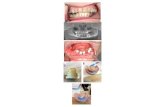
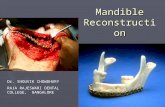
Mandible fractures
-
Upload
shivani-saluja -
Category
Education
-
view
3.717 -
download
4
Transcript of Mandible fractures
- 1.MANDIBULAR FRACTURE DR. SHIVANI SALUJA MDS ORALAND MAXILLOFACIAL SURGERY
2. SOME FACTS 2 Mandibular fracture > middle third fracture (anatomical factor) Minor mandibular fracture may be associated with head injury owing to the cranio-mandibular articulation Mandibular fracture may compromise the patency of the airway in particular with loss of consciousness----BILATERAL PARASYMPHYSIS FRACTURE Fracture of mandible occurred with frontal impact force as low as 425 lb (190 Kg) {Condylar fracture} 3. 3 Fracture of condyle regarded as a safety mechanism to the patient Frontal force of 800-900 lb (350-400 Kg) is required to cause symphysial fracture Mandible was more sensitive to lateral impact than frontal one---- ANGLE FRACTURE > CONDYLAR FRACTURE Long canine tooth and partially erupted wisdoms represent line of relatively weakness 4. Anatomical considerations 4 5. Anatomical considerations 5 Lateral pterygoid Medial pterygoid Genioglossus 6. 6 Blood supply Endosteal supply via the ID artery and vein Periosteal supply, important in aging due to diminishes and disappearance of alveolar artery (Supra Periosteal Fixation) Bradley 1972 Nerve Damage of inferior dental nerve Facial palsy by direct trauma to ramus Damage to mandibular division of facial nerve 7. Etiology of mandibular fractures 7 Vehicular accidents 43% Assaults,interpersonal violence,etc 34% Fall 7% Sports 4% Industries mishaps or work accidents 10% Pathological fractures or miscellaneous 2% 8. Classification of mandibular fractures 8 Simple or closed Compound or open Comminuted Greenstick Pathologic Multiple Impacted Atrophic Indirect Complicated or complex 9. SIMPLE FRACTURE Linear fracture which are not in communication with the exterior Rowe & Killeys Kruger is one in which the overlying integument is intact. 10. COMPOUND FRACTURE A fracture in which an external wound involving the skin, mucosa, or periodontal membrane communicates with the break in the bone. 11. COMMINUTED FRACTURE A fracture in which bone is splintered or crushed. 12. MULTIPLE FRACTURE A variety in which there are two or more lines of fracture on the same bone not communicating with each other. 13. GREENSTICK FRACTURE A fracture in which one cortex of the bone is broken, the other cortex been bent. SEEN IN CHILDREN 14. PATHOLOGICAL Fracture due to existing pathology 1. GENERALISED SKELETAL DEFORMITY 2. LOCALIED SKELETAL DEFORMITY 15. IMPACTED FRACTURE A fracture in which one segment is firmly driven into another. 16. ATROPHIC A spontaneous fracture resulting from atrophy of the bone, as in edentulous mandible 17. INDIRECT FRACTURE A fracture at a point distant from the site of injury COMPLICATED/COMPLEX A fracture in which there is considerable injury to the adjacent soft tissue or adjacent parts; may be simple or compound 18. Classification by anatomic region 18 Dingman and Natvig Condylar process Coronoid Ramus Angle Body Symphysis Parasymphysis Alveolar process 19. Body 30-40 % Angle 25-30 % Condyle 15-17 % Symphysis 7-15 % Ramus 3-9 % Alveolar 2-4 % Coronoid Process 1-2 % 20. HORIZONTALLY UNFAVOURABLE FRACTURES The masseter ,temporalis and medial pterygoid cause upward and medial pterygoid cause upward and medial displacement of the proximal segment VERTICALLY UNFAVOURABLE FRACTURES Medial and lateral pterygoids result in medial displacement of the proximal segment 20 21. HORIZONTALLY FAVOURABLE FRACTURE VERTCALLY FAVOURABLE FRACTURE 22. HORIZONTALLY UNFAVOURABLE FRACTURE VERTCALLY UNFAVOURABLE FRACTURE 23. Diagnosis of mandibular fractures 24 History Clinical examination Radiological examination 24. Clinical examination Mouth opening Occlusion Lacerations Colemans sign Step deformity (shoulder defect) Inspection Tenderness Crepitation Mobility of the teeth Foreign bodies Palpation 25. COLEMANS SIGN 26. SHOULDER DEFORMITY 27. Radiographic examination Plain radiograph OPG Lateral oblique PA mandible Lower occlusal CT scan 3-D CT MRI 28 28. Principles of mandibular fractures management 30 Reduction Fixation Immobilization 29. Reduction 31 Closed reduction Open reduction 30. Closed reduction 32 Indications a) Nondisplaced favorable fractures b) Grossly comminuted fractures c) Significant loss of overlying soft tissue d) Edentulous mandibular fractures e) Mandibular fractures in children f) Coronoid process fractures g) Condylar fractures 31. CLOSED REDUCTION Advantages Inexpensive Simple procedure Gives occlusion some leeway "to adjust itself No foreign body left in the body Disadvantages Cannot obtain absolute stability Long period of IMF PossibleTMJ sequelae Decrease range of motion of mandible Impaired pulmonary function 32. Open reduction 34 Displaced unfavourable fractures Multiple fractures of the facial bones Midface fractures and displaced bilateral condylar fracture Fractures of an edentulous mandible with severe displacement of fracture segment Edentulous maxilla opposing a mandibular fracture Delay of treatment and interposition of soft tissue between noncontacting displaced fractures fragments Malunion Conditions contraindicating Intermaxillary fixation 33. OPEN REDUCTION Advantages Early return to normal jaw function Avoidance of airway problems Absolute stability Bone fragments re- approximated exactly by visualization Low rate of malunion /nonunion Lower infection rate Avoids IMF Disadvantages Morbidity of surgical procedure Significant operating time Expensive hardware Secondary procedure for removal of hardware 34. Removal of a tooth from the fracture line ABSOLUTE INDICATION RELATIVE INDICATION Vertical fracture Dislocation or subluxation Periapical infection Infected fracture line Acute pericoronitis Functionless Advanced caries Advanced periodontal disease Doubtful teeth Teeth involved in untreated fractures presenting more than 3 days after injury 35. Methods of immobilization Osteosynthesis without Intermaxillary fixation Intermaxillary fixation Intermaxillary fixation with Osteosynthesis 36. Methods of immobilization 38 INTERMAXILLARY FIXATION Bonded brackets Dental wiring Direct Eyelet Arch bars Cap splints IMF screws 37. Various dental wiring techniques 39 Essigs wiring- (single double wiring) (Charles J. Essig ) Gilmers wiring Risdons wiring (Twisted labial wire) (E.Fulton Risdon) Ivy eyelet wiring (Robert H.Ivy ) Clovehitch wiring Col . Stouts multiloop wiring (R.A.Stout) Button wiring (Varaztad Hovhannes Kazanjian ) 38. Methods of immobilization 40 INTERMAXILLARY FIXATIONWITH OSTEOSYNTHESIS Transosseous wiring Circumferential wiring External pin fixation Bone clamps Transfixation with Kirschner wire 39. Period of immobilization 41 Young adult with Fracture of the angle receiving Early treatment in which Tooth removed from fracture line If a) Tooth retained in fracture line : add 1wk b) Fracture at the Symphysis: add 1 wk c) Age 40yrs and over : add 1or 2 wks d) Children and adolescents : subtract 1 wk 3 weeks 40. Methods of immobilization 42 OSTEOSYNTHESISWITHOUT INTERMAXILLARY FIXATION Compression plates Miniplates Lag screws 41. Rigid internal fixation 43 Dynamic compression plates Eccentric dynamic compression plates Locking plates---bicortical screws Lag screws 42. Indications of Rigid Osteosynthesis 44 Fractures in an edentulous part of the body of the mandible Concomitant fractures of the body and condyle Patients in whom IMF is contraindicated Fractures associated with closed head injury Continuity defects Fractures in which nonunion or malunion has occurred 43. Limitations and drawbacks Procedure is technically demanding, requires precise plate adaptation Danger of gap appearing in lingual border &alveolar region causing malocclusion All systems developed for this purpose require additional modification such as eccentric DCP or tension band in upper alveolus 44. .Load-Bearing versus Load-Sharing Fixation LOAD-BEARING FIXATION is a device that is of sufficient strength and rigidity that it can bear the entire load applied to the mandible during functional activities comminuted fractures of the mandible those fractures where there is very little bony interface because of atrophy, those injuries that have resulted in a loss of a portion of the mandible (defect fractures) 45. Load sharing devices Load-sharing fixation is any form of internal fixation that is of insufficient stability to bear all of the functional loads applied across the fracture by the masticatory system. requires solid bony fragments on each side of the fracture that can bear some of the functional load Fractures that can be stabilized adequately with load-sharing fixation devices are simple linear fractures,and constitute the majority of mandibular fractures Eg;-2.0 mm miniplating systems Lag screw techniques 46. Complications of rigid internal fixation 48 Infection Minor - not necessitating the plate removal Major - necessitating the plate removal Sensory Inferior alveolar nerve Mental nerve Motor Marginal mandibular nerve 47. Complications of rigid internal fixation 49 Malunion or nonunion malocclusion Restriction of craniofacial growth Hypertrophic scar formation Joint pain Injury to tooth roots Metal allergy 48. Champys Osteosynthesis lines 50 49. Fixation of miniplates for mandibular fractures 51 Angle fracture - superior aspect of the mandible extending on to the broad surface of the external oblique ridge Region between two mental foramina 2 plates are recommended 1. Subapical region of the Symphysis 2. Inferior border of the mandible Body of the mandible - one plate recommended just below the apices of the teeth but above the inferior alveolar nerve canal 50. Advantages of the Monocortical miniplate Osteosynthesis 56 Less soft tissue dissection. Less likely to palpable. No necessity for subsequent removal. Decrease the degree of stress shielding. Minimal risk of dental injury. Can also be performed under L.A . Decrease in surgical morbidity. 51. Limitations and potential complications 57 Not rigid Torsional movements resulting in infection or nonunion, or both Longer plates required to span communited fractures