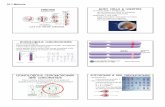
Functions of the Circulatory System Transport oxygen to cells Transport nutrients from the digestive...
-
date post
19-Dec-2015 -
Category
Documents
-
view
223 -
download
2
Transcript of Functions of the Circulatory System Transport oxygen to cells Transport nutrients from the digestive...


Functions of the Circulatory System
• Transport oxygen to cells• Transport nutrients from the
digestive system to body cells• Transport hormones to body cells• Transport waste from body cells to
excretory organs• Distribute body heat

Energy Requirements:• lots of mitochondria • aerobic respiration
Mechanisms and events of contractions:
1. All or none law- at organ level, not cellular level
2. Means of stimulation- autorhythmicy
3. Length of refractory period- cardiac (250ms), skeletal (1-2ms)

Location of Heart

Visceral pericardium • Outer protective layer composed of a serous
membrane • Includes blood capillaries, lymph capillaries, and
nerve fibers.
Layers of Cardiac Tissue

Myocardium • Relatively thick. • Consists largely of cardiac muscle tissue
responsible for forcing blood out of the heart chambers.
• Muscle fibers are arranged in planes, separated by connective tissues that are richly supplied with blood capillaries, and nerve fibers.
Layers of Cardiac Tissue

Endocardium • Consists of epithelial and connective tissue that
contains many elastic and collagenous fibers. • Connective tissue also contains blood vessels
and some specialized cardiac muscle fibers called Purkinje fibers.
• Lines all of the heart chambers and covers heart valves.
Layers of Cardiac Tissue

Pericardial Cavity

Layers of Cardiac Tissue

Heart Anatomy

Heart Anatomy

Heart Anatomy

Rightventricle
Leftventricle
Interventricularseptum
Heart Anatomy

CirculationCirculation

Components of the Human Components of the Human Circulatory SystemCirculatory System
The HeartBlood Vessels
BloodLymphatic Vessels
Lymph

Mechanisms & Events of Contraction
1. Means of stimulation2. Organ vs motor unit
contraction3. Length of absolute
refractory period

Microscopic Anatomy of Cardiac Muscle
Cardiac muscle cells are striated, short, fat, branched, and interconnected
Connective tissue matrix (endomysium) connects to the fibrous skeleton
T tubules are wide but less numerous; SR is simpler than in skeletal muscle
Numerous large mitochondria (25–35% of cell volume)

Figure 18.11a
Nucleus
DesmosomesGap junctions
Intercalated discs Cardiac muscle cell
(a)

Microscopic Anatomy of Cardiac Muscle
Intercalated discs: junctions between cells anchor cardiac cells • Desmosomes prevent cells from separating
during contraction• Gap junctions allow ions to pass;
electrically couple adjacent cells Heart muscle behaves as a functional
syncytium

Microscopic Anatomy of Cardiac Microscopic Anatomy of Cardiac MuscleMuscle

Microscopic Anatomy of Cardiac Microscopic Anatomy of Cardiac MuscleMuscle

Figure 18.8a
Pulmonary valveAortic valveArea of cutaway
Mitral valveTricuspid valve
Myocardium
Tricuspid(right atrioventricular)valveMitral(left atrioventricular)valveAorticvalve
Pulmonaryvalve
(b)
Pulmonary valveAortic valveArea of cutaway
Mitral valveTricuspid valve
Myocardium
Tricuspid(right atrioventricular)valve
(a)
Mitral(left atrioventricular)valveAortic valve
Pulmonaryvalve
Fibrousskeleton
Anterior
VALVES

Figure 18.8c
Pulmonaryvalve
AorticvalveArea ofcutawayMitralvalve
Tricuspidvalve
Chordae tendineaeattached to tricuspid valve flap
Papillarymuscle
(c)
VALVES



left ventricle
left atrium
pulmonary arteries
aorta
superior vena cava
inferior vena cava
right atrium
right ventricle
pulmonary vein
pulmonary arteries

bicuspid valve
aortic semilunar valve
tricuspid valve
pulmonary semilunar
valve
Heart ValvesHeart Valves


ContractioContraction Cycle of n Cycle of the Heartthe Heart

ContractiContraction Cycle on Cycle
of the of the HeartHeart

Contraction Contraction Cycle of the Cycle of the
HeartHeart

Cardiac OutputCO = the vol. of blood ejected from the l. or r. ventricle into the aorta or pulmonary trunk each min.
CO= SV x HR
SV= stroke vol.; the vol of blood ejected from the ventricle during each contraction (ml/beat)HR= heart rate; # beats/min, at rest ~60, exercise ~100

Cardiac Output (at rest)
SV = 75 ml/beat
HR = 75 beats/min
CO = 75 ml/b x 75 b/min
CO = 5250 ml/min = 5.25 L/min

Cardiac Output (exercise)
SV = 100 ml/beat
HR = 100 beats/min
CO = 100 ml/b x 100 b/min
CO = 10 L/min

Electrical Conductivity of the Heart

medulla
oblongata
pons
vagus
Nerve Nerve Innervation:Innervation:
Vagus nerve from medulla (parasympathetic division)
acetylcholine (slows heart)
Cardioacceleratory center in medulla (sympathetic) adrenaline from adrenal glands (speeds up heart)

• P = atrial depolarization ~ 0.1 sec atria contracts• QRS = ventricular depolarization ventricles contract
(lub), contraction stimulated by Ca++ uptake• T = ventricular repolarization ventricles relax (dub)
Electrocardiogram (ECG)
0.1 sec 0.3 sec 0.4 sec

Figure 18.17, step 1
Atrial depolarization, initiated bythe SA node, causes the P wave.
P
R
T
QS
SA node Depolarization
Repolarization
1
Excitation of the Excitation of the HeartHeart

Figure 18.17, step 2
Atrial depolarization, initiated bythe SA node, causes the P wave.
P
R
T
QS
SA node
AV node
With atrial depolarization complete,the impulse is delayed at the AV node.
P
R
T
QS
Depolarization
Repolarization
1
2

Figure 18.17, step 3
Atrial depolarization, initiated bythe SA node, causes the P wave.
P
R
T
QS
SA node
AV node
With atrial depolarization complete,the impulse is delayed at the AV node.
Ventricular depolarization beginsat apex, causing the QRS complex.Atrial repolarization occurs.
P
R
T
QS
P
R
T
QS
Depolarization
Repolarization
1
2
3

Figure 18.17, step 4
Ventricular depolarization iscomplete.
P
R
T
QS
Depolarization
Repolarization
4

Figure 18.17, step 5
Ventricular depolarization iscomplete.
Ventricular repolarization beginsat apex, causing the T wave.
P
R
T
QS
P
R
T
QS
Depolarization
Repolarization
4
5

Figure 18.17, step 6
Ventricular depolarization iscomplete.
Ventricular repolarization beginsat apex, causing the T wave.
Ventricular repolarization iscomplete.
P
R
T
QS
P
R
T
QS
P
R
T
QS
Depolarization
Repolarization
4
5
6

Figure 18.18
(a) Normal sinus rhythm.
(c) Second-degree heart block. Some P waves are not conducted through the AV node; hence more P than QRS waves are seen. In this tracing, the ratio of P waves to QRS waves is mostly 2:1.
(d) Ventricular fibrillation. These chaotic, grossly irregular ECG deflections are seen in acute heart attack and electrical shock.
(b) Junctional rhythm. The SA node is nonfunctional, P waves are absent, and heart is paced by the AV node at 40 - 60 beats/min.

Heart Sounds
Two sounds (lub-dup) associated with closing of heart valves• First sound occurs as AV valves close and
signifies beginning of systole• Second sound occurs when SL valves
close at the beginning of ventricular diastole
Heart murmurs: abnormal heart sounds most often indicative of valve problems

Coronary Artery Disease(CAD)
• Arteriosclerosis• HDL vs LDL

Homeostatic Imbalances
Angina pectoris• Thoracic pain caused by a fleeting
deficiency in blood delivery to the myocardium
• Cells are weakened Myocardial infarction (heart attack)
• Prolonged coronary blockage• Areas of cell death are repaired with
noncontractile scar tissue

Coronary Artery Disease(CAD)Diagnosis
• Stress test• Echocardiography• Cardiac catheterization• Coronary angiography

Coronary Artery Disease(CAD)Treatment
• Coronary bypass grafting (CABG)
• Percutaneous transluminal coronary angioplasty (PTCA)

Procedures for reestablishing blood flow in occluded coronary heart disease

Defibrillator

Inquiry
1. Name the 2 pacemakers of the heart.2. What is the QRS wave?3. What is the middle layer of heart tissue
called?4. What is the parietal pericardium?5. Why is the left ventricle thicker walled than
the right?6. What blood vessel returns blood from the
lungs to the heart?7. What is the function of the chordae tendinae?8. How does the heart avoid going into tetanus?9. What function does serous fluid serve?