Medical Nutrition Therapy for Liver, Biliary System, and Exocrine Pancreas Disorders Chapter 31.
-
Upload
amy-haynes -
Category
Documents
-
view
234 -
download
2
Transcript of Medical Nutrition Therapy for Liver, Biliary System, and Exocrine Pancreas Disorders Chapter 31.

Medical Nutrition Therapy for Liver, Biliary System, and Exocrine Pancreas Disorders
Medical Nutrition Therapy for Liver, Biliary System, and Exocrine Pancreas Disorders
Chapter 31Chapter 31

© 2004, 2002 Elsevier Inc. All rights reserved.
Hepatic FunctionsHepatic Functions
Macronutrient metabolism
– CHO: glycogenesis, glycogenolysis, gluconeogenesis, converts fructose & galactose to glucose, breaks down glucose for energy as needed
– Lipids: builds/breaks down TG, phospholipids, and Chol as needed, breaks down FA for energy, packages extra lipids in lipoproteins for transport to other body organs, manufactures bile and ketones when necessary
Macronutrient metabolism
– CHO: glycogenesis, glycogenolysis, gluconeogenesis, converts fructose & galactose to glucose, breaks down glucose for energy as needed
– Lipids: builds/breaks down TG, phospholipids, and Chol as needed, breaks down FA for energy, packages extra lipids in lipoproteins for transport to other body organs, manufactures bile and ketones when necessary

© 2004, 2002 Elsevier Inc. All rights reserved.
Hepatic Functions Hepatic Functions
Proteins: manufactures nonessential AA when needed, removes excess AA, removes ammonia and converts it to urea, makes other nitrogen-containing compounds the body needs, makes plasma proteins such as clotting factors
Other: detoxifies alcohol, drugs & poisons, helps dismantle old RBCs & recycles Fe, stores most vit/min’s, forms lymph, provides filter/flood chamber
Proteins: manufactures nonessential AA when needed, removes excess AA, removes ammonia and converts it to urea, makes other nitrogen-containing compounds the body needs, makes plasma proteins such as clotting factors
Other: detoxifies alcohol, drugs & poisons, helps dismantle old RBCs & recycles Fe, stores most vit/min’s, forms lymph, provides filter/flood chamber

© 2004, 2002 Elsevier Inc. All rights reserved.
Common Laboratory Tests Used to Test for Liver FunctionCommon Laboratory Tests Used to Test for Liver Function
Hepatic excretion
—Total serum bilirubin, urine bilirubin
Cholestasis tests
—Serum alkaline phosphatase
Hepatic enzymes
—ALT, AST
Hepatic excretion
—Total serum bilirubin, urine bilirubin
Cholestasis tests
—Serum alkaline phosphatase
Hepatic enzymes
—ALT, AST

© 2004, 2002 Elsevier Inc. All rights reserved.
Common Laboratory Tests Used to Test for Liver Function—cont’dCommon Laboratory Tests Used to Test for Liver Function—cont’d
Serum proteins
—PT, PTT, serum albumin
Markers of specific liver diseases
—Serum ferritin, ceruloplasmin
Specific tests for viral hepatitis
—IgM anti-HAV, anti-HBS, HCV-RNA
Serum proteins
—PT, PTT, serum albumin
Markers of specific liver diseases
—Serum ferritin, ceruloplasmin
Specific tests for viral hepatitis
—IgM anti-HAV, anti-HBS, HCV-RNA

© 2004, 2002 Elsevier Inc. All rights reserved.
Diseases of the LiverDiseases of the Liver
Acute viral hepatitis
Fulminant hepatitis
Chronic hepatitis
Alcoholic liver disease, alcoholic hepatitis, and cirrhosis
Acute viral hepatitis
Fulminant hepatitis
Chronic hepatitis
Alcoholic liver disease, alcoholic hepatitis, and cirrhosis

© 2004, 2002 Elsevier Inc. All rights reserved.
Diseases of the Liver—cont’dDiseases of the Liver—cont’d
Cholestatic liver diseases
—Primary biliary cirrhosis
—Sclerosing cholangitis
Inherited disorders
Other liver diseases
Cholestatic liver diseases
—Primary biliary cirrhosis
—Sclerosing cholangitis
Inherited disorders
Other liver diseases

© 2004, 2002 Elsevier Inc. All rights reserved.
Acute Viral HepatitisAcute Viral Hepatitis
Widespread inflammation of the liver that is caused by hepatitis viruses A, B, C, D, and E
Four phases of symptoms:
1. Prodromal phase
2. Preicteric phase
3. Icteric phase
4. Convalescent phase
Widespread inflammation of the liver that is caused by hepatitis viruses A, B, C, D, and E
Four phases of symptoms:
1. Prodromal phase
2. Preicteric phase
3. Icteric phase
4. Convalescent phase

© 2004, 2002 Elsevier Inc. All rights reserved.
Fulminant HepatitisFulminant Hepatitis
Syndrome in which severe liver dysfunction is accompanied by hepatic encephalopathy
Syndrome in which severe liver dysfunction is accompanied by hepatic encephalopathy

© 2004, 2002 Elsevier Inc. All rights reserved.
Chronic HepatitisChronic Hepatitis
At least 6-month course of hepatitis or biochemical and clinical evidence of liver disease with confirmatory biopsy findings of unresolving hepatic inflammation
At least 6-month course of hepatitis or biochemical and clinical evidence of liver disease with confirmatory biopsy findings of unresolving hepatic inflammation

© 2004, 2002 Elsevier Inc. All rights reserved.
Most Common Liver DiseaseMost Common Liver Disease
Alcohol excess and abuse
Fourth leading cause of death among middle-aged Americans
Alcohol problems are highest among young adults, ages 18 to 29.
Alcohol excess and abuse
Fourth leading cause of death among middle-aged Americans
Alcohol problems are highest among young adults, ages 18 to 29.

© 2004, 2002 Elsevier Inc. All rights reserved.
Alcoholic Liver DiseaseAlcoholic Liver Disease
Disease resulting from excessive alcohol ingestion characterized by fatty liver (hepatic steatosis), hepatitis, or cirrhosis
Disease resulting from excessive alcohol ingestion characterized by fatty liver (hepatic steatosis), hepatitis, or cirrhosis

© 2004, 2002 Elsevier Inc. All rights reserved.
Complications of Excessive Alcohol Consumption Stem Largely from Excess Hydrogen and from AcetaldehydeComplications of Excessive Alcohol Consumption Stem Largely from Excess Hydrogen and from Acetaldehyde

© 2004, 2002 Elsevier Inc. All rights reserved.
Alcoholic Liver DiseaseMetabolic ChangesAlcoholic Liver DiseaseMetabolic Changes
Steatorrhea
Wernicke-Korsakoff syndrome
Peripheral neuropathy
Pellagrous psychosis
Folate deficiency
Steatorrhea
Wernicke-Korsakoff syndrome
Peripheral neuropathy
Pellagrous psychosis
Folate deficiency

© 2004, 2002 Elsevier Inc. All rights reserved.
End-Stage Alcoholic Liver DiseasePossible CharacteristicsEnd-Stage Alcoholic Liver DiseasePossible Characteristics
Malnutrition
Portal hypertension with varices
Ascites
Hyponatremia
Hepatic encephalopathy
Glucose alterations
Malnutrition
Portal hypertension with varices
Ascites
Hyponatremia
Hepatic encephalopathy
Glucose alterations

© 2004, 2002 Elsevier Inc. All rights reserved.
End-Stage Alcoholic Liver DiseasePossible Characteristics—cont’dEnd-Stage Alcoholic Liver DiseasePossible Characteristics—cont’d
Fat malabsorption
Osteopenia
Thrombocytopenia with anemia
Fat malabsorption
Osteopenia
Thrombocytopenia with anemia

© 2004, 2002 Elsevier Inc. All rights reserved.
Cholestatic Liver DiseasesCholestatic Liver Diseases
Primary biliary cirrhosis (PBC)
—An immune-mediated chronic cirrhosis of the liver due to obstruction or infection of the small and intermediate-sized intrahepatic bile ducts, whereas the extrahepatic biliary tree and larger intrahepatic ducts are normal
—90% of patients are women
Primary biliary cirrhosis (PBC)
—An immune-mediated chronic cirrhosis of the liver due to obstruction or infection of the small and intermediate-sized intrahepatic bile ducts, whereas the extrahepatic biliary tree and larger intrahepatic ducts are normal
—90% of patients are women

© 2004, 2002 Elsevier Inc. All rights reserved.
Cholestatic Liver Diseases—cont’dCholestatic Liver Diseases—cont’d
Sclerosing cholangitis
—Fibrosing inflammation of segments of extrahepatic bile ducts, with or without involvement of intrahepatic ducts
Sclerosing cholangitis
—Fibrosing inflammation of segments of extrahepatic bile ducts, with or without involvement of intrahepatic ducts

© 2004, 2002 Elsevier Inc. All rights reserved.
Inherited DisordersInherited Disorders
Hemochromatosis
—Inherited disease of iron overload
Wilson’s disease
—Autosomal recessive disorder associated with impaired biliary copper excretion
α1-antitrypsin deficiency
—Causes cholestasis or cirrhosis and can cause liver and lung cancer
Hemochromatosis
—Inherited disease of iron overload
Wilson’s disease
—Autosomal recessive disorder associated with impaired biliary copper excretion
α1-antitrypsin deficiency
—Causes cholestasis or cirrhosis and can cause liver and lung cancer

© 2004, 2002 Elsevier Inc. All rights reserved.
Other Liver DiseasesOther Liver Diseases
Several other causes of liver disease, including
—Liver tumors
—Systemic diseases (rheumatoid arthritis, systemic sclerosis)
—Nonalcoholic steatohepatitis
—Acute ischemic and chronic congestive hepatopathy
—Parasitic, bacterial, fungal, and granulomatous liver diseases
Several other causes of liver disease, including
—Liver tumors
—Systemic diseases (rheumatoid arthritis, systemic sclerosis)
—Nonalcoholic steatohepatitis
—Acute ischemic and chronic congestive hepatopathy
—Parasitic, bacterial, fungal, and granulomatous liver diseases

© 2004, 2002 Elsevier Inc. All rights reserved.
Normal Liver vs. Damaged LiverNormal Liver vs. Damaged Liver

© 2004, 2002 Elsevier Inc. All rights reserved.
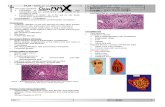
Microscopic Appearance of (A) a Normal Liver and (B) Acute Fatty LiverMicroscopic Appearance of (A) a Normal Liver and (B) Acute Fatty Liver
(Adapted from Bray GA. Gray DS, Obesity, part 1: Pathogenisis. West J Med 149:429, 1988; and Lew EA, Garfinkle L; Variations in mortality by weight among 750,000 men and women. J Clin Epidemiol 32:563, 1979.)(From Kanel G, Korula J. Atlas of Liver Pathology. W.B. Saunders, 1992.)

© 2004, 2002 Elsevier Inc. All rights reserved.
Clinical Manifestations of CirrhosisClinical Manifestations of Cirrhosis

© 2004, 2002 Elsevier Inc. All rights reserved.
Clinical Manifestations of CirrhosisClinical Manifestations of Cirrhosis

© 2004, 2002 Elsevier Inc. All rights reserved.
Factors That Affect Interpretation of Objective Nutrition Assessment Tests in Patients with End-Stage Liver Disease
Factors That Affect Interpretation of Objective Nutrition Assessment Tests in Patients with End-Stage Liver Disease
Body weight
Anthropometric measurements
Creatinine-height index
Nitrogen balance studies
Body weight
Anthropometric measurements
Creatinine-height index
Nitrogen balance studies
3-methylhistidine excretion
Visceral protein levels
Immune function tests
3-methylhistidine excretion
Visceral protein levels
Immune function tests

© 2004, 2002 Elsevier Inc. All rights reserved.
SGA Parameters for Nutritional Evaluation of Liver Disease PatientsSGA Parameters for Nutritional Evaluation of Liver Disease Patients
History –wt changes/fluctuations,diet, appetite, taste changes, early satiety, GI problems
Physical- muscle wasting, fat stores, fluid status(edema/ascites)
Existing conditions-disease state/other problems that may affect nutritional status
Nutritional rating (based on results of above parameters)
History –wt changes/fluctuations,diet, appetite, taste changes, early satiety, GI problems
Physical- muscle wasting, fat stores, fluid status(edema/ascites)
Existing conditions-disease state/other problems that may affect nutritional status
Nutritional rating (based on results of above parameters)

© 2004, 2002 Elsevier Inc. All rights reserved.
Severe Malnutrition and Ascites in a Man with End-Stage Liver DiseaseSevere Malnutrition and Ascites in a Man with End-Stage Liver Disease

© 2004, 2002 Elsevier Inc. All rights reserved.
Malnutrition in Liver Disease—CauseMalnutrition in Liver Disease—Cause
Algorithm content developed by John Anderson, PhD, and Sanford C. Garner, PhD, 2000. Updated by Jeanette M. Hasse and Laura E. Matarese, 2002.

© 2004, 2002 Elsevier Inc. All rights reserved.
Malnutrition in Liver Disease—PathophysiologyMalnutrition in Liver Disease—Pathophysiology
Algorithm content developed by John Anderson, PhD, and Sanford C. Garner, PhD, 2000. Updated by Jeanette M. Hasse and Laura E. Matarese, 2002.

© 2004, 2002 Elsevier Inc. All rights reserved.
Malnutrition in Liver Disease—Medical and Nutritional ManagementMalnutrition in Liver Disease—Medical and Nutritional Management
Algorithm content developed by John Anderson, PhD, and Sanford C. Garner, PhD, 2000. Updated by Jeanette M. Hasse and Laura E. Matarese, 2002.

© 2004, 2002 Elsevier Inc. All rights reserved.
Vitamin/Mineral Deficits in Severe Hepatic FailureVitamin/Mineral Deficits in Severe Hepatic Failure
Vitamin A
Vitamin D
Vitamin E
Vitamin K
Vitamin B6
Vitamin B12
Folate
Vitamin A
Vitamin D
Vitamin E
Vitamin K
Vitamin B6
Vitamin B12
Folate
Niacin
Thiamin
Zinc
Magnesium
Iron
Potassium
Phosphorus
Niacin
Thiamin
Zinc
Magnesium
Iron
Potassium
Phosphorus

© 2004, 2002 Elsevier Inc. All rights reserved.
Four Stages of Hepatic EncephalopathyFour Stages of Hepatic Encephalopathy
Stage Symptom
I Mild confusion, agitation, irritability, sleep disturbance, decreased attention
II Lethargy, disorientation, inappropriate behavior, drowsiness
III Somnolence but arousable, incomprehensible speech, confusion, aggression when awake
IV Coma
Stage Symptom
I Mild confusion, agitation, irritability, sleep disturbance, decreased attention
II Lethargy, disorientation, inappropriate behavior, drowsiness
III Somnolence but arousable, incomprehensible speech, confusion, aggression when awake
IV Coma

© 2004, 2002 Elsevier Inc. All rights reserved.
End-Stage Liver DiseaseHepatic EncephalopathyEnd-Stage Liver DiseaseHepatic Encephalopathy
1. Consider major causes of encephalopathy
• GI bleeding
• Fluid and electrolyte abnormalities
• Uremia
• Use of sedatives
• Hypo- or hyperglycemia
• Alcohol withdrawal
• Constipation
• Acidosis
1. Consider major causes of encephalopathy
• GI bleeding
• Fluid and electrolyte abnormalities
• Uremia
• Use of sedatives
• Hypo- or hyperglycemia
• Alcohol withdrawal
• Constipation
• Acidosis

© 2004, 2002 Elsevier Inc. All rights reserved.
End-Stage Liver DiseaseHepatic Encephalopathy—cont’dEnd-Stage Liver DiseaseHepatic Encephalopathy—cont’d
2. Treat underlying cause.
3. Treat with medications.
• Lactulose
• Neomycin
4. Ensure adequate diet is consumed.
2. Treat underlying cause.
3. Treat with medications.
• Lactulose
• Neomycin
4. Ensure adequate diet is consumed.

© 2004, 2002 Elsevier Inc. All rights reserved.
End-Stage Liver Disease End-Stage Liver Disease
Energy: 30 to 35 kcal/kg dry weight
BEE x 1.2 to 1.5, depending on degree of malnutrition
Fat: 25% to 40% of kcal
May try MCT if steatorrhea is present; with severe case, try fat restriction and discontinue if diarrhea does not improve
Protein: 1to 1.5 g/kg dry wt depending on degree of malnutrition, malabsorption, metabolic stress
Energy: 30 to 35 kcal/kg dry weight
BEE x 1.2 to 1.5, depending on degree of malnutrition
Fat: 25% to 40% of kcal
May try MCT if steatorrhea is present; with severe case, try fat restriction and discontinue if diarrhea does not improve
Protein: 1to 1.5 g/kg dry wt depending on degree of malnutrition, malabsorption, metabolic stress

© 2004, 2002 Elsevier Inc. All rights reserved.
End-Stage Liver Disease—cont’dEnd-Stage Liver Disease—cont’d
May try BCAA formulas for >grade 2 encephalopathy
CHO: high intake of both complex and simple carbohydrates
Vitamin and mineral supplements
Electrolytes: restrict sodium with edema or ascites (2-4 g/day)
Fluid: restrict fluid if hyponatremia is present
May try BCAA formulas for >grade 2 encephalopathy
CHO: high intake of both complex and simple carbohydrates
Vitamin and mineral supplements
Electrolytes: restrict sodium with edema or ascites (2-4 g/day)
Fluid: restrict fluid if hyponatremia is present

© 2004, 2002 Elsevier Inc. All rights reserved.
Amino Acids Commonly Altered in Liver DiseaseAmino Acids Commonly Altered in Liver Disease
Aromatic amino acids—serum levels increased
—Tyrosine
—Phenylalanine*
—Free tryptophan* Branched-chain amino acids—serum levels decreased
—Valine*
—Leucine*
—Isoleucine* Other amino acids—serum levels increased
—Methionine*
—Glutamine
Aromatic amino acids—serum levels increased
—Tyrosine
—Phenylalanine*
—Free tryptophan* Branched-chain amino acids—serum levels decreased
—Valine*
—Leucine*
—Isoleucine* Other amino acids—serum levels increased
—Methionine*
—Glutamine
—Asparagine—Histidine*
—Asparagine—Histidine*
* Denotes essentials amino acids* Denotes essentials amino acids

© 2004, 2002 Elsevier Inc. All rights reserved.
SummarySummary
Liver disorders—role of liver is so crucial to overall health, its destruction is quite serious
Goals—support maintenance of as much normal liver function as possible
Transplantation, if needed
Liver disorders—role of liver is so crucial to overall health, its destruction is quite serious
Goals—support maintenance of as much normal liver function as possible
Transplantation, if needed

© 2004, 2002 Elsevier Inc. All rights reserved.
Medications Commonly Used after Liver TransplantationMedications Commonly Used after Liver Transplantation
Azathioprine
Antithymocyte globulin
Basiliximab
Cyclosporine
Daclizumab
Glucocorticoids
Azathioprine
Antithymocyte globulin
Basiliximab
Cyclosporine
Daclizumab
Glucocorticoids
Muromonab-CD3
Mycophenolate mofetil
Sirolimus
Tacrolimus
15-deoxysperagualin
Muromonab-CD3
Mycophenolate mofetil
Sirolimus
Tacrolimus
15-deoxysperagualin

© 2004, 2002 Elsevier Inc. All rights reserved.
Nutrition Care Guidelines for Liver TransplantationNutrition Care Guidelines for Liver Transplantation
Pretransplantation
Immediate posttransplantation
Long-term posttransplantation
Pretransplantation
Immediate posttransplantation
Long-term posttransplantation
Calories
Protein
Fat
Carbohydrate
Sodium
Fluid
Calcium
Vitamins
Calories
Protein
Fat
Carbohydrate
Sodium
Fluid
Calcium
Vitamins

© 2004, 2002 Elsevier Inc. All rights reserved.
Liver Transplantation—DietLiver Transplantation—Diet
Nutrition support: pre- and posttransplant
Long-term preventive nutrition to optimize health and to avoid or minimize
—Excessive weight gain
—Hyperlipidemia
—Hyperglycemia
—Hypertension
—Osteopenia
Nutrition support: pre- and posttransplant
Long-term preventive nutrition to optimize health and to avoid or minimize
—Excessive weight gain
—Hyperlipidemia
—Hyperglycemia
—Hypertension
—Osteopenia

© 2004, 2002 Elsevier Inc. All rights reserved.
Relationship of Organs of the Upper AbdomenRelationship of Organs of the Upper Abdomen
A, Liver (retracted upward); B, gallbladder; C, esophageal opening of the stomach; D, stomach (shown in dotted outline); E, common bile duct; F, duodenum; G, pancreas and pancreatic duct; H, spleen; I, kidneys.
Courtesy The Cleveland Clinic Foundation, Cleveland, Ohio, 2002.

© 2004, 2002 Elsevier Inc. All rights reserved.
Some Tests of Pancreatic FunctionSome Tests of Pancreatic Function

© 2004, 2002 Elsevier Inc. All rights reserved.
Pancreatic Disorders—CausePancreatic Disorders—Cause
Algorithm content developed by John Anderson, PhD, and Sanford C. Garner, PhD, 2000.

© 2004, 2002 Elsevier Inc. All rights reserved.
Pancreatic Disorders—PathophysiologyPancreatic Disorders—Pathophysiology
Algorithm content developed by John Anderson, PhD, and Sanford C. Garner, PhD, 2000.

© 2004, 2002 Elsevier Inc. All rights reserved.
Pancreatic Disorders—Medical and Nutritional ManagementPancreatic Disorders—Medical and Nutritional Management
Algorithm content developed by John Anderson, PhD, and Sanford C. Garner, PhD, 2000. Updated by Jeanette M. Hasse and Laura E. Matarese, 2002.