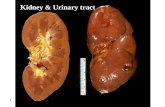
General diagnostics of the urinary tract
Transcript of General diagnostics of the urinary tract

General diagnostics of the kidneys and the urinary tract
Dr. Katalin Keltai3rd Department of Internal Medicine
Semmelweis University
3rd Year, Faculty of MedicineAcademic Year 2018/2019
1st Semester

Checking of a patient with kidney disease
�Aim is to detect specific signs and symptoms of kidney problems:�General physical examination �Checking of the urine*�Checking of blood pressure*�+abdominal US(?)*majority of patients with kidney disease have no complaints or
signs and only abnormalities of the urine examination or elevated blood pressure can suggest the underlying process

History� Family history
• Nephrolithiasis• Hypertension• Polycystic kidney• Tubular transport disaeses (Fanconi sy., etc.)
� Individual history� Previous infections(Streptococcus, recurrent cystitis, tbc)� Part of systemic diseases
� Diabetes � Hyperuricemy, uric acid nephritis, nephrolithiasis� Paraproteinemia� Autoimmun diseases (SLE)
� Drugs� NSAID, antibiotics (gentamycin, amfotericin), contrast
media� Allergic reaction
� medication (penicillin), transfusion� Hemolysis� Poisoning (heavy metal, organic dissolvents, ethylen-glycol)

Complaints� General complaints
� Tiredness, weakness, loss of appetite – not specific
� Headache� Dull, diffuse, constant – generally indicates hypertension or uremy
� Bladder pain– suprapubic dyscomfort = acute urinary retention, radiating to the urethra during urination = cystitis
� Prostate pain – pubic area, irritative urinary complaint
� Back pain (costovertebral)� Both sides, softens by laying down – acute glomerulonephritis� Unilateral, strong, crampy, from back radiates anteriorly and
downwards to the inner tight and to the grand labia/testis –nephrolithic colic attack
� Pulsatile kidney area pain uni/bilateral – acute pyelonephritis
� Nausea, vomiting� Nephrolithic colic attack� Gradually developing, ongoing for long time – chronic kidney failure
� Complaints on urination

Complaints on urination� Irritative
� Urgency = urgent urinary urge → cystitis, neurogen bladder� Dysuria = painful urination→ cystitis� Pollakisuria = frequent urination (obsessive, frequent urinary stimulus
and frequent low amount urination – cystitis)� Nocturia/nycturia = night urination
� Increased urine production (DM, diab insipidus, big fluid intake, diuretics (alcohol and coffein, too!))
� Decreased functional capacity of the bladder (neurogen, other compression, psychyc)
� Obstructive� Hesitation prostate hypertrophy� Sluggish urine jet urethral stricture� obstruction neurogen bladder� Dripping after urination foreign body
� Incontinence� Total� Stress (intraabdominal pressure increase)� urging� Ischuria paradoxa – Frequent, small urine amount, starts hard,
bladder is full – prostate hypertrophy

Complaints on urination� Change in quantity (fluid intake!)
� Anuria – < 400 ml/day� Oliguria – 400-800 ml/day� Polyuria - > 2000 ml/day
� Change in colour� concentration� Alkalic urine after a while brick-red precipitation –
phosphates� Brown ale, yellow foam – icterus, bilirubin� red – hemoglobin, blood (hematuria)� Reddish brown – porfirinuria� Brownish black - alcaptonuria
� Change in transparency� Pus – pyuria� Bacteria – bakteriuria� Protein - proteinuria


Physical examination� Inspection
� Skin• pale + edema = acut diffuse glomerulonephritis, nephrosis sy• Yellowish pale, grayish = uremia (anemia + urocrom precipitation)
� Edema (transsudate)� Whole body, subcutan, pronounced where subcutan tissues are
loose: face, around eyes, hands, feet-legs, scrotum.� Doesn’t or hardly keeps fingerprint, distribution doesn’t respect
gravitation� Ascites, pleural and pericardial fluid can be present
� Palpation� Lying on the back; normally not palpable (skinny!)� Trying to lift causes pain – nephritis, pyelonephritis� More information from abdominal US
� Auscultation� Epigastric bruit, both systolic and diastolic suggests renal artery
stenosis, but also can be caused by calcified aorta or hypertension.� Blood pressure measurement� Fundus examination

Urine examination„Kidney biopsy of the poor”
Obligatory for every patient as screening (even in complaintless patients)
� pH (5, vegetarian 7), acidic urine precipitates urate, alkalic precipitates phosphate
� Specific gravity (1001-1030)� Glomerular filtrate: 1010, if urine is the same - isosthenuria � Inability to concentrate: asthenuria + compensatory polyuria (3-4 l/day)
� Protein� Normally below 100 mg/24 h � In healthy individuals the glomerular capillary wall is permeable for molecules � less than 20 kD. The filtered low molecularweight proteins are reabsorbed
� in the proximal tubules.� 100-300 mg/24 h – microalbuminuria� 300 mg – 1 g – proteinuria� Over 3 g - nephrosis
� Sugar (normally not)� Bilirubin (normally not)� Urobilinogen � Nitrit (bacteria convert it from nitrate)� Sediment

Urine sediment
�Red blood cells�White blood cells�Microorganisms
�Bacteriuria
�Casts�Crystals, amorph particules

Urine sediment- Haematuria � Microscopic, macroscopic, diff. Hburia!, normally 1-1 RBC occurs
Dipstick can positive: Vitamin C, carrot, rebarb, myoglobin
� Renal origin only 10%� Glomerular
� IgA nephropathy� Thin GBM disease� Postinfectious glomerulonephritis� Membranoproliferativ GN� Systemic nephritises
� Extraglomerular� Polycystic kidney� Ureter stone� Kidney necrosis (poisoning)� Anticoagulant overdose� Trauma� Kidney tumor� Ureter catheter

Extrarenal (90%)� Bladder
� Tumor� Haemorrhagic cystitis� Prostate hypertrophy� Bilharziasis (Nile-delta)
� Urethra� infection, fresh red blood drop
Urine sediment- Haematuria

Haematuria evaluation
� History�At start / all the time / at the end of urination�Accompanied by pain, dysuric complaints�Medications, concommitant diseases
� Physical examination�Symptoms of systemic diseases (fever, lymph
nodes, abdominal mass, hypertension edema)
� Laboratory�Urine examination, culture, blood count, cytology
� Imaging�Abdominal-pelvic US, CT�Cystoscopy

Urine sediment– Pyuria = WBC!
�Most common infection�Acute infection 1 microbe�Chronic 2 or more microbes�Nosocomial – resistent strains
�Microbes – E. coli, Proteus, Klebsiella
�Classification�Urethritis, cystitis, pyelonephritis (ascending)�First, persistent, reinfection

Urine sediment- CastsOriginates from the tubules, has the shape of it
� Hyalin� Can be present normally in concentrated urine – mucoid precipitate� Fever, physical stress, diuretic th� Does NOT mean renal disease
� RBC� glomerulonephritis
� WBC� Pyelonephritis, interstitial nephritis
� Renal tubular cell� Acute tubular necrosis, interstitial nephritis
� Granular� Mostly macroglobulins (IgM)� Not specific, can be present in acute tubular
necrosis, nephritis� Big, waxy
� Chr. Kidney failure� Represents stasis in the collecting ducts
Hyalin
RBC
WBC
Granular

Urine sediment- Crystals
�Role in stone formation�Ca�Oxalate�Phosphates�Urate �Cystin

Persistent proteinuria� Primary glomerular causes
� Focal segmental glomerulonephritis� IgA nephropathy (i.e., Berger’s disease)� IgM nephropathy� Membranoproliferative glomerulonephritis� Membranous nephropathy� Minimal change disease
� Secondary glomerular causes� Alport’s syndrome� Amyloidosis� Collagen vascular diseases (e.g., systemic lupus er ythematosus)� Diabetes mellitus� Drugs (e.g., NSAIDs, penicillamine [Cuprimine], gol d, ACE inhibitors)� Fabry’s disease� Infections (e.g., HIV, syphilis, hepatitis, post-st reptococcal infection)� Malignancies (e.g., lymphoma, solid tumors)� Sarcoidosis� Sickle cell disease
� Tubular causes � Aminoaciduria� Drugs (e.g., NSAIDs, antibiotics)� Fanconi syndrome� Heavy metal ingestion� Hypertensive nephrosclerosis� Interstitial nephritis
� Overflow causes� Hemoglobinuria� Multiple myeloma� Myoglobinuria
Transient proteinuriaCongestive heart failureDehydrationEmotional stressExerciseFeverOrthostatic (postural) proteinuriaSeizures
PROTEINURIA

Functional examination of the kidney� A healthy person produces 120-150 ml/min (170-220 l/day)
glomerular filtrate (GF), most of it is reabsorbed� The amount of GF depends on the anatomical and functional status
of the glomeruli. If the renal blood supply is normal changes in the GF represent the disease of the glomerular mass
� The GF rate (GFR) can be measured indirectly with the assesment of the renal excretion of substances which 1. doesn’t bind to plasma proteins, 2. filtrates freely in the glomeruli, 3. doesn’t secrete and 4. doesn’t reabsorb in the tubules.
� Inulin → ideal, but the measurement is complicated and expensive
� creatinine → metabolite from the muscle, mostly fulfills the above criteria

Creatininenormal range: 50-100 µmol/l or 0.6-12 mg/dl
� Produced during the muscle metabolism� A small amount secretes in the tubules and this
amount increases as the GFR decreases –overestimates GFR
� In severe renal impairment, gut bacteria tear it down
� Dependent on the person’s meat intake and muscle mass (old age, cachexia ↓)
� Some medication (eg. Cimetidin, trimetoprim) decreases the tubular secretion of creatinine and could incorrectly suggest impaired renal function
� For accurate measurement stable plasma concentration is needed (for 24 hours), therefore it is not informative in the initial phase and the resolving of acute renal failure

Creatinine clearence(Cockroft-Gault formula)
normal value: 90-140 ml/min/1,73 m2
(140 – age) X body weight (kg)
GFR = __________________________
72 X Plasma creatinine (mg/dL)
Female individuals x 0,85 for the lesser muscle mass
Obes or edematous patients will have higher than real values

Urea – carbamide (BloodUreaNitrogen)(normal value: 2.9-7.1 mmol/l)
� Mainly produced by the liver, end product of protein demolition
� Glomeruli filtrate it and 30-70% is reabsorbed from the tubules
� Under-evaluates GFR� Hydration decreases, dehydration increases the reabsorbtion
and the BUN� Normally BUN: creatinine ratio is 1:10� Can be decreased
� Liver diseases� SIADH (syndrome of inappropriate antidiuretic hormon)
� Can be increased� Increased catabolism
• Gastointestinal bleeding• Cellular lysis• Steroid treatment
� High protein intake� Decreased renal perfusion
• Congestive heart failure• Renal artery stenosis

Imaging (past?)� X-ray � Iv. pyelography
�Assessment of renal excretion, functional, comarable, stone, obstruction
�Contrast media!�Nowadays CT supersedes it (contrast too, but
less radiation, better resolution)� Radioactive isotope techniques
�Indicates functional renal tissue inside a mass�Renal function (GFR) assessment�Renal blood flow assessment
�Low blood flow + decreased function = acute tubular necrosis
�Unilateral decrease in flow → renal artery occlusion

Imaging (present)� Ultrasound
�Cortical, medullar area, pyelon thickness, echogeniticity
�Kidney size�Cysts, stones, masses, urinary retention
� CT� MRI
�Can distinguish between the cortical and medullar area, diagnostic in glomerulonephritis, hydronephrosis, renal vascular lesions
�Suitable for staging of clear cell carcinoma (hypernephroma)
�Best visualisation of adrenal glands� Arteriography (therapeutic too)� Kidney biopsy

Indications for kidney biopsy
� Acute renal failure or chronic renal impairment of unknown origin
� Acute nephritis syndromes� Proteinuria and haematuria of unknown etiology� Staging for a previously diagnosed disease� Systemic disease with renal impairment (Wegener
granulomatosis, SLE, Goodpasture sy.)� BUT!
� <1%-ban bleeding, 0.1% transfusion�Nephrectomy/mortality ~ 0.01%

NORMAL PYELOGRAPHY

HYDRONEPHROSIS - PYELO

HYDRONEPHROSIS - CT

BENIGN PROSTATE HYPERTROPHY - CT

BLADDER STONE –PLAIN ABD X-RAY

BLADDER STONE - PYELO

MULTILAYER STONE AT THE BLADDER BASE-CT

CALYX STONE - PYELO

NEPHROLITH - CT

NEPHROLITHS
cystin CaHPO3
Ca oxalate
Coral stone

POLYCYSTIC KIDNEY - US

POLYCYSTIC KIDNEY, MULTIPLE CYSTS IN THE LIVER AND THE PANCREAS - CT

HORSESHOE KIDNEY – PYELO AND CT

RIGHT KIDNEY AND SEMINAL VESICLE AGENESIA -CT

KIDNEY TUMOR - PYELO

TRANSPLANTED KIDNEY - CT

BILATERAL RENAL ARTERY STENOSIS
BEFORE CATHETER DILATATION AND STENT IMPLANTATION ELŐTT…
AND AFTER




![7 Catheter-associated Urinary Tract Infection (CAUTI) · UTI Urinary Tract Infection (Catheter-Associated Urinary Tract Infection [CAUTI] and Non-Catheter-Associated Urinary Tract](https://static.fdocuments.us/doc/165x107/5c40b88393f3c338af353b7f/7-catheter-associated-urinary-tract-infection-cauti-uti-urinary-tract-infection.jpg)