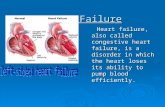
Drugs used in heart failure
-
Upload
mohammad-hadi-farjoo-md-phd -
Category
Health & Medicine
-
view
4.070 -
download
3
description
Transcript of Drugs used in heart failure

Drugs Used inHeart Failure
By
M.H.Farjoo M.D. , Ph.D.Shahid Beheshti University of Medical Science

Jan. 2007M.H.Farjoo
Drugs Used in Heart Failure
Introduction
Pathophysiology of Heart Failure
Cardiac Performance
Drugs Used In Heart Failure
Drug Pictures

Jan. 2007M.H.Farjoo
Introduction Heart failure occurs when cardiac output is
inadequate to provide the oxygen needed by the body.
The most common cause of heart failure is coronary artery disease.
Heart failure may be low output (more common) or high out put (rare)
In low output heart failure, cardiac output is below the normal range. Two major types exist: Systolic failure Diastolic failure

Jan. 2007M.H.Farjoo
Introduction Cont’d
Systolic failure: reduced cardiac output and reduced ejection fraction (<45%), is typical of acute failure (MI).
Diastolic failure: is a result of hypertrophy, stiffening and loss of adequate relaxation of the myocardium. Cardiac output is reduced but ejection fraction may be normal.
Heart failure due to diastolic dysfunction does not respond to positive inotropic drugs.

Jan. 2007M.H.Farjoo
Introduction Cont’d
High-output failure can result from hyperthyroidism, beriberi, anemia, and arteriovenous shunts.
This form of failure should be treated by correcting the underlying cause.
The manisfestations of all types of heart failure include: tachycardia, decreased exercise tolerance, shortness of breath, peripheral and pulmonary edema, and cardiomegaly.

Jan. 2007M.H.Farjoo
Introduction Cont’d
The primary defect in early heart failure resides in the excitation-contraction coupling of the heart
Therapy directed at noncardiac targets is more valuable in the long-term treatment of heart failure than positive inotropic agents.
Positive inotropic drugs can be very helpful in acute failure. They also reduce symptoms in chronic failure.

Jan. 2007M.H.Farjoo
Normal Cardiac Contractility
Contraction results from the interaction of activator calcium (during systole) with the actin-troponin-tropomyosin system
The amount released depends on the amount stored in the SR and on the amount of trigger calcium during the plateau of the action potential.

Jan. 2007M.H.Farjoo
Normal Cardiac Contractility Cont’d
A. Sensitivity of the contractile proteins to calcium Levosimendan is the most recent example of a drug that
increases calcium sensitivity (it may also inhibit phosphodiesterase) and reduces symptoms in models of heart failure.
B. The amount of calcium released from the sarcoplasmic reticulum
C. The amount of calcium stored in the sarcoplasmic reticulum
D. The amount of trigger calcium

Jan. 2007M.H.Farjoo
Normal Cardiac Contractility Cont’d
E. Activity of the sodium-calcium exchanger This antiporter uses the sodium gradient to move calcium
against its concentration gradient from the cytoplasm to the extracellular space.
The sodium-calcium exchanger's ability to carry out this transport is thus strongly dependent on the intracellular concentrations of both ions, especially sodium.
F. Intracellular sodium concentration and activity of Na+/k+ ATPase Na+/k+ ATPase, by removing intracellular sodium, is the
major determinant of sodium concentration in the cell.

Jan. 2007M.H.Farjoo
Pathophysiology of Heart Failure
Neurohumoral or extrinsic compensation involves two major mechanisms: The sympathetic nervous system Renin-angiotensin-aldosterone
The most important intrinsic compensatory mechanism is myocardial hypertrophy.


Jan. 2007M.H.Farjoo
Pathophysiology of Heart Failure Cont’d
The baroreceptor reflex is reset, with a lower sensitivity to arterial pressure in heart failure.
baroreceptor sensory input to the vasomotor center is reduced even at normal pressures; and sympathetic outflow is increased.
Remodeling is changes that occur in the stressed myocardium.
It includes proliferation of connective tissue and abnormal myocardial cells.

Jan. 2007M.H.Farjoo
Pathophysiology of Heart Failure Cont’d
The severity of heart failure. Class I failure: no limitations on ordinary activities and
symptoms that occur only with greater than ordinary exercise.
Class II: slight limitation of ordinary activities, which result in fatigue and palpitations with ordinary physical activity.
Class III: no symptoms at rest, but fatigue, etc, with less than ordinary physical activity.
Class IV: symptoms even when the patient is at rest.

Jan. 2007M.H.Farjoo
Cardiac Performance
Cardiac performance is a function of four primary factors: Preload
Afterload
Contractility
Heart rate

Jan. 2007M.H.Farjoo
Preload
Increased filling pressure increases oxygen demand. Preloads greater than 20-25 mm hg result in
pulmonary congestion. Preload is usually increased in heart failure because
of increased blood volume and venous tone. Reduction of filling pressure is the goal of salt
restriction and diuretic therapy in heart failure. Venodilator drugs (nitroglycerin) reduce preload by
redistributing blood into peripheral veins.


Jan. 2007M.H.Farjoo
Afterload
Afterload is the resistance against which the heart must pump blood: aortic impedance and systemic vascular resistance.
In chronic failure, there is a reflex increase in systemic vascular resistance (by sympathetic outflow and the renin-angiotensin system).
Endothelin, a potent vasoconstrictor peptide, may also be involved.
This sets the stage for the use of drugs that reduce arteriolar tone in heart failure.

Jan. 2007M.H.Farjoo
Contractility
Biopsy from failed hearts shows a reduction in intrinsic contractility.
As contractility decreases, there is a reduction in the velocity of muscle shortening, the rate of intraventricular pressure development (dP/dt), and the stroke output achieved.
The heart is still capable of some increase in all of these measures of contractility in response to inotropic drugs.

Jan. 2007M.H.Farjoo
Heart rate
Heart rate is a major determinant of cardiac output.
As the function of the heart decreases in failure, an increase in heart rate is the first compensatory mechanism.

Jan. 2007M.H.Farjoo
Drugs Used In Heart Failure Digitalis Other positive inotropic drugs:
Bipyridines β stimulants
Drugs without positive inotropic effects: Diuretics ACE inhibitors & angiotensin receptor blockers Vasodilators β blockers

Jan. 2007M.H.Farjoo
Digitalis
All of the cardiac glycosides, or cardenolides of which digoxin is the prototype combine a steroid nucleus.
They are extract of many common plants: Digitalis purpurea (Red foxglove) Digitalis lutea Convallaria majalis (Lily of the valley) Helleborus niger (Christmas rose)



Digitalis purpurea (Red foxglove)

Digitalis purpurea (Red foxglove)

Digitalis purpurea (Red foxglove)

Digitalis Lutea

convallaria majalis (Lily of the valley)

convallaria majalis (Lily of the valley)

helleborus niger (Christmas rose)

helleborus niger (Christmas rose)

helleborus niger (Christmas rose)

helleborus niger (Christmas rose)

helleborus niger (Christmas rose)

Jan. 2007M.H.Farjoo
Digoxin
Digoxin is obtained from Digitalis lanata (white foxglove).
It inhibits Na+/K+ ATPase (the sodium pump).
Cardiac effects Mechanical effects Electrical effects
Effects on other organs
Interactions with K+, Ca2+ and Mg2+
Digoxin Toxicity

Digitalis Lanata

Digitalis Lanata






Jan. 2007M.H.Farjoo
Mechanical effects
Cardiac glycosides increase contractility of the cardiac sarcomere by increasing the intracellular calcium concentration
This effect occurs in both normal and failing myocardium.
The responses are modified by cardiovascular reflexes and the pathophysiology of heart failure.

Jan. 2007M.H.Farjoo
Electrical Effects
At first action potential duration decreases which is the result of increased potassium conductance due to increased intracellular calcium.
At higher concentrations, resting membrane potential is made less negative due to inhibition of the sodium pump.
As toxicity progresses, afterpotentials ”delayed afterdepolarizations, DADs” appear due to overloading of the intracellular calcium stores.

Jan. 2007M.H.Farjoo
Electrical Effects Cont’d
DADs may elicit premature depolarizations or “ectopic beats” that are coupled to the preceding normal action potentials.
If DADs in the Purkinje system regularly reach threshold, bigeminy will be recorded on the ECG.
With further intoxication, each DAD-evoked action potential will itself elicit an afterpotential, and a self-sustaining tachycardia will be established.
Such a tachycardia may deteriorate into fibrillation; in the case of V.fib. it will be rapidly fatal unless corrected.

Digitalis-induced bigeminy:
NSR: normal sinus rhythm
PVB: premature ventricular beats


Jan. 2007M.H.Farjoo
Electrical Effects Cont’d
In the low dose, cardiac parasympathomimetic effects predominate which account for early electrical effects of digitalis.
Because cholinergic innervation is much richer in the atria, these actions predominantly affect atrial and AV nodal function.
At toxic levels, sympathetic outflow is increased which sensitizes the myocardium and exaggerates all the toxic effects of the drug.
The most common arrhythmias of digitalis toxicity include AV junctional rhythm, PVC, bigeminal rhythm, and second-degree AV blockade but any arrhythmia may be induced.



Jan. 2007M.H.Farjoo
Effects On Other Organs
The GI tract is the most common extra cardiac site of digitalis toxicity. It causes anorexia, nausea, vomiting, and diarrhea.
Central nervous system effects include vagal and CTZ stimulation.
In the elderly disorientation, hallucinations and visual disturbances (as color misperception) may occur.


Jan. 2007M.H.Farjoo
Interactions With K+, Ca2+, Mg2+
Potassium and digitalis inhibit each other's binding to Na+/K+ ATPase
Hyperkalemia reduces the enzyme-inhibiting actions of cardiac glycosides, whereas hypokalemia facilitates these actions.
Abnormal automaticity is inhibited by hyperkalemia. Moderately increased extracellular K+ therefore reduces the (toxic) effects of digitalis.

Jan. 2007M.H.Farjoo
Interactions With K+, Ca2+, Mg2+ Cont’d
Ca2+ facilitates the toxic actions of cardiac glycosides by accelerating the overloading of intracellular calcium stores.
Hypercalcemia increases the risk of a digitalis induced arrhythmia.
The effects of Mg2+ is opposite to those of calcium.
These interactions mandate evaluation of serum electrolytes in digitalis-induced arrhythmias.

Jan. 2007M.H.Farjoo
Digoxin Toxicity
Toxic effects may occur before the therapeutic end point is detected.
Serum digitalis, K+ levels and ECG should be monitored during therapy of digitalis toxicity.
If digitalis is being loaded slowly, simple omission of one dose and halving the maintenance dose often suffices.
In severe intoxication, serum K+ is already elevated, automaticity is depressed, and antiarrhythmic agents may lead to cardiac arrest.

Jan. 2007M.H.Farjoo
Digoxin Toxicity Cont’d
Digitalis-induced arrhythmias are made worse by cardioversion; this therapy should be reserved for V.Fib. If it is glycoside-induced.
Treatment is prompt insertion of a pacemaker and administration of digitalis antibodies (digoxin immune fab).
These antibodies recognize all cardiac glycosides in addition to digoxin.

Jan. 2007M.H.Farjoo
Bipyridines
Bipyridines that inhibit phosphodiesterases, are used in heart failure.
Inhibition of phosphodiesterase increases cAMP and increases contractility and vasodilation.
The bipyridines increase myocardial contractility by increasing inward calcium flux in the heart during the action potential.

Jan. 2007M.H.Farjoo
Bipyridines Cont’d
Although they have positive inotropic effects, most of their benefits derive from vasodilation.
Two successful bipyridines are: Inamrinone and Milrinone.
Inamrinone and milrinone are used only for acute heart failure or severe exacerbation of chronic heart failure.

Jan. 2007M.H.Farjoo
β Stimulants
Dobutamine (selective β1 agonist) has been widely used in heart failure.
It increases cardiac output together with a decrease in ventricular filling pressure.
Tachycardia may occur so angina or arrhythmias must be considered in patients with CAD.
Tachyphylaxis may be seen with any β-stimulant.
Dopamine is also used in acute heart failure and is helpful if blood pressure should be raised.

Jan. 2007M.H.Farjoo
Diuretics
They reduce venous pressure and ventricular preload.
This results in reduction of edema and cardiac size, which improves pump efficiency.
Aldosterone may cause myocardial and vascular fibrosis and baroreceptor dysfunction in addition to its renal effects.
For this reason the aldosterone antagonists, spironolactone and eplerenone, decrease morbidity and mortality in severe heart failure.

Jan. 2007M.H.Farjoo
ACE Inhibitors & ARBs
These drugs reduce peripheral resistance and afterload.
They also reduce salt and water retention and in that way reduce preload.
The reduction in tissue angiotensin also reduces sympathetic activity.
These drugs reduce the long-term remodeling of the heart and vessels.


Jan. 2007M.H.Farjoo
Vasodilators
The vasodilators are effective in acute heart failure.
They reduce preload (venodilation), or afterload (arteriolar dilation), or both.
Long-term use of hydralazine and isosorbide dinitrate can also reduce damaging remodeling of the heart.
Bosentan, an inhibitor of endothelin, is used in pulmonary hypertension. It has significant teratogenic and hepatotoxic effects.


Jan. 2007M.H.Farjoo
β Blockers
Most patients respond favorably to CERTAIN β-blockers.
These drugs can cause acute decompensation of cardiac function.
Bisoprolol, Carvedilol, and Metoprolol showed a reduction in mortality.
This effect was not observed with another β blocker, Bucindolol.

Jan. 2007M.H.Farjoo
Clinical Pharmacology
Diuretics are first-line therapy.
Digitalis is reserved for patients who do not respond adequately to diuretics, ace inhibitors, and β blockers.

Jan. 2007M.H.Farjoo
Clinical Pharmacology Cont’d
Steps in the treatment of chronic heart failure. 1. Reduce workload of the heart
A. Limit activity, put on bed rest B. Reduce weight C. Control hypertension
2. Restrict sodium intake
3. Restrict water (rarely required)
4. Give diuretics

Jan. 2007M.H.Farjoo
Clinical Pharmacology Cont’d
5. Give ACE inhibitor or angiotensin receptor blocker
6. Give digitalis if systolic dysfunction with 3rd heart sound or atrial fibrillation is present
7. Give β blockers to patients with stable class II-IV heart failure
8. Give vasodilators
9. Cardiac resynchronization if wide QRS interval is present in normal sinus rhythm

Jan. 2007M.H.Farjoo
Sodium Removal
In mild failure, start with a thiazide diuretic, switching to furosemide as required.
Hypokalemia can be treated with potassium supplementation or through the addition of an ACE inhibitor or a potassium-sparing diuretic.
Spironolactone or eplerenone should be considered in all patients with moderate or severe heart failure.
Serum potassium should be monitored in patients receiving any of these agents.

Jan. 2007M.H.Farjoo
ACE Inhibitors & ARBs
In patients with left ventricular dysfunction but no edema, an ACE inhibitor should be used first.
ACE inhibitors are superior to vasodilators and must be considered, along with diuretics, as first-line therapy for chronic failure.
ACE inhibitors cannot replace digoxin in patients already receiving that drug.
ACE inhibitors are beneficial in asymptomatic patients to those with severe chronic failure.
ARBs (losartan, candesartan) should only be used in patients who are intolerant of ACE inhibitors (usually because of cough).

Jan. 2007M.H.Farjoo
Vasodilators
The ACE inhibitors are nonselective arteriolar and venous dilators.
The choice of agent should be based on the patient status and hemodynamic measurements.
Poor response to other therapy usually involves both elevated filling pressures and reduced cardiac output.

Jan. 2007M.H.Farjoo
β Blockers & Ca2+ Channel Blockers
Such therapy is beneficial if initiated very cautiously at low doses.
Acutely blocking the supportive effects of catecholamines can worsen heart failure.
Several months of therapy may be required before improvement is noted.

Jan. 2007M.H.Farjoo
Digitalis
Digoxin is indicated in patients with heart failure and atrial fibrillation.
It is also most helpful in patients with a dilated heart and third heart sound.
It is usually given only if diuretics and ACE inhibitors have failed to control symptoms.
Only 50% of patients with normal sinus rhythm benefit from digitalis.
When symptoms are mild, slow “digitalization” (0.125-0.25 mg/d) is safer and as effective as the rapid method (0.5-0.75 mg every 8 hours for 3 doses, followed by 0.125-0.25 mg/d).

Jan. 2007M.H.Farjoo
Digitalis
In atrial fibrillation, reduction of ventricular rate is the best measure of glycoside effect.
In normal sinus rhythm, symptomatic improvement and reductions in heart size and rate signify optimum drug levels.

Jan. 2007M.H.Farjoo
Digitalis
Digitalis reduces hospitalization and deaths from progressive heart failure at the expense of an increase in sudden death.
Digitalis is useful in the management of atrial arrhythmias because of its cardioselective parasympathomimetic effects but calcium channel blockers and adenosine are preferred for this application.
Digitalis should be avoided in the Wolff-Parkinson-White syndrome. it increases the conduction of atrial arrhythmia through the aberrant pathway.
It is explicitly contraindicated in patients with Wolff-Parkinson-White syndrome and atrial fibrillation.

Jan. 2007M.H.Farjoo
Acute Heart Failure
A common cause of acute failure is MI.
Patients with MI are treated with emergency revascularization using either coronary angioplasty and a stent or a thrombolytic agent.
Measurements of arterial pressure, cardiac output, stroke work index, and pulmonary capillary wedge pressure are useful in patients with MI and acute heart failure.
Such patients can be characterized on the basis of three hemodynamic measurements: arterial pressure, left ventricular filling pressure, and cardiac index.


Jan. 2007M.H.Farjoo
Acute Heart Failure Cont’d
Among patients with acute decompensation, a small subset is found to have hyponatremia, due to increased vasopressin activity.
A new V1a and V2 receptor antagonist, conivaptan, has recently been approved for the parenteral treatment of euvolemic hyponatremia.

Effects of a cardiac glycoside, ouabain, on isolated cardiac tissue. The top tracing shows action potentials evoked during the control period, early in the "therapeutic" phase, and later, when toxicity is present. The middle tracing shows the light (L) emitted by the calcium-detecting protein aequorin (relative to the maximum possible, Lmax) and is roughly proportionate to the free intracellular calcium concentration. The bottom tracing records the tension elicited by the action potentials. The early phase of ouabain action (A) shows a slight shortening of action potential and a marked increase in free intracellular calcium concentration and contractile tension. The toxic phase (B) is associated with depolarization of the resting potential, a marked shortening of the action potential, and the appearance of an oscillatory depolarization, calcium increment, and contraction (arrows)








If something‘s rotating – go home, you need a break!

SummaryIn English

Thank youAny question?