March 29, 2011. Attempt to pass NG tube Esophageal atresia Choanal atresia Half have other...
-
Upload
jeffry-atkinson -
Category
Documents
-
view
223 -
download
0
Transcript of March 29, 2011. Attempt to pass NG tube Esophageal atresia Choanal atresia Half have other...

SURGERY BOARD REVIEWMarch 29, 2011

RESPIRATORY DISTRESS

UPPER AIRWAY
Attempt to pass NG tube Esophageal atresia Choanal atresia
Half have other congenital anomaly
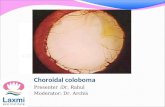
CHARGE Syndrome Coloboma Heart Atresia of choanae Retarded development Genital hypoplasia Ear

CHOANAL ATRESIA
Membranous 90% Bony 10% Gavage feed until repair Maintain oral airway

MACROGLOSSIA
True enlargement of tongue Vs. Glossoptosis in which normal tongue
protrudes from abnormally small oral cavity
Focal (pebbly, vescicle-like blebs) Congenital tumors (lymphangioma,
hemangioma) One-half
Hemihypertrophy

MACROGLOSSIA
Generalized (smooth surface) Beckwith-Wiedemann, hypothyroidism
Generalized (papillary, fissured) Down syndrome
Also poor tone
Progressive Mucopolysaccharidoses

QUESTION 1
This child was most likely to have which of the following metabolic abnormalities as a newborn?
A Hyperkalemia B Hypokalemia C Hyponatremia D Hypoglycemia E Metabolic Acidosis

BECKWITH WIEDEMANN SYN
Features Macroglossia Macrosomia Hypoglycemia (islet cell hyperplasia) Hemihypertrophy Hypospadias Omphalocele
18 month old with B.W. presents with gross hematuria: Wilms Tumor

PIERRE ROBIN SEQUENCE
Unusually small mandible (micrognathia) Posteriorly displaced
tongue Upper airway obstruction U-shaped cleft palate
May be part of a larger syndrome

LARYNGEAL LESIONS
Hoarseness Faint cry Aphonia Associated dyspnea

THORACIC LESIONS

QUESTION 2
Which is the most common abnormality?
A B C D E

TE fistulae: Most common types… 1 Esophageal atresia and distal fistula 2 Esophageal atresia and no fistula 3 H-Type (only one without atresia)
Manifestation may not be as severe
1 32

TE FISTULA
Inability to pass NG tube Use to drain secretions
Resp distress secondary Fistula Reflux of pouch contents
Inability to tolerate initial feed Excessive drooling May see distension of stomach (air fistula)
Avoid positive pressure ventilation Antenatal U/S: Microgastria, polyhydramnios

PURE ESOPHAGEAL ATRESIA
Dilated proximal pouch Gasless
abdomen Scaphoid
abdomen

BRONCHOPULMONARY FOREGUT MALFORMATION

BRONCHOPULMONARY FOREGUT MALFORMATION
Congenital Lobar Emphysema Congenital cystic adenomatoid
malformation Pulmonary sequestration Bronchogenic cyst

PULMONARY SEQUESTRATION
Portion of lungs perfused by systemic arteries Lacks normal connection with tracheobronchial
tree Intralobar:
Most common lower lobes Anywhere in thorax
Extralobar: Subdiaphragmatic or retroperitoneal Associated with other anomalies
Dx: MRI or angiogram

PULMONARY SEQUESTRATION

BRONCHOGENIC CYST
Occur any point along the tracheobronchial tree Centrally located
Does not communicate, fluid fill with wall composed of tissue resembling large airways
Typically present 2nd decade of life with recurrent wheezing, cough, pneumonia

BRONCHOGENIC CYST

CONGENITAL PULMONARY AIRWAY MALFORMATION (CPAM)
Previously known as Congenital Cystic Adenomatoid Malformation (CCAM)
Hamartomatous lesion Cystic and adenomatous elements
Resp distress, recurrent PNA, asymptomatic
Severe forms can be lethal after birth Surgical resection if symptomatic
Controversial if asymptomatic

CONGENITAL PULMONARY AIRWAY MALFORMATION (CPAM)

CONGENITAL LOBAR EMPHYSEMA
Results from area of poorly developed or absent cartilage
Check-valve effect Air trapping Lung hyperexpansion
Possible acute decompensation with positive pressure ventilation

GI OBSTRUCTION

GI OBSTRUCTION
Bilious emesis is always considered a red flag for mechanical obstruction.
Surgical emergency until proven otherwise

NONBILIOUS EMESIS IN INFANTS
Most common cause is overfeeding Second most common: GE Reflux

HYPERTROPHIC PYLORIC STENOSIS
Fairly common 1:300 Unknown genetic link Vomiting starts by 2wks old
Progressively projectile Age at presentation
Most commonly b/f 1 month Remember: 2wks-2months
Male predominance Firstborn

PYLORIC STENOSIS
Clinical Manifestations: Abdomen probably will not be distended
Can feed them to look for signs Distended over stomach immediately after
feeding Peristaltic waves Palpable olive
After vomiting Epigastric b/w midline and R midclavicular line

PYLORIC STENOSIS
Diagnosis Palpable Olive (no imaging required) Hypochloremic, hypokalemic
metabolic alkalosis Ultrasonography
Pyloric muscle Thickness 3-4mm Length 15-16mm

DIAGNOSIS
Upper GI the "string" sign the "double-track" sign the "beak" sign the "shoulder" sign

PYLORIC STENOSIS
Surgical treatment (pyloromyotomy) Fluid and electrolyte correction are
most important Surgery after these are corrected

QUESTION 3
You are working up a 4 month old infant with bilious vomiting. Findings on barium enema reveal cecum located in left upper abdomen. The most likely diagnosis is: A situs inversus B malrotation C intussusception D intestinal duplication

BILIOUS VOMITING IN INFANT Malrotation with midgut volvulus

MALROTATION WITH MIDGUT VOLVULUS
Proximal obstruction at distal duodenum/ proximal jejunum Bilious emesis May not have significant abdominal
distention until late Late finding: hematemesis,
hematochezia Bowel ischemia leading to perforation
and death

MALROTATION WITH MIDGUT VOLVULUS Diagnosis
Suspect in setting of: Bilious vomiting in infant (or older child) Abdominal films:
Gastric distention and duodenal dilatation Otherwise gasless abdomen



MALROTATION
Surgical correction Ladd Procedure
Division of Ladd bands Appendectomy Widening of mesentery Securing intestines in position of
nonrotation

DUODENAL ATRESIA
Bilious vomiting shortly after birth
May occur later Annular pancreas Duodenal stenosis Duodenal web Ladd bands
Associated with Down Syn and congenital heart disease in 30-50%

MECONIUM ILEUS
20% of patients with CF Meconium ileus is CF until proven
otherwise Intraluminal obstruction by thickened
meconium Distal ileum is small, may have
microcolon Possible proximal bowel dilitation “soap bubble” appearance

MECONIUM ILEUS
Contrast enema (may be temporarily therapeutic) Microcolon Inspissated meconium “rabbit pellets”
May perforate Intraperitoneal calcifications and
ascites prenatally

QUESTION 4 You are seeing a new 9
month old who has had difficultly stooling since birth. You see in the records that this imaging has recently been performed • Which information is FALSE?• A Rectal suction biopsy should be done• B Identification of transition zone is helpful• C Development of explosive diarrhea fits
with diagnosis• D Barium enema should be performed
following GI cleanout

HIRSCHSPRUNG DISEASE
Absence of ganglion cells in distal rectum
Bilious emesis and abdominal distention
BE: proximally dilated bowel (normal) Transition zone Distal decompressed segment (abnormal)
Barium study should preceed rectal exam or enemas
Definitive: rectal suction biopsy

HIRSCHSPRUNG DISEASE
May be diagnosed in older child with chronic constipation Requiring rectal stimulation to evacuate
Lifethreatening hirschsprung-related enterocolitis Explosive diarrhea Toxic megacolon Sepsis

INTUSSUSCEPTION
6mos-2yrs Older children more likely to have lead
point Meckel Polyp Lymphoma Intestinal duplication cyst Hematoma/inflammation
Hemophilia, HSP

INTUSSUSCEPTION
Classic location: ileocolic (may be ileo-ileal if there is a lead point)
Presentation Paroxysmal bouts of severe colicky
abdominal pain Drawing up legs Period of somnolence Normal activity between episodes
Unexplained lethargy or seizure-like episode

INTUSSUSCEPTION
Emesis may turn bilious late in course Current jelly stool: late finding “sausage-shaped mass” RUQ

INTUSSUSCEPTION
Evaluation: Start with plain films
Crescent sign, target sign If suspicion high, can go straight to air
contrast or barium enema Diagnostic and therpeutic
Emergent surgery if enema unsuccessful May recur in first 12 to 24 hrs

GI BLEEDING

NEWBORN
Swallowed maternal blood Apt-downey test Mix serum with sodium hydroxide
Pink: newborn Brown: swallowed maternal blood
Vitamin K Anal stenosis (fissures) Hirschsprung Severe gastritis or AGE NEC

NEC
Acute illness of unclear etiology associated with intestinal necrosis Inflammation Invasion of enteric gas forming organisms Dissection of gas into the muscularis and portal venous
system 1-3/1000 live births Incidence decreases with increasing gestational
age 13% occur in term infants
Preexisting illness is common Mortality rate 20-30%

NEC
Presentation Nonspecific systemic signs in a fed, well infant
Apnea Respiratory failure Lethargy Poor feeding Temp instability Abdominal signs
Distention Gastric retention Tenderness Vomiting Diarrhea Gross bleeding

NEC
Diagnosis Abdominal distention Rectal bleeding Abdominal radiographs
Early - abnormal gas pattern with dilated loops c/w ileus
Pneumatosis intestinalis Bubbles of gas in the
bowel wall Portal air: late finding If perforation suspected
Cross-table lateral Left lateral decubitus
Sentinel loop Abdominal ultrasound

NEC
Diagnosis Nonspecific
Blood studies CBC Coags
DIC Chemistries
Stool analysis Occult blood
Sepsis evaluation 20-30%

NEC
Management
Supportive care Bowel rest and decompression with intermittent suction TPN Fluid replacement CV support Resp support Hematologic support Metabolic support
Surgical intervention Reserved for perforation, obstruction

NEC
Management Antibiotic therapy
Vanc, gent, clinda Vanc, gent, flagyl Vanc, gent, zosyn Term infants
Amp, gent and clinda 10-14 day course
Unless complication

TODDLER GI BLEEDING
Painless rectal bleeding Meckel diverticulum
Can have massive bleeding Dx: technetium-99m pertechnetate isotope
scan False negatives possible
May present with complications: Volvulus Internal hernia Intussusception Acute inflammation (similar to appendicitis)

ESOPHAGEAL VARICES
Massive upper GI bleeding Portal HTN
Portal vein thrombosis h/o UVC
Hepatic cirrhosis Chronic liver failure
TPN-related liver disease Biliary atresia s/p Kasai Cystic fibrosis a1- antitrypsin deficiency Viral hepatitis

ESOPHAGEAL VARICES
Treatment Endoscopy
Direct visualization Banding Sclerosant techniques
Transjugular intracaval portosystemic shunting

DON’T FORGET
HSP (Henoch-Schonlein Purpura) Vasculitic conditions Arthralgias Palpable purpuric rash
Buttocks Lower extremities
NORMAL CBC HUS (Hemolytic Uremic Syndrome)
Renal failure, anemia, thrombocytopenia Very sick!!

OLDER CHILDREN
Benign hamartomatous juvenile polyps Age 2-8 Painless, low volume, streaks on stool Autonecrosis and slough into stool May prolapse through anus Surgical or endoscopic resection is
therapeutic

QUESTION 5
This 10 y/o child has had recurrent lower GI bleeding. What is your diagnosis? A Peutz-Jeghers B Familial adenomatous polyposis C Gardner’s Syndrome D Hereditary Hemorrhagic
Telangectasias

FAMILIAL POLYP DISORDERS Gardner’s
Polyps of small and large bowel: premalignant
Extra teeth Osteomas AD inheritance Surgical resection
Peutz-Jeghers Hamartomatous polyps:
premalignant Melanotic mucocutaneous
pigmentation lips, gums AD inheritance Surgical resection

DON’T FORGET
Maintain high index of suspicion for appendicitis Rare in toddlers, but 75% rupture prior to dx Don’t expect them to fit classic picture Obturator and psoas signs may help
In Children, classic features (pain followed by vomiting, fever, anorexia, migration to RLQ, rebound) neither sensitive nor specific Lack of migration to RLQ in 50% Absence of anorexia 40% No rebound tenderness 52%

DON’T FORGET
Imitators of appendicitis Yersinia Mesenteric adenitis Sickle crisis
Caution in adolescent female!!! Other causes of abdominal pain:
Lower lobe pneumonia DKA

ABDOMINAL MASSES

ABDOMINAL MASSES
What is it? Age Location Characteristics
Firm Cystic Mobile Fixed
Initial diagnostic studies History usually no significance

ABDOMINAL MASSES
Location Most important
factor Characteristics
Cystic Usually benign
Solid Predominantly
malignant
Age Second most
important factor

ABDOMINAL MASSES
Work up Plain films
Displacement Obstruction Calcification
Ultrasound Initial diagnostic
tool of choice Solid vs cystic

ABDOMINAL MASSES
Work up CT
Study of choice Extent of local disease Sites of distant
metastases Character of the lesion Contrast
Careful analysis of abdominal and pelvic structures
MRI

QUESTION 6
On examination of a newborn female, you palpate an abdominal mass. Ultrasound reveals a 6cm ovarian cyst. What should you tell these anxious parents?
A. Most ovarian cysts resolve spontaneously and therefore no treatment is needed
B. Large cysts >5cm are at risk for torsion and should be aspiratedC. These are very rare and have a high risk for malignant transformationD. They are caused by hormones produced by the fetus in utero