Extracranial Vertebral Artery Dissections: A Review of 13...
Transcript of Extracranial Vertebral Artery Dissections: A Review of 13...

1037
Extracranial Vertebral Artery Dissections:A Review of 13 Cases
Jean-Louis Mas, MD, Marie-Germaine Bousser, MD, Dominique Hasboun, MD,
and Dominique Laplane, MD
Clinical and radiologic findings in 13 patients (11 women, 2 men) with extracranial vertebral arterydissection are reported. Dissection was spontaneous in 8 patients, occurred after neck manipulation in2 and after a potential minor injury to the neck in 3. Six had a history of common migraine, 4 wereusing oral contraceptives at the time of dissection, and 3 had fibromuscular dysplasia. Dissection wasbilateral in 8 patients and associated with carotid dissection in 3. It usually presented with neck oroccipital pain preceding basilar ischemic symptoms by a few minutes to 1 month. In 3 patients,transient ischemic attacks were the only manifestation of basilar ischemia, and in 1 patient there wasno symptom of basilar ischemia despite bilateral vertebral dissection. In 19 of the 21 dissectedvertebral arteries, the angiographic appearance was that of an irregular stenosis, which was associat-ed in 6 arteries with pseudoaneurysmal formation. In 2 patients, 1 vertebral artery was occluded butthe contraiateral artery showed the typical irregular stenosis. The dissection involved only the thirdsegment in 33%, only the second segment in 24%, and 2 or more segments in 38%. Eleven patientswere treated with anticoagulants and 2 with aspirin; 11 recovered without sequelae and 2 had residualdeficit. No recurrence was observed (mean follow-up 34 months). At control angiography (n = 12) orultrasonic study (n = 1), 63% of dissected vertebral arteries had returned to normal, 26% showedmarked improvement, and 11% were occluded. Our patient characteristics are compared with thoseof previously published cases. The validity of the distinction between spontaneous dissection anddissection associated with minor trauma is discussed. (Stroke 1987; 18:1037-1047)
Extracranial vertebral artery dissection is recog-nized as a cause of stroke with increasing fre-quency.1"3 However, the clinical and radiolog-
ic features of this entity and its natural history are lesswell known than those of carotid dissection.4
The diagnosis of dissection relies on angiography,which reveals irregular stenosis with or without pseu-doaneurysm,2-5"7 double lumen,1 '3 or occlusion8 of 1 orboth extracranial vertebral arteries. Of these three fea-tures, the only pathognomonic one is the double lu-men. Stenosis is a less specific cause, but becomessuggestive when it is irregular and involves segmentsof the vertebral artery usually not involved by ather-oma. Occlusion is the least specific since it can be dueto thrombosis of any cause.4 We were interested instudying nonocclusive forms of extracranial vertebraldissection and report here on 13 such patients withspecial emphasis on the role of trauma, the long-termoutcome of these patients, and the evolution of thearterial lesions.
Subjects and MethodsThirteen consecutive patients (mean age 38.2 years,
range 26—48) with angiographically diagnosed extra-
From the Service de Neurologie, Centre Raymond Garcin, H6pi-tal Sainte-Anne (J.-L.M.) and the Clinique des Maladies du Sys-teme Nerveux, Hdpital de la Salp6triere (M.-G.B., D.H., D.L.),Paris, France.
Address for correspondence: Dr. J. L. Mas, Service de Neurolo-gie, Centre Raymond Garcin, Hdpital Sainte-Anne, 1 rue Cabanis,75674 Paris Cedex 14, France.
Received February 23, 1987; accepted June 10, 1987.
cranial vertebral artery dissection were observed fromNovember 1980 to November 1986 in one neurologydepartment. Patients whose angiogram showed onlyvertebral artery occlusion were excluded. Cases 3 and4 have already been published,9 and 4 others (Cases 1,6, 7, and 8) have been described angiographically.10
Patients were specifically asked about history ofmigraine (defined according to the Ad Hoc Committeeon Classification of Headache"), high blood pressure,diabetes mellitus, hypercholesterolemia, smoking,and past or current use of oral contraceptives. Particu-lar attention was paid to any unusual neck motion ortrauma that could have happened in the previousweeks, days, or hours as well as to all sports activitiesor strenuous exercises performed in the same period.The clinical findings are reported in Table 1.
All patients had blood cell count, sedimentationrate, protein electrophoresis, fasting serum glucoseand cholesterol, coagulation study (prothrombin time,activated partial thromboplastin time, platelet count),electrocardiogram, chest x-ray, brain computed to-mography (CT) scan, and cerebral angiography. Thelocation of the arterial stenosis on the angiograms wasdefined according to the following segmentation of thevertebral artery: first segment, VI, from its origin to itsentry into the foramen transverse of C6; second seg-ment, V2, from the foramen of C6 to that of C2; thirdsegment, V3, from C2 to the dura; and fourth segment,V4, intracranial vertebral artery. The angiographicfindings are reported in Table 2.
All patients had regular clinical follow-up until No-vember 1986. Evolution of the arterial lesions was
by guest on July 9, 2018http://stroke.ahajournals.org/
Dow
nloaded from

1038 Stroke Vol 18, No 6, November-December 1987
Table 1. Clinical Findings of Presently Reported Cases
Case
1
2
3*
4t
5
6
7
8
9t
10
11
12
13
Sex Age
F48
F36
F40
F42
M36
F32
F26
F27
F42
F43
F47
M38
F40
History
High BP
Migraine, pastuser of OC
High BP, cur-rent user ofOC
Current user ofOC, FMD
—
Pregnancy, pastuser of OC,FMD
Past user ofOC, smokingabuse
Past user ofOC, postpar-tum migraine
Current user ofOC, premen-strual head-aches
Migraine, cur-rent user ofOC, smokingabuse
Migraine
Migraine, FMD
Migraine, highBP
Neck trauma
No
No
No
No
Dubious
No
No
Neck manipulation
No
No
Neck manipulation
Dubious
Dubious
Neckor
headpain Ischemic signs
— VBTIA
+ L lateral med-ullary(NDMS)
+ VB TIA, bruit,Homer'ssyndrome
+ VB TIA, ca-rotid NDMS
+ Locked-insyndrome(MS)
+ L lateral med-ullary(NDMS)
+ Diffuse brain-stem (nodefinite syn-drome) (ms)
+ VB TIA,brainstem(no definitesyndrome)(NDMS)
+ No VB symp-toms, carotidTIA, NDMS
+ Lower brain-stem (MS)
+ Vestibular syn-drome (ms)
+ L lateral med-ullary(NDMS)
+ VBTIA,upper brain-stem (NDMS)
Treatment
AC (3 yr)
ASA
AC (7 mo), ASA
AC (1 yr), ASA
AC (5 mo), ASA
AC (9 mo), ASA
AC (6 mo)
AC (9 mo), ASA
AC (6 mo), ASA
ASA
AC (6 mo)
AC (2 mo), ASA
AC (3 mo), ASA
Immediateoutcome
Favorable
Favorable
Favorable
Favorable
Sequelae
Favorable
Favorable
Favorable
Favorable
Sequelae
Favorable
Favorable
Favorable
Follow-up
Length(months)
69
57
51
53
50
39
38
36
20
12
9
6
6
Recur-rence
No
No
No
No
No
No
No
No
No
No
No
No
No
BP, blood pressure; TIA, transient ischemic attack; VB, vertebrobasilar; AC, anticoagulant; OC, oral contraceptives; NDMS, nondisablingmajor stroke; ASA, aspirin; MS, major stroke; FMD, fibromuscular dysplasia; ms, minor stroke.
•Concomitant bilateral internal carotid artery dissection.tConcomitant unilateral internal carotid artery dissection.
assessed with angiography in 10 patients, with angiog-raphy and ultrasonography in 2 patients, and with ul-trasonography alone in 1 patient. The method of ultra-sonography (continuous-wave Doppler and duplexscanning) of the vertebral arteries has previously beendescribed,12 and detailed ultrasonic data on Patients 6,7, and 8 are reported in another paper.13
Patient 1A 48-year-old woman experienced bilateral blurred
vision, dizziness, loss of balance, and decreased sen-sation in her left hand and foot on December 3, 1980.These symptoms disappeared within a few hours.Right brachial arteriography on December 5, 1980,
showed an irregular stenosis of the second and proxi-mal third segments of the right vertebral artery with ananeurysmal dilatation at the C2 level. The distal rightvertebral artery was not opacified. The right carotidartery was normal. Anticoagulants were started on De-cember 6, 1980, and stopped 8 days later. On thefollowing day, she had numbness of the right side ofher face and decreased sensation of her left limbs.These symptoms disappeared over a few hours and shewas again given anticoagulants. Transfemoral arteri-ography on December 23, 1980, showed that the rightvertebral artery was normal except for a mild residualstenosis at the C4-C5 level. Internal carotid and leftvertebral arteries were normal. In October of 1983,
by guest on July 9, 2018http://stroke.ahajournals.org/
Dow
nloaded from

Mas et al Extracranial Vertebral Artery Dissections
Table 2. Angiographk Findings of Presently Reported Cases
1039
Case
1
2
3*
4t
5
6
7
8
9t
10
11
12
13
Vessel locus lesion
RVA: V2, V3 (distal RVA notopacified)
LVA: V3, V4
RVA: V3LVA: V2, V3
LVA: V3
RVA: V3LVA: V3
RVA: V2, V3 (distal RVA notopacified)
LVA: V2, V3
RVA: V2LVA: V2, V3
RVA: V2LVA: V2
RVA: V2LVA: V2
RVA: V3LVA: V2, V3
RVA: VI, V3, V4
LVA: V4
LVA: V3
LVA: V3
Vascular lesion
Irregular stenosis (C5-C1), aneurysmaldilatation (C2)
Irregular stenosis, aneurysmal dilatation(C2)
Severe stenosis (Cl)Irregular stenosis (C6-C3), aneurysmal
dilatation (C3-C2), sacciform aneu-rysm (Cl)
Severe stenosis (C2)
Severe stenosisIrregular stenosis
Irregular stenosis (C6-C1), aneurysmaldilatation (Cl)
Irregular stenosis (C6-C1)
Irregular stenosis (C6-C2)Irregular stenosis (C6-C1)
Occlusion (C6-C2)Irregular stenosis (C6-C2)
Stenosis (C3)Irregular stenosis (C6-C2), severe
stenosis (C2)
Irregular stenosis (Cl), aneurysm (Cl)Irregular stenosis (C5-C4), severe
stenosis (Cl)
Irregular stenosis (C2 to intracranialVA), aneurysmal dilatation (C7)
Occlusion (intracranial VA)
Irregular stenosis (Cl)
Irregular stenosis
Control angiography
Mild residual stenosis (C4-C5)
Normal
NormalNormal (US)
NormalNormal
NormalNormal
Occlusion (US)
Normal
Normal (US)Normal (US)
NormalNormal
NormalSlight irregularities
Mild residual stenosisNormal
Mild stenosis of intracranial VA
Occlusion
Normal
Slight irregularities
Timebetween
angiograms
18 days
4 yr, 8 mo
3 mo
2 mo16 mo
19 mo
9 mo
3 mo
3 mo
5 mo
7 days1 yr
7 mo
2 mo
2 mo
RVA, right vertebral artery; LVA, left vertebral artery; US, ultrasonography.•Concomitant bilateral internal carotid artery dissection.tConcomitant unilateral internal carotid artery dissection.
while still on anticoagulants, she had a right capsularhemorrhage. Anticoagulants were stopped. No furthersymptom has occurred since then.
Patient 2A 36-year-old woman suddenly developed pain and
stiffness in her neck on December 3, 1981. Her stiffneck persisted over the next few days and, on Decem-ber 15, she noted difficulty in swallowing, decreasedtemperature sensation over her right limbs, left ptosis,and about 1 hour later, severe vertigo and aphonia.Bilateral brachial arteriography on January 7, 1982,revealed a severe stenosis of the third and fourth seg-ments of the left vertebral artery with an aneurysmaldilatation at the C2 level. The right vertebral and inter-nal carotid arteries were normal. She was given 1 gaspirin/day for 1 year. She recovered completely overthe next few weeks and has been symptomless sincethen. In October of 1986, digitized intra-arterial arteri-ography showed a normal left vertebral artery.
Patient 3A 40-year-old woman had acute onset of headache,
neck pain, vomiting, and a bruit in her left ear on
January 20, 1982. Ten days later she had a brief loss ofconsciousness. Four days after her loss of conscious-ness, she experienced a sudden episode of bilateralblurred vision, which lasted 5 minutes. On admissionthe next day, examination was normal except for a leftHomer's syndrome and a bruit over the left side of herneck. Transfemoral arteriography on February 10,1982, revealed an irregular stenosis of the second seg-ment of the left vertebral artery (from C6 to C3), withaneurysmal dilatation at the C3^C2 level, a sacciformaneurysm at the Cl level, and a severe stenosis of thethird segment of the right vertebral artery at the Cllevel. Both internal carotid arteries were severely nar-rowed, the right one from 1 cm above the origin up tothe siphon and the left one at the C1-C2 level, withaneurysmal dilatation just below the entrance into thecarotid canal. The renal arteries were normal. Thepatient was given anticoagulants for 7 months fol-lowed by 1 g aspirin/day. The bruit and headache dis-appeared gradually over 2 weeks. On May 5, 1982,digitized intravenous arteriography was normal exceptfor the persistence of a sacciform aneurysm of the leftinternal carotid artery at the Cl level. The left vertebralartery was not properly opacified, but continuous-
by guest on July 9, 2018http://stroke.ahajournals.org/
Dow
nloaded from

1040 Stroke Vol 18, No 6, November-December 1987
wave Doppler of this artery was normal. She has beensymptomless since then.
Patient 4A 42-year-old woman experienced a 10-minute epi-
sode of bilateral blurred vision on February 20, 1982.A similar episode occurred the next day and was ac-companied by severe neck pain, which lasted a week.On February 28, she suddenly heard a pulsatile bruit inher right ear and developed weakness and numbness ofthe left side of her body, which gradually improved.Fifteen days after onset, clinical examination was nor-mal except for a slight impairment of joint positionsense on her left side. Transfemoral arteriography onMay 10, 1982, showed a severe stenosis of the thirdsegment of the left vertebral artery at the C2 level. Theright internal carotid artery was severely narrowedfrom 1 cm above the origin up to the entrance into thecarotid canal, with an aneurysm at the Cl level. Theleft internal carotid artery was not selectively catheter-ized but looked extremely irregular on global aortogra-phy. The right vertebral artery was normal. The rightrenal artery had a beaded appearance, suggestive offibromuscular dysplasia. On the day after angiogra-phy, she suddenly developed a moderate dysphasia,which gradually improved. She was given anticoagu-lants for 1 year followed by 1 g aspirin/day. Digitizedintravenous arteriography 2 months after onset showedrecanalization of the carotid and vertebral arteries, butthe aneurysm of the right carotid artery at the Cl levelwas still visible. On digitized intra-arterial arteriog-raphy 16 months later, the right carotid artery wasnormal. She has been symptomless since then.
Patient 5
A 36-year-old man with neck pain for 3 days devel-oped a locked-in syndrome over a few hours on March31, 1982. Several days before the onset of neck pain,he had done heavy work in his home but could notrecall any unusual neck movement. Transfemoral arte-riography on March 31 showed a severe stenosis of thethird portion of both vertebral arteries. Carotid arterieswere normal. Anticoagulants were started immediatelyand replaced 5 months later by 1 g aspirin/day. Hegradually improved but remains severely disabled witha right hemiparesis. On digitized intra-arterial arteri-ography performed on December 5, 1983, the verte-bral, carotid, and renal arteries were normal.
Patient 6A 32-year-old woman 38 weeks pregnant awoke
with a severe neck pain on March 15, 1983. Two dayslater, her blood pressure rose to 180/100 mm Hg and itwas decided to induce labor. Delivery was normal, buther neck pain persisted over the next few days. OnMarch 23, she had a diffuse headache followed 2 dayslater by severe vertigo and tingling over the left part ofher face and over her right limbs. Examination re-vealed a left Wallenberg syndrome. Bilateral brachialand left carotid arteriography on March 30, 1983,showed an irregular and severe stenosis of the second
and third segments of the right vertebral artery, with ananeurysmal dilatation at the Cl level. The distal intra-cranial vertebral artery and the basilar artery were notfilled by the right vertebral artery. The left vertebralartery was irregularly stenosed in its second and thirdsegments. The intracranial left vertebral artery and thebasilar artery were thin, but their walls were regular.There were slight irregularities of both internal carotidarteries suggestive of fibromuscular dysplasia. Shewas given anticoagulants for 9 months, then 1 g aspir-in/day. No symptoms occurred during follow-up, andthe only residual signs were a rotatory nystagmus anddecreased sensation over her left face. A digitized in-tra-arterial arteriography on December 12, 1983,showed a normal left vertebral artery; the right verte-bral artery was not opacified with certainty but it ap-peared occluded at duplex scanning on December 14,1983.
Patient 7A 26-year-old woman suddenly experienced severe
neck pain on July 8, 1983, followed a few minuteslater by paresthesia in both arms, on the upper part ofher back, her neck, and her left tongue. She had diffi-culty moving her upper limbs and moderate dysarthria.All symptoms disappeared spontaneously over thenext 3 days. Examination on July 21 disclosed onlyincreased deep tendon reflexes and decreased sensa-tion of her right thumb. Bilateral brachial arteriog-raphy on July 26, 1983, showed a severe and irregularstenosis of the second segment of the right vertebralartery and of the second and proximal third segmentsof the left vertebral artery with reinjection of the distalpart of both vertebral arteries via muscular arteries.She was treated with anticoagulants for 6 months andhas been symptomless since then. Ultrasonographyperformed on September 21, 1983, showed normalvertebral arteries.
Patient 8A 27-year-old woman experienced pain in the right
side of her neck on November 15, 1983, 2 weeks aftera normal delivery. On November 21, she had a neckmanipulation and the pain disappeared. She was per-fectly well until December 31, 1983, when she sud-denly experienced a 1-hour episode of paresthesia overher whole face with vertigo, aphonia, right hemipare-sis, and vomiting. She recovered completely, but a fewhours later she had a similar episode with horizontaldiplopia and difficulty in swallowing. She improvedagain, but on admission 2 days later, right facial andhand weakness, incoordination of her right limbs, andminor dysarthria were still present. A few hours afteradmission, she experienced numbness of her face andleft arm and a left hemiparesis, which disappearedcompletely in 1 hour. Transfemoral arteriography onJanuary 6, 1984, showed normal carotid arteries. Theright vertebral artery was occluded from C6 to C2 andwas reinjected via anastomosis with muscular arteries.The left vertebral artery was moderately and irregular-ly stenosed from C6 to C2. She was given anticoagu-lants for 9 months, then 1 g aspirin/day. She recovered
by guest on July 9, 2018http://stroke.ahajournals.org/
Dow
nloaded from

Mas et al Extracranial Vertebral Artery Dissections 1041
completely over the next few weeks and has beensymptomless since then. In April of 1984, digitizedintra-arterial arteriography showed normal vertebraland renal arteries.
Patient 9A 42-year-old woman with neck pain for 1 month
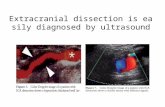
on November 11, 1984, suddenly experienced a righthemiparesis and dysphasia, which disappeared in 2hours. A few hours later, over 2 hours she developed adense hemiplegia and severe dysphasia. CT scanshowed a hypodensity in the left middle cerebral arteryterritory. Arch arteriography on November 19, 1984,revealed stenosis of the distal second segment (C3level) of the right vertebral artery. The left vertebralartery was irregularly narrowed in its second segmentand stenosed at the C2 level. This vessel was poorlyvisualized above C2, but its caliber looked normal.There was a tapered occlusion of the left internal carot-id artery. The right carotid artery was normal (Figure
1, left). She was given anticoagulants for 6 months,then 1 g aspirin/day. She recovered completely over afew weeks and has been symptomless since then. Atrepeat transfemoral angiography on April 16, 1985,the right vertebral artery was normal; the left vertebralartery was still slightly irregular in its second segment,but the severe stenosis previously seen at the C2 levelhad disappeared (Figure 1, right). The left internalcarotid artery remained occluded. Renal arteries werenormal.
Patient 10A 43-year-old women suddenly experienced a right
nuchal pain on October 10, 1985, which became bi-lateral a few days later. On October 22, 1985, shedeveloped dizziness, dysarthria, difficulty in swallow-ing, and obnubilation over the course of 1 hour. Ex-amination revealed increased deep tendon reflexes,left hemiplegia, left extensor plantar response, de-creased sensation on the left side of her face, and
FIGURE 1. Patient 9. Left: Arch arteriography, November 19, 1984. Stenosis of right vertebral artery at C3 level (large arrow),irregular stenosis of second segment of left vertebral artery with severe stenosis at C2 level (small arrows), tapered occlusion of leftinternal carotid artery (long arrow). Right: Transfemoral arteriography, April 16, 1985. Slight irregularities of second segment of leftvertebral artery and disappearance of severe stenosis at C2 level.
by guest on July 9, 2018http://stroke.ahajournals.org/
Dow
nloaded from

1042 Stroke Vol 18, No 6, November-December 1987
absent gag reflex. Digitized intra-arterial arteriographyon October 31, 1985, showed irregular stenosis of thethird segment of the right vertebral artery with an aneu-rysm at the Cl level (Figure 2, top left); the left verte-bral artery could not be opacified. Transfemoral arteri-ography on November 7, 1985, revealed mild residualstenosis of the right vertebral artery (Figure 2, topright), moderate stenosis of the proximal second seg-ment, and severe eccentric stenosis of the third seg-ment of the left vertebral artery (Figure 2, bottom left).The carotid arteries were normal. She was given 0.5 gaspirin/day for 9 months and recovered incompletely.In November of 1986, she was admitted again becauseof sudden recurrence of nuchal pain. Examination wascomparable with the previous one. A left brachial arte-riography revealed a normal left vertebral artery (Fig-ure 2, bottom right).
Patient 11A 47-year-old woman, while pushing the cord of the
phone with her foot on January 20, 1986, suddenlyexperienced a left occipital pain that worsened duringthe following hours. From January 21 to 27, 1986, shehad 4 neck manipulations, but the pain remained un-changed. On February 2, 1986, she experienced oscil-lopsia and vomiting. Examination 2 days later dis-closed a rotatory nystagmus on left lateral gaze. Rightbrachial arteriography on February 7, 1986, showed ananeurysmal dilatation of the first segment (Figure 3)and an irregular stenosis of the third and fourth seg-ments of the right vertebral artery, which did not fillthe basilar artery. A digitized intra-arterial arteriog-raphy on February 13, 1986, revealed normal carotidarteries, occlusion of the fourth segment of the leftvertebral artery, and retrograde filling of the basilarartery and both posterior inferior cerebellar arteries.She was treated with anticoagulants, recovered com-pletely in a few days, and has been symptomless sincethen. At the control digitized intra-arterial arteriog-raphy in September of 1986, the right vertebral arterywas normal except for a mild stenosis of its fourthsegment, whereas the left vertebral artery remainedoccluded.
Patient 12A 38-year-old man had pain and stiffness in the left
part of his neck in early March of 1986. The pain lastedfor 5 days and reappeared 20 days later. On March 27,while turning his head to look over his shoulder, he felta "cracking" in his neck, after which the pain disap-peared. The following morning, he experienced dizzi-ness, vomiting, and loss of balance when walking. Inthe evening, he had difficulty in swallowing and asevere inspiratory dyspnea. Examination showed de-creased sensation of his right limbs, left Homer'ssyndrome, and left pharyngeal paralysis. Bilateral bra-chial arteriography on April 4, 1986, showed moderateand irregular stenosis of the third segment of the leftvertebral artery. The right vertebral artery was verythin and did not fill the basilar artery. The right internalcarotid artery was normal. He was given anticoag-
ulants for 2 months, then 1 g aspirin/day. Examination3 months after the onset disclosed only a left Homer'ssyndrome. Transfemoral arteriography on June 11,1986, revealed a normal left vertebral artery and abeaded appearance of the right renal artery suggestiveof fibromuscular dysplasia. The right vertebral arterycould not be opacified.
Patient 13A 40-year-old woman noted neck and back pain
after washing the walls and ceiling of her kitchen onMay 11, 1986. Ten days later, she had a 10-minuteepisode of vertigo and vomiting. On the following day,she was admitted to our hospital because of clouding ofconsciousness. Examination also found slurredspeech, bilateral extensor plantar responses, and pa-ralysis of vertical gaze. Bilateral brachial arteriog-raphy on May 28, 1986, revealed stenosis of the thirdsegment of the left vertebral artery at the Cl level. Shewas given anticoagulants for 3 months, then 1 g aspir-in/day and improved rapidly. On July 23, 1986, ex-amination was normal, and digitized intra-arterial an-giography showed only slight irregularities of the leftvertebral artery.
DiscussionThe incidence of extracranial vertebral artery dis-
section is not precisely known; for both carotid andvertebral dissections, it is estimated to be from "1 to 3cases per year in large academic-affiliated hospitals.1"The fact that our 13 patients were seen in 6 years in alarge neurology department is in accordance with thisfigure and suggests that this disease is not uncommon.
To compare our patient characteristics with those ofthe previously published cases, we reviewed publishedreports of pathologically confirmed2'5"7'415 and angio-graphically diagnosed'-216"3* extracranial vertebral dis-sections, again excluding patients whose angiogramshowed only vertebral artery occlusion. In some re-ports, 16-18,21.22.24.27,29.34.35 a u t h o r s were uncertain of thenature of the arterial lesion and did not call the processdissection. These cases, however, were clinically andangiographically similar to those reported as dissectionand will therefore be taken into account. Thirty-eightcases with 49 nonocclusive forms of extracranial verte-bral dissection have thus been selected (Table 3).
The present study confirms that vertebral dissectionoccurs predominantly in middle-aged adults, but thefemale preponderance was more marked in our study(85%) than in previous reports (53%).
Particular attention has been paid in our study tosome factors that might predispose to arterial dissec-tion: chronic hypertension and atherosclerosis, fibro-muscular dysplasia, migraine, and oral contraceptiveuse. Chronic hypertension was present in 3 of ourpatients; none had arteriographic evidence of athero-sclerosis. Angiographic evidence of fibromusculardysplasia is reported in about 15% of extracranial ca-rotid dissection and in 0 .5 -1% of all arteriograms4; itwas found in 23% of the patients in our series and in5% in previous reports. The higher prevalence of fibro-
by guest on July 9, 2018http://stroke.ahajournals.org/
Dow
nloaded from

Mas et al Extracranial Vertebral Artery Dissections 1043
\
W-006/04:Vertebrate I
FIGURE 2. Patient 10. Top left: Digitized intra-artehal arteriography, October 31, 1985. Irregular stenosis of third segment of rightvertebral artery with aneurysm at Cl level (arrow). Top right: Transfemoral arteriography, November 7, 1985. Mild residual stenosisof right vertebral artery (arrow). Bottom left: Transfemoral arteriography, November 7, 1985. Severe stenosis of third segment of leftvertebral artery (arrow). Bottom right: Left brachial arteriography, November 1986. Normal appearance of third segment of leftvertebral artery.
by guest on July 9, 2018http://stroke.ahajournals.org/
Dow
nloaded from

1044 Stroke Vol 18, No 6, November-December 1987
FIGURE 3. Patient 11. Right brachial arteriography, Feb-ruary 7, 1986. Aneurysmal dilatation of right vertebral artery atC7 level (arrow).
muscular dysplasia in our series could be due to thefact that carotid angiograms were available in all casesand renal angiograms in 6 of 13 cases. A history ofmigraine was more frequent in our series (46%) than inprevious reports of vertebral (8%) or carotid (11%)dissection.4 There are at least two reasons for the dis-crepancy between our data and the literature: first, thefemale preponderance in our population and, second,the fact that all our patients were specifically askedabout migraine. The association of migraine withdissection raises the possibility that the migraine-asso-ciated dissections were not dissections but rather com-plicated migraine with vasospastic changes on arteri-ography. However, this hypothesis is very unlikely.Among 6 such patients in the present series, 3 had ananeurysmal formation (Figure 3) in addition to steno-sis, which could not be due to vasospasm. Anotherwho had stenosis without aneurysm had increased di-ameter of both vertebral arteries on duplex scanning,which later returned to normal. '3 Four women (36%) in
our series were taking oral contraceptives at the time ofthe dissection; 4 additional women were past users oforal contraceptives, and 2 of these had their dissectionduring pregnancy or post partum. In prior reports, only10% of women were taking oral contraceptives at thetime of dissection. Internal carotid artery dissectionafter childbirth has been described,37 but the occur-rence of an extracranial vertebral artery dissection dur-ing pregnancy or post partum has, to our knowledge,never been reported. The high prevalence of migraineand hormonal factors in our series suggests that theycould be implicated in the pathogenesis of dissection.A case-control study is needed to test the associationbetween these two factors and dissection of cervicalarteries.
Clinical symptoms and signs were similar to thosepreviously decribed. Pain, usually located in the occi-put and/or posterior neck, was the presenting symptomin about 80% of the cases in our series as well as in theliterature, and preceded the first ischemic symptomfrom a few minutes to 1 month. Basilar ischemicsymptoms were present in 33 of 38 published cases(87%) and in 12 of our 13 cases. In 1 of our cases, aswell as in 5 reported cases,7'415'22-29 there were nobasilar ischemic symptoms; in 4 cases (References15, 22, 29, our Case 9), vertebral dissection was dis-covered when exploring a concomitant carotid dissec-tion. One patient7 experienced an isolated headachewhile another patient,14 dead of peritonitis, had bilater-al vertebral dissection discovered at autopsy. In allpublished cases with basilar ischemia and in 9 of our12 cases, the clinical presentation was a completedstroke, only rarely preceded by transient ischemic at-tacks (TIAs) (2 published reports and 2 in our series).Among completed strokes, the roughly 30% preva-lence of lateral medullary syndrome found in our seriesis in accordance with the literature but in disagreementwith the statement by Hart and Easton1 that extracrani-al vertebral artery dissection "usually presents withfeatures of the lateral medullary syndrome." TIAswere the only manifestation of basilar ischemia in 3 ofour cases and in none in the literature, which suggeststhat some cases may be underdiagnosed because of thestill-widespread reluctance to perform vertebral angi-ography. The development of good quality digitizedangiography should overcome this reluctance, andfour-vessel angiograms should be performed in youngor middle-aged adults presenting with "true" basilarTIAs,38 particularly if preceded by neck or head pain.
Extracranial vertebral artery dissection was morefrequently bilateral (61%) and associated with carotiddissection (23%) in the present series than in previouscases (29% and 8%, respectively), but a number ofpublished cases did not have four-vessel angiograms.Since it was decided to exclude vertebral artery occlu-sion as the only angiographic sign of dissection fromboth the present study and the review of the literature,it is not astonishing that the major finding was irregularstenosis of the extracranial vertebral artery; it was pres-ent in all our cases in at least 1 vertebral artery and inall but 2 published cases. In these 2 cases, 1 had a
by guest on July 9, 2018http://stroke.ahajournals.org/
Dow
nloaded from

Mas el al Extracranial Vertebral Artery Dissections 1045
Table 3. 51 Cases of Extracranial Vertebral Artery Dissection
No.
Age (range)
Sex ratio F/M
Migraine
Oral contraceptives
Rbromuscular dysplasia
Bilateral vertebral artery dissection
Carotid dissection
Localization||
VI only
V2 only
V3 only
^ 2 segments
Prior reports
38
34.7 (16-56)
1.1/1
3 (8%)
2 (10%)§
2 (5%)
11 (29%)
3 (8%)
(n = 49)
3 (6%)
10 (20%)
28 (57%)
8 (16%)
Present series
13
38.2 (26-48)
5.5/1
6 (46%)
4 (36%)
3 (23%)
8 (62%)
3 (23%)
(« = 21)110
5 (24%)
7 (33%)
8 (38%)
Spontaneous*
19
36.4 (25-48)
3.5/1
4 (21%)
6 (32%)
3 (16%)
9 (47%)
5 (26%)
(n = 28)
1 (4%)4 (14%)
11 (39%)
12 (43%)
Minor traumat
23
33.9 (15-49)
1.6/1
3 (13%)
0
1 (4%)
8 (35%)
1 (4%)
(/i = 31)l
0
9 (29%)
17 (55%)
4 (13%)
Dubious^
9
38.1 (29-56)
0.5/1
2 (22%)
0
1 (11%)
2 (22%)
0
(n = 11)2 (18%)
2 (18%)
7 (64%)
0
•Prior reports1.2,6,7,22,23,26,29 ^ pTesent ^^es (Cases 1-4, 6, 7, 9, 10).tPrior reports15-21'24'25'27'3032-36 and present series (Cases 8, 11).tPrior reports2'5'6'14'28'31 and present series (Cases 5, 12, 13).§Percent of women.|| n, number of dissected vertebral arteries.llOne patient had intracranial dissection on one side and extracranial dissection on the other side.
double lumen aspect1 and 1 an isolated pseudoaneu-rysm.5 Stenosis with pseudoaneurysm was found in29% of the cases (6 of 21 dissected arteries) in ourseries and in 20% of the cases in published reports. Thepresent study confirms the rarity of dissection limitedto the first segment (VI) of the vertebral artery. Themain discrepancy between our study and previous re-ports lies in the frequency of dissections restricted tothe V3 segment and of extensive dissection involving 2or more segments. In our series, these findings oc-curred in 33 and 38%, respectively, compared with 57and 16% in previous reports. No evidence of distalembolization, particularly to the posterior cerebral ar-tery, was observed in the present series, even in caseswith early angiograms. Distal embolization has pre-viously been reported in 2 patients with extracranialvertebral dissection625 and in 15% of cases with carotiddissection.4 It therefore seems that in the present se-ries, the dissecting process was more severe — at leastangiographically — than in previous ones, with agreater frequency of bilateral and extensive dissectionand of carotid involvement.
Follow-up angiography was performed from 7 daysto several years after the first angiography in 12 pa-tients with 19 vertebral dissections in the present seriesand in 16 published cases with 18 vertebral dissec-tions. The results were similar: normalization in 63%(12 of 19) initially dissected arteries compared with61% of cases, marked improvement in 26% of arteriescompared with 33% of cases, and occlusion in veryrare instances (11% in our series compared with 6% inpublished cases). Normalization or improvement isthus extremely frequent in this condition and an excel-lent argument in favor of the diagnosis. Combiningdata from our series and the literature, the return tonormal was observed in 3 weeks-56 months (mean 8.6
months) and improvement with residual stenosis in 7days-7 months (mean 2.7 months). This suggests thatresidual stenosis is just a step toward normalizationrather than a persisting sequela or evidence of preexist-ing arterial disease. However, the above figures mere-ly reflect the dates of angiographic controls and not thetrue timing of arterial improvement. Marked improve-ment was observed as early as 7 days after the firstangiogram in 1 of our cases, which stresses the pointthat the first angiography should be performed as earlyas possible so as not to overlook the diagnosis. Thetiming of control angiography is open to debate sincethe natural history remains poorly documented. If onlythose cases with control angiography performed within3 months after the first are taken into account (n = 20vertebral arteries), 60% were already normal and 40%improved; these proportions are similar to those foundwhen all cases (regardless of interval between angiog-raphies) are taken into account. This sugests that con-trol angiography could be performed around the thirdmonth.4
Secondary thrombotic and embolic complicationsare the rationale for use of anticoagulants and anti-platelets in dissection.4 Eleven of our patients weregiven anticoagulants; 10 recovered without significantsequelae and 1 had significant residual deficit. Aspirinwas given as the first treatment in the 2 remainingpatients; 1 recovered without sequelae and 1 had sig-nificant residual deficit. Prior reports with outcomedata include 27 patients. Ten patients21819-2*-30-32-33 weregiven anticoagulants; in 8, signs resolved satisfactori-ly, and 2 were left with significant residual deficit.Twelve patients2-6'5-20-22-25-29-31-34 were not given anti-coagulants; 6 recovered without significant sequelae, 5had residual deficit, and 1 died. The remaining 5 pa-tients6-7'617-21 were treated surgically; 3 recovered
by guest on July 9, 2018http://stroke.ahajournals.org/
Dow
nloaded from

1046 Stroke Vol 18, No 6, November-December 1987
without sequelae and 2 had residual deficit. The pres-ent study and previous ones indicate that anticoagu-lants are not harmful in this condition and could evenbe of benefit although no conclusion can be drawnfrom the comparison of nonrandomized treatmentgroups. Long-term outcome of patients with extracra-nial vertebral dissection appears to be favorable. In ourseries, long-term follow-up lasted 6-69 (average 34)months; no recurrence was observed. Prior reports in-clude 12 patients2-6-16-18-21-22-29-33 with follow-up of > 1year (average 21 months); only 1 patient had a recur-rent stroke, 1 year after the first stroke, the etiology ofwhich was uncertain.6
The relation of trauma to dissection is a complexissue. In the present series, dissection occurred afterneck manipulation in 2 patients and after a potentialminor injury to the neck in 3. The remaining 8 patientsabsolutely denied any recent trauma or abnormalmovement of the neck. Evidence from differentsources demonstrates that vertebral arteries may becompromised by head motion24 and, because of animpressive temporal relation, vertebral dissection hasbeen linked to chiropractic manipulation and to a vari-ety of circumstances associated with abrupt change inhead position.4 However, the degree of injury to theneck that could induce dissection is difficult to definequantitatively, and the potential role of minor necktraumas such as head turning while driving a car doesnot explain why such trivial traumas are inconsequen-tial in most people.1
We defined 3 categories according to the presence ofa potential traumatic event preceding the dissectionand its relation with it: 1) spontaneous, when there wasno recording of any form of injury to the neck or head;2) minor trauma, when there was a close temporalrelation of dissection with minor trauma (neck manipu-lation, sport activities, etc.); and 3) dubious, when thetemporal relation of dissection with potential traumawas questionable. In Table 3 are presented some char-acteristics of patients with extracranial dissections ac-cording to this classification. Compared with dissec-tion related to minor trauma, spontaneous dissection ismore frequent in women (F/M sex ratio 3.5/1 vs.1.6/1), more frequently involves a long portion of thevessel, and is more frequently associated with carotiddissection. Oral contraceptive use and fibromusculardysplasia are also more frequent in patients with spon-taneous dissection. However, these differences areminimal, and no specific particularity emerges thatcould discriminate spontaneous dissections from thoserelated to minor trauma. These two varieties can there-fore probably be considered two portions of the samespectrum and not two different entities.
AcknowledgmentsWe wish to thank Professors Chain and Rondot and
Dr. Gazengel for referring Patients 1, 7, 10, and 13and for allowing us to publish this material.
References1. Hart RG, Easton JD: Dissectons. Stroke 1985; 16:925-9272. Caplan LR, Zarins CK, Hemmati M: Spontaneous dissection
of the extracranial vertebral arteries. Stroke 1985; 16:1030-1038
3. Biller J, Hingtgen WL, Adams HP, Smoker WRK, GoderskyJC, Toffol GJ: Cervicocephalic arterial dissections. A ten-yearexperience. Arch Neurol 1986;43:1234-1238
4. Hart RG, Easton JD: Dissections of cervical and cerebral arter-ies. Neurol Clin 1983; 1:155-182
5. Ouchy H, Ohara I, Iwabuchi T, Suzuki J: Dissecting aneurysmof the extracranial portion of the vertebral artery. Vase Dis1965;2:340-344
6. Bladin PF: Dissecting aneurysm of carotid and vertebral arter-ies. VascSurg 1974;8:203-223
7. Hugenholtz H, Pokrupa R, Montpetit VJA, Nelson R, RichardMT: Spontaneous dissecting aneurysm of the extracranial ver-tebral artery. Neurosurgery 1982;10:96-100
8. Simeone FA, Goldberg HI: Thrombosis of the vertebral arteryfrom hyperextension injury to the neck. J Neurosurg 1968;29:540-543
9. Mas JL, Goeau C, Bousser MG, Chiras J, Verret JM, TouboulPJ: Spontaneous dissecting aneurysms of the internal carotidand vertebral arteries. Two case reports. Stroke 1985;16:125-129
10. Chiras J, Marciano S, Vega Molina J, Touboul PJ, Poirier B,Bories J: Spontaneous dissecting aneurysm of the extracranialvertebral artery (20 cases). Neuroradiology 1985;27:327-333
11. Ad Hoc Committee on Classification of Headache: Classifica-tion of headache. JAMA 1962;179:717-718
12. Touboul PJ, Bousser MG, Laplane D, Castaigne P: Duplexscanning of normal vertebral arteries. Stroke 1986;17:921-923
13. Touboul PJ, Mas JL, Bousser MG, Laplane D: Duplex scan-ning in extracranial vertebral artery dissection. Stroke 1986;17:921-923
14. Bostrom K, Liliequist B: Primary dissecting aneurysm of theextracranial part of the internal carotid and vertebral arteries. Areport of three cases. Neurology 1967; 17:179-186
15. Ringel SP, Harrison SH, Norenberg MD, Austin JH: Fibro-muscular dysplasia: Multiple "spontaneous" dissecting aneu-rysms of the major cervical arteries. Ann Neurol 1977; 1:301-304
16. Kanshepolsky J, Danielson H, Flynn RE: Vertebral artery in-sufficiency and cerebellar infarct due to manipulation of theneck. Bull Los Angeles Neurol Soc 1972;37:62-66
17. Nagler W: Vertebral artery obstruction by hyperextension ofthe neck. Report of three cases. Arch Phys Med Rehabil1973;54:232-240
18. Mehalic T, Farhat SM: Vertebral artery injury from chiroprac-tic manipulation of the neck. Surg Neurol 1974;2:125-129
19. Bladin PF, Memory J: Mechanisms in cerebral lesions in trau-ma to high cervical portion of the vertebral artery-rotationinjury. Proc Aust Assoc Neurol 1975;12:35—41
20. Davidson KC, Weiford EC, Dixon GD: Traumatic vertebralartery pseudoaneurysm following chiropractic manipulation.Radiology 1975;115:651-652
21. Mueller S, Sahs AL: Brainstem dysfunction related to cervicalmanipulation. Neurology 1976;26:547-550
22. Mokri B, Houser OW, Sundt TM: Idiopathic regressing arte-riopathy. Ann Neurol 1977;2:466-^72
23. Fisher CM, Ojemann RG, Roberson GH: Spontaneous dissec-tion of cervico-cerebral arteries. Can]NeurolSci 1978;5:9-19
24. Krueger BR, Okazaki H: Vertebral-basilar distribution infarc-tion following chiropractic cervical manipulation. Mayo ClinProc 1980;55:322-332
25. Schellhas KP, Latchaw RE, Wendling LR, Gold LHA: Verte-brobasilar injuries following cervical manipulation. JAMA1980;244:1450-1453
26. Bradac GB, Kaembach A, Bolk-Weischedel D, Finck GA:Spontaneous dissecting aneurysm of cervical cerebral arteries.Neuroradiology 1981;21:149-154
27. Sherman DG, Hart RG, Easton JD: Abrupt change in headposition and cerebral infarction. Stroke 1981 ;12:2—6
28. Dragon R, Saranchak H, Lakin P, Strauch G: Blunt injuries ofthe carotid and vertebral arteries. Am J Surg 1981; 141:497-50O
29. Alpert JN, Gerson LP, Hall RJ, Hallman GL: Reversible an-giopathy. Stroke 1982;13:100-105
by guest on July 9, 2018http://stroke.ahajournals.org/
Dow
nloaded from

Mas et al Extracranial Vertebral Artery Dissections 1047
30. Goldstein SJ: Dissecting hematoma of the cervical vertebralartery. Case report. J Neurosurg 1982;56:451-454
31. Nichelli P, Gibertoni M, Guerzoni C: Delayed cerebellar in-farction following a car accident. Stroke 1983;14:617-619
32. Cellerier P, Georget AM: Dissection des arteres vertebralesapres manipulation du rachis cervical. A propos d'un cas. JRadiol 1984;65:191-196
33. Katirji MB, Reinmuth OM, Latchaw RE: Stroke due to verte-bral artery injury. Arch Neurol 1985;42:242-248
34. Tramo MJ, Hainline B, Petito F, Lee B, Caronna J: Vertebralartery injury and cerebellar stroke while swimming: Case re-port. Stroke 1985;16:1039-1042
35. Hilton-Jones D, Warlow CP: Non-penetrating arterial traumaand cerebral infarction in the young. Lancet 1985; 1:1435-1438
36. Roualdes G, Lartigue C, Boudigue MD, Van der Marcq P,Dravineau J, Desplat A, Bataille B: Dissection de l'artere ver-t£brale dans sa portion extracranienne apres un match de ten-nis. Press Med 1985;14:2108
37. Wiebers DO, Mokri B: Internal carotid artery dissection afterchildbirth. Stroke 1985; 16:956-959
38. Millikan CH, Bauer RB, Goldschmidt J, Goldstein M, Hey-man A, Meyer JS, Moossy J, Mount L, Siekert RG, StallonesR, Toole JF, Reinmuth OM, Scheinberg P: Classification andOutline of Cerebrovascular Disease II. Stroke 1975;6:566-616
KEY WORDS • dissection • extracranial vertebral artery
by guest on July 9, 2018http://stroke.ahajournals.org/
Dow
nloaded from

J L Mas, M G Bousser, D Hasboun and D LaplaneExtracranial vertebral artery dissections: a review of 13 cases.
Print ISSN: 0039-2499. Online ISSN: 1524-4628 Copyright © 1987 American Heart Association, Inc. All rights reserved.
is published by the American Heart Association, 7272 Greenville Avenue, Dallas, TX 75231Stroke doi: 10.1161/01.STR.18.6.1037
1987;18:1037-1047Stroke.
http://stroke.ahajournals.org/content/18/6/1037World Wide Web at:
The online version of this article, along with updated information and services, is located on the
http://stroke.ahajournals.org//subscriptions/
is online at: Stroke Information about subscribing to Subscriptions:
http://www.lww.com/reprints Information about reprints can be found online at: Reprints:
document. Permissions and Rights Question and Answer available in the
Permissions in the middle column of the Web page under Services. Further information about this process isOnce the online version of the published article for which permission is being requested is located, click Request
can be obtained via RightsLink, a service of the Copyright Clearance Center, not the Editorial Office.Stroke Requests for permissions to reproduce figures, tables, or portions of articles originally published inPermissions:
by guest on July 9, 2018http://stroke.ahajournals.org/
Dow
nloaded from