Dry eye ppt
-
Upload
prerna-garg -
Category
Health & Medicine
-
view
1.615 -
download
4
description
Transcript of Dry eye ppt

DRY EYEDry eye is a multifactorial disease of the tears
and ocular surface that results in symptoms
of discomfort, visual disturbance, and tear
film instability with potential damage to the
ocular surface. It is accompanied by
increased osmolarity of the tear film and
inflammation of the ocular surface.

TEAR FILM The presence of precorneal
layer of liquid was first
demonstrated by Fischer in
1928.
Rollet described it as 6th
layer of cornea.
Wolff was the first to describe
the structure of tear film.
Tear film is a 3 layered
structure-
Lacrimal secretory
system has been divided
into 2 parts-
a. Basic secretors- goblet
cells, accessory lacrimal
glands, oil glands
B. reflex secretor- main
lacrimal gland


The concept of the 3 layer architecture has been replaced by
the concept of an integrated aqueous and mucin gel with a
graded concentration of mucins under a dynamic lipid layer.
The outer lipid layer is secreted by the meibomian glands. Lid
movement during blinking releases the lipid from the glands.
This layer prevents evaporation of the aqueous layer and also
acts as a surfactant allowing spread of the tear film. The
synthesis and secretion is influenced by hormones. Androgen
receptor and receptor proteins are found in the nuclei of the
glands.

Middle aqueous layer is secreted by the main and accessory lacrimal
glands.
Accessory lacrimal glands of Krause, Wolfring and Manz produce the
basal tear secretion. Androgen and Estrogen receptors have been
found on these glands, androgen function is more critical.
The main lacrimal gland produces the reflex secretion in response to
corneal and conj sensory stimulation, tear break up and ocular
inflammation mediated via the 5th cranial nerve. Responsible for 95% of
the aqueous component. It is decreased by topical anaesthesia and
during sleep. The innervation of the lacrimal gland is by sympathetic,
parasympathetic and sensory nerves.

The functions of this layer-
1. to provide oxygen from atmosphere to the cornea
2. anti bacterial function
3. to wash away debris and noxious stimuli and allow passage to
leucocytes after injury
4. to provide a smooth optical surface to the cornea.
The inner mucin layer is produced by the conjunctival and corneal
epithelial cells-goblet cells. Mucins are responsible for the wetting
of the corneal surface. Secretory mucins (MUC 5A) are secreted
by the goblet cells. The transmembrane mucins ( MUC 1 , MUC 4)
form the glycocalyx and are produced by non goblet cell epithelia.


Mucus is produced when the electrolyte composition of the
tear film changes from normal or when it becomes
hyperosmolar. Also sympathetic and parasympathetic nerves
are located adjacent to the conj goblet cells and sensory
stimulation of the cornea causes goblet cell mucus discharge.
The potassium concentration of the tear film is about 5 times
higher than in aqueous humor or serum. The normal
osmolarity is 306 +/- 2 mosm/l. it is lowest in the morning and
increases as the day progresses.

Dry eye is recognized as a disturbance of the Lacrimal Functional
Unit (LFU), an integrated system comprising -- the lacrimal glands,
ocular surface (cornea, conjunctiva and meibomian glands) and
lids, and the sensory and motor nerves that connect them.
This functional unit controls the major components of the tear film in
a regulated fashion and responds to environmental,
endocrinological and cortical influences.

CLASSIFICATION OF DRY EYE
1. AQUEOUS TEAR
DEFICIENT DRY EYE–
lacrimal tear deficiency
a. Sjogren syndrome- primary/ secondary
b. Non sjogren syndrome-
---lacrimal gland deficiencies
---lacrimal gland duct obstruction
---reflex block
---systemic drugs
2. EVAPORATIVE DRY EYE-
A. Intrinsic- meibomian gland dysfunction
-- disorders of lid aperture
--low blink rate
--drug action
b. Extrinsic-- Vit A deficiency- Topical drugs- preservatives- Contact lens wear- Ocular surface disease-
Allergy

Conditions associated with non-Sjogren syndrome dry eye
Primary lacrimal gland deficiencies
Age-related dry eye
Congenital alacrima
Familial dysautonomia
Secondary lacrimal gland deficiencies
Lacrimal gland infiltration
-Sarcoidosis
-Lymphoma
-AIDS
Graft vs host disease
Lacrimal gland ablation
Lacrimal gland denervation

Obstruction of the lacrimal gland ducts
Trachoma
Cicatricial pemphigoid and mucous membrane pemphigoid
Erythema multiforme
Chemical and thermal burns
Reflex hyposecretion
Reflex sensory block
Contact lens wear
Diabetes
Neurotrophic keratitis
Reflex motor block
VII cranial nerve damage
Multiple neuromatosis

Age related dry eye
With increasing age, there is an increase in ductal pathology that
could promote lacrimal gland dysfunction by its obstructive effect.
These alterations include periductal fibrosis, interacinar
fibrosis, paraductal blood vessel loss and acinar cell
Atrophy. lymphocytic glandular infiltrates were found in 70% of lacrimal
glands studied and considered to be the basis of the fibrosis. Appearances were likened to the less severe grades of Sjogren
syndrome.
It has been suggested
that the low-grade dacryoadenitis could be caused by
systemic infection or conjunctivitis or, alternatively, that
subclinical conjunctivitis might be responsible for stenosis
of the excretory ducts.

Congenital alacrimia- Triple A syndrome ( Allgrove syndrome) –
AC, alacrimia, addison’s disease
Familial Dysautonomia- Riley day syndrome:
generalized insensitivity to pain accompanied by a marked
lack of both emotional and reflex tearing, within a multisystem
disorder. There is a developmental and progressive neuronal
abnormality of the cervical sympathetic and parasympathetic
innervations of the lacrimal gland and a defective sensory
innervation of the ocular surface, which affects both small
myelinated (Aδ) and unmyelinated (C) trigeminal neurons.

Obstruction of the lacrimal ducts- can occur following any
condition causing cicatricing conjunctivitis. ( trachoma,
ocp, erythema multiforme, sjs, chemical and thermal
burns)
Mechanisms:
-Obstruction of the ducts of the main palpebral and accessory
lacrimal glands leads to aqueous-deficient dry eye.
-Obstructive MGD.
-Lid deformity influences tear film spreading by
affecting lid apposition and dynamics.

Reflex hyposecretion
1. reflex sensory block- in conditions of ocular sensory loss : decreases reflex induced lacrimal secretion and reduces the blink rate. In addition there is loss of trophic support to the ocular surface due to deficient release of sub P / nerve growth factors.
CAUSES:
a. Infective
Herpes simplex keratitis
Herpes zoster ophthalmicus
b. Corneal surgery
Limbal incision (extra-capsular cataract extraction)
Keratoplasty
Refractive surgery
PRK
LASIK
RK

c. Neurotrophic Keratitis
d. Topical anaesthesia – decreases blink rate by about 30% and tear
secretion by 60-75%
e. Systemic medications
Beta blockers
Atropine-like drugs
f. Other causes
Chronic contact lens wear – hard and extended wear
Diabetes mellitus – (sensory or autonomic neuropathy or due to
microvascular changes in the lacrimal gland)
Aging


Evaporative dry eyeIntrinsic causes
Extrinsic causes
1. meibomian gland dysfunction
( posterior blepharitis)- mc
Causes include- acne rosacea,
seborrheic dermatitis, atopic
dermatitis, treatment of acne with
isotretinoin.
Simple/ Cicatricial
Shine and McCulley
have shown that constitutional
differences in meibomian lipid
composition exist in different
individuals.
1. ocular surface diseases- imperfect
surface wetting, early tear film
breakup, tear hyperosmolarity, and
dry eye.
a. vit A deficiency- Vit A is essential for
development of goblet cells and
expression of mucins. Its deficiency
can also lead to lacrimal acinar
damage.
b. topical drugs and preservatives ( BAC)-
causes expression of inflammatory
cell markers leading to epithelial cell
damage, apoptosis and goblet cell
loss

In subjects with high levels of
cholesterol esters , esterases and
lipases produced by normal lid
commensals release ffa’s and
glycerides into the tear film which act
as source of iritation or soap
formation-“meibomian foam”.
Therefore there is loss of the normal
tear film phospholipids and chol
esters which leads to evaporation. In
blepharitis these commensals are
increased in no.
2. disorders of lid aperture and lid/
globe congruity-
ectropion, entropion, lagophthalmos,
eyelid coloboma, proptosis
2. Contact lens wear – 50%
correlation between hydration of CL and dry
eye symptoms is controversial.
3. Allergic conjunctivitis-
include
seasonal allergic conjunctivitis, vernal
keratoconjunctivitis, and atopic
keratoconjunctivitis
- release of inflammatory cytokines lead to loss
of cell surface mucins.
- surface irregularities on the cornea and
conjunctiva lead to tear film instability .
- In chronic disease, MGD occurs.

3. low blink rate-
Physiological / extrapyramidal disorders (parkinson’s)
- Lid swelling can interfere with lid apposition and tear film spreading
- Use of antihistaminics also contribute to dry eye.

CAUSATIVE MECHANISM OF DRY EYE

Reflex tear secretion is the initial compensatory mechanism in
response to the ocular irritation but with time the chronic inflammation
leads to decrease in corneal sensation which compromises the reflex
response and leads to an even greater tear film instability.
Ocular protection index-
TFBUT divided by Inter-blink interval (IBI)
If the OPI is <1.0, the patient has an exposed ocular surface, putting them
at risk for the development of the signs and symptoms of dry eye,
whereas if the OPI is ≥1.0, the patient's ocular surface is tear film
protected. The OPI has proven to be useful in assessing the factors
that may cause or exacerbate dry eye.


CLINICAL FEATURES Symptoms-
Most common symptoms include FB sensation, burning, itching, dryness,
soreness, heavy lids, photophobia, ocular fatigue and reflex tearing.
These symptoms characteristically worsen during the day.
Stringy discharge, crusting of lids and transient blurring of vision can also occur.
A history of exacerbation by reading, computer use, or in windy environment is
often elicited.
Enquire about contact lens use, ocular allergy, infections, and eyelid, corneal and
prior refractive surgery.
Medical history includes presence of any CTD/ autoimmune disease, DM, thyroid
eye disease, parkinson’s, sarcoidosis, Bells’s palsy, bone marrow transplant,
periorbital radiation or cranial tumors.

Signs
External observation of the face for acne rosacea.
Lids and lashes- examined for lagophthalmos, infrequent blinking, floppy
eyelids, lid retraction, ectropion, entropion, notching, trichiasis, distichiasis.
Lid margins- observation of meibomian gland architecture and openings,
presence of blepharitis, telangiectasia, scurf and position and siza of lacrimal
puncta. Enlargement of lacrimal gland is checked.
Function of 5th and 7th cranial nerve has to be checked.
Conjunctiva- may show mild redness and keratinization.
Tear film- marginal tear meniscus, presence of foam or debris suggestive of
MGD. In the dry eye, lipid contaminated mucin accumulates in the tear film
as particles and debris that move with each blink.



Cornea-
a. Punctate epithelial erosions in the interpalpebral and inferior cornea.
b. Mucus filaments- stain with rose bengal
c. Mucus plaques- composed of mucus, epithelial cells, proteinaceous and lipoidal material.


TESTS USED TO DIAGNOSE AND MONITOR DRY EYE DISEASE The tests measure the following
parameters- A. tear film stability – Break up time B. tear production – Schirmer test,
Fluorescein Clearance,
Tear osmolarity C. Ocular surface disease – corneal /
conjunctival stains and impression cytology

TFBUT: it is the interval between the last complete blink and the
appearance of the first randomly distributed dry spot. Flourescein 2% or a flourescein strip moistened with normal
saline is instilled in the lower fornix. The patient is asked to blink several times. Tear film is examined with broad beam in cobalt blue filter.
The time taken for the appearance of a dark spot is noted. The established cut off for diagnosing dry eye is < 10 sec.
however, few authors have suggested a cut off of < 5 sec when small volume of fluorescein is instilled.
Abnormal in ADDE and MGD Fluorescein BUT has important limitations. Touching of the
filter paper strip to the conjunctiva can stimulate reflex tearing.


The Non-Invasive Tear Film Break-up Time Test
They are called Non Invasive because the eye is not touched.
Instruments such as a keratometer, hand-held keratoscope or Tearscope
are required to measure NIBUT. A prerupture phase that precedes actual
break up of the tear film can also be observed with some techniques.
This pre-rupture phase is termed Tear Thinning Time (TTT).
Measurement is achieved by observing the distortion (TTT) and/or break
up (NIBUT) of a keratometer mire (the reflected image of keratometer
grid). The clinician focuses and views the crisp mires, and then records
the time taken for the mire image to distort (TTT) and/or break up
(NIBUT). NIBUT measurements are longer than fluorescein break up
time. NIBUT values of less than 15 seconds are consistent with dry eyes.
TTT / NIBUT are considered to be more patient-friendly, repeatable and
precise.

Schirmer Test- Assesses the aqueous tear production.
No. 41 Whatmann filter paper is placed in the lower fornix for 5
min and the amount of wetting is seen. The patient is instructed to
look forward and to blink normally during the course of the test. A
negative test (more than 10 mm wetting of the filter paper in 5
minutes) means normal quantity of tears. Patients with dry eyes
have wetting values of less than 5 mm in 5 minutes.
Its main utility is in diagnosing patients with severe dry eyes. Schirmer 1- is done without anaesthesia so it measures the basal
and the reflex secretion. Schirmer 2- measures the basal secretion- after putting anaesthetic
Abnormal- <10mm without anaesthesia , for diagnosis- <5 mm
<6mm with anaesthesia Sensitivity is poor : 10%- 25%

Many clinicians regard the Schirmer test as unduly invasive and
of little value for mild to moderate dry eyes. Other less invasive
methods to assess the adequacy of tear production have been
developed. The Phenol red thread test is one such test . A
cotton thread impregnated with phenol red dye is used. Phenol
red is pH sensitive and changes from yellow to red when wetted
by tears. The crimped end of a 70mm long thread is placed in the
lower conjunctival fornix. After 15 seconds, the length of the color
change on the thread - indicating the length of the thread wetted
by the tears -is measured in millimeters. Wetting lengths should
normally be between 9mm and 20mm. Patients with dry eyes
have wetting values of less than 9 mm.


Flourescein clearance test
5 microliter of fluorescein is placed on the ocular surface and the
residual dye is measured in a schirmer strip placed on the lower lateral
margin at intervals of 1, 10, 20, 30 minutes. At the end of the 30 min,
i.e., the last test, Schirmer strip is inserted after nasal stimulation.The
presence of flourescein on each strip is compared to a standard scale
or measured using flourophotometry. In normal eyes the value will have
fallen to zero after 20 minutes. Delayed clearance is observed in all dry
eye states.
It allows one to determine the basal tear secretion, reflex tear
secretion under nasal stimulation, and tear clearance, at the same
time.

ATD- aq tear deficiency

DTC- delayed tear clearnce


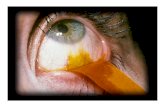
Vital staining-
A. Flourescein- synthesised by Baeyer in 1871
the intact corneal epithelium because of its high lipid content
resists penetration of water soluble flourescein and so is not
stained by it. Any break in the epithelial barrier permits rapid
penetration leading to staining of the areas with denuded
epithelium.
B. Rose bengal stain- :
1% liquid rose bengal is instilled into the eye. The examiner
uses white light to assess the amount of staining.

VAN BIIJSTERVELD SCORINGIntensity scored in 2 exposed conjunctival zones and corneaScore 0-3 for each zone. 0 for absent, 1 for just present, 2 for moderate staining and 3 for gross staining.Maximum score 9.Score more than 3.5 was considered abnormal.Rose bengal stains the dead or devitalized epithelial layer which have lost or altered mucous layer.

C. Lissamine green- similar to rose bengal but much less irritating.

Tear lysozyme levels- lysozyme is produced by the main and accessory lacrimal gland. It represents 20% of the protein content in tears. Its levels are decreased in early stages of dry eye.
Tear lactoferrin levels- it is also secreted by the lacrimal gland. Levels are decresed in dry eye. Immunoassay kits are available to measure its levels. Like ‘LACTOPLATE’
It is a plate containing gel loaded with rabbit anti-human-lactoferrin antiserum. Tear-moistened filter paper discs containing lactoferrin were placed on the gel. The lactoferrin concentration could be determined by measuring the concentric ring of precipitate after 72 hours incubation at room temperature.

Tear film osmolarity- the recommended cut
off value is 316 mosm/ l (overall predictive
accuracy of 89% for the diagnosis). In the
past it has been offered as a gold standard in
dry eye diagnosis, but its general utility is
hindered because it needs expert technical
support, available in only a small no of
specialized laboratories.

Impression cytology
It is a non invasive technique of collection of the most superficial layers of the
ocular surface by applying different collecting device (usually nitrocellulose filter
papers) so that cells adherent to that surface are subsequently removed from
the tissue and further processed.
It was first introduced in 1977 by Egbert et al.
1. A piece of filter paper is applied to the conjunctival surface for approximately 2-
5 seconds.
2. The filter paper is removed from the conjunctiva in a peeling motion to ensure
maximal collection of surface cells.
3. The cells are fixed using fixatives like formaldehyde , glutaraldehyde, ethanol
and methanol.

4. The cells that are adherent to the filter paper are stained to enhance
the visibility of the goblet cells with counter staining of the epithelial
cells to increase the contrast of the goblet cells.
5. The specimen is examined under a light microscope and various
analyses of the visible cells are conducted.

NELSON’S GRADINGGrade 0: small round epithelial cells with a eosinophilic staining
cytoplasm, large basophilic nuclei with an n/c ratio of 1:2, abundant goblet cells( >5oo cells/mm2)
Grade 1: Slightly larger and more polygonal cells , smaller nuclei,with n/c ratio of 1:3 , goblet cells are reduced in number (350-500 cells/mm2), preserved plump , with an intensely oval shape PAS positive cytoplasm.
Grade 2: even larger& polygonal epithelial cells, occasionally multinucleated with variable staining cytoplasm, small nuclei with n/c ratio 1:4- 1:5, goblet cells markedly decreased in number (100-150 cells mm2) , smaller and less intensely PAS positive.
Grade 3: large &polygonal with basophilic staining cytoplasm small pyknotic nuclei ,occasionly completely absent,n/c ratio >1:6, very few goblet cells(100 cells/mm2).

Squamous metaplasia involves 3 major steps- loss of
goblet cells, increase in cellular stratification and
keratinization
Stages-
Stage0- normal cellular structure
Stage 1 – partial loss of goblet cell, no keratinization
Stage 2- total loss of goblet cells, increase in sixe of epithelial
cells
Stage 3- early and mild keratinization
Stage 4 – moderate keratinization
Stage 5- advanced keratinization

TREATMENT A. tear supplementation- Lubricants
B. tear retention- 1. punctal occlusion
2. moisture chamber spectacles
3. Bandage Contact lenses
C. Tear stimulation- Secretagogues
D. biological tear substitutes- 1. serum
2. Salivary gland
autotransplantation
E. Anti- inflammatory therapy- 1. cyclosporine
2. Corticosteroids
3. tetracyclines
F. essential fatty acids
G. environmental strategies

The foremost objectives in caring for patients with
dry eye disease are to improve the patient’s
ocular comfort and quality of life, and to return
the ocular surface and tear film to the normal
homeostatic state. Although symptoms can
rarely be eliminated, they can often be
improved, leading to an improvement in the
quality of life.

lubricants The term artificial tears is a misnomer as they do not mimic the
composition of human tears. Most of them function only as
lubricants. Few recent ones mimic the electrolyte composition of
tears.
The ideal artificial lubricant should be preservative-free, contain
potassium, bicarbonate, and other electrolytes and have a
polymeric system to increase its retention time.
The main variables in the formulation of ocular lubricants regard the
concentration of and choice of electrolytes, the osmolarity and the
type of viscosity/polymeric system, the presence or absence of
preservative, and, if present, the type of preservative.

A. Electrolyte composition- solutions containing electrolytes/ ions
have been shown to be beneficial in treating ocular surface damage
due to dry eye. Potassium and bicarbonate are most critical.
Potassium is important to maintain corneal thickness, and bicarbonate
promotes recovery of the epithelial barrier function and helps in
maintaining the normal epithelial ultrastructure. ( hypotears ,
genteel eye drops)
B. Osmolarity- since the tear film in patients with dry eye is
hyperosmolar, these lubricants should be hypo-osmolar but with a
high colloidal osmolality. so compatible solutes like glycerin,
erythritol and levocarnitine.

C. Viscosity agents- macromolecule complexes added to lubricants
act as viscosity agents. They increase the residence time, incresing
the duration of action and penetration of the drug. Viscous agents
also protect the ocular surface epithelium. Eg. CMC (mc), HPMC,
HMC, polyvinyl alcohol, PEG, glycol 400, propylene glycol. Highly
viscous agents have the disadvantage that they cause blurring of
vision and caking and drying on eyelashes. Lower molecular wt
viscous agents help to minimize these problems. ( Systane contains
HP- Guar which is a gelling agent containing glycol 400 and
propylene glycol.) Hyaluronic acid has also been tried as a viscosity
agent.

D. Preservatives- particularly BAK and disodium EDTA. Most
commonly used preservative in eye drops is BAK. It has been
found that its excessive use excites the inflammatory cell
markers like HLA-DR and ICAM 1 and causes epithelial cell
damage, apoptosis and decrease in goblet cell density.
Therefore leading to decrease in mucin- MUC 5A. The toxicity
is related to its concentration, frequency of dosing and the
severity of dry eye. In mild dry eye it can be well tolerated
even if used 4-6 times a day but in mod- sev dry eye potential
for toxicity is high due to decreased tear secretion and
decreased turnover.

Less toxic preservatives are now used more frequently.
Like polyquad, Na chlorite( purite), Na perborate.
These are ‘vanishing’ preservatives. < Na chlorite - Na
and Cl on exposure to UV light, Na perborate- water
and oxygen on contact with tear film. >
Ointments and gels have a longer retention time as
compared to artificial tears.

Punctal occlusion It is of greatest value in patients with mod- sev KCS who have not responded
to topical treatment. Introduced by Beetham in 1935, he used electrocautery.
1. temporary occlusion- by inserting collagen plugs into the canaliculi that
dissolve in 1-2 wks. If patient is asymptomatic after 1-2 weeks permanent
occlusion can be done.
2. reversible occlusion- by inserting silicon or long lasting collagen plugs that
dissolve in 2-6 months. They include – FREEMAN silicon plug which is
dumbbell shaped and a HERRICK plug which is shaped like a golf tee.
3. permanent occlusion- is done in patients with severe dry with repeated
schirmer’s test value less than 5 mm. it is done by coagulating the proximal
canaliculus with cautery, either thermal coagulation or diode laser cautery.

FREEMAN SILICON PLUG
HERRICK’S INTRA CANALICULAR PLUG

Beneficial outcome has been reported in 74-86% patients treated
with punctal plugs.
Contraindications-
1. allergy to the materials used
2. punctal ectropion
3. pre existing NLD block
4. patients with clinical ocular surface inflammation
5. infection of lacrimal canaliculus or sac
Complications-
1. spontaneous extrusion – mc , particularly with freeman style (50%)
2. internal migration of the plug
3. biofilm formation and infection and pyogenic granuloma

Moisture chamber spectacles
Tsubota et al reported an increase in periocular humidity in
subjects wearing these spectacles.

Bandage Contact lenses
They help to protect and hydrate the corneal surface in severe dry eye conditions. Silicone rubber lenses and gas permeable scleral bearing hard contact lenses can be used.

Tear stimulation- secretagogues
They increase the aqueous secretion or mucin
production or both.
These agents are currently under investigation
They include- diquafosol, rebamipide,
gefarnate, ecabet sodium, 15- HETE.
Cholinergic agonists- pilocarpine ( 5 mg qid) ,
cevimeline

Biological tear substitutes Include serum or saliva.
They maintain the morphology and support the proliferation of
primary corneal epithelial cells better than tear substitues.
Serum has been used in the concentration ranging from 20% to
100%. The efficacy is dose dependant. It is not FDA approved as
yet.
Salivary gland autotransplantation can be done. But since saliva
is hypo osmolar as compared to tears it can lead to microcystic
corneal edema. Therefore this is indicated only in end stage dry
eye disease, with schirmer test value </=1 mm, conjunctivalized
surface epithelium and persistent severe pain despite punctal
occlusion and hourly application of unpreserved lubricating drops.


Anti inflammatory therapy Hyperosmolarity of tear film is pro -inflammatory. Inflammation
leads to ocular surface disease. So, anti inflammatory agents have
been evaluated for use in dry eye. These include-
a. cyclosporin
b. corticosteroids
c. tetracycline
Cyclosporin is used in the concentration of 0.1% or 0.05%. Treated
eyes had approximately 200% increase in conjunctival goblet cell
density. It is used in moderate to severe aqueous deficiency. Most
common side effect includes burning on instillation. Other is
conjunctival hyperemia. Therapeutic benefit is achieved in about a
month.

Corticosteroids have been reported to decrease ocular
irritation, decrease corneal fluorescein staining and
improve filamentary keratitis. Low dose steroid therapy
can be used for short term (2 weeks) to suppress
discomfort and epithelial disease secondary to
inflammation. It is usually used along with or before
starting cyclosporin therapy.

TETRACYCLINES- they are attributed to have anti- bacterial
properties ( therefore decreasing the bacteria producing lipases) ,
anti- inflammatory properties( by decreasing wbc chemotaxis and
phagocytosis and also decreasing the activity of collagenase,
phospholipase , MMP’s and decreasing the production of IL-1 and
TNF alpha) and anti- angiogenic properties.
They are therefore indicated in-
Acne rosacea
Posterior blepharitis – 100 mg doxycycline is given BD for the first
week and then OD for 6-12 weeks. Some studies have suggested
equal improvement with even 20 mg BD for 1-2 months.

Essential fatty acids Omega 6 fatty acids are precursors of arachidonic acid
and certain pro-inflammatory lipid mediators ( PGE2,
LTB4), whereas omega 3 fatty acids found in fish oil
( also in walnuts, flax seeds, soyabean, tofu) inhibit the
synthesis f these lipid mediators and block the
production of IL 1 and TNF alpha. So they have been
found to decrease the incidence of dry eye.

DRY EYE SEVERITY
1 2 3 4
DISCOMFORT Mild or episodic Under env stress
Moderate episodic or chronic
Severe frequent or constant
Severe, disabling
Visual symptoms
None or episodic
Annoying episodic
Chronic / constant
Constant, disabling
Conj. injection None- mild None-mild +/- +/++
Conj. staining None-mild variable Moderate- marked
marked
Corneal staining None-mild variable Marked central Severe punctate erosions
Corneal/ tear signs
None- mild Mild debris, decrease meniscus
Filamentary keratitis, mucus clumping, inc tear debris
Fil. Keratitis, mucus clumping, inc tear debris, ulcer
Lid/ meibomian glands
MGD +/- +/- frequent Trichiasis, keratinizn, symblepharon
TFBUT (sec) Variable </=10 </= 5 immediate
Schirmer score (mm/5 min)
Variable </=10 </= 5 </= 2

Treatment recommendations according to severity level
Level 1:
Education and environmental/dietary modifications
Elimination of offending systemic medications
Artificial tear substitutes, gels/ointments
Eye lid therapy
Level 2:
If Level 1 treatments are inadequate, add:
Anti-inflammatories
Tetracyclines (for meibomianitis, rosacea)
Punctal plugs
Secretogogues
Moisture chamber spectacles

Level 3:
If Level 2 treatments are inadequate, add:
Serum
Contact lenses
Permanent punctal occlusion
Level 4:
If Level 3 treatments are inadequate, add:
Systemic anti-inflammatory agents
Surgery (lid surgery, tarsorrhaphy; mucus
membrane, salivary gland, amniotic
membrane transplantation)








![Dr.Aghaie-management of dry eye [Read-Only]erc.mums.ac.ir/images/erc/eyecenter/Dr.aghaei.lacri.pdf · Dry Eye : treatment Dry eye /ocular surface disorder is : progressive , life-long](https://static.fdocuments.us/doc/165x107/5c5f186309d3f2515c8d2852/draghaie-management-of-dry-eye-read-onlyercmumsacirimageserceyecenterdr.jpg)