Foot and Ankle Pain
description
Transcript of Foot and Ankle Pain

Foot and Ankle Pain
Prof. Dr. Ece AYDOĞ
Physical Medicine and Rehabilitation

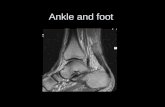
FUNCTIONAL ANATOMY AND BIOMECHANICS The ankle, or tibiotalar,
joint comprises the articulation between the foot (talus) and the lower leg (distal tibia and fibula).

Anatomic regions Forefoot; toes and
metatarsal bones; metatarsophalangeal (MTP) and interphalangeal joints
Midfoot; tarsometatarsal (TMT) joints connect the forefoot to the midfoot, which comprises the three cuneiform bones, the navicular, and the cuboid
Hindfoot; talus and calcaneus, talocalcaneal (subtalar), talonavicular, and calcaneocuboid articulations.

PHYSICAL EXAMINATION
Location of swelling Deformity;
Hallux valgus or bunion Hammer toes, Flatfoot deformity (characterized by hindfoot
valgus/forefoot abduction). Callosities Rheumatoid nodules Ulcerations Wear patterns: “A deformed foot can deform any good shoe; in fact, in
many cases the shoe is a literal showcase for certain disorders.”

Hallux Valgus
Gece Ateli


Flatfoot Deformity

Flatfoot Deformity

Rheumatoid nodules Diabetic ulcer

PHYSICAL EXAMINATION
Metatarsal heads and MTP joints palpation in patients with RA or nonarthritic metatarsalgia; tenderness, synovitis, and swelling.
Tenderness over the posterior aspect of calcaneus; Achilles tendinitis
Pain over the medial tubercle (palpable on the medial plantar surface); plantar fasciitis.
Tenderness over sinus tarsi of the hindfoot (located laterally, just anterior and distal to the tip of the fibula); talocalcaneal joint pathology
Tenderness over the anterior joint line usually correlates with ankle joint pathology.

Calcaneal medial tubercule (Plantar fasciitis)
Talocalcaneal yoint pathology

PHYSICAL EXAMINATION
Range of motion analysis: 10 to 20 degrees of
dorsiflexion 40 to 50 degrees of
plantar flexion.

Normal hindfoot inversion and eversion are each approximately 5 degrees.

COMMON CAUSES OF ANKLE PAIN
ANTERIOR AND CENTRAL ANKLE PAIN Spur and osteophyte formation
Arthritis (degenerative or inflammatory) Anterior tibial tendon tendinitis or tendinosis
Stress fractures
Osteochondral defect

POSTERIOR JOINT PAINAchilles tendon
in most instances, Achilles pain results from degenerative tendinosis, with or without an overlying tendinitis.
associated intratendinous spur formation is common
spur excision also frequently entails tendon débridement, reconstruction, and transfer.

Spur formation(Plantar calcaneal and achilles tendon)

Achilles tendon
protected by two distinct bursae.
more superficial bursa is immediately subcutaneous and becomes inflamed primarily with irritation from ill-fitting shoes with a tight counter (“pump bump”).

Achilles tendon
“retrocalcaneal” bursa is a larger structure that lies deep to the Achilles tendon. Inflammation of this structure often accompanies Achilles tendinitis/tendinosis.
It also may be irritated by an enlarged posterior superior calcaneal tuberosity, sometimes referred to as a Haglund's deformity.

MEDIAL ANKLE PAIN
Stress fracture
Arthritis
Inflammation or degeneration (or both) of the posteromedial flexor tendons, including the posterior tibial tendon and the flexor hallucis longus and flexor digitorum longus tendons
long-standing synovitis and dysfunction of posterior tibial tendon ultimately may lead to collapse of the arch and the development of an acquired flatfoot deformity.

MEDIAL ANKLE PAIN
Tarsal tunnel syndrome is another cause of posteromedial ankle pain. pain that radiates
into the plantar foot
percussion of the tarsal tunnel reproduces these symptoms (Tinel's sign).

LATERAL ANKLE PAIN
Stress fracture Arthritis Peroneal tendon pathology;
tenosynovitis
longitudinal “split” tears
chronic tendon instability
the tendons sublux over the posterolateral edge of the fibula, causing pain and attritional tearing

COMMON CAUSES OF FOOT PAIN
FOREFOOT PAIN The forefoot region is a common location of
foot pain.

Rheumatoid Arthritis
inflammation and progressive MTP synovitis eventually lead to capsular distention and destruction.
loss of collateral ligament stability and, finally, destruction of the articular cartilage and bone

FOREFOOT PAIN
Hallux valgus deformity or bunion; commonly encountered in patients with and without
inflammatory arthritis RA; 70% progression of this deformity may be accelerated
further by loss of support from the adjacent lesser MTP joints.
Hallux rigidus Degenerative arthritis Sesamoiditis Osteonecrosis Fracture

FOREFOOT PAIN
Claw toes Hammer toes Mallet toes Etiologies;
arthritis, trauma, nerve/muscle imbalance, and chronic use of shoes with inadequate toe boxes.
Instability; mechanical causes (long second metatarsal) inflammatory disease MTP joint subluxation

Claw toe
Mallet finger

FOREFOOT PAIN
Metatarsalgia Gastrocnemius contracture or tight Achilles tendon; the
forefoot is prematurely loaded during the stance phase of gait.
Hammer toes and mallet toes can result in downward pressure on the metatarsal heads, leading to metatarsalgia.
In elderly patients and patients with inflammatory arthritis, atrophy of the plantar fat pad of the forefoot also can result in metatarsalgia.

LATERAL FOREFOOT
Morton's neuroma: between the third and
fourth metatarsal heads
burning, aching, or shooting pain
symptoms are especially exacerbated with tight shoes
.

LATERAL FOREFOOT
Bunionette: angular deformity of
the fifth toe
pain over the lateral aspect of the fifth metatarsal head

MIDFOOT PAIN
Arthritis at the TMT joints most frequently the first TMT joint on the
medial side of the foot instability of the first TMT joint, repetitive
stress can lead to dorsiflexion of the first metatarsal
midfoot arthritis can lead to an abduction deformity of the foot, where the forefoot and metatarsals deviate outward.

MIDFOOT PAIN
lateral midfoot pain: peroneal tendinitis stress fracture of the fifth metatarsal
medial midfoot pain: accessory navicular bone osteonecrosis of the native navicular bone insertional posterior tibial tendinitis

HINDFOOT PAIN
joints of the hindfoot talonavicular talocalcaneal calcaneocuboid
degenerative and inflammatory arthritis RA; 21% to 29%
posterior tibial tendinitis and dysfunction Inflammation Degeneration Dysfunction

HEEL PAIN Plantar fasciitis;
inferior heel pain worse when first getting up in the morning or getting up after
sitting for a long time Achilles tendinosis;
posterior heel pain worse during or after exercise
Nerve entrapment; first branch of the lateral plantar nerve (Baxter's nerve) medial heel pain
Calcaneal stress fracture; medial and lateral pain Calcaneal stress fracture usually can be distinguished by a
positive “squeeze test,” with compression of both sides of the heel.

NONOPERATIVE TREATMENT
Medical management Nonsteroidal anti-inflammatory drugs
Steroids
Disease-modifying antirheumatic drugs

NONOPERATIVE TREATMENT
Shoewear modification deep, wide toe box firm heel counter soft heel
Well-constructed walking or jogging shoes usually provide sufficient room for mild-to-moderate deformities

NONOPERATIVE TREATMENT
Often it is necessary to prescribe a custom orthotic insert for patients with more moderate deformities
It is typically necessary to remove the insole of the shoe to make
room for the orthotic insert
Custom orthoses; rigid, semirigid, softer accommodative devices
Rigid and semirigid orthoses usually are used to correct supple deformities and should be used with caution in patients with arthritis
Most walking or jogging shoes suffice.



NONOPERATIVE TREATMENT
More commonly, these patients, especially if they have RA, benefit from accommodative orthoses (i.e., orthoses made of softer material that can be molded to “accommodate” a deformity)
Accommodative orthoses can be modified further by incorporating a “relief” under a deformity, further unloading it
When sending patients for orthoses, it is best to provide the
orthotist with a prescription that includes the patient's precise diagnosis (e.g., metatarsalgia) and the type of orthosis and any modifications desired (e.g., a “custom accommodative orthosis with a relief under the lesser metatarsal heads”).

Injections
Mixture of anesthetic and corticosteroid
Injection of a corticosteroid near or directly into a tendon can adversely affect the biomechanical properties of the tendon, ultimately leading to rupture
Avoid corticosteroid injections into the lesser MTPs when there is evidence of joint instability. Such injections can lead to further attenuation of the
joint capsule and result in frank joint dislocation.

OPERATIVE TREATMENT
If symptoms persist despite nonoperative management, surgical intervention should be considered Arthrodesis (joint fusion), Arthroplasty (joint replacement), Corrective osteotomy, Tendon débridement and transfer, Synovectomy (joint or tendon).