Morning Report August 4, 2009. HSP AKA Henoch-Schönlein Purpura Most common form of systemic...
-
Upload
darleen-curtis -
Category
Documents
-
view
215 -
download
0
Transcript of Morning Report August 4, 2009. HSP AKA Henoch-Schönlein Purpura Most common form of systemic...

Morning Report
August 4, 2009


HSP
AKA Henoch-Schönlein Purpura Most common form of systemic vasculitis in
children 90% of cases are pediatric Majority are self limited

HSP
Epidemiology 3-15 years of age
Mean – 6-7 years Slight male predominance Less frequently in black children Rare in summer Triggers
Preceding URI in 50% Other infections, vaccinations, insect bites Underlying cause is unknown

HSP
Pathogenesis Immune-mediated
vasculitis IgA deposition
small vessels of skin and kidneys

HSP
Classic Tetrad Palpable purpura
Without thrombocytopenia or coagulopathy Present in almost all patients
Arthritis/Arthralgia 75%
Abdominal Pain 50%
Renal Disease 21-54%
Not all symptoms must be present for diagnosis Takes days to weeks to develop May present as abd pain or joint complaints*

HSP
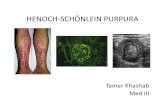
Rash Erythematous, macular
or urticarial wheals Wheals coaslesce and
evolve to ecchymoses, petechiae and palpable purpura
Crops, symmetrical distribution, located in gravity/pressure dependant areas
Lower extremities Toddlers – buttocks,
face, trunk and UE

HSP
Arthritis/Arthralgia Transient or migratory Oligoarticular
1 – 4 joints Nondeforming w/o
chronic sequelae Involved joints
Hip, knee, ankle Less common – elbow,
wrist or hand Periarticular swelling and
tenderness No effusion, erythema
or warmth Cause considerable pain
and limited motion

HSP
GI Mild symptoms
Nausea, vomiting, pain, transient paralytic ileus Severe symptoms
Hemorrhage, bowel ischemia and necrosis, intussusception, bowel perforation
Seen within 8 days of rash Pain caused by submucosal hemorrhage and
edema

HSP
Intussusception Most common severe
GI complication Limited to small bowel
60% Ileal-Ileal

HSP
Renal Mild
Isolated hematuria and/or proteinuria Severe
Acute nephropathy w/ renal insufficiency Within 4 weeks of presentation Excellent prognosis*
Small risk of progressive disease Nephrotic syndrome is poor prognostic sign*

HSP
Other manifestations Orchitis Seizures Parotitis Carditis Pulmonary hemorrhage

HSP
Recurrence 1/3 of cases Within 4 months Milder and shorter

HSP Diagnosis is Mainly Clinical
Unusual presentations may require biopsy Lab*
No test is diagnostic IgA elevated in 50-70% Platelet count and coags normal
If inconclusive on H&P U/A*
RBCs, casts, proteinuria Screen beyond acute presentation

HSP
Treatment* Outpatient Mainly supportive
Hydration IVFs or TPN
Rest Symptomatic relief of pain
NSAIDs
Edema Elevation of area

HSP
When to admit? Not maintaining hydration Severe abdominal pain Significant GI bleeding AMS Severe joint involvement limiting ambulation Renal Insufficiency
HTN and/or nephrotic syndrome

HSP
Steroids Use is controversial Reported benefits include
Decreased duration of abdominal pain Decreased risk of intussusception, recurrence, renal
involvement Have not been proven in studies
Recommended for use with severe abdominal pain Prednisone 1-2mg/kg/day (max 60-80mg) Methylprednisone 0.8-1.6mg/kg/day (max 64mg/day) Weaned over 4-8 weeks

HSP
Prognosis Excellent Resolves within 1 month Recurrence in 1/3
Milder
Morbidity GI Renal

HSP
Follow Up UA and BP
1st 2 months Weekly or biweekly
If results remain normal space to monthly then every other month for the 1st year