Essentials of Our Current Understanding: Abdominal Wall Blocks · 2017. 4. 10. · Posterior...
Transcript of Essentials of Our Current Understanding: Abdominal Wall Blocks · 2017. 4. 10. · Posterior...
-
REGIONAL ANESTHESIA AND ACUTE PAIN
SPECIAL ARTICLE
Essentials of Our Current Understanding:Abdominal Wall Blocks
Ki Jinn Chin, FRCPC,* John G. McDonnell, MD, FCARCSI,† Brendan Carvalho, MD,‡ Aidan Sharkey, FCAI,†Amit Pawa, FRCA,§ and Jeffrey Gadsden, MD, FRCPC, FANZCA||
Abstract: Abdominal wall blocks rely on the spread of local anestheticwithin musculofascial planes to anesthetize multiple small nerves or plex-uses, rather than targeting specific nerve structures. Ultrasonography is pri-marily responsible for the widespread adoption of techniques includingtransversus abdominis plane and rectus sheath blocks, as well as the intro-duction of novel techniques such as quadratus lumborum and transversalisfascia blocks. These blocks are technically straightforward and relativelysafe and reduce pain and opioid requirements in many clinical settings.The data supporting these outcomes, however, can be inconsistent becauseof heterogeneity of study design. The extent of sensory blockade is alsosomewhat variable, because it depends on the achieved spread of local an-esthetic and the anatomical course of the nerves being targeted. The blocksmainly provide somatic analgesia and are best used as part of a multimodalanalgesic regimen. This review summarizes the anatomical, sonographic,and technical aspects of the abdominal wall blocks in current use, examin-ing the current evidence for the efficacy and safety of each.
(Reg Anesth Pain Med 2017;42: 133–183)
Regional anesthesia of the trunk and abdominal wall has tradi-tionally centered on epidural analgesia, but enthusiasm forthis has waned with the increasing use of minimally invasive lap-aroscopic techniques, aggressive postoperative anticoagulationregimens, and emphasis on early ambulation. The popularity ofabdominal wall blocks, on the other hand, has dramatically in-creased in the last decade, thanks to the introduction of simpleyet effective techniques such as the transversus abdominis plane(TAP) block and the widespread availability of ultrasound (US)imaging. There has been an accompanying explosion in the scien-tific literature on abdominal wall blocks, and the purpose of thisreview is to summarize the current state of knowledge, with theaim of providing a guide to clinical application of these tech-niques, as well as future avenues of research. Toward these ends,the review describes the applied anatomy of the abdominal wall,as well as the sonoanatomy and basic technical considerationsof the blocks in current use. These include the TAP block,ilioinguinal-iliohypogastric (II-IH) block, rectus sheath block,and the newer techniques of transversalis fascia plane (TFP) blockand quadratus lumborum (QL) block. The evidence for clinical
From the *Department of Anesthesia, Toronto Western Hospital, University ofToronto, Toronto, Ontario, Canada; †Department of Anaesthesia, Clinical Sci-ences Institute, National University of Ireland, Galway, Ireland; ‡Departmentof Anesthesiology, Perioperative and Pain Medicine, Stanford UniversitySchool of Medicine, Stanford, CA; §Department of Anaesthesia, Guy's andSt Thomas' Hospitals, London, United Kingdom; and ||Department of Anesthe-siology, Duke University Medical Center, Durham, NC.Accepted for publication October 12, 2016.Address correspondence to: Ki Jinn Chin, FRCPC, Department of Anesthesia,
TorontoWestern Hospital, University of Toronto, McL 2-405, 399 BathurstSt, Toronto, Ontario, Canada M5T 2S8 (e‐mail: [email protected]).
The authors declare no conflict of interest.Copyright © 2017 by American Society of Regional Anesthesia and Pain
MedicineISSN: 1098-7339DOI: 10.1097/AAP.0000000000000545
Regional Anesthesia and Pain Medicine • Volume 42, Number 2, March
Copyright © 2017 American Society of Regional Anesthesia and Pain
outcomes of efficacy and safety associated with the various blocktechniques is discussed, including the specific application of ab-dominal wall blocks in the obstetric population.
ANATOMY OF THE ABDOMINAL WALLThe abdominal wall is a continuous cylindrical myofascial
structure that attaches to the thoracic cage superiorly, the pelvicgirdle inferiorly, and the spinal column posteriorly. The anatomi-cal relationship between the muscles and fascial layers of the ab-dominal wall is complex, and it is useful from both a conceptualand practical standpoint to consider the anterolateral and posteriorsections of the abdominal wall separately.
Anterolateral Abdominal WallThe anterolateral abdominal wall extends between the poste-
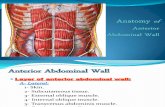
rior axillary lines on either side (Fig. 1). The superior boundariesare the costal margin of the 7th to 10th ribs and xiphoid processof the sternum, and the inferior boundaries are the iliac crests, in-guinal ligament, pubic crest, and symphysis. The layers of the ab-dominal wall are (from superficial to deep) skin and subcutaneoustissue, the abdominal muscles and associated aponeuroses,transversalis fascia, extraperitoneal fat, and parietal peritoneum.
The anterolateral abdominal wall has 3 flat muscles (externaloblique, internal oblique, transversus abdominis) arranged in con-centric layers and 1 paired vertical muscle in the midline (rectusabdominis). A small number of individuals have a second smallvertical midline muscle, the pyramidalis, which is of little clinicalsignificance. All 3 flat muscles taper off into aponeuroses as theyapproach the midline, and these aponeuroses form the tendinousrectus sheath that encases the rectus abdominis muscle (RAM).They blend in the midline with the aponeuroses of the other sideto form the linea alba. The specifics of how the muscles and theiraponeuroses relate to each other, as well as the various points ofreference on the abdominal wall (eg, midaxillary line, anterior ax-illary line, midclavicular line), will determine the layers visible onUS at different transducer locations.
The external oblique muscle (EOM) originates on the exter-nal aspect of the 5th to 12th ribs, and its fibers descend in aninferomedial direction to insert on the anterior iliac crest, lineaalba, and pubic tubercle (Fig. 1). Anteriorly, the EOM tapers offinto an extensive aponeurosis medial to the midclavicular lineand inferior to a line between the anterior superior iliac spine(ASIS) and the umbilicus; thus, in this area, only 2 muscle layers,internal oblique muscle (IOM) and transversus abdominis muscle(TAM), will be apparent onUS imaging (Fig. 2). The inferior edgeof the EOM aponeurosis forms the inguinal ligament; its medialedge blends with the aponeurosis of IOM to form the anteriorrectus sheath.
The IOM originates from the iliac crest inferiorly and thethoracolumbar fascia posteriorly, and its fibers ascend in asuperior-medial direction (perpendicular to those of the EOM)to insert on the inferior borders of the 10th to 12th ribs and thelinea alba. It is a fleshy muscle that on US imaging often appears
-April 2017 133
Medicine. Unauthorized reproduction of this article is prohibited.
mailto:[email protected]
-
FIGURE 1. Surface anatomy, muscular layers, and nerves of the anterolateral abdominal wall. The EOM and IOM and aponeuroses havebeen cut away on the right to show the TAP. The lateral cutaneous branches arise from their respective spinal nerves at or posterior to themidaxillary line and supply the skin of the lateral abdominal wall up to themidclavicular line. The T7-T9 nerves enter the TAP at ormedial to themidclavicular line. Communicating branches between the spinal nerves give rise to plexuses of nerves within the TAP and the rectus sheath.The rectus sheath is deficient midway between the umbilicus and pubis. AAL indicates anterior axillary line; MAL, midaxillary line; MCL,midclavicular line; PAL, posterior axillary line).
Chin et al Regional Anesthesia and Pain Medicine • Volume 42, Number 2, March-April 2017
as the thickest of the 3 flat muscle layers (Fig. 3). Medial to themidclavicular line, the IOM tapers off into its aponeurosis andcontributes to the formation of the rectus sheath.
The TAM originates on the internal aspect of the 7th to 12thcostal cartilages, the thoracolumbar fascia, and iliac crest. As itsname indicates, the fibers run transversely to insert on the lineaalba and pubic tubercle. Like the EOM and IOM, it tapers off me-dially into an aponeurosis that blends with the others to form therectus sheath (Fig. 1). The transition frommuscle into aponeurosisoccurs along a crescent-shaped line, and thus just inferior to thecostal margin, TAM runs deep to rectus abdominis for a short dis-tance before tapering off into its aponeurosis (Fig. 4).
The RAM is a paired muscle that originates on the pubiccrest and symphysis and ascends vertically to insert on the xiphoidprocess and fifth to seventh costal cartilages (Fig. 1). It is encasedwithin the rectus sheath and is attached to the anterior aspect ofthe rectus sheath by 3 or 4 transverse tendinous insertions. Theseinsertions divide the anterior rectus sheath compartment into sep-arate subcompartments, giving the RAM its “6-pack” appearancein thin muscular subjects and consequently impeding cranio-caudal spread of injectate. The posterior rectus sheath compart-ment, by comparison, is unsegmented and is thus a more logicalplace for local anesthetic injection.
The rectus sheath is formed by the blending of aponeurosesfrom the EOM, IOM, and TAM. In the superior three-quartersof the RAM, the anterior layer of the rectus sheath is formed bythe EOM and IOM aponeuroses. The IOM aponeurosis splits into
134
Copyright © 2017 American Society of Regional Anesthesia and Pain
2 layers and also contributes to the posterior layer of the rectussheath together with the TAM aponeurosis (Fig. 5A). However, in-ferior to the level of the ASIS (at the arcuate line), all 3 aponeuro-ses pass anterior to the RAM and form the anterior layer of therectus sheath. The inferior one-quarter of the RAM is thereforelined on its posterior aspect only by its epimysium and thetransversalis fascia (Figs. 1 and 5B).
Posterior Abdominal WallUnderstanding the structure of the posterior abdominal wall
is essential to the landmark-guided TAP block and the more novelUS-guided abdominal wall blocks, such as the TFP block andQL block.
Of the 3 muscle layers of the anterolateral abdominal wall,the TAM and IOM taper off posteriorly into their origins fromthe thoracolumbar fascia. The EOM, on the other hand, ends pos-teriorly in a free edge, which abuts against the latissimus dorsimuscle (Fig. 6).
The thoracolumbar fascia is a complex tubular structure ofblended aponeuroses and fascial layers that encases the deep mus-cles of the back and, as its name suggests, extends from the lumbarto thoracic spine.1,2 Tracing it laterally from its anchor point on thespinous processes and supraspinous ligament, the thoracolumbarfascia splits into 3 layers: the posterior and middle layers enclosethe paraspinal (erector spinae) muscles, and the middle and ante-rior layers enclose the QLmuscle (QLM), which is a quadrilateral
© 2017 American Society of Regional Anesthesia and Pain Medicine
Medicine. Unauthorized reproduction of this article is prohibited.
-
FIGURE 2. Anatomy of the US-guided II-N and IH-N block. The IH-N and II-N emerge from the lateral border of psoas major and run over theanterior surface of QL, then the deep aspect of TAMand its aponeurosis. Both nerves pierce TAM to enter TAP at a variable location posteriorto the ASIS. The US probe may be placed in 1 of 2 locations (blue lines). (1) The recommended approach is to place the probe parallel andsuperior/posterior to the line connecting the umbilicus and the ASIS. The edge of the probe rests against the iliac crest (IC), which is visible asan acoustic shadow. In this position, the 3muscular layers of the abdominal wall are visible. The II-N and IH-N are located in the TAP betweenIOM and TAM and lie very close to the iliac crest. The AB-DCIA lies more medially in the TAP, as does the subcostal nerve (T12). Injection oflocal anesthetic is performed in the TAP close to the IC (circle), avoiding the nerves if they are visible. (2) If the probe is placed inferior to the lineconnecting the umbilicus and the ASIS, only the IOM and TAM are visible as muscle layers. The EOM has tapered off into its aponeurosis(EOA). The ilioinguinal and iliohypogastric nerves in this area are ascending through IOM into more superficial and subcutaneous planes andare not easily visualized or consistent in their location. AB-DCIA indicates ascending branch of deep circumflex iliac artery; IC, iliac crest; IH-N,iliohypogastric nerve; II-N, ilioinguinal nerve.
Regional Anesthesia and Pain Medicine • Volume 42, Number 2, March-April 2017 RA of the Abdominal Wall
muscle extending between the 12th rib and the (internal lip of the)iliac crest (Figs. 2 and 6). Medial and anterior to the QLM lies thepsoas major muscle. The posterior and middle layers of thora-columbar fascia fuse again lateral to the paraspinal muscles andmerge with the aponeuroses of the IOM and TAM.1,2
The transversalis fascia is a thin areolar tissue that lines thedeep surface of TAM and separates it from the parietal perito-neum. It is 1 part of the larger endoabdominal fascia that linesthe entire internal aspect of the abdominal wall. As such, it is con-tinuous inferiorly with the fascia iliaca3 and medially with theinvesting fascia of QLM and psoas major muscle (Fig. 6). In fact,the terms “anterior layer of thoracolumbar fascia” and “transversalisfascia” may be used interchangeably when referring to the fasciallayer investing the anterior surface of QLM.1 The transversalisfascia follows the QLM and psoas major superiorly through thediaphragm, passing under the lateral and medial arcuate ligamentsand blending with the endothoracic fascia of the thorax.4,5 Theserelationships of the thoracolumbar fascia, transversalis fascia andassociated muscles have important implications for the potentialspread of local anesthetic injected in the posterior abdominal wall.
The triangle of Petit (or inferior lumbar triangle) is the pri-mary surface anatomical landmark for the TAP block. It is bor-dered inferiorly at its base by the iliac crest, laterally by themedial free edge of EOM and medially by the lateral edge oflatissimus dorsi (Fig. 7). The triangle is covered superficially byskin and subcutaneous tissues, whereas its anterior (deep) flooris formed by IOM and the thoracolumbar fascia, which separates
© 2017 American Society of Regional Anesthesia and Pain Medicine
Copyright © 2017 American Society of Regional Anesthesia and Pain
it from the fat-filled retroperitoneal space. However, cadavericstudies indicate that there is significant anatomic variability inthe triangle of Petit.7,8 It was quite small in the majority of subjects(3.6 cm2 on average7) and even absent in 18% of subjects becauseof overlapping of the free edges of EOM and latissimus dorsi.8
This inconsistency limits its usefulness as a reliable surfaceanatomical landmark.
Innervation of the Anterior Abdominal WallThe anterior abdominal wall is innervated by the thora-
coabdominal nerves and the ilioinguinal and iliohypogastricnerves (Fig. 1). The thoracoabdominal nerves originate from theanterior rami of the lower 7 thoracic spinal nerves (T6-T12) andare the continuation of the respective intercostal nerves. The T12nerve is often also referred to as the subcostal nerve. They eachgive off a lateral cutaneous branch in the midaxillary line, whichascends to enter the subcutaneous tissues along the anterior axil-lary line and supplies the lateral abdominal wall. The anteriorbranches of the thoracoabdominal nerves subsequently emergefrom the costal margin and travel in the neurovascular TAP be-tween IOM and TAM. Note that the upper segmental nerves T6-T9 only enter the TAP medial to the anterior axillary line (T6 en-ters it just lateral to the linea alba) and that the other nerves enterit progressively more laterally (Fig. 1).9 This has implications forthe pattern of nerve involvement that can be expected by injectionat different locations in the TAP. Within the TAP, the lower seg-mental nerves (T9-L1) give off multiple communicating branches
135
Medicine. Unauthorized reproduction of this article is prohibited.
-
FIGURE 3. Anatomy of the anterolateral abdominal wall and the US-guided (USG) subcostal and lateral TAP blocks. The USG subcostalTAP block targets the T6 to T10 nerves, where they emerge into the TAP from under the costal margin. The probe is placed parallel andadjacent to the costal margin (blue line). Closer to the midline, the TAP is the plane between RAM and TAM. The EOM and IOM exist asaponeuroses in this region, which contribute to the formation of the anterior rectus sheath. The EOM and IOM become visible as the probeis moved more laterally along the costal margin. Injection may be performed at multiple points along the costal margin (circles) or a needleinserted in-plane in a continuous track along the costal margin (the oblique subcostal TAP block approach). Note that the lateral cutaneousbranches of the thoracoabdominal nerves are not covered by the block. The USG lateral TAP block targets the T10 to T12-L1 nerves. The probeis placed in a transverse orientation between the costal margin and iliac crest and in the midaxillary line. Injection is performed in the TAPbetween IOM and TAM (circle), with the needle usually inserted in an anterior-to-posterior direction. The TAM has a characteristic darkerhypoechoic appearance and is usually significantly thinner than the IOM.
Chin et al Regional Anesthesia and Pain Medicine • Volume 42, Number 2, March-April 2017
to form a longitudinal TAP plexus, from which the terminal ante-rior branches arise.9
The terminal anterior cutaneous branches of the thoraco-abdominal nerves enter the rectus sheath at its lateral margin(the linea semilunaris). In the vast majority of cases (89%), thenerves run deep to the posterior surface of RAM before ascendingto pierce it 1.6 to 2.6 cm from its lateral edge.10 However, thesenerves occasionally directly pierce the lateral edge of the RAMand thus may be missed by a rectus sheath block. Once again,the nerves branch and communicate to form a longitudinal rectussheath plexus, before entering the subcutaneous tissue of the ante-rior abdominal wall.9
The existence of TAP and rectus sheath plexuses indicatesthat individual terminal nerves have multiple segmental originsand that the traditional depiction of the cutaneous innervation ofthe abdominal wall in terms of well-demarcated dermatomes isnot wholly accurate.11 This may be an explanation for the discrep-ancies between radiographically visualized spread of injectate inthe TAP, apparent extent of clinical analgesia, and the cutaneoussensory block observed in studies.6,12,13
The ilioinguinal and iliohypogastric nerves are classically de-scribed as terminal branches of the anterior ramus of the L1 spinalnervewith occasional contribution fromT12. Although this is truein the majority of individuals, there is significant variability, withup to 20% having origins from the L2 and L3 nerve roots.14–16
Both nerves emerge at the lateral border of psoas major and runinferolaterally on the ventral surface of QLM and TAM, just
136
Copyright © 2017 American Society of Regional Anesthesia and Pain
superior and parallel to the iliac crest (Fig. 2). The exact locationat which the nerves pierce TAM and enter the TAP is variable,but this is usually in the region of the anterior third of the iliac crestrather than more posteriorly.14,17,18 The iliohypogastric nerve en-ters the TAP earlier in its course than the ilioinguinal nerve, andin a significant number of individuals, the ilioinguinal nerve onlyenters the TAP very close to the ASIS (medial to the anterior ax-illary line).9 Both nerves continue to ascend through the IOMand EOM to supply the abdominal wall in the inguinal and pubicregions. They pierce the IOM at a variable distance medial to theASIS (approximately 3 ± 2 cm medial to ASIS and 1 cm superiorto inguinal ligament in adults.14 The anatomic variability in theircourse contributes to the high failure rates for blockade of thesenerves with the TAP block19,20 and the landmark-guided tech-niques of II-IH block.21,22
Vasculature of the Anterior Abdominal WallThere is a rich network of arteries and veins within the TAP,
which supplies the anterior abdominal wall and promotes the ab-sorption of local anesthetic injected in this plane. The main arter-ies are continuations of the lower thoracic intercostal arteries andthe deep circumflex iliac arteries. Within the rectus sheath, bilat-eral superior epigastric arteries (continuations of the internalthoracic arteries) anastomose with the deep inferior epigastricarteries (which arise from the external iliac arteries) and are atrisk of accidental puncture during rectus sheath block.
© 2017 American Society of Regional Anesthesia and Pain Medicine
Medicine. Unauthorized reproduction of this article is prohibited.
-
FIGURE 4. Anatomy of the anterolateral abdominal wall and the US-guided (USG) rectus sheath block. This block targets the terminalmuscular branches and anterior cutaneous branches of the thoracoabdominal nerves. The probe is placed in a transverse orientationsuperior to the umbilicus to visualize the lateral aspect of the RAM and rectus sheath. Close to the costal margin, the TAM is often visible lyingdeep to RAM. If the probe is placed inferior to the midpoint between umbilicus and pubic symphysis, the posterior rectus sheath is absent,and the deep surface of RAM is bounded by its epimysium and transversalis fascia. Injection is performed in the posterior rectus sheathcompartment between the lateral aspect of RAM and its deep investing layer of fascia (circles), to target the nerves before they ascendthrough RAM into their subcutaneous location.
Regional Anesthesia and Pain Medicine • Volume 42, Number 2, March-April 2017 RA of the Abdominal Wall
TAP BLOCKThe landmark-guided TAP blockwas first described in 200123
and has since undergone multiple modifications. The “TAP block”is therefore a nonspecific term encompassing a heterogeneous groupof approaches that share the common end point of local anestheticinjection into the neurovascular fascial plane superficial to theTAM. The aim in all cases is to block some or all of the lower 6 tho-racic spinal nerves (T7-T12) and the iliohypogastric and ilioinguinalnerves (L1). The approaches differ primarily in the site of needle in-sertion and injection, which, because of the complex course of thelower thoracoabdominal nerves and interplay between muscularand aponeurotic layers of the abdominal wall at different locations,leads in turn to differences in the spread of local anesthetic and extentof analgesia. There has been a lack of consistency in the terminologyused to describe the different US-guided approaches24–26 and this re-view uses the nomenclature outlined in Table 1.
Landmark-Guided TAP Block
TechniqueThe landmark-guidedTAPblockwas first described byRafi23,44
and later byMcDonnell et al.6 Both authors describe the chief sur-face landmark as the insertion of the latissimus dorsi on the iliaccrest. The site of needle insertion is immediately anterior to this“latissimoiliac point (LIP)”44 and just superior to the iliac crest,in the triangle of Petit (Fig. 7). Given the variability in the sizeand presence of the triangle of Petit,7,8 the LIP may be a more ac-curate and consistent landmark.
McDonnell et al6 recommend seeking a “double-pop” as theend point for needle insertion, the first pop representing penetrationof the EOM fascia and the second pop the deep fascia of IOM.
© 2017 American Society of Regional Anesthesia and Pain Medicine
Copyright © 2017 American Society of Regional Anesthesia and Pain
Rafi,44 on the other hand, recommends contacting the externallip of the iliac crest and “walking” the needle tip over it until a sin-gle pop (penetration of the deep fascia of IOM) is obtained. Re-gardless, the subjective nature of tactile pops as end points forneedle insertion may contribute to failure of the technique, partic-ularly in inexperienced hands.45
Pattern of injectate spread and sensory blockRadiological studies indicate that 20 to 40 mL of local anes-
thetic injected using the landmark-guided TAP approach willspread within the TAP from the iliac crest superiorly to the costalmargin, anteriorly to the midaxillary line, and posteriorly to thelateral border of QLM.6,46 This TAP spread was thought to be re-sponsible for block efficacy (hence the name) and has been theprinciple upon which subsequent modifications have been based.However, posterior extension of injectate spread into the planebetween transversalis fascia and the ventral surface of QLM,and thence upward into the thoracic paravertebral space, hasalso been reported.46 It is postulated that this may be the moreimportant mechanism for producing analgesia, particularly abovethe T10 level, because the T7-T9 nerves only enter the TAPmedial tothe anterior axillary line and close to the costal margin. This patternof posterior and cranial spread is not seen with any of the US-guidedTAP approaches, and they may therefore have little in common withthe landmark-guided TAP block apart from the name.
The extent of cutaneous sensory block that can be achieved isless clear. McDonnell et al6 reported achieving a sensory block ofthe anterior abdominal wall from T7 to L1 in 6 volunteers (12blocks), but the precise sites of sensory testing were not described.Carney et al46 mapped the extent of sensory loss in 8 blocks andfound this was variable; in particular, blockade of the anterior
137
Medicine. Unauthorized reproduction of this article is prohibited.
-
FIGURE5. A, Sonoanatomy of the RAM and sheath in the supraumbilical region, with a corresponding schematic diagram showing the fascialand aponeurotic layers. The TAM is visible deep to the lateral edge of the RAM. Both the internal oblique aponeurosis and the transversusabdominis aponeurosis contribute to the posterior rectus sheath. The transversalis fascia and peritoneum lie deep to the posterior rectus sheathbut cannot always be clearly distinguished as separate layers. B, Sonoanatomy of the RAM and sheath in the infraumbilical region below thearcuate line, with a corresponding schematic diagram showing the fascial and aponeurotic layers. Here, there is no posterior rectus sheath.The layer immediately deep to the perimysium of RAM is transversalis fascia. The aponeuroses of all 3 muscle layers contribute only to theanterior rectus sheath. EOA indicates external oblique aponeurosis; IOA, internal oblique aponeurosis; P, peritoneum; SC, subcutaneous tissue;TAA, transversus abdominis aponeurosis; TF, transversalis fascia.
Chin et al Regional Anesthesia and Pain Medicine • Volume 42, Number 2, March-April 2017
138 © 2017 American Society of Regional Anesthesia and Pain Medicine
Copyright © 2017 American Society of Regional Anesthesia and Pain Medicine. Unauthorized reproduction of this article is prohibited.
-
FIGURE 6. Anatomy of the posterior abdominal wall and the US-guided QL block. The EOM ends in a free edge abutting the latissimusdorsi. The IOM and TAM end in aponeuroses that blend with the thoracolumbar fascia. The thoracolumbar fascia itself splits into 3 layers(posterior, middle, and anterior) that envelop the QLM and ESM. The QL block is performed by placing a curvilinear probe on theposterolateral aspect of the abdominal wall in a transverse oblique orientation, between the iliac crest and costal margin (blue line).Key landmarks for identifying the QLM are the VB, TP, and PMM. At the L3-L4 level, the large intestine in the peritoneal cavity may be seendeep to the abdominal wall muscles (as it is here); at the L2-L3 level, the kidney is usually visible in the retroperitoneal space. The circlesindicate points for local anesthetic injection either anterior or posterior to QLM. ESM indicates erector spinae muscle; PMM, psoas majormuscle; TP, transverse process; VB, vertebral body.
FIGURE 7. Line drawing of the surface anatomy of the abdominal wall, including the lumbar triangle of Petit (arrows). As can be seen fromthe diagram, the triangle is bounded posteriorly by the latissimus dorsi muscle and anteriorly by the external oblique with the iliac crestforming the base of the triangle. The floor of the triangle is formed by the IOM. Reproduced with permission from McDonnell et al.6
Regional Anesthesia and Pain Medicine • Volume 42, Number 2, March-April 2017 RA of the Abdominal Wall
© 2017 American Society of Regional Anesthesia and Pain Medicine 139
Copyright © 2017 American Society of Regional Anesthesia and Pain Medicine. Unauthorized reproduction of this article is prohibited.
-
TABLE
1.Ultrasou
nd-G
uide
dAb
dominalWallB
locks
Block
Techn
ique
Clin
ical
Indication
Com
ments
SubcostalT
APblock2
7,28
Probepositio
n:placed
lateraltoxiphoidprocess;
paralleltocostalmargin.Injectionsite:(1)
Medialtolin
easemilu
naris:deep
toRAM
and
superficialtoTA
Mwhere
TAM
tapersoff
medially
into
itsfascialcontributionto
the
posteriorrectus
sheath.(2)
Lateralto
linea
semilu
naris:deep
toIO
Mandsuperficial
toTA
M.L
Adosing:0
.2–0.3mL/kgperblock,
concentrationadjusted
tokeep
with
inmax
recommendeddose
range(inmg).
Somaticanalgesiaforincisionsin
upper
(T6-T7to
T9-T10)anterior
abdominalwall.
Will
notcover
incisionslateraltoanterior
axillarylin
e.
Oblique
subcostalT
APblock2
9,30
Probepositio
n:Midclavicular
lineto
anterior
axillarylin
e;paralleltocostalmargin.
Injectionsite:E
xtensive
injectiontrackin
TAP,
deep
toIO
MandsuperficialtoTA
M,along
theentirecostalmargin.LAdosing:
0.2–0.3mL/kgperblock,concentration
adjusted
tokeep
with
inmax
recommended
dose
range(inmg).
Somaticanalgesiaforincisionsin
upper
(T6-T7to
T9-T10)anterior
abdominalwall.
Technically
challengingneedleinsertion.
Will
notcover
incisionslateraltoanterior
axillarylin
e.
Lateral(m
idaxillary)
TAPblock3
1,32
Probepositio
n:Midaxillarylin
e;paralleland
superior
toiliac
crest.Injectionsite:D
eepto
IOM
andsuperficialtoTA
M,inmidaxillarylin
e.LAdosing:0
.2–0.3mL/kgperblock,
concentrationadjusted
tokeep
with
inmax
recommendeddose
range(inmg).
Somaticanalgesiaforincisionsin
lower
(T10
toT12-L1)
anterior
abdominalwall.
Will
notcover
incisionslateraltoanterior
axillarylin
e.L1isnotconsistently
covered.
Bilaterald
ual-TA
Pblock1
2,28,33
Com
binatio
nof
bilateralsubcostalandlateral
TAPblocks.L
Adosing:0
.15–0.2mL/kgper
block,concentrationadjusted
tokeep
with
inmax
recommendeddose
range(inmg).
Somaticanalgesiaforextensive(T7-T12)
incisionsin
anterior
abdominalwall.
Will
notcover
incisionslateraltoanterior
axillarylin
e.
II-IHnerveblock3
4,35
Probepositio
n:Posteriorandsuperior
toASIS,
paralleltothelin
ebetweenASISandum
bilicus.
Injectionsite:M
edialtoacousticshadow
ofASISwith
intheTA
P.LAdosing:0
.1–0.15mL/kg,
concentrationadjusted
tokeep
with
inmax
recommendeddose
range(inmg).
Somaticanalgesiaforincisionsin
theright
orleftiliac
fossaof
theabdomen.
Visualizationof
nerves
isnotalwayspossible
ornecessary.
Rectussheath
block3
6,37
Probepositio
n:Transverseorientationlateralto
linea
alba
andjustsuperior
toum
bilicus.
Injectionsite:M
edialtoacousticshadow
ofASISwith
intheTA
P.LAdosing:0
.1–0.2
mL/kg
perside,concentratio
nadjusted
tokeep
with
inmax
recommendeddose
range(inmg).
Somaticanalgesiaformidlin
eincisionsin
anterior
abdominalwall.
Bilateralinjectio
nsrequired.D
ivided
injections
superior
andinferior
toum
bilicus
may
provide
forbetterspread.
AnteriorQLblock3
8–41
Probepositio
n:Posterioraxillarylin
e,parallel
toiliac
crest.Injectionsite:A
nterior(deep)
toQLM.L
Adosing:0
.2–0.3mL/kgperblock,
concentrationadjusted
tokeep
with
inmax
recommendeddose
range(inmg).
Analgesiaformidlower
(T8-T12)incisionsin
anterior
abdominalwall.
Needlemay
beinserted
inlateral-to-m
edial
direction3
8,39or
posterior-to-anterior
(transmuscularapproach
40,41 ).L
umbarplexus
blockmay
occurwith
theposterior-to-anterior
(transmuscular)approach.
Chin et al Regional Anesthesia and Pain Medicine • Volume 42, Number 2, March-April 2017
140 © 2017 American Society of Regional Anesthesia and Pain Medicine
Copyright © 2017 American Society of Regional Anesthesia and Pain Medicine. Unauthorized reproduction of this article is prohibited.
-
PosteriorQLblock3
8Probepositio
n:Posterioraxillarylin
e,parallel
toiliac
crest.Injectionsite:P
osterior
(superficial)
toQLM.L
Adosing:0
.2–0.3mL/kgperblock,
concentrationadjusted
tokeep
with
inmax
recommendeddose
range(inmg).
Analgesiaformidlower
(T8-T12)incisionsin
anterior
abdominalwall.
Lum
barplexus
blockmay
occur.
TFP
block4
2,43
Probepositio
n:Posterioraxillarylin
e,parallel
toandagainstiliaccrest,andangled
slightly
inferiorly.Injectio
nsite:D
eepto
taperedtip
ofTA
Mandsuperficialtotransversalis
fascia.
LAdosing:0
.2–0.3mL/kgperblock,
concentrationadjusted
tokeep
with
inmax
recommendeddose
range(inmg).
Analgesiaforincisionsover
theanterior
iliac
crest,theanterior
iliac
crestitself,andL1
derm
atom
eof
theanterior
abdominalwall.
Siteof
LAdepositio
nismoreinferior
and
anterior/lateraltothatof
theQLblock.
Lum
barplexus
blockmay
occur.
LAindicateslocalanesthetic;U
SG,U
S-guided.
Regional Anesthesia and Pain Medicine • Volume 42, Number 2, March-April 2017 RA of the Abdominal Wall
© 2017 American Society of Regional Anesthesia and Pain Medicine
Copyright © 2017 American Society of Regional Anesthesia and Pain
abdominal wall was patchy and incomplete. Areas that were consis-tently blocked were the area of injection, groin, and upper lateral thigh.
US-Guided Lateral TAP Block
TechniqueThe US-guided lateral TAP block was first described in
2007.31,47 Ultrasound allows direct visualization of the abdominalwall layers, needle placement, and local anesthetic spread in theTAP, and this was critical in popularizing the TAP block. Descrip-tions of the technique vary slightly in the published literature, butin general, the US transducer is placed in a transverse orientationmidway between the costal margin and iliac crest and centered onthe midaxillary line (Fig. 3).32 The needle is inserted in the ante-rior axillary line in-plane to the transducer and enters the TAP inthe midaxillary line (Figs. 3 and 8). Although initially touted asa US-guided version of the landmark-guided TAP block, it is nowclear that the US-guided lateral TAP is quite different with regardtowhere local anesthetic is injected. The point of needle entry intothe TAP is anterior and superior to the LIP and triangle of Petit,which results in a different pattern of injectate spread.
Pattern of injectate spread and sensory blockRadiological studies indicate that the US-guided lateral TAP
produces injectate spread confined to an area centered around themidaxillary line and that extends only as far as the costal margin,the iliac crest, and the anterior axillary line in most cases.46,48 Pos-terior spread beyond the midaxillary line is limited compared withthe landmark-guided TAP block.33,46 Thoracoabdominal nervesthat are consistently involved include T10, T11, T12, and, to alesser extent, L1.19,48 T9 and above are usually not involved, asthey enter only the TAP medial to the anterior axillary line.
The evidence for the extent of cutaneous sensory block isconflicting andmay depend on whether assessment involves com-prehensive area mapping or merely “point” testing using tradi-tional dermatomal maps and surface landmarks. Studies usingthe latter approach indicate that craniocaudal coverage is variable,but the results are fairly consistent with the cadaveric dye studies.In general, the US-guided lateral TAP consistently provides block-ade of the T11-T12 dermatomes and, in the majority of cases,also the T10 dermatome.12,19,49 The T9 and L1 dermatomes areblocked less than 50% of the time.19 Laterally, the block doesnot usually extend beyond the midclavicular or anterior axillaryline,12,19 and this is attributed to failure to anesthetize the lateralcutaneous branches of the segmental nerves, which arise and leavethe TAP posterior to the midaxillary line. Increasing the volumeof injectate (eg, from 15 mL to 30 mL in an adult patient) doesnot appear to significantly increase the extent of spread.12,46
On the other hand, in studies where the area of cutaneoussensory loss is systematically mapped out, this appears to behighly variable and to follow a nondermatomal distribution thatdoes not extensively involve the anterior abdominal wall.13,46
Støving et al13 observed a greater proportion of sensory loss(76% vs 24%) lateral to the line passing through the ASISrather than medial to it, suggesting that the lateral cutaneousbranches may be anesthetized after all. As in previous studies,the craniocaudal extent of sensory loss was confined to theinfraumbilical area. There was evidence of significant blockadeof the abdominal musculature, which may partly explain the dis-crepancy between the limited pattern of cutaneous sensory lossobserved in this study and clinical reports of good analgesic effi-cacy. The nondermatomal pattern may be due to the aforemen-tioned existence of a TAP plexus and overlapping contributionof multiple spinal nerves to individual terminal branches.9
141
Medicine. Unauthorized reproduction of this article is prohibited.
-
FIGURE 8. Ultrasound-guided lateral TAP block. A, Preinjection image. The US probe is placed in a transverse orientation between thecostal margin and iliac crest in the midaxillary line. A needle is advanced in an anterior-to-posterior direction through the muscular layers ofthe abdominal wall to reach the TAP between IOM and TAM. The TAM has a characteristic darker hypoechoic appearance and is usuallysignificantly thinner than the IOM. B, Postinjection image. Local anesthetic (LA) has distended the TAP, separating IOM and TAM. SCindicates subcutaneous tissue. Reproduced with permission from KJ Chin Medicine Professional Corporation.
Chin et al Regional Anesthesia and Pain Medicine • Volume 42, Number 2, March-April 2017
US-Guided Subcostal TAP Block
TechniqueThe US-guided subcostal TAP block was described in 2008
as a means of reliably providing analgesia of the supraumbilicalabdominal wall (T6-T9) and is based on the fact that these nervesenter the TAP at the costal margin and medial to the anterior axil-lary line (Fig. 3). The original description involved insertion of a100- to 150-mm needle into the TAP close to the xiphoid process,advancing it in an inferolateral direction and injecting local anes-thetic parallel to the costal margin and as far as the anterior iliaccrest.29 Alternatively, the needle may be inserted in the anterioraxillary line and in a superomedial direction toward the xiphoidprocess; this allows preoperative placement of a catheter outsidethe surgical field.33,50 This approach, subsequently termed the“oblique subcostal TAP block,”30 requires a high degree of tech-nical skill. Subsequent modifications include performing mul-tiple separate injections along the costal margin27 or performing
142
Copyright © 2017 American Society of Regional Anesthesia and Pain
a single “point” injection either medial to the linea semilunaris(between RAM and TAM)12 or lateral to it (between IOM andTAM)27,51 (Fig. 9).
Pattern of injectate spread and sensory blockCadaveric and volunteer studies support the potential to
block the upper segmental nerves (T6-T9) as they emerge intothe abdomen. However, the extent of sensory block seen withthe subcostal TAP block is variable and may depend on wherethe local anesthetic is deposited in relation towhere nerves emergefrom under the costal margin into the TAP. Injection lateral to thelinea semilunaris produces a block centered on T10-T11 and notextending higher than T9 most of the time.19,27 If T6-T8 coverageis desired, local anesthetic should be injected medial to the lineasemilunaris, between RAM and TAM, and as close to the xiphoidprocess as possible.12,27 Even then, it appears difficult to achievespread to T6 and T7 more than 50% to 70% of the time.28,33
© 2017 American Society of Regional Anesthesia and Pain Medicine
Medicine. Unauthorized reproduction of this article is prohibited.
-
FIGURE 9. Sonoanatomy of the US-guided subcostal TAP block. The probe is placed parallel and adjacent to the costal margin. Closer to themidline (upper image A), the TAP is the plane between RAM and TAM. The EOM and IOM exist as aponeuroses in this region, whichcontribute to the formation of the anterior rectus sheath. The EOM and IOM become visible as the probe is moved more laterally along thecostal margin (lower image B). The asterisks indicate suitable injection points for a US-guided subcostal TAP block. SC indicatessubcutaneous tissue. Reproduced with permission from KJ Chin Medicine Professional Corporation.
Regional Anesthesia and Pain Medicine • Volume 42, Number 2, March-April 2017 RA of the Abdominal Wall
Injection that extends to the lateral aspect of the costal marginand iliac crest can produce a block that extends inferiorly to T12and occasionally the L1 dermatome.19,27 The lateral cutaneousbranches are not blocked, and thus, incisional analgesia doesnot extend lateral to the anterior axillary line.33,52
US-Guided Bilateral Dual TAP Block
TechniqueA combination of the US-guided subcostal and lateral TAP
blocks, termed the US-guided bilateral dual -TAP block and in-volving a total of 4 injections, has been proposed as a method ofproviding analgesia to the entire anterior abdominal wall.12,28 Inthe original description, the subcostal block is performed by a“point” injection medial to the linea semilunaris, between RAMand TAM. Sondekoppam et al33 have recently proposed a modifi-cation that utilizes an extended needle track similar to the obliquesubcostal approach and is designed primarily to allow the preoper-ative insertion of catheters outside the surgical field. Needle inser-tion occurs in a lateral-to-medial direction, starting at the anterioraxillary line and traveling along the costal margin superiorly toreach the linea semilunaris. The needle is then withdrawn andinserted inferiorly toward the pubic symphysis and parallel tothe inguinal ligament to provide coverage of the lower abdomen.
Pattern of injectate spread and sensory blockIn their evaluations of the US-guided bilateral dual-TAP
block, Børglum et al12 have shown that the lateral TAP block pro-duces spread confined to the lower abdomen and a sensory blockof T10-T12, whereas the subcostal TAP block produced spread inthe upper abdominal TAP. By combining the two, they were ableto consistently obtain a cutaneous sensory block of T9-T12 with
© 2017 American Society of Regional Anesthesia and Pain Medicine
Copyright © 2017 American Society of Regional Anesthesia and Pain
extension to T7-T8 in the majority of subjects and occasionallyas high as T6.12,28
Sondekoppam et al33 evaluated their own modified tech-nique in a small cadaveric study and similarly found dye spreadinvolving T8 to L1 thoracoabdominal nerves in the majority of in-jections and spread to T7 in a small proportion. The lateral extentof dye spread was confined to an area between the anteriorand midaxillary line, leading the investigators to conclude thatthe lateral cutaneous branches are unlikely to be covered inthis approach.
Surgical TAP BlockSeveral surgical approaches to the TAP block have been de-
scribed. In laparoscopic surgery, the surgeon inserts a block nee-dle percutaneously, with entry into the TAP signaled by tactilepops and confirmed by visualization of inward bulging of theTAM as local anesthetic is injected.53 An alternative techniquehas been described in open abdominal surgery, where the woundedges are retracted and a needle inserted from the interior of theabdomen through the parietal peritoneum and into the TAP as sig-naled by a single tactile pop.54–56 Finally, a technique of surgicaldissection into the TAP, followed by direct injection or placementof a catheter, has been described in abdominoplasty57 and abdom-inal flap breast reconstruction surgery.58 Advantages cited for thesurgical approach include better matching of the site of injectionto site of surgery, ease and speed of performance, and accuracyof injection into the correct tissue plane. There are no studies ex-amining the spread of injectate with surgically placed TAP blocksor catheters, and most of the clinical data come from case seriesand retrospective case-control studies.57,59–61 Although the lattersuggest that surgical TAP blocks can reduce early postoperative
143
Medicine. Unauthorized reproduction of this article is prohibited.
-
Chin et al Regional Anesthesia and Pain Medicine • Volume 42, Number 2, March-April 2017
opioid requirements and improve pain scores, the limited random-ized controlled trial (RCT) data available at present, mostly in thesetting of laparoscopic abdominal54,56,62 and breast reconstructionsurgery,63 indicate only a modest analgesic benefit compared with pla-cebo. In particular, Lapmahapaisan et al56 failed to showanalgesic ben-efit in pediatric open abdominal surgery, which they attributed to thelimited ability of their TAP block to cover subcostal incisions.
Clinical Efficacy of the TAP BlockA recent meta-analysis of US-guided TAP block (encom-
passing all approaches and surgery types) concluded that itconfers a statistically significant but clinically modest analgesicbenefit (mean reductions of 6 and 11 mg of intravenously admin-istered [IV] morphine at 6 and 24 hours, respectively) in adult pa-tients undergoing abdominal laparotomy, laparoscopy, or cesareandelivery.64 A similar meta-analysis of pediatric TAP and rectussheath blocks also reported analgesic benefit but only in the earlypostoperative period (first 6-8 hours).65 The authors in both arti-cles rightly note that their findings should be viewed with cautionin view of the pronounced heterogeneity in the included studiesand their analysis. As presented previously, different TAP blockapproaches produce different patterns of local anesthetic spread,46
which may in turn influence analgesic efficacy. This caveat mustbe borne in mind when interpreting the overall evidence for clin-ical efficacy of the TAP block in various surgical settings and maybe partly responsible for some of the conflicting data. In particu-lar, the landmark-guided TAP block appears to have a differentmechanism of action from the US-guided TAP blocks. The poste-rior and cranial spread to the thoracic paravertebral space demon-strated with the landmark-guided TAP block may producesuperior analgesia and thus explain the preponderance of favor-able analgesic outcomes in studies that used this approach. Inthe following section, we present a qualitative review of the evi-dence for the different TAP block approaches according to typeof surgery, with data from the RCTs summarized in Table 2.
Upper Abdominal Surgery
Major open upper abdominal surgeryThe US-guided subcostal TAP is preferred to the US-guided
lateral TAP block in upper abdominal surgery because it is morelikely to cover the supraumbilical dermatomes. For extensivesurgery, both approaches may be combined as in the bilateraldual-TAP block. There are no published data on the efficacyof the landmark-guided TAP block specifically in upperabdominal surgery.
Four studies compared the postoperative analgesia providedby US-guided TAP blocks with thoracic epidural analgesia inmajor upper abdominal surgery.50,52,66,67 Two of these utilizedbilateral subcostal TAP catheters inserted at the end of surgery andan intermittent bolus regimen of local anesthetic52,66; one utilizeda preincisional single-shot subcostal TAP block67; and the fourthinserted preincisional bilateral dual-TAP catheters (4 in total,using the approach described by Sondekoppam et al33) with con-tinuous infusion of local anesthetic.50 On the whole, these studiesindicate that subcostal TAP block is a useful alternative in upperabdominal surgery where epidural analgesia is contraindicatedor undesirable and also has fewer adverse effects, particularly hy-potension.50,66,67 Nevertheless, thoracic epidural analgesia is stilllikely to provide superior analgesia compared with the subcostalTAP block, particularly if the incision extends lateral to the ante-rior axillary line,52 if there is a large component of visceral pain,or if TAP catheters are not utilized to extend analgesic duration.Furthermore, TAP catheter insertion can be technically complex,
144
Copyright © 2017 American Society of Regional Anesthesia and Pain
time consuming, and associated with technical failure52 when insertedpostoperatively because of disruption of the normal tissue planes.
Laparoscopic cholecystectomyBoth US-guided subcostal and lateral TAP blocks have
been studied in laparoscopic cholecystectomy. The subcostalTAP provides superior analgesia compared with the lateral TAPblock,68,69 which is not surprising given that a standard laparo-scopic cholecystectomy utilizes subcostal port sites in additionto a periumbilical one.
Although early studies suggested that the lateral TAP blockmay be of benefit,70,71 they suffered from methodological limita-tions, including use of a surgical technique utilizing only infra-umbilical port sites, and lack of a multimodal analgesic regimen.Subsequent studies have shown marginal benefit of TAP blocksin reducing opioid consumption or pain scores.72–75 Overall,TAP blocks do not have a routine place in laparoscopic cholecys-tectomy, given the low pain scores that can be achieved withsystemic multimodal analgesia and local anesthetic infiltrationof port sites.72,75
Bariatric surgeryTwo RCTs have examined the analgesic efficacy of TAP
blocks in laparoscopic gastric (roux-en-Y) bypass surgery, withconflicting results.51,76 Although Sinha et al76 reported that a post-surgical US-guided TAP block reduced 24-hour opioid consump-tion and pain scores, no details on the TAP block technique andintraoperative or postoperative analgesic regimen were supplied,and it appears likely that multimodal analgesia was not adminis-tered. Albrecht et al,51 on the other hand, found that when addedto a regimen of intraoperative ketorolac, local anesthetic infiltra-tion of port sites, and postoperative acetaminophen a presurgicalUS-guided subcostal TAP block did not significantly reduce24-hour opioid consumption, time to first analgesic request, orpain scores up to 48 hours. At this time, therefore, TAP blocksdo not appear to be a useful addition to multimodal analgesia inthis population.
Lower Abdominal Surgery (Nonobstetric)
Major gynecological surgery including totalabdominal hysterectomy
Multiple studies have examined the role of bilateral TAPblocks in major open gynecological surgery, especially total ab-dominal hysterectomy. A 2013 meta-analysis of data from 4 pub-lished studies (one using the landmark-guided TAP block77 andthe others using the US-guided lateral TAP block78–80) reportedthat TAP blocks significantly reduced 24-hour opioid consump-tion and reduced rest and dynamic pain at 2 hours but not 24 hoursfollowing hysterectomy.110
More recent studies are less positive, however. Two studiesthat investigated the addition of bilateral US-guided lateral TAPblocks to a perioperative multimodal analgesia regimen of nonste-roidal anti-inflammatory drugs (NSAIDs) and acetaminophenfound no difference in 24-hour opioid consumption.81,82 Therewere minimal reductions in rest and dynamic pain, with thegreatest effect observed in the first 2 postoperative hours. Simi-larly, 2 studies83,84 comparingUS-guided lateral TAP block to pla-cebo in the setting of robotic surgery for gynecologic cancer foundno difference in 24-hour opioid consumption or pain scores. Twoadditional studies, on the other hand, both using the landmark-guided TAP approach, reported that bilateral TAP blocks werebeneficial in reducing postoperative opioid consumption and painscores compared with either placebo85 or wound infiltration.86
© 2017 American Society of Regional Anesthesia and Pain Medicine
Medicine. Unauthorized reproduction of this article is prohibited.
-
TABLE
2.Su
mmaryof
RCTs
onTA
PBloc
ks
Stud
yStan
dardized
Man
agem
ent
Intervention
Com
parator
Ana
lgesicOutcomes
Other
Outcomes/Com
ments
Major
upperab
dominal
surgery
Nirajetal,522011
N=62,openhepatobiliary
orrenalsurgery
(incision
superior
toT10).Intraop:
GA+T7-T9epidural
20mLof
0.25%
bupivacaine.Postop:P
Oacetam
inophen1gevery
6h,IV
tram
adol
5-100mg
every6hprn.
BilateralU
SGsubcostalT
AP
cathetersinserted
atend
ofsurgery.Interm
ittent
bolusesof
1mg/kg
0.375%
bupivacaine
every8hfor72
h.
Postop
patient-controlled
epiduralinfusion
of0.125%
bupivacaine
+fentanyl
2μg/m
Lat6-12
mL/h.
Similarpainscores
atrestand
oncoughing
upto72
hpostop.S
ignificantly(Sig)
moretram
adoluseinTA
Pvs
epiduralgroup(m
edian
400mgvs
200mg).8
patients
(30%
)intheTA
Pgrouphad
painfrom
lateralincisions
ordrainsites.
Therapeuticsuccessrateof
63%
inTA
Pgroupvs
78%
inepiduralgroup(N
S).
Technicalfailure
ofTA
Pcatheter
insertionin
7%.
45%
ofTA
Pcathetershad
tobe
resitedpostop
vs7%
ofepidurals.
Wahba
and
Kam
al,662014
N=44,upper
abdominal
surgery.Intraop:
GA+IV
fentanyl
infusion.P
ostop:
IVPC
Amorphine.No
system
icMMA.
BilateralU
SGsubcostal
TAPcathetersinserted
atendof
surgery.Loading
dose
of20
mLfollowed
by15
mLof
0.25%
bupivacaineevery8h
for48
h.
T9-T10
thoracicepidural,
inserted
preop.Postop:
loadingdose
of10
mL
of0.125%
bupivacaine
followed
byinfusion
at6-8mL/h.
Sighigher
pain
scores
atrest
andon
coughing
upto
48h
postop
intheTA
Pgroup.
Sigmorepatientsneeding
IVPC
Amorphinein
TAP
vsepiduralgroup(100%
vs73%).Sigshortertim
eto
firstm
orphinedose
inTA
Pvs
epiduralgroup(m
ean
210vs
311min).Sighigher
morphineuseon
POD1in
TAPvs
epiduralgroup
(median18
vs12
mg)
and
POD2(m
edian11
vs7mg).
Siglongertim
etoflatusinTA
Pvs
epiduralgroup(m
ean52
vs45
h).S
igshortertim
eto
ambulationinTA
Pvs
epidural
group(m
ean48
vs63
h)Sig
lowerincidenceof
hypotension
inTA
Pvs
epiduralgroup(9%
vs46%).Low
erpatient
satisfactioninTA
Pvs
epidural
group(m
edian1vs
3on
0-to
3-pointscale).
Wuetal,672013
N=82,openradical
gastrectom
y.Intraop:
GA+IV
remifentanil
infusion
+IV
sufentanil
bolusesevery1.5h.
Postop:IVPC
Amorphine.
Nosystem
icMMA.
Bilateralp
reincisional
USG
obliq
uesubcostal
TAPblocks
with
20mL
of0.375%
ropivacaine.
GAgroup:no
block,
system
icanalgesiaonly.
TEAgroup:T8-T9
thoracicepidural,
inserted
preop.Intraop:
Loading
dose
8mL
0.25%
ropivacaine,
followed
by5mL
0.25%
ropivacaine
every1h.Postop:
infusion
of0.125%
bupivacaine+morphine
8μg/mLat5mL/h.
TAPvs
GAgroups:S
iglower
dynamicpainscores
at0-6h
inTA
Pgroup,butsimilarrest
anddynamicpainscores
upto
72h.Siglessmorphineuseat
0-6h(m
edian5vs
8mg)
inTA
Pgroup,butsimilaratall
otherintervalsup
to72
h.TA
Pvs
TEAgroups:S
imilarrest
anddynamicpainscores
upto72
h.Similarmorphineuse
at0-6h(m
edian5vs
3mg)
butsighigherinTA
Pgroup
atallotherintervalsup
to72
h.
Technicalfailure
ofepidural
insertionin
2patients(7%)in
TEAgroup.Higherintraop
ephedrinerequirem
entand
incidenceof
postoperative
hypotensionin
theTEAvs
TAPor
GAgroup(21%
vs0%
vs0%
).
Contin
uednextpage
Regional Anesthesia and Pain Medicine • Volume 42, Number 2, March-April 2017 RA of the Abdominal Wall
© 2017 American Society of Regional Anesthesia and Pain Medicine 145
Copyright © 2017 American Society of Regional Anesthesia and Pain Medicine. Unauthorized reproduction of this article is prohibited.
-
TABLE
2.(Con
tinued)
Stud
yStan
dardized
Man
agem
ent
Intervention
Com
parator
Ana
lgesicOutcomes
Other
Outcomes/Com
ments
Ganapathy
etal,502015
N=50,openlaparotomy.
Intraop:
GA+IV
fentanyl
orhydrom
orphoneboluses
prn.Postop:acetaminophen
650mgevery6h,
naproxen
500mgevery
12h,gabapentin
300mg
every12
h.
Bilateralp
reincisionalUSG
dual-TAPcatheters(4
intotal)usinglateral-to-m
edial
approach.L
oading
dose
20mLof
0.5%
ropivacaine
ateach
catheter
site,followed
byinfusion
of0.35%
ropivacaineat4–5mL/h
into
the2catheterson
each
side
usingaY-connectorand
elastomericpump.Postop:
IVPC
Ahydrom
orphone
T7-T8or
T8-T9thoracic
epiduralanalgesia(TEA),
inserted
preopandloaded
with
0.25%
bupivacaine
5mL+3mLprnto
achieveaT6-T12
sensory
block.Intraop:
infusion
of0.1%
bupivacaine+
hydrom
orphone10
μg/m
Lat8mL/h.P
ostop:
infusion
of0.1%
bupivacaine+
hydrom
orphone10
μg/m
Lat8mL/h
with
3mLPC
Abolusevery20
min
prn
for72
h.
Similarrestanddynamicpain
scores
inboth
groups
upto
72h.Similarmorphine
useat0-24
hin
TAPvs
TEA
group(m
ean14
vs16
mg)
and48-72h(13vs
10mg),
butsig
higher
inTA
Pgroup
at24-48h(13vs
5mg).
Fewer
patientswith
pain
scores
>5/10
inTA
Pgroup
(15%
vs29%,n.s.)
Noblockfailuresineithergroup.
Similarly
high
patient
satisfactionscores
inboth
groups.H
igherincidenceof
significanthypotension
inTEA
group(21%
vs0%
).Longer
blockperformance
timein
TAPgroup(m
ean36
min
vs15
min).
Lapmahapaisan
etal,562015
N=54,pediatricmajor
open
abdominalsurgery(upper
>lower).Intraop:
GA+IV
fentanyl
prn.Postop:IV
fentanyl
ormorphineprn.
NoMMA.
Group
I:bilateralsurgicalT
AP
blocks
with
0.5–1mL/kg
0.25%
bupivacaineatend
ofsurgery.
Group
II:W
ound
infiltration
with
0.5–1mL/kg0.25%
bupivacaineatend
ofsurgery.Group
III:
Noblocks.
Nosigdifference
between
groups
inincidenceof
inadequateanalgesiaor
proportio
nof
pain-free
patients.Nosigdifference
inopioid
useover
24hor
timeto
1stanalgesicuse
betweengroups.
Lap
aroscopiccholecystectom
yBhatia
etal,682014
N=60,laparoscopic
cholecystectom
yIntraop:
GA+IV
morphine0.1mg/kg.
Postop:IVacetam
inophen1g
every6h,IV
tram
adol
1–2mg/kg
prn.
Group
I:BilateralU
SGlateral
TAP.Group
II:B
ilateralU
SGsubcostalT
APBolus
injection
of15
mL0.375%
ropivacaine
oneach
side;allblocks
performed
atendof
surgery.
Group
III:Noblocks.
Siglower
restanddynamic
painscores
with
(a)
subcostalT
APvs
noblock
upto24
h;(b)lateralT
AP
vsno
blockup
to2h;(c)
subcostalT
APvs
lateral
TAPfrom
4-24
h.Low
er24
htram
adolusein
subcostalT
APvs
lateral
TAPvs
noblock(m
ean
27mgvs
89mgvs
125mg).
Longertim
etofirstrequest
foropioidinsubcostalT
AP
vslateralT
APvs
noblock
(mean552minvs
411min
vs150min).
Nosigdifference
innausea,
vomiting,orsedationbetween
groups.M
eandynamicpain
scores
(0–10)
inpatients
receivingno
blockranged
from
2.5to4.2during
1st24h.
Chin et al Regional Anesthesia and Pain Medicine • Volume 42, Number 2, March-April 2017
146 © 2017 American Society of Regional Anesthesia and Pain Medicine
Copyright © 2017 American Society of Regional Anesthesia and Pain Medicine. Unauthorized reproduction of this article is prohibited.
-
Shin
etal,692014
N=45,laparoscopic
cholecystectom
yIntraop:
GA+IV
ketorolac30
mg
+IV
fentanyl
prnPostop:
IVfentanyl,IVketorolac
30mgprnin
PACU;
IVnalbuphine
10mgprn
inward.NoMMA.
Group
II:B
ilateralU
SGlateral
TAP.Group
III:BilateralU
SGobliq
uesubcostalT
APBolus
injectionof
20mL0.375%
ropivacaineperside;all
blocks
performed
preincision.
Group
1:no
blocks.
Siglower
restanddynamic
painscores
with
(a)subcostal
TAPvs
noblockup
to3h;
(b)lateralT
APvs
noblockup
to1h;(c)subcostalT
APvs
lateralT
APfrom
1–24
h.Nosigdifference
inanalgesic
usebetweengroups.
Oblique
subcostalT
APtended
toproducecutaneoussensory
blockfrom
T9-T10
vsT12-L1
with
lateralT
AP(but
not
consistentlyseen).Mean
dynamicpain
scores
(0-10)
inpatientsreceivingno
block
ranged
from
3.0to
4.7at
3–24
h.El-Daw
latly
etal,702009
N=42,laparoscopic
cholecystectom
yusing
4infraumbilicalports.
Intraop:
GA+sufentanil
0.1μg/kgprnPostop:IV
PCAmorphine.NoMMA.
Preincisionalb
ilateralU
SGlateralT
APblockwith
15mL0.5%
bupivacaine
perside.
Noblocks.
Sigless
intraopsufentanilin
TAPgroup(m
ean8.6μg
vs23.0μg).Sigless
morphine
usein
24hin
TAPgroup
(mean10.5mgvs
22.8
mg).
Pain
scores
notassessed.
Raetal,712010
N=54,laparoscopic
cholecystectom
y.Intraop:
GA(TIVA)+remifentanil
infusion.P
ostop:
IVfentanyl
20μg
prnor
IVketorolac
30mgprnin
PACU,and
IVketorolac30
mgevery
8hfor1st2
4h.
Preincisionalb
ilateralU
SGlateralT
APblocks
with
15mLof
LAperside.
Group
I:0.25%
bupivacaine.
Group
II:0
.5%
bupivacaine.
Control
group:
noblocks.
Siglower
pain
scores
inboth
TAPgroups
vscontrolg
roup
upto
24h.Similarpain
scores
betweenTA
Pgroups.F
ewer
patientsin
either
TAPgroup
received
ketorolacor
fentanyl
inPA
CUvs
control.
Fewer
patientsin
either
TAP
groupcomplainedof
sleep
disturbancedueto
pain.
Petersen
etal,722012
N=74,laparoscopic
cholecystectom
y.Intraop:
GA(TIVA)+remifentanil
infusion
+IV
sufentanil
0.2μg/kgatendof
surgery.
Postop:P
Oacetam
inophen
1gevery6h,PO
ibuprofen
400mgevery6h.IV
morphine2.5mgprnin
1st2
h;PO
ketobemidone
2.5mgprnin
2–24
h.
Preincisionalb
ilateralU
SGlateralT
APwith
20mL0.5%
ropivacaineperside.
Noblocks.
Sigreductionindynamicand
restpainover24
h(m
easured
asarea
undercurve).S
iglower
morphineuseinTA
Pvs
control
groups
at0-2h(m
edian5mg
vs7.5mg).N
osigdifference
inketobemidoneuseinTA
Pvs
controlg
roupsat2–24
h(m
edian0mgvs
5mg).
Similarincidenceof
nausea
and
vomiting,and
levelo
fsedation
betweengroups.G
raphicaldata
indicatethatdifferencesinpain
scorearemostm
arkedup
to8h,butsimilarat24
h.
Tolchard
etal,732012
N=43,laparoscopic
cholecystectom
y.Intraop:
GA+fentanyl
3μg/kg+
acetam
inophen15–20mg/kg
+diclofenac
0.5mg/kg.
Postop:IVfentanyl
20μg
prnin
PACU;IM
morphine,
POtram
adol,orPO
codeine
and“non-opioid”
analgesics
inward.
Preincisionalu
nilateralU
SGsubcostalT
APblockwith
1mg/kg
ofbupivacaine
(meanvolume22
mL).
PostoperativeLA
infiltrationof
port
siteswith
1mg/kg
bupivacaine(m
ean
volume21
mL).
Siglower
pain
scores
inTA
Pgroupup
to4h.Similar
numberof
patientsrequired
fentanyl
inPA
CUbutd
ose
was
siglower
inTA
Pgroup
(median0.9vs
1.5μg/kg).
Siglower
opioid
usein
TAPgroupover
8h(m
edian
9.2mgvs
16.9mgIV
morphineequivalents).
Shortertim
eto
dischargefrom
PACUin
TAPgroup(m
edian
65vs
110min).
Chenetal,742013
N=40,laparoscopic
cholecystectom
y.Intraop:
GA+IV
fentanyl
0.5μg/kg
prnPostop:IVmorphine
0.05
mg/kg
prn.NoMMA.
Preincisionalb
ilateralo
blique
subcostalT
APwith
20mLof
0.375%
ropivacaineperside.
IVmorphine0.1mg/kg
post-inductio
nof
GA.
Nosigdifference
inintraop
fentanyluseinTA
Pvs
control
groups
(mean24.5vs
31.3μg)
orinpostop
morphineuse
(0.0mgvs
0.4mg).
Nosigdifference
insedatio
nor
nausea
andvomiting
between
groups.S
igshortertim
eto
extubatio
nin
TAPgroup
(mean10.4minvs
12.4
min).
Contin
uednextpage
Regional Anesthesia and Pain Medicine • Volume 42, Number 2, March-April 2017 RA of the Abdominal Wall
© 2017 American Society of Regional Anesthesia and Pain Medicine 147
Copyright © 2017 American Society of Regional Anesthesia and Pain Medicine. Unauthorized reproduction of this article is prohibited.
-
TABLE
2.(Con
tinued)
Stud
yStan
dardized
Man
agem
ent
Intervention
Com
parator
Ana
lgesicOutcomes
Other
Outcomes/Com
ments
Ortizetal,752012
N=74,laparoscopic
cholecystectom
y.Intraop:
GA+IV
ketorolac30
mg+IV
fentanyl
50μg
prn+IV
morphineprnatendof
surgery.
Postop:H
ydrocodone
10mg+
acetam
inophen1gevery6h,IV
morphine4mgevery3hprn.
Preincisionalb
ilateralU
SGlateralT
APblocks
with
15mL
of0.5%
ropivacaineperside.
Preincisionalinfiltratio
nof
portsiteswith
total
of20
mLof
0.5%
ropivacaine.
Nosigdifference
inpainscores
betweengroups
upto24
h.Nosigdifference
inintraop
fentanyluseinTA
Pvs
control
groups
(mean237vs
245μg),
intraopmorphineuse(m
ean
5.0vs
5.8mg),or24
hmorphine
use(16.1vs
15.4mg)
Similarincidenceof
nausea
betweengroups.
Bariatricsurgery
Sinhaetal,762013
N=100,laparoscopicgastric
bypass
surgery.Intraop:
GA,noanalgesicdetails
given.Postop:T
ramadol
(route,dose,andinterval
notspecified).NoMMA.
PostoperativebilateralU
SGTA
Pblocks
(not
specified
ifsubcostalo
rlateral)with
20mLof
0.375%
ropivacaineperside.
Noblocks.
Siglower
pain
scores
inTA
Pvs
controlg
roup
upto
24h.Pain
scores
werehighestat1
h(m
edian2vs
4)andlowest
at24
h(0
vs1).S
iglower
tram
adol
usein
TAPvs
controlg
roup
over
24h
(mean9mgvs
48mg).
Shortertim
eto
ambulatio
nin
TAPvs
controlg
roup
(mean6.3hvs
8.0h).
Albrecht
etal,512013
N=57,laparoscopicgastric
bypass
surgery.Intraop:
GA+remifentanilinfusion
+IV
ketorolac30
mg+LA
infiltrationof
portsiteswith
20mLof
0.25%
bupivacaine.
Postop:IVfentanyl
+IV
morphineprnin
PACU.P
Oacetam
inophenevery6h+
POoxycodone5–10
mg
every4hprn,or
IVmorphine2–6mgIV
every
3hprn.
Preincisionalb
ilateralU
SGsubcostalT
APblocks
with
30mLof
0.25%
bupivacaine
perside.
Noblocks.
Similarrestanddynamicpain
scores
upto
48h.Nosig
difference
in24
hopioid
usein
TAPvs
control
group(m
ean32.2
mg
vs35.6mgIV
morphine
equivalents).N
osig
difference
intim
eto
1st
analgesicrequestinTA
Pvs
controlg
roup
(52vs
25min).
Similarratesof
nausea
and
vomiting,pruritusand
length
ofhospitalstay
betweengroups.
Major
gynecologicalsurgery
Carney
etal,772008
N=50,totalabdominal
hysterectomy.Intraop:
GA+IV
morphine
0.15
mg/kg
+PR
diclofenac
100mg+PR
acetam
inophen1g.Postop:
IVPC
Amorphine+PR
acetam
inophen1gevery
6h+PR
diclofenac
100mgevery16
h.
Preincisionalb
ilateralL
MG
TAPblockwith
1.5mg/kg
of0.75%
ropivacaine(m
ax20
mL)perside.
Sham
bilateralT
AP
blocks
with
20mL
0.9%
salin
e.
Siglower
restpain
scores
inTA
Pvs
controlg
roup
at6h(m
edian2vs
4),24h,
(median1vs
3)and36
h(m
edian1vs
3).S
iglower
morphineusein
TAPvs
controlg
roup
over
24h
(mean21.1vs
39.6mg)
andover
48h(26.8vs
55.3mg).S
iglonger
time
to1stP
CAmorphine
requestinTA
Pvs
control
group(m
edian45
vs12.5min).
Siglower
rateof
sedatio
nin
TAPvs
controlg
roup
(37%
vs63%).Similarrateand
severity
ofnausea.
Chin et al Regional Anesthesia and Pain Medicine • Volume 42, Number 2, March-April 2017
148 © 2017 American Society of Regional Anesthesia and Pain Medicine
Copyright © 2017 American Society of Regional Anesthesia and Pain Medicine. Unauthorized reproduction of this article is prohibited.
-
Atim
etal,782011
N=60,totalabdominal
hysterectomy.Intraop:
GA+IV
diclofenac
75mg+IV
tram
adol
0.5mg/kg.P
ostop:
IVPC
Atram
adol
+IM
pethidine1mg/kg
prn.
NoMMA.
Group
I:preincisionalb
ilateral
USG
lateralT
APblocks
with
20mL0.25%
bupivacaine
perside.G
roup
II:W
ound
infiltrationwith
20mL0.25%
bupivacaineatendof
surgery.
Sham
bilateralT
AP
blocks
with
20mL
0.9%
salin
e.
Low
errestanddynamicpain
scores,and
tram
adol
usein
TAPvs
controlg
roup
upto
24h.Similarrestand
dynamicpain
scores
inTA
Pvs
infiltrationgroup
upto
4h,butlow
erin
TAP
groupat6hand24
h.Low
ertram
adol
usein
TAP
groupup
to24
h.Siglower
restanddynamicpain
scores
ininfiltrationvs
controlg
roup
upto
4h.
Griffith
setal,792010
N=65,m
ajor
gynecological
surgeryviamidlin
eincision.
Intraop:
GA+IV
morphine
0.1–0.2mg/kg
+IV
acetam
inophen1g+IV
parecoxib40
mg.Postop:
IVPC
Amorphine+PO
/IV
acetam
inophen1gevery6h.
BilateralU
SGlateralT
AP
blocks
with
20mLof
0.5%
ropivacaineperside
after
wound
closure.
Sham
bilateralU
SGTA
Pblocks
with
0.9%
salin
e.
Nosigdifference
inincidence
ofsevere
restor
dynamicpain
(>5/10)at2hor
24h.Nosig
difference
inmorphineusein
TAPvs
controlg
roupsat2h
(mean11.9vs
13.5mg)
or24
h(36vs
34mg).
Nodifference
inincidence
ofnausea,vom
iting,
pruritu
s,or
sedatio
n.
Shin
etal,802011
N=32,gynecologicalsurgery
viatransverse
incision.
Intraop:
GA(TIVA)+
remifentanilinfusion.Postop:
IVPC
Aketorolac-sufentanil.
RescueIV
meperidineor
ketorolacprn.NoMMA.
Preincisionalb
ilateralU
SGlateralT
APblockwith
20mL
0.375%
ropivacaineperside.
NoTA
Pblocks.
Siglower
pain
scores
inTA
Pvs
controlg
roup
at2h(m
ean3.0
vs5.2),24h(m
ean0.9vs
2.2)
butn
ot48
h(0.4
vs1.6).N
osigdifference
inIV
PCAuse
inTA
Pvs
controlg
roup
over
48h(102
mLvs
108mL)
Low
errescue
analgesicusein
TAPvs
controlg
roup.
Sighigher
satisfactionscores
inTA
Pvs
controlg
roup
upto
48h.
Røjskjaer
etal,812015
N=46,totalabdominal
hysterectomy.Intraop:
GA
(TIVA)+remifentanil
infusion
+IV
sufentanil
0.3μg/kgatendof
surgery.
Postop:IVPC
Amorphine+
POacetam
inophen1gevery
6h+ibuprofen600mg
every6h.
Preincisionalb
ilateralU
SGlateralT
APblockwith
20mL
0.75%
ropivacaineperside.
Sham
bilateralU
SGTA
Pblocks
with
0.9%
salin
e.
Siglower
restpain
scores
inTA
Pvs
controlg
roup
at2h,and
lower
dynamicpain
scores
at8h.Nosigdifferencesin
restor
dynamicpain
atother
timepoints.N
osigdifference
inmorphineusein
TAPvs
controlg
roup
at24
h(m
ean
36vs
33mg).
Nosigdifferencesbetween
groups
inPA
CUlengthof
stay,timetofirstm
obilization,
nausea
orvomiting.
Gasanova
etal,822013
N=75,totalabdominal
hysterectomy.Intraop:
GA+IV
fentanyl
prn+IV
morphine0.1–0.15
mg/kg.
Postop:IVPC
Amorphine.
Group
I:BilateralU
SGlateral
TAPblocks
with
20mL0.5%
bupivacaineperside
atendof
surgery+IV
ketorolac30
mg+
postop
MMA.G
roup
II:T
AP
blocks
atendof
surgeryonly.
Group
III:IntraopIV
ketorolac30
mg.
Postop
MMA:IV
ketorolac30
mg
every6h+PO
acetam
inophen
650mgevery6h.
Nosigdifference
inrestingpain
scores
betweengroups
over
48h.
Sigdifference
indynamicpain
scores
betweengroups
IandIII,
butn
otbetweengroups
IandII,
orIIandIII.Nosigdifference
inmorphineusebetweengroups
at24
h(Ivs
IIvs
III:38.4
vs38.6
vs42.6mg).
Similarincidenceandseverity
ofnausea
andvomiting.
Contin
uednextpage
Regional Anesthesia and Pain Medicine • Volume 42, Number 2, March-April 2017 RA of the Abdominal Wall
© 2017 American Society of Regional Anesthesia and Pain Medicine 149
Copyright © 2017 American Society of Regional Anesthesia and Pain Medicine. Unauthorized reproduction of this article is prohibited.
-
TABLE
2.(Con
tinued)
Stud
yStan
dardized
Man
agem
ent
Intervention
Com
parator
Ana
lgesicOutcomes
Other
Outcomes/Com
ments
Hotujec
etal,832015
N=64,robotic-assisted
laparoscopicgynecologic-
oncologicsurgery.Intraop:
GA.N
ootheranalgesics
given.Postop:“standard
managem
ent”with
IV+PO
opioidsandNSA
IDs.
Preincisionalu
nilateralU
SGlateralT
APblockwith
30mL
0.25%
bupivacaine.
Sham
TAPblock
with
0.9%
salin
e.Nosigdifference
inpain
scores
at24
hin
TAPvs
controlg
roup
(mean6.44
vs6.97).Nosig
difference
inmorphineuseat
24hin
TAPvs
controlg
roup
(mean64.9
vs69.3
mg).
Nosigdifference
inpatient
satisfactionwith
analgesia
betweengroups.
Torupetal,842015
N=65,robotic-assisted
laparoscopichysterectomy.
Preop:
POacetam
inophen
1g+diclofenac
50mgor
ibuprofen400mg.Intraop:
GA(TIVA)+reminfentanil
infusion
+IV
morphine
0.2mg/kg.Postop:IV
PCA
morphine+PO
acetam
inophen
1gevery6h+diclofenac
50mgor
ibuprofen400mg
every8h.
Preincisionalb
ilateralU
SGlateralT
APblockwith
20mL
0.5%
ropivacaineperside.
Sham
TAPblocks
with
0.9%
salin
e.Nosigdifference
inpain
scores
inTA
Pvs
controlg
roup
at1h
(median4.2vs
4.0)
orover
24h
(2.0vs
2.1).N
osigdifference
inmorphineuseat24
hin
TAPvs
controlg
roup
(median17.5mg
vs17.5mg).
Nosigdifferencesin
nausea
orvomiting
betweengroups.
Amrand
Amin,852011
N=68,totalabdominal
hysterectomy.Intraop:
GA+IV
fentanyl
1μg/kgprnPostop:IV
morphine20–50μg/kgprn.
NoMMA.
Group
I:Preincisionalb
ilateral
LMGTA
Pblocks
with
20mL
0.375%
bupivacaine.Group
II:
TAPblocks
atendof
surgery.
Group
III:Sh
amblock.
Siglower
dynamicpain
scores
upto
48hin
both
groupIand
IIvs
groupIII.Siglower
dynamicpain
scores
upto
48h
ingroupIvs
II.S
iglower
intraop
fentanyl
requirem
entsin
groupI
vsIIvs
III(m
ean81
vs170
vs166μg).Siglower
morphine
useat48
hin
both
groupIandII
vsgroupIII(m
ean21
mgvs
33mgvs
66mg).S
iglonger
time
tofirstanalgesicrequestinboth
groupIandIIvs
groupIII(135
vs120vs
102min).
Low
erincidenceof
PONV
ingroupIandIIvs
III
(16%
vs29%
vs67%).
Siglower
incidenceof
chronicpain
ingroupI
vsgroups
IIandIII.
Failu
reof
TAPblock
(absence
ofloss
tocold
sensation)
was
6%.
These
patientswere
excluded
from
analysis.
Sivapurapu
etal,862013
N=52,gynecological
surgery(unspecified).
Intraop:
GA+IV
fentanyl
0.5μg/kgprn.Postop:
IVPC
Amorphine.
NoMMA.
BilateralL
MGTA
Pblock
with
0.3mL/kgof
0.25%
bupivacaineperside
atend
ofsurgery.
Wound
infiltration
with
0.6mL/kgof
0.25%
bupivacaine.
Siglower
pain
scores
inTA
Pvs
infiltrationgroupup
to24
h.Siglower
morphineusein
TAP
vsinfiltrationgroupat24
h(m
ean22
vs29
mg).S
iglonger
timeto
1stanalgesicusein
TAP
vsinfiltrationgroup
(148
vs85
min).
Chin et al Regional Anesthesia and Pain Medicine • Volume 42, Number 2, March-April 2017
150 © 2017 American Society of Regional Anesthesia and Pain Medicine
Copyright © 2017 American Society of Regional Anesthesia and Pain Medicine. Unauthorized reproduction of this article is prohibited.
-
DeOliveira
etal,872011
N=75,laparoscopic
hysterectomy.Intraop:
GA+remifentanilinfusion
+IV
hydrom
orphone
10μg/kg+IV
ketorolac
30mg.Postop:IVPC
Ahydrom
orphone+ibuprofen
600mgevery6h.
Group
I:preincisionalb
ilateral
USG
lateralT
APblocks
with
20mL0.5%
ropivacaineperside.
Group
II:p
reincisionalbilateral
USG
lateralT
APblocks
with
20mL0.25%
ropivacaineperside.Group
III:bilateral
sham
blocks
with
20mL0.9%
salin
e.
Siglower
pain
scores
forboth
groups
IandIIvs
groupIII
upto
24h.Siglower
opioid
usein
groupIvs
both
groups
IIandIIIover
24h(m
edian7.5
vs15
vs15
mgIV
morphine
equivalents).
Sigbetterquality
ofrecovery
scores
inboth
groupI
andIIvs
groupIII.
Kaneetal,882012
N=58,laparoscopichysterectomy.
Intraop:
GA+IV
ketorolac
30mg+unspecifiedanalgesics
prnPostop:“Standard”PO
and
IVanalgesics
(unspecified)
BilateralU
SGlateralT
AP
blocks
with
20mL0.5%
ropivacaineperside
attheendof
surgery.
NoTA
Pblocks.
Nosigdifference
inpain
scores
inTA
Pvs
controlg
roup
at2h
(median5vs
6)or
24h(m
edian
5vs
5).N
osigdifference
inmorphineusein
TAPvs
control
groupon
POD0(m
edian11.7vs
11.8mg)
andPO
D1(m
edian
7.5vs
9.0mg).
Nosigdifference
inquality
ofrecovery
scores
betweengroups.
Calleetal,892014
N=197,outpatient
laparoscopic
hysterectomy.Intraop:
GA+
remifentanilinfusion+IV
morphineprnPostop:IV
morphineprnin
PACU.P
Oacetam
inophen1gevery
6h+PO
ibuprofen400mg
every8hpost-discharge.
BilateralsurgicalT
AP
blocks
with
1.5mg/kg
bupivacainein
20mL
perside
attheend
ofsurgery.
Sham
TAPblocks
with
20mL0.9%
salin
eperside.
Siglower
pain
scores
atdischarge
inTA
Pvs
controlg
roup
(mean
3.8vs
3.1).N
osigdifferences
inpain
scores
betweengroups
at24
h,48
h,or
72h.Nosig
differencesin
perioperative
morphineusein
TAPvs
control
group(m
ean1.8vs
1.49
mg).
Nosigdifference
inPA
CU
oroveralllengthof
stay
betweengroups.
Bhattacharjee
etal,902014
N=90,totalabdominal
hysterectomy.Intraop:
GA+IV
fentanyl
0.5μg/kg
prn+IV
acetam
inophen1g.
Postop:IVtram
adol
2mg/kg
prnfor1std
osethen
every8
h+IV
acetam
inophen1g
every6h.
Preinductionbilateral
LMGTA
Pblocks
with
0.5mL/kg0.25%
bupivacaineperside.
Sham
TAPblocks
wit