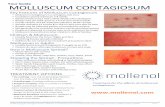
Molluscum
description
Transcript of Molluscum

DOJ Contents
Molluscum Contagiosum Daniel Hanson and Dayna G. Diven Dermatology Online Journal 9(2): 2 Primary Health, Boise, Idaho USA
Abstract
Molluscum contagiosum is a disease caused by a poxvirus of
the Molluscipox virus genus that produces a benign self-limited
papular eruption of multiple umbilicated cutaneous tumors. This
common viral disease is confined to the skin and mucous
membranes. Transmission requires direct contact with infected
hosts or contaminated fomites. It is generally thought to infect
humans exclusively, but there are a few isolated reports of
Molluscum contagiosum occurring in chickens, sparrows, pigeons,
chimpanzees, kangaroos, a dog, and a horse. The infection is found
worldwide and has a higher incidence in children, sexually active
adults, and those who are immunodeficent.
Introduction
Molluscum contagiosum, a cutaneous and mucosal eruption
caused by a Molluscipox virus, was first described and later
assigned its name by Bateman in the beginning of the nineteenth
century.[1] In 1841 Henderson and Paterson described the
intracytoplasmic inclusion bodies now known as molluscum or
Henderson-Paterson bodies.[2] In the early twentieth century,
Juliusberg, Wile, and Kingery were able to extract filterable virus
from lesions and show transmissibility.[3,4] Goodpasture later
described the similarities of molluscum and vaccinia.[5] Though
generally thought to infect only humans, case reports of the virus
occurring in other animals have been published. [6,7,8,9]
Incidence
Molluscum contagiosum virus (MCV) can be found
worldwide with a higher distribution in the tropical areas. The
disease is more prevalent in children with the lesions involving the
Page 1 of 11Molluscum Contagiosum
14/2/2007http://dermatology.cdlib.org/92/reviews/molluscum/diven.html

face, trunk, and extremities. In adults the lesions are most
often found near the genital region. The disease is endemic with a
higher incidence within institutions and communities where
overcrowding, poor hygiene, and poverty potentiate its spread.[10]
Over the last 30 years its incidence has been increasing, mainly as
a sexually transmitted disease, and it is particularly rampant as a
result of concurrent human immunodeficiency virus (HIV)
infection.[11] The worldwide incidence is estimated to be between
2% and 8%.[12] Less then 5% of the children in the United States
are believed to be infected. Between 5% and 20% of patients with
HIV have symptomatic MCV.[13,14] There are four main subtypes
of molluscum contagiosum: MCV I, MCV II, MCV III, and MCV
IV.[15,16] All subtypes cause similar clinical lesions in genital and
nongenital regions. Studies show MCV I to be more prevalent
(75%–90%) than MCV II, MCV III, and MCV IV, except in
immunocompromised individuals.[17,18] There are, however,
regional variations in the predominance of a given subtype and
differences between individual subtypes in different countries.[19]
Pathogenesis
This disease is transmitted primarily through direct skin
contact with an infected individual. Fomites have been suggested
as another source of infection, with molluscum contagiosum
reportedly acquired from bath towels, tattoo instruments, and in
beauty parlors and Turkish baths.[10] The average incubation time
is between 2 and 7 weeks with a range extending out to 6 months.
Infection with the virus causes hyperplasia and hypertrophy of the
epidermis.[12] Free virus cores have been found in all layers of the
epidermis. So-called viral factories are located in the malpighian
and granular cell layers.[12] The molluscum bodies contain large
numbers of maturing virions. These are contained intracellularly in
a collagen-lipid-rich saclike structure that is thought to deter
immunological recognition by the host.[20] Rupture and discharge
of the infectious virus-packed cells occur in the center of the lesion.
MCV induces a benign tumor instead of the usual necrotic pox
lesion associated with other poxviruses.[21]
Clinical manifestations
MCV produces a papular eruption of multiple umbilicated
lesions. The individual lesions are discrete, smooth, and dome
shaped. They are generally skin colored with an opalescent
character. The central depression or umbilication contains a white,
waxy curdlike core. The size of the papule is variable, depending
upon the stage of development, usually averaging 2–6 mm. Papules
Page 2 of 11Molluscum Contagiosum
14/2/2007http://dermatology.cdlib.org/92/reviews/molluscum/diven.html

may exceed 1 cm in size in immunosuppressed hosts. The
papules may become inflamed spontaneously or after trauma and
present atypically in size, shape, and color. The lesions are often
grouped in small areas but may also become widely disseminated.
Any cutaneous surface may be involved, but favored sites
include the axillae, the antecubital and popliteal fossae, and the
crural folds. Rarely, MCV lesions occur in the mouth or
conjunctivae.[22,23,24] Autoinoculation is common. Children
usually acquire molluscum nonsexually at both genital and
nongenital areas. MCV in adults affects the groin, genital area,
thighs, and lower abdomen and is often acquired sexually. Around
10% of cases develop an eczematous dermatitis around the lesions,
but this disappears as the infection resolves.[25] Patients with
atopic dermatitis can have a disseminated eruption. Eruptions in
immunocompromised indiviuals are very resistant to treatment.
[13,26]
Dermatopathology
Histologically, molluscum contagiosum exhibits
intraepidermal lobules with central cellular and viral debris. In the
basal layer, enlarged basophilic nuclei and mitotic figures are seen.
Progressing upward, the cells show cytoplasmic vacuolization and
then eosinophilic globules. The nucleus becomes compressed at the
level of the granular cell layer, and the molluscum bodies lose their
internal structural markings. Undisrupted lesions show an absence
of inflammation, but dermal changes can include an infiltrate that
is lymphohistiocytic, neutrophilic, or granulomatous. The latter has
been seen in solitary lesions. Antibody to MCV by indirect
immunofluorescence has been found in 69% of patients with
visible lesions.[27] Polymerase chain reaction can detect MCV in
skin lesions.[28] Currently, there is no in-vitro or animal model for
MCV. MCV can undergo an abortive infection in some cell lines,
which can cause confusion with herpes simplex virus by
laboratories.[29] Two sets of investigators have infected human
skin with molluscum contagiosum and grafted it onto athymic
mice, although there was no continued viral replication.[30,31]
Diagnosis
The clinical appearance of molluscum contagiosum is in most
cases diagnostic. Though molluscum cannot be cultured in the
laboratory, histological examination of a curetted or biopsied lesion
can also aid in the diagnosis in cases that are not clinically obvious.
The thick white central core can be expressed and smeared on a
Page 3 of 11Molluscum Contagiosum
14/2/2007http://dermatology.cdlib.org/92/reviews/molluscum/diven.html

slide and left unstained or stained with Geimsa, Gram, Wright,
or Papanicolaou stains to demononstrate the large brick-shaped
inclusion bodies. Electron microscopy has also been used to
demonstrate the poxivirus structures. Immunohistochemical
methods using a polyclonal antibody allows recognition of
molluscum contagiosum in fixed tissue.[32] In-situ hybridization
for MCV DNA has also been utilized.[33] Molluscum contagiosum
lesions must be differentiated from verruca vulgaris, condyloma
accuminata, varicella, herpes simplex, papillomas, epitheliomas,
pyoderma, cutaneuos cyptococcosis, epidermal inclusion cyst,
basal cell carcinoma, papular granuloma annulare,
keratoacanthoma, lichen planus, and syringoma or other adenexal
tumors.
Treatment
Molluscum cantagiosum is a self-limited disease, which, left
untreated, will eventually resolve in immunocompetent hosts but
may be protracted in atopic and immunocompromised individuals.
Some patients pick and scratch at the lesions, a habit that may lead
to scarring. In addition, some schools and daycare centers will not
admit children with visible molluscum papules. When patients seek
medical attention and desire to rid themselves of the papules, there
are several means of therapeutic destruction to help speed
resolution. The decision whether treatment is necessary depends on
the needs of the patient, the recalcitrance of their disease, and the
likelihood of treatments to leave pigmentary alteration or scarring.
Most of the common treatments consist of various means to
traumatize the lesions. Antiviral and immune-modulating
treatments have recently been added to the options. The following
is a brief summary of some of the more common treatments.
Cryosurgery
One of the most common, quick, efficient methods of
treatment is cryotherapy. Liquid nitrogen, dry ice, or Frigiderm are
applied to each individual lesion for a few seconds. Repeat
treatments in 2–3-week intervals may be required.[34] Hyper- or
hypopigmentation and scarring may be caused by this treatment.
Evisceration
An easy method to remove the lesions is eviscerating the core
with an instrument such as a scalpel, sharp tooth pick, edge of a
glass slide, or any other instrument capable of removing the
Page 4 of 11Molluscum Contagiosum
14/2/2007http://dermatology.cdlib.org/92/reviews/molluscum/diven.html

umbilicated core. Because of its simplicity, patients, parents,
and caregivers may be taught this method so new lesions can be
treated at home.[35,36] This method is simple but may not be
tolerated by small children.
Curettage
Curettage is another method of removal. It can be used with
and without light electrodessication. This method is more painful,
and it is recommended that a topical anesthetic cream be applied to
the lesions before the procedure to decrease the pain. This method
has the advantage of providing a reliable tissue sample to confirm
the diagnosis.[35,37]
Tape stripping
Another reported treatment involves the use of adhesive tape.
The adhesive side of the tape is repeatedly applied to and removed
from the lesion for 10–20 cycles. This action effectively removes
the superficial epidermis from the top of the lesion.[38] However,
repeated use of the same strip has the potential to spread the virus
to adjacent, uninvolved skin.
Podophyllin and podofilox
A 25% suspension in a tincture of benzoin or alcohol may be
applied once a week. This treatment requires some precautions. It
contains two mutagens, quercetin and kaempherol. Some of the
listed side effects include severe erosive damage in adjacent
normal skin that may cause scarring and systemic effects such as
peripheral neuropathy, renal damage, adynamic illeus, leucopenia,
and thrombocytopenia, especially if used generously on mucosal
surfaces. Podofilox is a safer alternative to podophyllin and may be
used by the patient at home. The recommended use usually consists
of application of 0.05 ml of 5% podofilox in lactate buffered
ethanol twice a day for 3 days.[35,38] The active agent is
absolutely contraindicated in pregnancy.
Cantharidin
Cantharidin (0.9% solution of collodian and acetone) has been
used with success in the treatment of MCV. This blister-inducing
agent is applied carefully and sparingly to the dome of the lesion
with or without occlusion and left in place for at least 4 hours
Page 5 of 11Molluscum Contagiosum
14/2/2007http://dermatology.cdlib.org/92/reviews/molluscum/diven.html

before being washed off. Cantharidin can cause severe
blistering. It should be tested on individual lesions before treating
large numbers of lesions. It should not be used on the face. When
tolerated, this treatment is repeated every week until the lesions
clear. Usually 1–3 treatments are necessary.[39]
Iodine solution and salicylic acid plaster
A 10% iodine solution is placed on the molluscum papules
and, when dry, the site is covered with small pieces of 50%
salicylic acid plaster and tape. The process is repeated daily after
bathing. After the lesions have become erythematous in 3–7 days,
only the iodine solution is applied. Resolution has been reported in
a mean of 26 days.[40] Maceration and erosion can result.
Tretinoin
Tretinion 0.1% cream has been used in the treatment of MCV.
It is applied twice daily to the lesions. Resolution was reported by
day 11. Trace erythema at the site of prior lesions was a noted side
effect.[41] Tretinion 0.05% cream has also been used with success
and decreased irritation.[35]
Cimetdine
Oral cimetidine has successfully been used in extensive
infections.[42] The histamine 2-receptor antagonist stimulates
delayed-type hypersensivity. One uncontrolled study showed
resolution in 9 of 13 patients. In this study, the dosage was 40
mg/kg/day in two divided doses for 2 months.[43] The authors
recommended further placebo-controlled, double-blind studies be
completed to determine the efficacy of cimetidine in treating MCV.
Because cimetadine interacts with many systemic medications, a
review of the patient's other medications is recommended.
Potassium hydroxide
Another treatment option is the use of potassium hydroxide. In
one study, an aqueous solution of 10% KOH was applied topically
twice daily to all lesions with a swab. The treatment was
discontinued when an inflammatory response or superficial ulcer
became evident. Resolution occurred in a mean of 30 days.[44]
This treatment had some complications including hypertrophic scar
formation and persistent or transitory hyper- and
Page 6 of 11Molluscum Contagiosum
14/2/2007http://dermatology.cdlib.org/92/reviews/molluscum/diven.html

hypopigmentation. A subsequent study in pediatric patients
recommended the use of 5% KOH and found it equally effective
with many fewer side effects.[45]
Pulsed dye laser
The use of pulsed dye laser for the treatment of MC has also
been documented with excellent results. The therapy was well
tolerated, without scars or pigment anomalies. The lesions resolved
without scarring at 2 weeks. Studies show 96%–99% of the lesions
resolved with one treatment.[46,47] The pulsed dye laser is quick
and efficient, but its expense makes it less cost effective than other
options.
Imiquimod
Imiquimod 5% cream has been used topically to treat MCV by
inducing high levels of IFN-α and other cytokines locally.[48,49]
This potent immunomodulatory agent is well tolerated, although
application site irritation is common. It has had no known systemic
or toxic effects in children.[50] It is applied to the area nightly for 4
weeks. Clearing can take up to 3 months.
Cidofovir
Cidofovir is a nucleoside analog that has potent antiviral
properties. Several small studies and case reports describe the
successful use of cidofovir applied topically or administered by
intralesional injection in several virally induced cutaneous diseases.
[51] Cidofovir cream 3% has been used successfully to treat MCV
in studies, with clearing in 2–6 weeks.[52] Its high cost, need for
extemporaneous preparation, and carcinogenicity in some studies
have limited its use.[51]
Conclusion
Molluscum Contagiosum is a common, generally benign, viral
infection of the skin. It is common in children, sexually active
adults, and immunodeficient patients. It is caused by the
molluscipox virus, a member of the poxviridae family. This virus
differs from other poxviruses in that it causes spontaneously
regressing, umbilicated tumors of the skin rather than poxlike
vesicular lesions. In immunocompetent, nonatopic patients
molluscum contagiosum is usually a self-limited disease for which
Page 7 of 11Molluscum Contagiosum
14/2/2007http://dermatology.cdlib.org/92/reviews/molluscum/diven.html

treatment is not mandatory. However, when treatment is
deemed appropriate, multiple local therapeutic options are
available. For patients with impaired immune functions with
widespread and potentially disfiguring eruptions, the usual local
destructive therapies are ineffective; antiviral and
immunomodulatory medications have been more successful.
References
1. Bateman F. Molluscum contagiosum. In: Shelley WB, Crissey JT, eds. Classics in Dermatology. Springfield IL; Charles C Thomas, 1953, p20. 2. Brown ST, Nalley JF, Kraus SJ. Molluscum contagiosum Sex Transm Dis 1981;8:227-234. 3. Juliusberg M. Zur Kenntnis des virus des Molluscum contagiosum. Dtsch Med Wochenschr 1905;31:1598-1599. 4. Wile and Kingery, J Cutan Dis., 1917 XXVII, p.431. 5. Bretz S. Molluscum Contagiosum. Emedicine Juournal April 25,2001;2(4). 6. Pusey WA. Moluscum contagiosum In: The Principals and Practice of Dermatology, 4th ed. Appleton, 1924, pp 989-990. 7. Douglas JD, Tanner KN, Prine JR, Van Riper DC, Derwelis SK. Molluscum contagiosum in chimpanzees. J Am Vet Med Assoc 1967;151:901-904. 8. Dangall BG, Witson GR: Molluscum contagiosum in a red kangaroo. Australas J Dermatol 1974;15:115. 9. IB Van Resburg, MG Collett, N Ronen, T Gerdes. Molluscum contagiosum in a horse. J S Afr Vet Assoc 1991;62:72-74. 10. Postlethwaite R. Molluscum contagiosum: A review. Arch Environ Health 1970; 21: 432-452. 11. Becker TM, Blout JH, Douglas J, Judson FM. Trends in molluscum cantagiosum in the United States, 1966-1983. Sex Transm Dis 1986;13:88-92. 12. Billstein SA. Mattaliano VJ Jr. The "nuisance" sexually transmitted diseases: Molluscum contagiosum, scabies, and crab lice. Med Clin North Am 1990; 74: 1487-1505. 13. Schwartz JJ. Myskowski PL: Molluscum contagiosum in patients with human immunodefificiency virus infection. J Am
Page 8 of 11Molluscum Contagiosum
14/2/2007http://dermatology.cdlib.org/92/reviews/molluscum/diven.html

Acad Dermatol 1992;27:583. 14. Lombardo PC. Molluscum contagiosum and the acquired immunodeficiency syndrome. Arch Dermatol 1985; 121: 834-835. 15. Scholz J, Rosen-Wolff A, Burgert K et al. Epidemiology of molluscum contagiosum using genetic analysis of the viral DNA. J Med Virol 1989; 27: 87-90. 16. Porter CD, Archard LC: Characterization by restriction mapping of three subtypes of molluscum contagiosum virus. J Med Virol 1992;38:1. 17. Gottlieb SL, Myskowki PL. Molluscum contagiosum. Int J Dermatol 33: 453-461,1994. 18. Yamashita H, Uemura T, Kawashima M. Molecular epidemiologic analysis of Japanese patients with molluscum contagiosum. Int J Dermatol 1996;35:99-105. 19. Nakamura J, Muraki Y, Yamada M, Hatano Y, Nii S. J Med Virol 1995;46(4):339-48. 20. Burgert JJ, Darai G. Recent advances in molluscum contagiosum virus research. Arch Virol Suppl 1997;13:35-47. 21. Diven DG, An overview of poxviruses, J AM Acad Dermatol 2001;44:1-14. 22. Whitaker SB, Wiefand SE, Budnick SD. Inraoral molluscum contagiosum. Oral Surg Oral Med Oral Pathol. 1991;72: 334-336. 23. Ingraham HJ, Schoenleber DB. Epibulbar molluscum contagiousm. Am J ophthalmol 1998;125:394-396. 24. Vannas S, Lapinleimu K. Molluscum contagiosum of the skin, caruncle, and conjunctiva. Acta Ophthalmol 1967;45:314-321. 25. De Oreo GA, Johnson HH, Binkley GW. An eczematous reaction associated with molluscum contagiosum. Arch Dermatol 1956; 74: 344-8. 26. Cotton DW, Cooper C, Barrett DF, Leppard BJ. Severe atypical molluscum contagiosum infection in an immunocommpromised host. Br J Dermatol 1987;116:871-876. 27. Shirodaria PV, Mattews RS. Observations on the antibody responses in molluscum contagiosum. Br J Dermatol 1997;96:29-34. 28. Thompson CH. Identification and typing of molluscum
Page 9 of 11Molluscum Contagiosum
14/2/2007http://dermatology.cdlib.org/92/reviews/molluscum/diven.html

contagiosum virus in clinical specimens by polymerase chain reaction. J Med Virol 1997;53:205-211. 29. Hovenden JL, Bushhell TE. Molluscum contagiosum: possible culture misdiagnosis as herpes simplex[letter]. Genitourin Med 1991;67:270. 30. Fife KH, Whitfield M, Faust H, Goheen MP, Bryan J, Brown DR. Growth of molluscum contagiosum virus in a human foreskin xenograft model. Virology 1996;226:95-101. 31. Buller RM, Burnett J Chen W, Kreider J. Replication of molluscum contagiosum virus. Virology 1995;213:655-659. 32. Penneys NJ, Matsuo S, Mogollon R. The identification of molluscum infection of immunohistochemical means. J Cutan Pathol 1986;13:97-101. 33. Thompson CH, Biggs IM, DeZwart-Steffe RT. Detection of molluscum contagiosum virus DNA by in-situ hybridization. Pathology 1990;22:181-186. 34. Janniger CK, Schwartz RA. Molluscum Contagiosum in children. Cutis 1993;52: 194-196. 35. Valentine CL, Diven DG, Treatment modalities for molluscum contagiosum. Dermatologic Therapy 2000;13: 285-289. 36. Epstein WL. Molluscum contagiosum. Semin Dermatol 1992;11: 184-189. 37. Janniger CK, Schwartz RA. Molluscum Contagiosum in children. Cutis 1993; 52: 194-196. 38. Arndt KA. Manualof dermatologic therapeutics, 5th ed. Boston: Little Brown, 339-340, 1995. 39. Silverburg NB, Sidbury R, Mancini AJ. Childhood molluscum contagiosum: Experience with cantharidin therapy in 300 patients. J Am Acad Dermatol 2000;43: 503-507. 40. Ohkuma M. Molluscum contagiosum treated with iodine solution and salicylic acid plaster. Int J Dermatol 1990;29:443-445. 41. Papa CM, Berger RS. Venereal herpes-like molluscum contagiosum: treatment with tretinoin. Curis 1976;18:537-540. 42. Avella J, Binder H, Madsen J, Ashkenase P. Effect of histamine H2 receptor antagonists on delayed hypersensitivity. Lancet 1978:1:624-626.
Page 10 of 11Molluscum Contagiosum
14/2/2007http://dermatology.cdlib.org/92/reviews/molluscum/diven.html

43. Dohil M, Prendiville JS. Treatment of Molluscum contagiosum with oral cimetidine: clinical experience on 13 patients. Pediatric Dermatol 13:310-312. 44. Romiti R, Ribeiro AP, Grinblat BM. Treatment of molluscum contagiosum with potassium hydroxide: A clinical approach in 35 children. Pediatr Dermatol 1999;16: 228-231. 45. Romiti R, Ribeiro AP, Romiti N. Evaluation of the effectiveness of 5% potassium hydroxide for the treatment of molluscum contagiosum. Pediatr Dermatol 2000;17(6):495. 46. Hammes S, Greve B, Raulin C. [Molluscum contagiosum: treatment with pulsed dye laser] Hautarzt 2001;52;38-42. 47. Hughes PS. Treatment of molluscum contagiosem with the 585-nm pulsed dye laser. Dermatol Surg 1998;24: 229-230. 48. Hengge UR, Esser S, Schultewolter T, Behrendt C, Meyer T, Stockfleth E. Goos M. Self administered topical 5% imiquimod for the treatment of common warts and molluscum contagiosum. British Journal of Dermatology 2000;143: 1026-1031. 49. Tyring SK, Arany I, Stanley MA et al. A randomized, controlled, molecular study of condylomata acuminate clearance during treatment with imiquimod. J Infec Dis 1998;178:551-5. 50. Barba Ar, Kapoor S, Berman B. An open label safety study of topical imiquimod 5% cream in the treatment of Molluscum contagiosum in children. Dermatol Online J 2001; Vol 7(1), 20. 51. Zabawski EJ Jr. A review of topical and intralesional cidofovir. Dermatology Online J 2000;6(1):3 52. Zabawaski EJ Jr, Cockerell CJ. Topical cidofovir for molluscum contagiosum in children[letter] Pediatr Dermatol 1999;16(5):414-415.© 2003 Dermatology Online Journal
© 2003 Dermatology Online Journal
Page 11 of 11Molluscum Contagiosum
14/2/2007http://dermatology.cdlib.org/92/reviews/molluscum/diven.html