InsomniaOSA Final MSmyth - Wild Apricot2 OBSTRUCTIVE SLEEP APNEA 5 Normal airway Abnormal airway...
Transcript of InsomniaOSA Final MSmyth - Wild Apricot2 OBSTRUCTIVE SLEEP APNEA 5 Normal airway Abnormal airway...

1
INSOMNIA VS. SLEEP APNEAMorganne Smyth, Pharm.D.
Pharmacy Practice Resident
St. Luke’s Medical Center, Boise, ID
ISHP 2013 Spring Meeting
LEARNINGOBJECTIVES
� List key differences between insomnia and obstructive sleep apnea
� Identify at least two appropriate pharmacologic
treatment options for insomnia
� Assess how current FDA warnings have affected
options for the treatment of insomnia
2
INTRODUCTION – OBSTRUCTIVE SLEEP APNEA
� Obstructive Sleep Apnea (OSA)
� Affects up to 4% of middle-aged adults
� Common complaints
� Loud snoring
� Disrupted sleep
� Daytime sleepiness
� Up to 80% of patients with OSA are undiagnosed
� 50% of patients who present with a stroke have sleep
apnea
� 35% of patients with high blood pressure have sleep
apnea 3
Victor LD, Am Fam Physician, 1999, Nov 15;60(8):2279-86.
National Stroke Foundation, 2005, www.stroke.org
SLEEP APNEA
� “Apnea” is Greek for “without breath”
� Breathing ‘pauses’ during sleep
� At least ten-second intervals of absence of breathing
� Multiple seconds to minutes (up to 30 times/hr)
� Snorting/choking/gasping sound may occur when
breathe again
� Usually not associated with breathing problems
during the day
� Difficult to diagnose
� Symptoms usually recognized by spouse (loud snoring)
� Polysomnogram (sleep study) for diagnosis4
U.S. Food and Drug Administration, Consumer Updates, 2013.

2
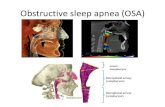
OBSTRUCTIVE SLEEP APNEA
5
Normal airway Abnormal airway
during sleep
Obstruction
Victor LD, Am Fam Physician, 1999, Nov 15;60(8):2279-86.
SLEEP APNEA QUESTIONNAIRE
6
Victor LD, Am Fam Physician, 1999, Nov 15;60(8):2279-86.
SLEEP APNEA RISK FACTORS
� Age � 40-60 years highest risk
� Ethnicity� African American, Pacific Islander, and Hispanic groups at higher risk
� Family history
� Obesity
� Physical characteristics� Large neck (>17” in men; >16” in women)
� Facial/Shull characteristics (narrow upper jaw, receding chin, overbite, large tongue, soft palate changes)
� Smoking and alcohol use
� Other medical conditions� Diabetes, GERD 7
Victor LD, Am Fam Physician, 1999, Nov 15;60(8):2279-86.
CONSEQUENCES OF SLEEP APNEA
� Increased risk of the following:
� Heart conditions
� Chest pain
� Cardiac arrhythmias (irregular heartbeat)
� Heart attack
� Stroke
� Motor vehicle accidents
� Work-related accidents
� Depression
8
U.S. Food and Drug Administration, Consumer Updates, 2013.

3
TREATING SLEEP APNEA
� First line � Behavioral measures
� Lose weight
� Decrease alcohol intake
� Decrease/stop taking medications that make you
drowsy
� Second line � CPAP
� CPAP (continuous positive airway pressure) machine
� Other options
� Dental appliances/devices
� Surgery
� There are currently NO medication therapies available to treat obstructive sleep apnea
9
U.S. Food and Drug Administration, Consumer Updates, 2013, www.fda.gov
CPAP THERAPY
� Mask over nose/mouth
� Connects to machine
kept at the bedside
� Mild air pressure used to keep airway open
� Decreases sleep disruptions from
decreased oxygen intake
� Decreases snoring
� Leads to decreased daytime sleepiness
10
National Heart, Lung, and Blood Institute [Internet], Department of Health and Human Services, 2012, www.nhlbi.nih.gov
DENTAL APPLIANCES/DEVICES
� Used for OSA in patients unable to tolerate or have not have improvement with CPAP therapy
� Mandibular advancement device (MAD)
� Most widely used
� Forces lower jaw forward and down
� Tongue retaining device (TRD)
� Splint that hold the tongue in place
� Disadvantages
� Not as effective as CPAP
� Pain, dry lips, tooth discomfort
� May cause long term changes in dental structure11
University of Maryland Medical Center, obstructive sleep apnea - dental devices, 2009, www.umn.edu
DENTAL APPLIANCES/DEVICES
12
Mandibular
advancement device
Tongue retaining
device

4
INTRODUCTION - INSOMNIA
� One of the most common medical complaints
� 35% of the population reports insomnia within the
last year
� Increasing prevalence with increasing age
� More common in:
� Females
� Unemployed
� Divorced, widowed, separated
� Lower socioeconomic status
� Only 30% of patients with insomnia report the problem to their physician
13
UpToDate, Overview of Insomnia, 2013, www.uptodate.com
CLASSIFICATION OF SLEEP DISORDERS
Primary Sleep Disorders
Dyssomnias – abnormality in amount, quality, or timing of sleep
Primary insomnia
Primary hypersomnia
Narcolepsy
Breathing-related sleep disorder
Circadian rhythm sleep disorder
Jet lag
Shift work
Parasomnias – abnormal behavioral or psychological events
associated with sleep
Nightmare/Sleep terror disorder
Sleepwalking
Sleep disorders related to another mental disorder14
Wells BG, Pharmacotherapy Handbook, 2009, pg. 814.
DURATION
� Transient (2-3 days) or short term (up to 3 weeks)
� Jet lag
� Shift work changes
� Acute illness
� Major life events
� Chronic insomnia (greater than 1 month)
� Medical disorder
� Psychiatric disorder
� Medication-related cause
15
Wells BG, Pharmacotherapy Handbook, 2009, pg. 814.
INSOMNIA DIAGNOSIS
� One or more of the following:
� Difficulty initiating sleep
� Difficulty maintaining sleep
� Waking up too early or nonrestorative/poor sleep
quality
� Problems with sleep despite adequate
opportunity for sleep
� Different from sleep deprivation
� Must also have daytime impairment from
sleep difficulty
16
Schutte-Rodin S, J Clin Sleep Med, 2008 Oct 15;4(5):487-504.

5
DAYTIME IMPAIRMENT
� One of the following to qualify for daytime impairment
� Fatigue or lethargy
� Problems with attention, concentration, or memory
� Poor school/work performance
� Irritability
� Low motivation or energy
� Increased errors/accidents at work or while driving
� Headaches
� GI symptoms
� Concerns or worries about sleep loss17
Schutte-Rodin S, J Clin Sleep Med, 2008 Oct 15;4(5):487-504.
HOW MUCH SLEEP IS ENOUGH?
024681012141618
Ho
ur
s o
f S
lee
p
Average Amount of Required Sleep
18
U.S. Food and Drug Administration, Consumer Updates, 2013, www.fda.gov
INSOMNIA OR NOT?
� Some people require only a few hours of sleep with no residual daytime sleepiness
� As people age, they require less sleep
� NOT considered insomnia due to absence of daytime
symptoms
� Does not appear to be associated with adverse health
outcomes
� Called “short sleep requirement” or “short sleepers”
� Spending less time sleeping due to busy lifestyle
� NOT considered insomnia if sleep comes easily when
given the opportunity
� Known as “sleep deprivation” 19
Schutte-Rodin S, J Clin Sleep Med, 2008 Oct 15;4(5):487-504.
HOW IS OSA DIFFERENT THAN INSOMNIA?
� Obstructive sleep apnea is caused by a physical obstruction of the airway
� Awakening due to decreased oxygen intake
� Given the opportunity to sleep (without the
obstruction), individuals are able to sleep
� Similar to “sleep deprivation” problem
� Would sleep if had adequate opportunity
� CANNOT be treated with medication
� Many medications used to treat insomnia need to be avoided
in patients with obstructive sleep apnea
� Avoid central nervous system depressants (i.e.
benzodiazepines)
20
UpToDate, Overview of Insomnia, 2013, www.uptodate.com

6
CONSEQUENCES OF INADEQUATE SLEEP
� Decreased quality of life
� Tired, sleepiness, confusion, anxiety, depression
� Less likely to receive job promotions, more sick time
� Comorbidities
� May have increased risk of high blood pressure, heart
attacks, and other heart conditions
� Strongly associated with development of psychiatric
disorders
� Depression, anxiety, drug abuse
21
UpToDate, Overview of Insomnia, 2013, www.uptodate.com
MEDICATION-RELATED CAUSES
� Beta blockers � Metoprolol
� Asthma medications � Albuterol, theophylline
� Antidepressants � Fluoxetine, nortriptyline
� Decongestants � Pseudoephedrine
� Stimulants � ADHD medications
� Steroids� Prednisone, methylprednisolone
*List not inclusive
of all medication-
related causes
22
Chawla J, Insomnia, 2013, emedicine.medscape.com
INSOMNIA AND OTHERMEDICAL CONDITIONS
01020304050607080
Prevalence of Chronic Insomnia in other
Medical Conditions
Insomnia
No Insomnia
Taylor DJ, Sleep, 2007 Feb;30(2):213-8.
23
MENOPAUSE AND INSOMNIA
� More sleep complaints during perimenopausalperiod
� Insomnia common complaint in women with early
menopause
� May be secondary to vasomotor symptoms (hot
flashes, night sweats) during menopause
� Sleep quality has shown to be better after
menopause
� More deep sleep and longer sleep times
� More self-reported dissatisfaction with sleep (even
though getting ‘better’ sleep)
Young T, Sleep, 2003, Sep;26(6):667-72.
24

7
MANAGEMENT
� Identifying cause of insomnia (if identifiable)
� Treat comorbid conditions
� Education
� Sleep hygiene
� Stress management
� Monitoring of mood symptoms
� Eliminating unnecessary pharmacotherapy
� Pharmacologic therapies
25
Schutte-Rodin S, J Clin Sleep Med, 2008 Oct 15;4(5):487-504.
BEHAVIORAL THERAPY
� Sleep hygiene
� Stimulus control
� Relaxation
� Sleep restriction
� Cognitive therapy
� Cognitive behavioral therapy
26
Schutte-Rodin S, J Clin Sleep Med, 2008 Oct 15;4(5):487-504.
UpToDate, Overview of Insomnia, 2013, www.uptodate.com
SLEEPHYGIENE
� Sleep only as long as you need to feel rested� Get out of bed
� Maintain a regular sleep schedule
� Do NOT force sleep
� Avoid caffeine after lunch
� Avoid alcohol near bedtime
� Avoid smoking/nicotine intake
� Decrease stimuli in bedroom
� Take care of worries before bed
� Exercise 20 mins. during the day � 4 – 5 hours prior to bedtime
� Avoid daytime naps 27
UpToDate, Overview of Insomnia, 2013, www.uptodate.com
STIMULUS CONTROL
� People who suffer from insomnia associated the bed/bedroom with fear of not sleeping
� Do not go to bed unless sleepy
� Only used the bed for sleep or sex
� Do not spend > 20 mins in bed without falling asleep
� Get up and do something relaxing
� Alarm set to wake a same time everyday
� No naps allowed
28
UpToDate, Overview of Insomnia, 2013, www.uptodate.com

8
RELAXATION THERAPY
� Used each evening prior to sleep
� Progressive muscle relaxation
� Head-to-toe progression of contraction followed by
relaxation
� Relaxation response
� Lie or sit comfortably
� Close eyes and focus on deep breathing
� Focus on one neutral image
� Peaceful word or place
29
UpToDate, Overview of Insomnia, 2013, www.uptodate.com
SLEEP RESTRICTION THERAPY
� Stay in bed longer to make up for lost sleep
� Shift in circadian rhythm
� Decrease time spent in bed to time actually sleeping (not < 5 hours)
� No naps during the day
� Sleep efficiency calculated
� Time sleeping/time in bed (%)
� ↑ time by 15-30 mins when > 85%
30
UpToDate, Overview of Insomnia, 2013, www.uptodate.com
COGNITIVE THERAPY
� Patients awake at night
� Concern of poor functioning next day
� Worry exacerbates difficulty sleeping
� Work with therapist
� Deal with anxiety
� Establish realistic expectations
31
UpToDate, Overview of Insomnia, 2013, www.uptodate.com
COGNITIVE BEHAVIORAL THERAPY
� Combines many strategies over several weeks
32
Stimulus Control
Sleep Restriction
Cognitive Therapy
Sleep Hygiene
Education
UpToDate, Overview of Insomnia, 2013, www.uptodate.com

9
PHARMACOLOGICAL THERAPY
� Benzodiazepines
� Non-benzodiazepine sedatives
� Melatonin agonist
� Antihistamines
33
UpToDate, Treatment of Insomnia, 2013, www.uptodate.com
PHARMACOLOGICAL TREATMENT
� Caution in the following patient groups
� Pregnancy
� Fetal malformations in first trimester
� Alcohol consumption
� Excessive sedation
� Renal/hepatic disease
� Accumulation of drug
� Pulmonary disease/Sleep apnea
� Worsen disease/hypoventilation
� Nighttime decision-makers
� On-call, taking care of children
� Older adults
� Increased risk of side effects34
UpToDate, Overview of Insomnia, 2013, www.uptodate.com
BENZODIAZEPINES
� Benzodiazepines have sedative, anxiolytic, muscle relaxant, and anticonvulsant properties� Reduce time to onset of sleep
� Increase total sleep time
� All schedule IV controlled substances
� Medications commonly used� Triazolam (Halcion®)
� Quick-acting, but also short-acting
� Lorazepam (Ativan®)
� Short-intermediate acting
� Estazolam (Prosom®) and temazepam (Restoril™)
� Intermediate-acting
� Flurazepam (Dalmane®) and quazepam (Doral®)
� Long-acting due to active metabolites 35
Wells BG, Pharmacotherapy Handbook, 2009, pg. 814.
BENZODIAZEPINES
� Adverse Effects� Drowsiness, incoordination, decreased concentration, and cognitive deficits
� Daytime tolerance to these effects may occur
� Anterograde amnesia
� Abuse risk
� Tolerance� May develop after 2 – 12 weeks of continuous use
� Rebound insomnia� Decrease risk by taking lowest dose and tapering medication
� Increased falls and hip fractures� Longer-acting flurazepam and quazepam increase falls/fractures especially in the elderly 36
Wells BG, Pharmacotherapy Handbook, 2009, pg. 814.

10
NON-BENZODIAZEPINES
� Zolpidem (Ambien™)
� Minimal anxiolytic activity
� No muscle relaxant properties
� Not an anticonvulsant
� Comparable efficacy to benzodiazepines
� Zaleplon (Sonata®)
� Rapid onset, half-life of 1 hour
� Does NOT reduce nighttime awakenings or help
increase total sleep time
� Eszopiclone (Lunesta™)
� Rapid onset
� Approved to help with sleep onset and maintenance 37
Wells BG, Pharmacotherapy Handbook, 2009, pg. 814.
NON-BENZODIAZEPINES
Drug Indication Half-life Notes
Zolpidem
(Ambien)
Sleep onset
insomnia
~2.5 hrs New warnings released in
January 2013
Zolpidem CR
(Ambien CR)
Sleep onset or
maintenance
insomnia
1.4 – 4.5
hrs
Controlled-release formula
Zolpidem
sublingual
(Intermezzo)
Sleep
maintenance
insomnia
1.4 – 6.7
hrs
To be given in the middle of
the night
Zaleplon
(Sonata)
Sleep onset
insomnia
1 hour Not indicated for long-term
use
Eszopiclone
(Lunesta)
Sleep onset or
maintenance
insomnia
6 – 9 hrs For sleep onset and
maintenance
38
UpToDate, Treatment of Insomnia, 2013, www.uptodate.com
NON-BENZODIAZEPINES
� Adverse effects
� Similar to benzodiazepines
� Less severe
� Dizziness
� Headache
� Somnolence
� Daytime sedation
� Complex-sleep related behaviors
� Unpleasant taste (Eszopiclone)
� Hallucinations (Zolpidem)
� Less risk of abuse versus benzodiazepines
39
Wells BG, Pharmacotherapy Handbook, 2009, pg. 814
UpToDate, Treatment of Insomnia, 2013, www.uptodate.com
COMPLEX SLEEP-RELATED BEHAVIORS
� Non-benzodiazepines
� Sleep eating
� Sleep driving
� Phone calls while sleeping
� Engaging in sexual behaviors
while not fully awake
� Higher doses of medications
have been attributed to these
complex sleep behaviors
40
U.S. Food and Drug Administration, Consumer Updates, 2013.
Hwang TJ, J Clin Psychiatry, 2010 Oct;71(10):1331-5

11
MELATONIN AGONIST
� Ramelteon (Rozerem™)� Involved with circadian rhythm
� Fewer and less severe side effects than benzodiazepines and non-benzodiazepines� Less daytime residual effects
� No withdrawal or rebound insomnia
� Not known to be habit-forming
� Only sedative-hypnotic that is not a controlled substance
� Common side effects� Somnolence
� Nausea
� Fatigue
� Headache 41
UpToDate, Treatment of Insomnia, 2013, www.uptodate.com
ANTIHISTAMINES
� First-generation (sedating) antihistamines
� Most common
� Diphenhydramine (Benadryl®)
� Doxylamine (Unisom®)
� Less effective than other options
� Anticholinergic side effects
� Dry mouth
� Blurred vision
� Urinary retention
� Constipation
� Side effects usually more severe in elderly patients 42
UpToDate, Treatment of Insomnia, 2013, www.uptodate.com
Wells BG, Pharmacotherapy Handbook, 2009, pg. 814
INSOMNIA TREATMENT
� General recommendations
� Do not take medications for insomnia unless you
have a full 7-8 hours to dedicate to sleep
� Lowest doses needed
� Decrease daytime sleepiness/side effects
� Easier to taper off medication
� Use for the shortest time necessary
� Decrease risk of tolerance
� Try other non-medication therapies
� Caution during next day when starting new
insomnia medications
� Recognize how the medication will affect you43
UpToDate, Treatment of Insomnia, 2013, www.uptodate.com
ZOLPIDEMWARNING
� January 2013 FDA Safety Communication
� Blood levels of zolpidem in certain patients may be high
enough in the morning to impair activities requiring
alertness (i.e. driving)
� Highest risk in extended-release product (Ambien CR®)
� New recommendations to consider lower doses in all
patients
� Decrease dose especially in women due to slower
elimination of the drug from the body
� Slower elimination has not been demonstrated in men,
but lower doses should be recommended in general
44
U.S. Food and Drug Administration [Internet], Zolpidem Containing Products: Drug Safety Communication - FDA Requires
Lower Recommended Doses, 2013, www.fda.gov

12
INSOMNIA IN THE ELDERLY
� Up to 60% of adults > 65 years of age suffer from insomnia
� Age-related changes in sleep patterns
� Underlying illness
� Medication side effects
� Less sleep necessary
� Risk of using traditional sleep aids is higher in
elderly patients
� 5 - 33% of elderly patients receive a benzodiazepine
or other non-benzodiazepine sleep aids45
Insomnia in the elderly. Pharmacist's Letter/Prescriber's Letter 2009;25(9):250919.
NON-PHARMACOLOGICOPTIONS IN THE
ELDERLY
� Identify and manage exacerbating factors
� Pain
� Shortness of breath (heart failure)
� Chest pain
� COPD
� GI disease (acid reflux, ulcer)
� Neurologic or mood disorders
� Parkinson’s, dementia, anxiety, depression
46
Insomnia in the elderly. Pharmacist's Letter/Prescriber's Letter 2009;25(9):250919.
NON-PHARMACOLOGICOPTIONS IN THE
ELDERLY
� Target sleep hygiene
� Avoid nicotine, alcohol, and caffeine
� Increase exercise and light exposure in the day
� Limit napping
� Reduce light and noise in the sleep environment
� Keep temperature comfortable
� Avoid meals and liquids close to bedtime
47
Insomnia in the elderly. Pharmacist's Letter/Prescriber's Letter 2009;25(9):250919.
PHARMACOLOGICOPTIONS
� Some evidence that newer non-benzodiazepine hypnotics are safer for the elderly
� ↓ sleep cycle changes, rebound insomnia, tolerance,
and hangover
� Start with lower doses in older patients
� May try ramelteon (Rozerem)
� No dependence/abuse risk
� Helps in sleep initiation, but not maintenance
48
Insomnia in the elderly. Pharmacist's Letter/Prescriber's Letter 2009;25(9):250919.

13
PHARMACOLOGICOPTIONS
� Other options
� Trazodone, an antidepressant, may increase deep
sleep
� Not well studied, early on appears to be beneficial
� Non-habit forming
� AE: Dry mouth, nausea, arrhythmias, orthostatic
hypotension
49
Insomnia in the elderly. Pharmacist's Letter/Prescriber's Letter 2009;25(9):250919.
SELF-TREATMENT IN THE ELDERLY
� Alcohol
� Causes early awakening
� Antihistamines (i.e. diphenhydramine)
� Anticholinergic effects, cognitive impairment, urinary
retention
� Residual daytime sleepiness
� Melatonin
� Helps with difficulty falling asleep
� Valerian
� May takes several night/weeks to see benefit
� Kava
� AVOID, may cause hepatotoxicity50
Insomnia in the elderly. Pharmacist's Letter/Prescriber's Letter 2009;25(9):250919.
META-ANALYSIS - ELDERLY INSOMNIA
� 24 Randomized Controlled Trials� 2417 subjects with insomnia > 60 years of age
� No other psychiatric/psychological disorders
� Treated with benzodiazepines, zopiclone, zolpidem, zapelon, diphenhydramine, and placebo
� Results� Sleep time increased by ~25 min/night
� Benzodiazepines increased sleep by ~34 min/night
� Adverse effects� Cognitive events ~5 times as common
� Daytime fatigue ~4 times more common
� Adverse events similar between benzodiazepine and non-benzodiazepines
51
Glass J, BMJ, 2005 Nov 19;331(7526):1169.
META-ANALYSIS – TREATMENT BENEFIT
52
Glass J, BMJ, 2005 Nov 19;331(7526):1169.

14
META-ANALYSIS – ADVERSE EFFECTS
53
Glass J, BMJ, 2005 Nov 19;331(7526):1169.
META-ANALYSIS
� Limitations
� Medications grouped together
� Subjective measures
� Excluded patients with other
psychiatric/psychological disorders
� Did not assess dependence risk
� Conclusions
� Clinical benefits of sleep aids in the elderly may be
modest
� Greater risk of adverse events occurring in the older
population
54
Glass J, BMJ, 2005 Nov 19;331(7526):1169.
SUMMARY
� Insomnia diagnosis� Difficultly initiating, maintaining, or poor quality/nonrestorative sleep
� Daytime impairment
� Difficulty despite adequate time for sleep
� Obstructive sleep apnea treatments� Lifestyle changes
� CPAP therapy
� No medication therapies available
� Insomnia treatments� Behavioral therapies are first line
� New zolpidem recommendations� Lower doses in women due to slower elimination
� Risks of pharmacologic treatment in the elderly may outweigh the benefit
55
REFERENCES
� Chawla J, Park Y, Passaro EA. Insomnia. Medscape Reference. c2013 WebMD LLC [updated 18 Jan 2013, cited 15 Mar 2013]. Available from: http://emedicine.medscape.com/article/1187829-overview
� Glass J, Lanctôt KL, Herrmann N, Sproule BA, Busto UE. Sedative hypnotics in older people with insomnia: metaanalysis of risks and benefits. BMJ. 2005 Nov 19;331(7526):1169.
� Hwang TJ, Ni HC, Chen HC, Lin YT, Liao SC. Risk predictors for hypnosedative-related complex sleep behaviors: a retrospective, cross-sectional pilot study. J ClinPsychiatry. 2010 Oct;71(10):1331-5
� Insomnia in the elderly. Pharmacist's Letter/Prescriber's Letter 2009;25(9):250919.
� National Heart, Lung, and Blood Institute [Internet]. What is CPAP? Department of Health and Human Services [updated 13 Dec 2011, cited 15 Mar 2013]. Available from: http://www.nhlbi.nih.gov/health/health-topics/topics/cpap/
� National Stroke Foundation [Internet]. Stroke Related Sleep Disorders. National Stroke Foundation c2005 [cited 13 Mar 2013]. Available from: http://www.stroke.org/site/DocServer/SLEEPQ.pdf?docID=862
� Schutte-Rodin S, Broch L, Buysse D, Dorsey C, Sateia M. Clinical guideline for the evaluation and management of chronic insomnia in adults. J Clin Sleep Med. 2008 Oct 15;4(5):487-504.
� Taylor DJ, Mallory LJ, Lichstein KL, Durrence HH, Riedel BW, Bush AJ. Comorbidityof chronic insomnia with medical problems. Sleep. 2007 Feb;30(2):213-8.
56

15
REFERENCES (CONT.)
� U.S. Food and Drug Administration [Internet]. Consumer Updates. U.S. Department of Health and Human Services Available from: www.fda.gov/consumer/features/sleepdrugs073107.html
� U.S. Food and Drug Administration [Internet]. Zolpidem Containing Products: Drug Safety Communication - FDA Requires Lower Recommended Doses. U.S. Department of Health and Human Services [updated 1 Jan 2013, cited 14 Mar 2013]. Available from: http://www.fda.gov/Safety/MedWatch/SafetyInformation/SafetyAlertsforHumanMedicalProducts/ucm334738.htm
� University of Maryland Medical Center [Internet]. Obstructive sleep apnea - Dental Devices. c2011 University of Maryland Medical Center [updated 23 Jun 2009, cited 15 Mar 2013]. Available from: http://www.umm.edu/patiented/articles/what_dental_devices_used_treat_sleep_apnea_000065_9.htm
� UpToDate [database on the Internet]. Overview of insomnia. Waltham, MA: UpToDate, Inc.; c2013. Available from: www.uptodate.com
� Victor LD. Obstructive sleep apnea. Am Fam Physician. 1999 Nov 15;60(8):2279-86.
� Wells BG, DiPiro JT, Schwinghammer TL, DiPiro CV. Sleep Disorders. In: Pharmacotherapy Handbook. 7th ed. New York, NY: McGraw-Hill;2009:814.
� Young T, Rabago D, Zgierska A, Austin D, Laurel F. Objective and subjective sleep quality in premenopausal, perimenopausal, and postmenopausal women in the Wisconsin Sleep Cohort Study. Sleep. 2003 Sep;26(6):667-72.
57
QUESTIONS?
58



![Obstructive Sleep Apnea and Diabetes - SM Journals · 2016-12-14 · sleep apnea, and 30 events/hour or more is considered severe sleep apnea [7]. Due to increased airway resistance](https://static.fdocuments.us/doc/165x107/5f8e2bfb7b2ea557be0e5510/obstructive-sleep-apnea-and-diabetes-sm-journals-2016-12-14-sleep-apnea-and.jpg)