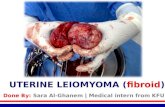
Overview of Sonography-guided Transcervical Fibroid Ablation · uterus-preserving treatment option...
Transcript of Overview of Sonography-guided Transcervical Fibroid Ablation · uterus-preserving treatment option...

1 | ML 06072 -001.B
Overview of Sonography-Guided
Transcervical Fibroid Ablation
David Toub, MD
Medical Director, Gynesonics

3 | ML 06072 -001.B
The Need for a New Treatment Option for Symptomatic Fibroids
In a published national survey of affected women:1
Women delayed seeking treatment for an average of 3.6 years, with 32%
waiting more than five years.
79% of women want to avoid invasive surgery that can require lengthy
recoveries.
Women of all ages are asking for alternatives to hysterectomy and want a
uterus-preserving treatment option regardless of their desire for
childbearing.
1) Borah BJ, Nicholson WK, Bradley L, Stewart EA. The impact of uterine leiomyomas: a national survey of affected women. Am J Obstet Gynecol. Oct 2013;209(4):319 e1-319 e20.

4 | ML 06072 -001.B
Transcervical Fibroid Ablation (TFA)
Volumetric, image-guided radiofrequency ablation
Enables optimized ablated volume of targeted fibroid
Avoids multiple passes of energized needles through the serosa
Not a global therapy; can treat the fibroids that are likely to be symptomatic
Incites thermal fixation and coagulative necrosis
Not associated with infarction-related post-embolization syndrome.

5 | ML 06072 -001.B
Sonata Transcervical Fibroid Ablation System
FDA cleared and CE marked
Uses radiofrequency (RF) energy to ablate fibroids
under real-time intrauterine sonography (integrated
within device)

6 | ML 06072 -001.B
Intended UseThe Sonata System is intended for diagnostic intrauterine imaging and transcervical treatment
of symptomatic uterine fibroids, including those associated with heavy menstrual bleeding.
Contraindications
Current pregnancy; active pelvic infection; known or suspected gynecologic malignancy or premalignant disorders such as atypical endometrial hyperplasia;
presence of one or more intratubal implants for sterilization; and presence of an intrauterine device (IUD), unless removed prior to the introduction of the
Sonata Treatment Device.
Patient Selection Considerations
Safety and effectiveness with regard to fertility and fecundity after the use of the Sonata System have not been established, and effectiveness in women with
clinically significant adenomyosis has not been established.
Anticipated Postoperative Events and Potential Risks
Anticipated postoperative events include: abdominopelvic pain/cramping; back pain; constipation; dizziness/fatigue; headache; fever; malaise;
nausea/vomiting; sloughing and, less commonly, intact expulsion of ablated fibroid tissue per vaginam (particularly after ablation of submucous fibroids),
and vaginal spotting/bleeding/dysmenorrhea. Potential risks associated with fibroid ablation using the Sonata System include: allergic reactions (including
rash) to device materials; bowel or bladder perforation; cervical/vaginal laceration or tear; dysmenorrhea; electrical shock; hematometrium; hemorrhage;
infections: major and minor local and systemic infections, including intrauterine infection; retention of device fragment; skin burn from the dispersion of RF
energy; thrombotic events; unintended injury to the uterus, cervix or vaginal vault, adjacent organs or tissue; unknown risk to future pregnancies; and
complications including death.
To learn more about the Sonata System, visit us at gynesonics.com/sonata-system or sonatatreatment.com

7 | ML 06072 -001.B
Sonata System Technology
Sonata System Hardware and Software
No manual measurements - all done graphically
Scalable ablations up to 49mm x 42mm
1.5 to 7-minute ablation times
RF generator modulates power (≤ 150W) to
keep electrode tip temperatures ~105 C
Sonata Treatment Device
Combines intrauterine ultrasound with
delivery of RF energy
8.3 mm tip diameter (27 Fr dilatation)

8 | ML 06072 -001.B
SMART Guide: Graphical Overlays on Live Ultrasound Image
IUUS Probe Tip
Ablation Zone
Thermal Safety
Border
Ablation Zone: (red inner ellipse)
A graphical representation of the average
region of tissue ablation.
Thermal Safety Border: (green outer ellipse)
The distance at which tissue is safe from
potential of thermal damage.

9 | ML 06072 -001.B *Data on file at Gynesonics. MTF 190719-01
No Manual Measurements Necessary with SMART Guide
Algorithms used to display the SMART Guide were developed and validated by 1,928
clinical and bench tests including direct uterine serosal temperature measurements.*
Tissue is safe from any treatment effect at or beyond the Thermal Safety Border.
The size and position of
the Ablation Zone is
selected by the
gynecologist under
real-time ultrasound
guidance.
The Thermal Safety
Border adjusts
automatically to
correspond with
changes to the
Ablation Zone.

10 | ML 06072 -001.B
100% fibroid volume ablated
Predictable Targeting and Optimized Fibroid Volume Ablation
Fibroids were treated transcervically with the
Sonata System prior to elective hysterectomy
two weeks later.
The treating gynecologist utilized the SMART
Guide to target fibroids.
Uteri were sectioned and ablations assessed.
Pathologists found that ablations were located
and sized as predicted.
Full Reference: Garza-Leal, JG, Toub, D, León, IH, et al. Transcervical, intrauterine ultrasound-guided radiofrequency ablation of uterine fibroids with the VizAblate System: safety, tolerability, and ablation
results in a closed abdomen setting. Gynecol Surg (2011) 8: 327.
90% fibroid volume ablated
Viable, non-ablated fibroid
tissue.
Fibroid B:
4.1 x 3.7 x 3.8 cm Fibroid A:
2.8 x 2.5 x 2.1 cm
Ablated fibroid tissue.

11 | ML 06072 -001.B
Designed to Treat All Non-Pedunculated Uterine Fibroid Types
The Sonata System is designed to ablate or
partially ablate the target fibroids in GREEN
FIGO Leiomyoma Subclassification System

12 | ML 06072 -001.B
The FAST-EU trial:
12-month clinical outcomes of women
after intrauterine sonography-guided
transcervical radiofrequency ablation
of uterine fibroids.
Brölmann H, Bongers M, Garza-Leal JG et al.
Gynecol Surg. 2016; 13: 27-35.

13 | ML 06072 -001.B
Brölmann H, Bongers M, Garza-Leal JG
et al. The FAST-EU trial: 12-month
clinical outcomes of women after
intrauterine sonography-guided
transcervical radiofrequency ablation
of uterine fibroids. Gynecol Surg. 2016;
13: 27-35.
Baseline 3-months 12-months
Time course series on MR, courtesy of Jose Gerardo Garza-Leal, MD
FAST-EU
Clinical Trial
Objective To establish the safety and effectiveness of the Sonata
System in the treatment of symptomatic uterine fibroids
Study Design ▪ 50 patients treated at 7 centers in Europe and Mexico
3-months ▪ 90% of patients had a reduction in menstrual bleeding
12-months
▪ 92% of patients were free from surgical reintervention
for heavy menstrual bleeding
▪ 54% mean reduction in menstrual bleeding
▪ 67% mean reduction in fibroid volume
▪ 88% overall patient satisfaction

14 | ML 06072 -001.B
The SONATA Pivotal IDE Trial:
Ultrasound-Guided Transcervical Ablation of
Uterine Leiomyomas
12-Month Results
Chudnoff S, Guido R, Roy K, Levine D, Mihalov L,
Garza-Leal JG. Obstetrics & Gynecology. 2019; 133: 13-22.
Transcervical Radiofrequency Ablation of
Symptomatic Uterine Fibroids:
2-Year Results
Miller CE, Osman KM, J Gynecol Surg
2019; 35:345-349

15 | ML 06072 -001.B
12 Month Results
Chudnoff S, Guido R, Roy K, et al.
Ultrasound-Guided Transcervical Ablation of
Uterine Leiomyomas. Obstet Gynecol; 2019;
133: 13-22.
2-Year Results
Miller CE, Osman KM, Transcervical
Radiofrequency Ablation of Symptomatic
Uterine Fibroids: 2-Year Results of the
SONATA Pivotal Trial
J Gynecol Surg 2019; 35:345-349
SONATA
Pivotal IDE TrialObjective To establish the safety and effectiveness of the Sonata System
in the treatment of symptomatic uterine fibroids
Study Design Prospective, longitudinal, multicenter, single-arm
interventional study. 22 sites with 147 patients treated.
Subjects followed at 10 days, 30 days, 3, 6, 12, 24 and 36
months.
Co-Primary
Endpoints
Reduction in menstrual blood loss (MBL) as assessed by
pictorial blood loss assessment chart (PBAC)
Rate of surgical reintervention for heavy menstrual bleeding
(HMB) due to treatment failure
Quality of Life
Measures
Patient-reported outcomes included the Uterine Fibroid
Symptom Health-Related Quality of Life Questionnaire (UFS-
QOL) and the Overall Treatment Effect Questionnaire (OTE)

16 | ML 06072 -001.B
Treatment Summary, Procedure Time, and Length of Stay
Total Fibroids Ablated 442
Mean # Ablated Fibroids per Patient 3.0 (range:1-9)
Mean # Ablations per Fibroid 1.1 ± 0.4
Procedure Time (minutes)(time elapsed from insertion of device to removal of device)
Median
40.0 min Mean
46.9 ± 29.7min
Length of Stay (hours)(time elapsed from insertion of device to time of discharge)
Median
2.3 hours
Mean
2.5 ± 1.2
Return to Normal Activity (days)Median
1 day
Mean
2.2 ± 2.2

17 | ML 06072 -001.B
Well-Tolerated Procedure with Choice of Anesthesia
*pain scores captured on a 0-10 scale
Anesthesia Regimen
% of patients who underwent GA 50.3%
% of patients who had CS 49.7%
Mean Pain* During Procedure
GA .01
CS .47
Mean Pain* During Recovery
GA 3.4
CS 1.9
Patients Who Found the Procedure Tolerable 98%

18 | ML 06072 -001.B
80% of Fibroids Treated in SONATA Trial were NOT Amenable to
Treatment with Operative Hysteroscopy

19 | ML 06072 -001.B
Significant Reduction in Menstrual Bleeding
through 12 Months
303.6
175.9159.5
143.8
0
50
100
150
200
250
300
350
Baseline 3M 6M 12M
Mean Pictorial Blood Loss Assessment Chart (PBAC)
All p < 0.001
-39% -48% -51%
▪ 86% of patients reported a reduction
in menstrual bleeding at 3 months
post-procedure.
▪ 95% of patients reported a reduction
in menstrual bleeding at 12 months
▪ 65% of women reported >50%
reduction in menstrual bleeding.
▪ Sonata was effective in patients
where their only qualifying fibroid
was one or more intramural type 3.

20 | ML 06072 -001.B
Safety Profile
▪ No device-related Serious Adverse Events (SAEs)
▪ 2 procedure-related SAEs; both resolved with no sequelae
▪ DVT 15 days post-procedure
▪ Vaginal discharge with low-grade fever and cramping 28 days post-procedure
▪ Overnight hospital stay for antibiotic administration per hospital policy
▪ Cultures negative for infection

21 | ML 06072 -001.B
Rapid Return to Normal Activity and Work
▪ 50% of patients returned to normal activity
by the next dayOn average, patients resumed normal
functions:
▪ Diet at 0.8 ± 1.3 days
▪ Sleep at 0.7 ± 1.6 days
▪ Urinary function at 0.2 ± 0.8 days
▪ Bowel function at 1.4 ± 1.9 days
▪ Mean return to normal activity: 2.2 days ± 2.2 days
▪ Mean return to work: 3.6 ± 2.6 days

22 | ML 06072 -001.B
Timepoint
Cumulative
Surgical
Reinterventions
Cumulative Surgical
Reintervention Rate
(Binomial)
Cumulative Surgical
Reintervention Rate
(Life-Table)
Cumulative Surgical
Reintervention Rate
(Kaplan-Meier)
1 Year 1 0.7% 0.7% 0.7%
2 Year 7 5.5% 5.2% 5.0%
3 Year 11 9.2% 8.5% 8.2%
Low Rate of Surgical Reintervention for HMB through 3 Years
Surgical reintervention rates remained low through 3 years regardless of statistical analysis methods.

23 | ML 06072 -001.B
Improvements in Work and Activity Impairment
Maintained through 3 Years
All p-values < 0.001 compared to baseline
50.9%
57.9%
11.4% 11.7%14.6% 13.7%12.5%
14.3%
0.0%
10.0%
20.0%
30.0%
40.0%
50.0%
60.0%
Overall Work Impairment
(absenteeism + presenteeism)
Activity Impairment
Me
an
Wo
rk a
nd
Act
ivit
y I
mp
air
me
nt
Baseline 12M 24M 36M

24 | ML 06072 -001.B
Significant Quality of Life Improvements Persist
Through 3 Years
All p-values < 0.001 compared to baseline
54.9
26.922.7 22.6 23.7 22.2
40.3
77.9
84.0 84.2 82.7 83.1
0.0
20.0
40.0
60.0
80.0
100.0
Baseline 3M 6M 12M 24M 36M
SSS HR-QoL
Symptom Severity Score (SSS) and Health Related Quality of Life (HR-QoL) Outcomes

29 | ML 06072 -001.B
Bongers M, Quinn SD, Mueller MD,
et al. Evaluation of Uterine Patency
following Sonography-Guided
Transcervical Ablation of Fibroids.
Eur J Obstet Gynecol Reprod Biol.
2019;242:122-125.
OPEN Trial
Objective Characterize incidence of new intrauterine adhesions following
Sonata treatment
Study Design Post-market, prospective, multicenter, single-arm, observational
study in Europe. Indenting fibroid required for inclusion.
• Hysteroscopic assessment at baseline and 6-weeks
Endpoint Incidence of new adhesions at 6 weeks per European Society of
Hysteroscopy adhesion scoring by independent readers

30 | ML 06072 -001.B
OPEN Trial Results:
No Adhesiogenesis After Treatment
37 patients enrolled at 6 sites
Mean patient age: 42.4 ± 7.2 years (range 29-55)
Mean ablated fibroid diameter: 3.2 ± 1.6 cm (range 1-8 cm)
2 patients withdrew prior to follow-up
35 pairs of baseline and follow-up hysteroscopies
were evaluated by independent readers.
1 patient video was unevaluable (no agreement in evaluation
by any of the 3 independent readers)
34 showed no sign of adhesions after Sonata per agreement in
evaluation by 2 independent readers
6 out of 34 patients had apposing submucous fibroids ablated
with no resulting adhesions

31 | ML 06072 -001.B
Systematic Review and Meta-analysis of Studies
Radiofrequency Ablation of Uterine Fibroids
Bradley LD, Pasic RP, Miller LE. Clinical Performance of Radiofrequency Ablation for Treatment of Uterine Fibroids: Systematic Review and Meta-Analysis
of Prospective Studies. J Laparoendosc Adv Surg Tech A. 2019;1507-1517.
OBJECTIVETo examine the evidence regarding typical patient outcomes
with radiofrequency ablation (RFA)
OUTCOMES
FOR ANALYSIS
• Procedure time and patient recovery metrics
• Change in fibroid volume
• Symptom Severity Scores and Health-Related QOL Scores
• Reinterventions
N=32 articles
1283 unique patients
CONCLUSIONS
Radiofrequency ablation (RFA) of uterine fibroids significantly
reduces fibroid volume, provides significant durable improve-
ments in fibroid-related quality of life and is associated with
favorable reintervention rates.
REPORTED KEY
OUTCOMES
LAPAROSCOPIC
APPROACH
TRANSCERVICAL
APPROACH
Mean procedure
time73 min 44 min
Mean time to
discharge10.7 hours 2.5 hours
Mean return to
normal activities9.0 days 3.3 days
Mean time to
return to work6.5 days 3.6 days

32 | ML 06072 -001.B
Summary of Key Outcomes
Outcomes associated with sonography-guided transcervical fibroid ablation
(TFA) to treat symptomatic uterine fibroids:
A significant reduction in mean menstrual bleeding
Low surgical reintervention for HMB
Well tolerated by patients with rapid return to normal activity
Significant and durable improvements in fibroid symptoms and health-related
quality of life
High patient satisfaction and willingness to recommend this treatment

33 | ML 06072 -001.B
THANK YOU!