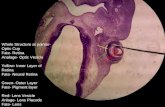
Embryo - Ear
-
Upload
std-dlshsi -
Category
Documents
-
view
124 -
download
4
Transcript of Embryo - Ear

z
EAR: OVERVIEW
EYE EAR
APPEARANC
EDay 22
Day 22 (but, becomes apparent at day 24)
PRIMORDIU
M (ANLAGEN)
Optic Groove (Vesicle)
Otic Vesicle
DEVELOPM
ENT
From Inside, Outward
From Outside, Inward
EMBRYONIC LOCATION
At the level of the Diencephalon
At the level of the Rhombencephalon
General Function of the Ear
Hearing (Audition) Perception of gravity through balance
(Equilibrium)
The 3 Distinct Parts of the Ear (External, Middle & Internal)
External Ear
Collecting of sounds (sound waves) Pinna notching
o Cancelling noise
o Focusing on a specific sound
E.g. as in, isolating the voice of the person talking to you in a noisy environment.
Middle Ear
Amplification of Sound Conduction of vibration from the
tympanic membrane to the → cochlea via the oval window.
Consist of ossicula (ossicle) – conducts sound waves to form vibration (mechanical)
o Malleus (hammer)
o Incus (anvil)
o Stapes (stirrup)
Internal Ear
Converts the sound waves (vibration) into nerve impulses (electrical) ramified axons CN VIII
EMBRYOLOGY: DEVELOPMENT OF THE EAR Page 1
SUBJECT: EMBRYOLOGY
TOPIC: DEVELOPMENT OF THE EAR
LECTURER: DR. JOSE ANTONIO AMISTAD
DATE: MARCH 2011

*CN VIII: Vestibular part = Balance; Cochlear/Spiral = HearingAt 4 weeks age of gestation,The Otic Pits are found dorsal/posterior to the rhombencehalon.
From the surface ectoderm forms the Otic Placode
On day 24 the (A) otic placode invaginates to form the (B) otic pit. The otic pit will continue to invaginate, and the rims of the otic pit will fuse to form the (C) otic vesicle.
Figure: A. 24 days. B. 27 days. C. 4.5 weeks
Otic Placode → Otic Pit → Otic Vesicle → Internal Ear
Neural crest cells and some cells on the medial side of the otic vesicle migrate medial to the otic vesicle forming the statoacoustic ganglion.
Neural crest cells + medial otic vesicle = statoacoustic ganglion
Development of the otocyst (otic/auditory vesicle)
The dorsal portion will form the utricle and the ventral portion will form the saccule. The extension above the utricle forms the endolymphatic duct which forms the endolymphatic sac at the superior end. The connection between the utricle and saccule is the utricolosaccular duct or vestibule.
During embryonic period, the endolymphatic duct is attached to the utricle. Upon birth until adulthood, the endolymphatic is continuous with the saccule.
Functions of the endolymphatics
Secretes endolymph/absorb excess endolymph
Responsible for phagocytosis and immunodefense
The inferior tip of the saccule will form a tubular outpocketing (cochlear duct) and penetrate the mesoderm (loose mesenchyme). It will extend spirally forming two and a half (2 ½) turns. (Wikipedia says: 2 ¾) The lower end of the saccule is connected to the cochlear duct through a short membranous tube called ductus reuniens.
The utricle, saccule and the endolymphatic (duct/sac) form the membranous labyrinth, and the bone that covers it forms the bony labyrinth.
The innermost part of the vestibule is the macula acusticae (sensory unit of the vestibule). It is between the saccule and the utricle responsible for perception of gravity (vestibular purposes). It contains sensory cells called crista ampullaris (also cupula)
In other references: The crista ampullaris is defined as an elevation at the inner surface of the ampulla of each semicircular canal.
Going back to the cochlear duct…
The cochlear duct becomes the main house for endolymph. This endolymph is contained in the scala media. Earlier, it was mentioned the formation of cochlear duct will penetrate the mesoderm; this mesoderm (around) will form a cartilage completing the cochlea. It is shown in the following diagram labelled ‘cartilaginous shell’. This will form 2 cavities for the perilymph. Located above is the scala vestibuli and below is the scala tympani. The vestibular membrane or the reissner’s membrane separates the scala vestibuli and scala tympani.
Endolymph = ↑ K+, ↓ Na+
Perilymph = ↑ Na+, ↓ K+
**mneumonic: Magkano ang kendi? Piso‘Kendi’ (‘K’ potassium; ‘Endi’ Endolymph), ‘Piso’ (‘P’ perilymph; ‘so’ sodium)
Development of the organ of Corti
EMBRYOLOGY: DEVELOPMENT OF THE EAR Page 2

The hair cells and the tectorial membrane found at the floor of the cochlear duct overlying the basilar membrane forms the sensory unit of the cochlea called the organ of Corti.
During 10 weeks there is a pseudostratified lining of the scala media, on the 28th day it is divided into two ridges – the inner ridge (thinner) and the outer ridge (thicker). The thinner inner ridge will form the spiral limbus. The spiral limbus forms the tectorial membrane (gelatinous protein-polysaccharide) a.k.a. copula.
Filaments of the vestibular nerve pass through the crista( of the crista ampullaris) to reach hair cells on its surface; the hair cells are capped by the copula, a gelatinous protein-polysaccharide mass
Components of the tectorial membrane: α-tectorin β-tectorin otogelin (which makes it thicker) collagen type 11 (which comes from the spiral
limbus)
The inner ridge it connected to the outer ridge through teeth like structure called the auditory teeth of Huschke.
In other references, the acoustic teeth is defined as, tooth-shaped formations or ridges occurring on the vestibular lip of the limbus lamina spiralis of the cochlear duct.
The outer ridge will form 3 rows of outer hair cells and 1 row of inner hair cell. The superior of the inner hair cells is composed of stereocilia in progressively increasing heights. The tallest cilium is called the kinocilium which is connected superiorly to the tectorial plate. This is important the formation of signals to the brain.
The outer hair cells are shorter than the inner hair cells. To reach the tectorial membrane the outer hair cells are supported by the Deiters
cells (not Deiter’s). Between the outer hair cells, Deiters cell and the inner haircell is a space called the subtectorial space. To maintain the distance between the inner and outer hair cells, there is a membrane called the Hardesty membrane.
The Hensen’s stripe is the attachment of the outer ridge to the spiral ligament that holds the scala media.
In other references: inner part of the tectorial membrane is thin and overlies the auditory teeth of Huschke; its outer part is thick, and along its lower surface, opposite the inner hair cells, is a clear band, named Hensen’s stripe, due to the intercrossing of its fibers.
The bony axis of the cochlea which holds the scala media is formed by the modiulus. This also holds the ramifying axons of the auditory nerve.
Development of the semicircular canals
At the end of the utricle forms flattened outpocketing which later form the semicircular canals. This will form a continuous space inside. Medial to these semicircular formations, the apposing walls will start to fuse and become invaded by caspases leading to its disappearance.
3 semicircular canals1. Transverse/Lateral/Horizontal2. Posterior (nothing else, NOT inferior)3. Anterior/Superior
Saccule forms the bony cochlea the utricle forms the semicircular canal
The semicircular canal has a dilated and a non-dilated end. The
EMBRYOLOGY: DEVELOPMENT OF THE EAR Page 3

dilated end is the crus ampullare and the non-dilated end is the crus non-ampullare. The Ampulla contains the crista ampullaris (which is composed of cupula and ,kinocilium)
The close proximity of the endolymphatic duct and perilymphatic duct with the cranial vault may cause the CSF to flow out from the ear during injuries at this location – as in, vehicular accidents.
MIDDLE EAR Incus (Pharyngeal arch 1) Maleus (Pharyngeal arch 1) Stapes (pharyngeal arch 2)
**Mneumonic: IM#1; Second
**Modern alternative theory: some parts of Maleus come from PA2; for the purpose of studying we stick with the above.
The dorsal end of pharyngeal arch 1 and 2 will form the pinna.
The pharyngeal pouch (endodermal) it will extend laterally to the condensed mesenchyme, this condensed mesenchyme will form the tympanic cavity that will house the ossicles. It also forms the area of otic tension of the tympanic membrane.
The 3 ossicles are the earliest bones that will ossify. During 12 weeks age of gestation they ossify within 2 days. Of the 3, the stapes is the oldest bone. The rapid ossification deprives these bones to grow bigger causing them to be very small.
FGF-ERK2 – responsible for type and shape of ossicles;( ERK=extracellular signal regulated kinase 2)
NOX2 – (NADPH Oxidase Homeobox 2)
DUSP6 – (Dual Sensitivity Phosphate 6) Shape of the pinna
The innermost part of the cleft between PA 1 and 2 (Pharyngeal groove) which is ectodermal undergoes meatal plugging or solid epithelial proliferation. This leads to the elongation of the canal. During 7th month age of gestation, this meatal plug dissolves. The floor of this meatal plug forms the myringa (transparent vibrating membrane; lower portion of tympanic membrane)
In Myringotomy or Incision of the tympanic membrane is done at the area of the myringa using a knife for paracentesis called myringotome. This paracentesis allows accumulated fluid to move out of the middle ear through the tympanic membrane.
The tympanic membrane is formed by the fusion of 3 germ layers – Meatal plug ectodermal, tympanic cavity (endodermal), and the intermediate layer of the tympanic cavity called fibrous stratum (mesodermal).
EMBRYOLOGY: DEVELOPMENT OF THE EAR Page 4

Development of the PinnaClockwise numerical Hillocks (1-6)
1 –tragus6 – anti-tragus2-5 – helix
Formation of the other parts such as anti-helix is secondary to the development of 2-5
Zaheer’s ear – Absence of hillock 6 (earphone syndrome)
Selhurst’s handle– enlarged 2-5 (cup handle ear)
Stahl’s ear – formation of a third crura at the superior crus
Cryptotia – Absence of Auricular fossa Cryptophthalmia – Fusion of eyelids Darwin’s tubercle – a small inconstant
projection from the upper end of the posterior portion of the incurved free margin of the helix of the auricle
CLINICAL CORRELATION
A and B = Preauricular pits
C and D = Preauricular tag or appendages
These are hints of internal ear problem or indicate early presbycusis.
Amblyopia – Poor vision caused by abnormal development of visual areas of the brain in response to abnormal visual stimulation during early development.
Say-Barber-(Miller) syndromeo Macrotia
o Bulbus nose
o Hypertelorism
o Telecanthus
o Hirsutism
o Skin folding of the neck
o Macrostomia
o Absence of mammary glands
Eerler Landos
o Hypersensitivity of ear’s elastic cartilage
o Lysyl oxidase deficiency
Börjeson-Forssman-Lehmann syndrome
o Selhurst handle (ear)
o Shortened toe
o Gynecomastia (male)
o Mental retardation
o Trunkal obesity
SHORT syndrome
o Tooth decay
EMBRYOLOGY: DEVELOPMENT OF THE EAR Page 5

o Short stature
o Corectopia
Microtia
Grade
I – miniature ear
II – cleft, “hemi-ear”
III – absence of ear canal, peanut vestige
IV – dorsal end or total absence of ear
*Grade III & IV have absence of ossicles and tympanic membrane, although surgically repairable
*BAHA – Bone anchor hearing aid
* Grade I & II – stop in ear development
Strabismus
o Entotropia – type of strabismus in which the visual axes converge
o Exotropia – type of strabismus in which the visual axes diverge
*Entropion - infolding of the margin of an eyelid
*Ectropion - A rolling outward of the margin of a part
*Corectopia - Eccentric location of the pupil so that it is not in the center of the iris.
o Embryotoxon
o Congenital limbal(limbus) opacity
Common cause of congenital cataract – German measles
Adult cataract – commonly caused by Diabetes mellitus type 2
Cyclopia – single eye
Synophthalmia – fused eye
Proboscsis – A long flexible snout
Coloboma – found in CHARGE syndrome
CHARGE syndrome (association)
coloboma of the eye, heart defects (typically tetralogy of Fallot, patent ductus arteriosus, or ventricular or atrial septal defect), atresia of the choanae, renal anomalies and retardation of growth and/or development, genital anomalies in males such as small penis or cryptorchidism, and ear abnormalities or deafness
4 types of cataract
Sutural/Structural Cataract (inverted ‘Y’) - a congenital type of cataract with opacities along the Y sutures of the fetal lens nucleus; usually does not affect vision
Lamellar cataract - a cataract in which the opacity is limited to the cortex
Globular cataract
leukocoria, leukokoria - Reflection from a white mass within the eye giving the appearance of a white pupil.
Red eye reflex – secondary to mirroring of light on the tapetum lucidum
Ishihara test (3 seconds flashing of image)
Thompson wool test
Monochromacy
cone monochromacy
o Grayscale vision
rod monochromacy
o Blindness rely to other wavelengths such as sound
o Loud talking
Dichromacy
Trichromacy
Red 564-580 nm
EMBRYOLOGY: DEVELOPMENT OF THE EAR Page 6

Green 532-540 nm
Blue 400-440 nm
Protanopia (red)
Red = dark brown/gray
Green = yellow
Blue = Blue
Deuteronopia
Red = yellow
Green = yellow
Blue = blue
Tritanopia
Red = red
Green = green / blue-green
Blue = light blue / pink
Lea’s Test
Landolt chart (C-like letters)
Snelen’s chart
-letters discovered by sloan
END OF TRANSCRIPTION
SUMMER!!!
EMBRYOLOGY: DEVELOPMENT OF THE EAR Page 7