluid requirement mL/ hour
First 10 kg 100 m L/kg 4 m L/kg/hr
Second 10 kg + 50 m L/kg + 2 m L/kg/hr
Subsequent kg + 20 m L/kg + 1 m L/kg/hr
-
8/18/2019 Peds Fluid Mx Dn
22/41
PAGE 18 NSW HEALTH Infa nts and Children — Acute Mana gemen t of Ga stroent eritis
The m ajority of children w ill not
require rehydration for m ore than a
5% deficit in the first 24 hours.
The volum es for rehydration and
m aintenance are calculated separately,
as the basis for calculation of each isdifferent.
For rehydration: W eight (in kg) X %
dehydration X 10 = m L deficit needed
for rehydration. For exam ple, a 9 kg
child estim ated to be 5% dehydrated,
rehydration volum e is 9 X 5 X 10 =
450 m L. (see Table 1 on page 8 for a
guide to assessing dehydration)
For maintenance: C alculate volum e
according to the child’s w eight, as in
the table (page 17):
For exam ple: A child w eighing 25 kg
has a m aintenance fluid requirem ent
for 24 hours of:
(10 X 100) + (10 X 50) + (5 X 20) =
1600 m L per 24 hours.
N ote:
– M aintenance fluids for infants less
than 6–9 m onths is 120m L/kg
– There are alternative m ethods for
calculating m aintenance fluid
requirem ents (see A ppendix 7 for
an exam ple).
A dd the tw o volum es (rehydration +
m aintenance) together. C alculate the
rate to give the total volum e over 24
hours. Start by giving 0.9% N aC l +
2.5% G lucose or 0.45% N aCl + 2.5%
G lucose over the first 6-8 hours, then
review the child’s progress.
DO NOT USE LOW SODIUM-
CONTAINING FLUIDS (any fluid w ith
less sodium than 0.45% N aC l)FOR
ONGOING TREATMENT.
Form al review by a M edical O fficer
after 6–8 hours is generally required.C heck hydration. C heck patient
physically, including m ental state.
Take note of parental observations or
concerns.
There is som e em erging evidence that
0.9% N aC l + 2.5% G lucose solution
m ay be a m ore appropriate IV solutionfor rehydration in gastroenteritis16.
Rapid im provem ent over 2–4 hours is
the ‘norm ’. O nset of any new sym ptom s
(e.g. drow siness, headache, abdom inal
pain) dem and urgent review . A typical
behaviour of the patient should raise
the question of an alternate diagnosis.
Repeat EU C if the child still appears
unw ell, if the electrolytes w ere
m arkedly abnorm al initially, or if the
child w as seriously unw ell initially.
Repeat EU C should also be planned for
the child w ho continues on IV fluids.
A dd potassium ~3 m m ol/kg/24hrs
w hen urine is passed, if initial serumpotassium w as norm al (up to 5 m m ol/
kg/24hrs if m arked hypokalaem ia is
present). G enerally this is achieved by
adding 10 m m ol of potassium as KC l
to each 500 m L bag of IV fluid.
-
8/18/2019 Peds Fluid Mx Dn
23/41
NSW HEALTH Infa nts and Children — Acute Mana gemen t of Ga stroent eritis PAGE 19
Hypernatraemia (serum sod ium>149 mmol/L)
Do not follow the Acute Gastroenteritis
Guideline for fluid administration.
Early consultation with a Paediatrician
is essential.
H ypernatraem ic dehydration is uncom m on,
but potentially m ore dangerous than w hen
serum sodium is initially norm al or slightly
low . There is a greater likelihood of cerebral
oedem a, seizures and brain dam age.
C linically, the degree of dehydration m ay
be underestim ated.
If shock is present, resuscitate w ith a fluid
bolus of 20 m L/kg, using 0.9% N aC l or
H artm ann’s solution.
C ontinuing rehydration should proceed
slow ly (usually over at least 48 hours),
initially using 0.9% N aC l + 2.5% G lucose.
Hyponatraemia (serum sodium
-
8/18/2019 Peds Fluid Mx Dn
24/41
PAGE 20 NSW HEALTH Infa nts and Children — Acute Mana gemen t of Ga stroent eritis
G enerally, children being enterally
rehydrated do not require blood tests.
If nasogastric rehydration is required
beyond 4 hours of rapid nasogastric
rehydration, check EU C and BG L.
M edical reassessm ent of the patient,
including hydration status, is required.
A ll children w ith severe dehydration or
w ith intravenous therapy, need EU C ,
BG L.
C onsider blood culture and FBC if the
child has a tem perature >39ºC .
G enerally urine culture is not required
but urinalysis is helpful.
It is generally unnecessary to send
stool for M C & S or viral studies. In
som e circum stances (e.g. bloody
diarrhoea, history of travel, and
com m unity outbreak of gastroenteritis)
it m ay be appropriate to undertake
these tests.
Infants and children w ho are severely
dehydrated require constant
observation and m onitoring, including,
w here possible, cardiac m onitoring,
pulse oxim etry, frequent blood
pressure m easurem ent and urine
output m easurem ent.
Every child being treated in hospital for
gastroenteritis, w hether or not having
intravenous therapy, requires
observation of, and recording of,
standard observations (e.g. pulse,
respiration, tem perature etc.) on a
regular basis (not less than 4-hourly).
C hildren needing IV fluid therapy
require EU C and BG L check at initial
assessm ent. If initial EU C w as m arkedly
abnorm al, or if the child’s condition
has not started to im prove, or if the
child w as severely dehydrated recheck
EU C at 6–8 hours. Results should be
checked w ithin tw o hours.
If there is failure to im prove,
deterioration or developm ent of new
signs, there should be discussion w ith
the A dm itting M edical O fficer.
A daily lightly clothed w eight can be a
useful clinical param eter in the
assessm ent of progress afteradm ission, as w ell as a retrospective
guide to the accuracy of the initial
assessm ent of dehydration.
Investigations and O bservations
-
8/18/2019 Peds Fluid Mx Dn
25/41
NSW HEALTH Infa nts and Children — Acute Mana gemen t of Ga stroent eritis PAGE 21
Reintroduction of Diet
C hildren w ho are not dehydrated should
continue to be fed an age-appropriate
diet. C hildren w ho require rehydration
should recom m ence age appropriate diets
as soon as vom iting settles. This should bew ithin the first 12–24 hours. Form ula-fed
infants should recom m ence full strength
form ula.
Refer to G astroenteritis fact sheet jointly
developed by the C hildren’s Hospital
W estm ead, the Sydney C hildren’s H ospital
and the John H unter C hildren’s H ospital.The fact sheet is available at:
w w w .chw .edu.a u/pa rents/fa ctsheets
w w w .sch.edu .a u/he a lth /fa ctshe et s
w w w .ka leidoscope .org.a u/pa rents/
factsheets .htm
-
8/18/2019 Peds Fluid Mx Dn
26/41
PAGE 22 NSW HEALTH Infa nts and Children — Acute Mana gemen t of Ga stroent eritis
References
1. H unt JB, Elliott EJ, Fairclough PD et al.
W ater and solute absorption from
hypotonic glucose-electrolyte solutions in
hum an jejunum .Gut. 1992;33:479–483.
2. Booth I, Ferreira R, D esjeux JF et al.
Recom m endation for com position of
oral rehydration solutions for the
children of Europe. Report of an
ESPG A N w orking group. J Pediat ric
Gastroenterology and Nut rition.
1992;14:113–115.
3. Ferreira RM C C , Elliott EJ, W atson A JM
et al. D om inant role for osm olality in
the efficacy of glucose and glycine-containing oral rehydration solutions:
studies in a rat m odel of secretory
diarrhoea.Acta Paediat rics. 1991;
81:46–50.
4. H unt JB, Thillainayagam A V, Salim
A FM et al. W ater and solute
absorption from a new hypotonic oral
rehydration solution: evaluation inhum an and anim al perfusion m odels.
Gut. 1992;33:1652–1659.
5. International Study G roup on Reduced-
osm olarity O RS solutions. M ulticentre
evaluation of reduced-osm olarity oral
rehydration salts solution.Lancet.
1995;345:282–285.
6. W alker-Sm ith JA , Sandhu BK, Isolauri E
et al. Recom m endations for feeding in
childhood gastroenteritis.J Paediat ric
Gastroenterology and Nutrition.
1997;24:619–620.
7. M ackenzie A , Barnes G . Random ised
controlled trial com paring oral and
intravenous rehydration therapy in
children w ith diarrhoea.BMJ.
1991;303:393–6
8. Sharifi J, G havam i F, N ow rouzi Z et al.
O ral versus intravenous rehydration
therapy in severe gastroenteritis.
Archives of Diseases in Children. 1985;60:856–860.
9. Issenm an RM , Leung A K. O ral and
intravenous rehydration of children.
Can Fam Phy. 1993;39:2129–2136.
10. Vesikari T, Isolauri E, Baer M . A
com parative trial of rapid oral and
intravenous rehydration in acute
diarrhoea.Acta Paediatric Scand.
1987;76:300–305.
11. Santosham M , D aum RS, D illm an L et
al. O ral rehydration therapy of infantile
diarrhoea.New Eng J Med.
1982;306:1070–1076.
-
8/18/2019 Peds Fluid Mx Dn
27/41
NSW HEALTH Infa nts and Children — Acute Mana gemen t of Ga stroent eritis PAGE 23
12. Tam er A M , Friedm an LB, M axw ell SRW
et al. O ral rehydration of infants in a
large U S urban m edical center. Journal
of Pediatrics. 1985;107:14–19.
13. Listernick R, Zieserl E, Davis AT. O utpatient
oral rehydration in the U nited States.
Am J Dis Child. 1986;140:211–215.
14. N ager A L, W ang VJ. C om parison of
nasogastric and intravenous m ethods
of rehydration in pediatric patients
w ith acute dehydration.Pediatrics.
2002;109(4):566–572.
15. G rem se D A . Effectiveness ofnasogastric rehydration in hospitalised
children w ith acute diarrhoea. J
Paediatric Gastroenterology and
Nutrition. 1995;21:145–148.
16. N eville KA et al. Isotonic is better than
hypotonic saline for intravenous
rehydration of children w ith gastroent-
eritis: a prospective random ised study.
Arch Dis Child 2006 M ar; 91 (3): 226–232
-
8/18/2019 Peds Fluid Mx Dn
28/41
PAGE 24 NSW HEALTH Infa nts and Children — Acute Mana gemen t of Ga stroent eritis
A peria A et al. Salt and w ater hom eostasis
during oral rehydration therapy.J
Pediatr 1983;103:364–69
Arm on K, Stephenson T, M acFaul R et al. An
evidence and consensus based guideline
for acute diarrhoea m anagem ent.Arch
Dis Child 2001;85;132–142
Bhargava SK et al. O ral therapy of
neonates and young infants w ith
W orld H ealth O rganisation
Rehydration Packets: a controlled trial
of tw o sets of instructions J Paediat r
Gastroenterol Nutr 1986;5:416–22
Blum D et al. Safe oral rehydration ofhypertonic dehydration.J Paediat r
Gastroenterol Nutr 1986;5:232–35
Borow itz SM . A re antiem etics helpful in
young children suffering from acute
viral gastroenteritis? Arch Dis. Child
2005; 35:646–648
Brill SA , Stew art TR, Brundage SI,
Schreiber M A . Base deficit does not
predict m ortality w hen secondary to
hyperchlorem ic acidosis.
Shock.17(6):459–62, 2002.
Bullivant EM , W ilcox C S, W elch W J.
Intrarenal vasoconstriction during
hyperchlorem ia: role of throm boxane.
American Journal of Physiology . 256(1Pt 2):F152–7, 1989.
C arey M J, A itken M E. D iverse effects of
antiem etics in children.NZ Med J.
1994;107(989):452–3
C enters for D isease C ontrol and
Prevention. M anaging acute
gastroenteritis am ong children: oral
rehydration, m aintenance, and
nutritional therapy.Pediatrics.
2004;114:507
C H O IC E Study G roup. M ulticenter,
random ized, double–blind clinical trial
to evaluate the efficacy and safety of a
reduced osm olarity oral rehydration
salts solution in children w ith acute
w atery diarrhoea.Pediatrics. 2001
107(4):613–8
C hristakis DA , W right JA , Rivara F.
Prom ethazine therapy for
gastroenteritis: tow ards a better
understanding of use, risks and
benefits…including com m entary by
Saur P.Ambulatory Child Health .1998; 4(2):181–7
Chubeddu LX, Trujillo LM , Talm aciu I,
G onzales V, G uariguata J, Seijas J,
M iller IA , Paska W . A ntiem etic activity
of ondansetron in acute gastroenteritis.
Aliment Pharmacol Ther. 1997
Feb;11(1):185–91
Bibliography
-
8/18/2019 Peds Fluid Mx Dn
29/41
NSW HEALTH Infa nts and Children — Acute Mana gemen t of Ga stroent eritis PAGE 25
C utting W A M et al. Safety and efficacy of
three oral rehydration solutions for
children w ith diarrhoea (Edinburgh
1985–5).Acta Paediat r Scand 1989
M ar; 78(2):253–8.
D uggan C , Fontaine O , Pierce N F, et al.Scientific rationale for a change in the
com position of oral rehydration
Solution.JAMA. 2004; 291:2628–31
D urw ard A , Skellett S, M ayer A , Taylor D ,
Tibby SM , M urdoch IA . The value of
the chloride: sodium ratio in
differentiating the aetiology of
m etabolic acidosis.Intensive Care
Medicine. 27(5):828–35, 2001.
D urw ard A , Tibby SM , Skellett S, A ustin C ,
A nderson D , M urdoch IA . The strong
ion gap predicts m ortality in children
follow ing cardiopulm onary bypass
surgery.Pediat ric Crit ical Care
Medicine . 6(3):281–5, 2005.ESPG A N W orking G roup.
Recom m endations for com position of
oral rehydration solutions for the
children of Europe.J Pediat r
Gastroenterol Nut r. 1992; (1):113–5
Farthing M JG . O ral rehydration: an
evolving solution.J Pediat r
Gastroenterol Nut r. 2002 M ay–Jun;34
Suppl 1:S64–7
Freedm an SB, A dler M , Seshadri R, et al.
O ral ondansetron for gastroenteritis in
a paediatric em ergency departm ent.N
Engl J Med. 2006 354(16):1698–705
H ahn S, Kim Y, G arner P. Reduced
osm olarity oral rehydration solution for
treating dehydration due to diarrhoea
in children: system atic review .BMJ.
2001; 323:81–85
H ahn S, Kim Y, G arner P. Reducedosm olarity oral rehydration solution for
treating dehydration caused by acute
diarrhoea in children (C ochrane
Review ).Cochrane Database Sys Rev.
2002;(1):C D 002847
H o A M , Karm akar M K, C ontardi LH , N g
SS, H ew son JR. Excessive use of norm al
saline in m anaging traum atized patients
in shock: a preventable contributor to
acidosis. Journal of Trauma–Injury
Infect ion & Crit ical Care. 51(1):173–7,
2001.
H unt JB, Elliott EJ, Fairclough PD , C lark
M L, Farthing M JG . W ater and solute
absorption from hypotonic glucose–electrolyte solutions in hum an
jejunum . Gut. 1992 A pr;33(4):479–83
Isolauri E. Evaluation of an oral rehydration
solution w ith N a 60m m ol/L in infants
hospitalised for acute diarrhoea or
treated as outpatients.Acta Paediatr
Scand ; 74:643–49
Kellum JA . Fluid resuscitation and
hyperchlorem ic acidosis in
experim ental sepsis: im proved
short–term survival and acid-base
balance w ith H extend com pared w ith
saline.Crit ical Care Medicine.
30(2):300–5, 2002.
-
8/18/2019 Peds Fluid Mx Dn
30/41
PAGE 26 NSW HEALTH Infa nts and Children — Acute Mana gemen t of Ga stroent eritis
King C K, G lass R, Bresee JS, D uggan C ,
C enters for D isease C ontrol and
Prevention. M anaging acute
gastroenteritis am ong children: oral
rehydration, m aintenance, and
nutritional therapy.MMWR RecommRep. 2003 N ov 21;52(RR–16):1–16
Kw on KT, Rudkin SE, Langdorf M I.
A ntiem etic use in pediatric
gastroenteritis: a rational survey of
em ergency physicians, pediatricians,
and pediatric em ergency physicians.
Clin Pediat r. 2002 N ov–Dec 41(9):
641–52
Lem an P. U tility of ondansetron in children
w ith vom iting.Ann Emerg Med. 2002
Sep;40(3):366–7
Li ST, D iG iuseppe D L, C hristakis DA .
A ntiem etic use for acute
gastroenteritis in children.Arch Pediatr
Adolesc Med. 2003 M ay;157(5):475–9Listernick R, Zieseri E et al. O utpatient oral
rehydration in the U nited States.Am J
Dis Child. 1986;140:211–215
M ackenzie A , Barnes G . Random ised
controlled trial com paring oral and
intravenous rehydration therapy in
children w ith diarrhoea.Br Med J.
1991;303:393–396
M urphy M S. G uidelines for m anaging
acute gastroenteritis based on a
system atic review of published
research.Arch Dis Child . 1998
Sep;79(3):279–84
M urphy C, H ahn S, Volm ink J. Reduced
osm olarity oral rehydration solution for
treating cholera. C ochrane Database
Sys Rev. 2004, Issue 4. A rt.
N o:C D 003754
N ager A L, W ang VJ. Com parison ofnasogastric and intravenous m ethods
of rehydration in paediatric patients
w ith acute dehydration.Paediatrics
2002;109:566–72
N alin D R, H irschhorn N , G reenough W
3rd, Fuchs G J, C ash RA . C linical
concerns about reduced–osm olarity
oral rehydration solution.JAMA. 2004
Jun 2;291(21):2632–5
N eville KA , Verge C F, Rosenberg A R,
O’M eara M W , W alker JL. Isotonic is
better than hypotonic saline for
intravenous rehydration of children
w ith gastroenteritis: a prospective
random ised study.Archives of Diseasein Childhood. 91(3):226–32, 2006.
O ral rehydration solutions for the children
of Europe. Proceedings of a w orkshop
held at XXI annual m eeting of
ESPG A N , C openhagen 1988. Acta
Paediat r Scand Suppl. 1989;364:1–50
O’M alley CM , Frum ento RJ, H ardy M A ,
Benvenisty A I, Brentjens TE, M ercer JS
et al. A random ized, double–blind
com parison of lactated Ringer’s
solution and 0.9% N aC l during renal
transplantation.Anesthesia &
Analgesia. 100(5):1518–24, table of
contents, 2005.
-
8/18/2019 Peds Fluid Mx Dn
31/41
NSW HEALTH Infa nts and Children — Acute Mana gemen t of Ga stroent eritis PAGE 27
O zuah PO , A vner JR, Stein RE. O ral
rehydration, em ergency physicians,
and practice param eters: a national
survey.Pediatrics. 2002
Feb;109(2):259–61
Prough D S, Bidani A . H yperchlorem icm etabolic acidosis is a predictable
consequence of intraoperative infusion
of 0.9% saline.Anesthesiology.
90(5):1247–9, 1999.
Pow ell C VE, H eine RG , Priestley SJ.
Random ised-controlled trial of rapid vs
24-hour nasogastric rehydration in
children w ith acute gastroenteritis and
m oderate dehydration: PG 3-13.J Pediat r
Gastroenterol Nutr. 2005 M ay;40(5):651
Ram sook C , Sahagun-C arreon I, et al. A
random ized clinical trial com paring
oral ondansetron w ith placebo in
children w ith vom iting from acute
gastroenteritis.Ann Emerg Med 2002A pr;39(4):397–403
Reid F, Lobo D N , W illiam s RN , Row lands
BJ, A llison SP. (A b)norm al saline and
physiological H artm ann’s solution: a
random ized double-blind crossover
study.Clinical Science. 104(1):17–24,
2003.
Reeves JJ, Shannon M W , Fleisher G R.
O ndansetron decreases vom iting
associated w ith acute gastroenteritis: a
random ized, controlled trial.Pediatrics .
2002 A pr;109(4):e62
Spirko BA . A ntiem etic use for
gastroenteritis in children.Ann Emerg
Med. 2003 A pr;41(4):585–6; authorreply 586–7
Loo D M , van der G raaf F, Ten W T. The
effect of flavouring oral rehydration
solution on its com position and
palatability.J Pediat r Gastroenterol
Nutr. 2004 ;39(5):545–8
Saberi M S et al. O ral rehydration ofdiarrhoeal dehydration. C om parison of
high and low sodium concentration in
rehydration solutions.Acta Paediatr
Scand 1983;72:167–70
Santosham M et al. O ral rehydration
therapy of infantile diarrhoea; a
controlled study of w ell-nourished
children hospitalised in the U nited
States and Panam a.N Engl J Med.
1982;306:1070–1076
Santosham M et al. O ral rehydration
therapy for acute diarrhoea in
am bulatory children in the U nited
States: a double-blind com parison of
four different solutions.Paediatrics.1985;76:159–166
Scheingraber S, Rehm M , Sehm isch C ,
Finsterer U . Rapid saline infusion
produces hyperchlorem ic acidosis in
patients undergoing gynecologic surgery.
Anesthesiology. 90(5):1265–70, 1999.
Skellett S, M ayer A , D urw ard A , Tibby SM ,
M urdoch IA . C hasing the base deficit:
hyperchloraem ic acidosis follow ing
0.9% saline fluid resuscitation.
Archives of Disease in Childhood.
83(6):514–6, 2000.
Sokucu S et al. O ral rehydration therapy
in infectious diarrhoea. C om parison of
rehydration solutions w ith 60 and 90m m ol sodium per litre.Acta Paediatr
Scand 1985;74:489–94
-
8/18/2019 Peds Fluid Mx Dn
32/41
PAGE 28 NSW HEALTH Infa nts and Children — Acute Mana gemen t of Ga stroent eritis
Steele A , G ow rishankar M , A braham son S,
M azer C D , Feldm an RD , H alperin M L.
Postoperative hyponatrem ia despite
near-isotonic saline infusion: a
phenom enon of desalination.
Annals of Internal Medicine.126(1):20–5, 1997.
Vesikari T et al. A com parative trial of
rapid and intravenous rehydration in
acute diarrhoea.Acta Paediatr Scand
1987;76:300–305
W alker-Sm ith JA , Sandhu BK, Isolauri E et
al. G uidelines prepared by the ESPG A N
w orking group on acute diarrhoea:
recom m endations for feeding in
childhood gastroenteritis.J Pediat r
Gastroenterol Nutr. 1997 24(5):619–20
W aters JH , G ottlieb A , Schoenw ald P,
Popovich M J, Sprung J, N elson D R.
N orm al saline versus lactated Ringer’s
solution for intraoperative fluidm anagem ent in patients undergoing
abdom inal aortic aneurysm repair: an
outcom e study.Anesthesia &
Analgesia. 93(4):817–22, 2001.
W ilcox C S. Regulation of renal blood flow
by plasm a chloride.Journal of Clinical
Investigation.71(3):726–35, 1983.
W ilkes NJ, W oolf R, M utch M , M allett SV,
Peachey T, Stephens R et al. The
effects of balanced versus saline-based
hetastarch and crystalloid solutions on
acid-base and electrolyte status and
gastric m ucosal perfusion in elderly
surgical patients.Anesthesia &
Analgesia.93(4):811–6, 2001.
W illiam s EL, H ildebrand KL, M cCorm ick
SA , Bedel M J. The effect of
intravenous lactated Ringer’s solution
versus 0.9% sodium chloride solution
on serum osm olality in hum an
volunteers.Anesthesia & Analgesia .88(5):999–1003, 1999.
-
8/18/2019 Peds Fluid Mx Dn
33/41
NSW HEALTH Infa nts and Children — Acute Mana gemen t of Ga stroent eritis PAGE 29
A ppendices
Appendix One – Glossary
Word/
Abbreviation
Definition
A dm itting M edicalO fficer
M ost senior m edical officer under w hom the child is adm itted tohospital
BG L Blood G lucose (Sugar) Level
FBC Full Blood C ount
H artm ann’s solution Isotonic intravenous solution (see ‘Com position’table A ppendix Tw o)
O RS O ral Rehydration Solution
EUC Electrolytes, Urea and Creatinine. Ideally this should include m easurem ent
of serum sodium , potassium , chloride, bicarbonate, urea and creatinine. It
is recognised that not all local laboratories offer all of these param eters 24
hours. It is essential that the serum sodium be m easured on any child
w ho is receiving intravenous rehydration therapy.
-
8/18/2019 Peds Fluid Mx Dn
34/41
PAGE 30 NSW HEALTH Infa nts and Children — Acute Mana gemen t of Ga stroent eritis
OsmolalitymOsm/L Na
+
mmol/L Cl
-
mmol/L Glucoseg/L K
+
mmol/L
0.9% N aC l 300 150 150 – –
Hartm ann’s
Solution274 129 109 – 5
0.45% N aC l &
2.5% G lucose292 76 76 25 –
0.9% N aC l &
2.5% G lucose448 150 150 25 –
Appendix Two – IVT Composition
-
8/18/2019 Peds Fluid Mx Dn
35/41
NSW HEALTH Infa nts and Children — Acute Mana gemen t of Ga stroent eritis PAGE 31
Appendix Three – Parent Oral Rehydration
Documentation Form
Oral Fluids for your Child with Gastroenteritis
Please give your child:
1. Frequent breastfeeds if you are breastfeeding or
2. A n O ral Rehydration Solution
D ilute juice (e.g. 1 part apple juice to 4 parts w ater) is not as effective but som etim es m ay
be used if your child is not dehydrated.
Your child’s w eight is ______ kg.
Your child should drink about _________ m L every 5 m inutes (½ m L/kg) or 1 H ydralyte®
iceblock (62.5m L) every ______ M inutes.
U se the 10 m L syringe to m easure the fluid unless using H ydralyte® iceblock. G ive the fluid
to your child in a syringe, teaspoon, bottle or cup.
(O ne H ydralyte® iceblock = 62.5 m L)
Please record every tim e you give your child fluid and every tim e your child vom its, passes
urine or has diarrhoea:
TIME FLUID TYPE VOLUME VOMIT DIARRHOEA URINE1
2
3
4
5
6
7
8
9
10
11
12
13
14
1516
-
8/18/2019 Peds Fluid Mx Dn
36/41
PAGE 32 NSW HEALTH Infa nts and Children — Acute Mana gemen t of Ga stroent eritis
NSW Child
Health Networks
ORAL FLUIDS for
YOUR CHILD with GASTROENTERITIS
The nurse w ho assessed your sick child has placed you into an appropriate category for
urgency to see the doctor. It is m ost likely that your child has gastroenteritis and needs fluid
treatm ent. H ere in hospital w e use oral fluids w hile you are w aiting to see a doctor.
If you have been giving your child fluids at hom e, you are probably here because you feelthis has been unsuccessful. The w ay w e give oral fluids here m ay be slightly different and is
often successful. The other side of this sheet explains exactly how m uch fluid and how
often w e w ant you to give it to your child.
W hen your child sees the doctor a decision w ill be m ade as to w hether you can go hom e,
or w hether your child needs a sm all tube through the nose into the stom ach or a drip to
provide extra fluid for a few hours. Som etim es this is all it takes to m ake your child feel a
lot better and you w ill then be able to go hom e. If this doesn’t im prove your child, he orshe m ay need to be adm itted to hospital for further treatm ent.
-
8/18/2019 Peds Fluid Mx Dn
37/41
NSW HEALTH Infa nts and Children — Acute Mana gemen t of Ga stroent eritis PAGE 33
Appendix Four – Parent Information
A G astroenteritis Fact Sheet jointly developed by John H unter C hildren’s Hospital,
Sydney C hildren’s Hospital and C hildren’s Hospital W estm ead is available at:
w w w .ka leido scope.o rg.a u/pa rent s/fa ctshe et s.ht m
w w w .sch.edu .a u/he a lth /fa ctshe et s
w w w .chw .ed u.a u/pa rent s/fa ctshe et s
Disclaimer: The fact sheet is for educational purposes only. Please consult w ith your doctor
or other health professional to ensure th is information is right for your child.
-
8/18/2019 Peds Fluid Mx Dn
38/41
PAGE 34 NSW HEALTH Infa nts and Children — Acute Mana gemen t of Ga stroent eritis
Appendix Five – Resources
Fuller details m ay be necessary in practice, especially for the m anagem ent of children
w ith m oderate or severe dehydration. Possible sources include:
N SW H ealth D epartm ent C IA P w ebsite, M anaging Y oung C hildren and Infants w ith
G astroenteritis in H ospitals at: w w w .ciap.health.nsw .gov.au also
The C hildren’s H ospital W estm ead H andbook, 2004 (Sections 7 — Fluid Therapy, and
Section 16 — G astroenterology), available as a book from the C hildren’s Hospital at
W estm ead, or at:w w w .chw .edu.a u/pa rents/fa ctsheet s
G astroenteritis Fact Sheet jointly developed by the John H unter C hildren’s Hospital,
Sydney C hildren’s Hospital and C hildren’s Hospital W estm ead at:
w w w .ka leido scope.o rg.a u/pa rent s/fa ctshe et s.ht m
w w w .sch.edu .a u/he a lth /fa ctshe et s
w w w .chw .ed u.a u/pa rent s/fa ctshe et s
-
8/18/2019 Peds Fluid Mx Dn
39/41
NSW HEALTH Infa nts and Children — Acute Mana gemen t of Ga stroent eritis PAGE 35
Appendix Six – Significant Changes From
2002 CPG Version
Levels of dehydration m odified Rapid and standard rehydration techniques included and volum e calculations am ended
IV Fluid Therapy section m odified
Enteral Rehydration Therapy section included
M edications section revised and expanded
Indication for blood chem istry revised
Reintroduction of diet m odified H yponatrem ia section added
Parent fluid docum entation form included
Appendix Seven – Alternative Calculation
for Maintenance Fluids
Calculate the maintenance fluid requirement, for 24 hours, by age:
–Infants up to 9 m onths: 120–140m L/kg/24hrs
–Children 9–24 m onths: 90–100m L/kg/24hrs
–Children 2–4 years: 70–90m L/kg/24hrs
–Children 4–8 years: 60–70m L/kg/24hrs
–O lder children: 50–60m L/kg/24hrs
-
8/18/2019 Peds Fluid Mx Dn
40/41
PAGE 36 NSW HEALTH Infa nts and Children — Acute Mana gemen t of Ga stroent eritis
Appendix Eight – Working Party Members
Dr Christopher Webber (Chair)
Paediatric Em ergency Physician and
C onsultant PaediatricianEm ergency D epartm ent
Sydney C hildren’s H ospital
Dr Matthew Chu
D irector of Em ergency M edicine
C anterbury H ospital
Dr Steven Doherty (to March 2007)Em ergency Physician
Em ergency D epartm ent
Tam w orth H ospital
Dr Patrick Moore
Staff Specialist Paediatrician
Fairfield H ospital
Dr Kristen Neville
Paediatric Endocrinologist
Sydney C hildren’s H ospital
Dr Susan Phin
Paediatric Em ergency Physician
Em ergency D epartm ent
C hildren’s Hospital W estm ead
Mr Phillip Way
C linical N urse C onsultant
Rural C ritical C areH unter N ew England A rea H ealth Service
Ms Rhonda Winskill
C linical N urse C onsultant, Paediatrics
H unter N ew England A rea H ealth Service
Ms Leanne Crittenden
C oordinatorN orthern C hild H ealth N etw ork
Ms Judy Lissing
C oordinator
G reater Eastern and Southern
C hild H ealth N etw ork
Ms Halina NagielloC oordinator
W estern C hild H ealth N etw ork
Ms Mary Crum
Senior A nalyst
C linical Policy Branch (Secretariat)
N SW H ealth
Mr Bart Cavalletto
M anager, Statew ide Paediatric Services
N SW H ealth
-
8/18/2019 Peds Fluid Mx Dn
41/41





![New Years Poster [Peds] 8 - FFF Enterprises · Title: New Years Poster [Peds] 8.5x11 Subject: New Years Poster [Peds] 8.5x11 Keywords: New Years Poster [Peds] 8.5x11 Created Date:](https://static.fdocuments.us/doc/165x107/5fd6db4c8a000945d6684aca/new-years-poster-peds-8-fff-title-new-years-poster-peds-85x11-subject-new.jpg)