Dr ahmed esawy 6 bowel imaging chronic mesenteric ischemia cmi abdominal angina aa
-
Upload
ahmed-esawy -
Category
Health & Medicine
-
view
17 -
download
0
Transcript of Dr ahmed esawy 6 bowel imaging chronic mesenteric ischemia cmi abdominal angina aa


Dr. Ahmed Abdallah Eisawy
MBBS M.Sc MD

Chronic Mesenteric Ischemia
CMI
Abdominal Angina (AA)
Imaging

acute or chronic
arterial or venous
occlusive or non-occlusive

Coeliac Axis
Superior Mesenteric Artery
Inferior Mesenteric Artery

A_ foregut supply by ceiolic artery or trunk
B_midgut supply by superior mesenteric artery
C_ hind gut supply by inferior mesenteric artery


Coeliac Axis
Splenic Artery
Common
Hepatic
Artery
Left HA
Right HA
Left Gastric Artery
Gastro-
duodenal
Artery
Superior
Pancreatico-
duodenal
artery
Right Gastro-epiploic Artery

SMA
Inferior Pancreatico-duodenal Artery
Jejunal
Branch
Ileal Branch
Middle
Colic
Artery
Right Colic
Artery
Ileocolic
Artery

Left Colic Artery
Sigmoid
branches
Superior
Hemorrhoidal
artery
IMA

Pancreatico
-duodenal
arteries Marginal
artery of
Drummond &
paracolic
arcade
Reverse flow from
the internal iliac
artery

Abdominal Angina (AA)
CMI

It is a disorder characterized by the classical triad of:
Recurrent transient episodes of post-
prandial abdominal pain
Steatorrhoea with sever loss of weight
The patient’s avoidance of food
Patients present in their 50s or 60s
Male: Female = 1:3

Causes :
atherosclerosis
Arteritis.
Fibro-muscular hyperplasia.
Pressure on the coeliec artery by the crus of the diaphragm.

1. Plain : Normal or dilated loops.
2. Ba. :
Dilated loops with thick oedematous folds.
Thumb printing, fold thickening and separation of bowel loops.
CT:
Confirms bowel dilatation and wall thickening.
Show the thrombus in artery or vein.
Confirms the presence of air in the bowel wall and portal venous system.

Diagnostic
Interventional

I. Abdominal Imaging Plain Film Barium Studies Contrast material-enhanced CT Ultrasonography Magnetic resonance cholangiography
II. Imaging of Visceral Arteries Duplex Ultrasound CT angiography MR angiography Conventional angiography

US&DUPLEX

Normal Celiac Artery
Uniform velocities and
waveform configuration
High-diastolic flow feeding a
low resistance bed
No turbulence

PSV 150 cm/sec
EDV 20 cm/sec
IMA similar to SMA but high RI
CELIAC similar but high diastolic velocity

Normal spectral waveforms in the superior mesenteric artery. (a) Fasting waveform from a 26-day-old neonate shows a high-resistance flow pattern .
(b) Postprandial waveform
from a 6-day-old neonate
shows a low-resistance
pattern with an increase
in diastolic flow velocity .

Arises 1.5 cm below celiac
Just superior to renal arteries
LRV passes underneath SMA

ARISES FROM LEFT ,ANTERIOR ASPECT OF AORTA
JUST DISTAL TO ITS DIVISION
COURSES INFERIOR AND SLIGHT TO LEFT
MAY BE ONLY 1-3 MM IN DIAMETER

Uniform velocities and waveform configuration
Low diastolic feeding a high resistent bed vascular
In a fasting patient
No turbulence

Stenosis 70% or greater
PSV < 200 cm/sec
EDV < 55 cm/sec

High-grade stenosis at the origin of the celiac trunk and superior mesenteric artery in a patient with abdominal angor; pulsed Doppler measurements show peak velocities of over 250 cm/sec and turbulence

Stenosis 70% or greater
PSV < 275 cm/sec
EDV < 45 cm/sec
Focal increase in velocity
Post-stenotic turbulence

Stenosis 70% or greater
PSV < 200 cm/sec
EDV < 45 cm/sec
Focal increase in velocity
Post-stenotic turbulence

No detectable Doppler flow
Collateral pathways visualized
Increase in velocities may be noted in remaining patent
Splanchnic vessels

Accurate imaging modality used for screening of proximal coeliac & SMA.
Gives anatomic & functional information.
PSV > 275 and 200cm/s is highly specific for 70% artery stenosis
EDV > 45 cm/s is more accurate.

Spiral CT and rapid bolus injection of CM
Multidetector row CT provides more detailed information. 3D volume rendering and MIP imaging.


Takayasu SMA narrowing, Takayasu arteritis.

show high-grade stenoses at the origins of the celiac trunk and SMA.
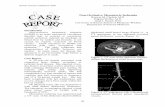
Abdominal CT scans show signs of bowel ischemia, with distended small bowel loops and wall thickening. Results of surgery performed the following day confirmed necrosis of the entire small bowel. The patient died the day after surgery.

Multi-detector row CT angiogram
shows a mildly stenotic celiac trunk
and a high-grade atherosclerotic
obstruction of the SMA. The IMA is not
seen
SMA
Digital subtraction angiogram (DSA)

Typical CT angiographic appearance of AA: phase 2—treatment planning (same patient as in ). (a, b) Paraaxial (a) and parasagittal (b) curved MPR images allow evaluation of vessel diameter at the stenosis (line 1) and in the distal segment (line 2) of the SMA (7 mm). (c-e) Locations of the resulting orthogonal cuts are shown in c and d; e displays the length of the segment requiring percutaneous treatment (18 mm). The ostial diameter is not well assessed because of the proximity of the stenosis. The patient experienced relief from symptoms after placement of a balloon-expandable, 31-gauge stainless-steel 7 x 22-mm stent.


6 months after stent placement to assess patency show that the stent is correctly positioned,

Percutaneous treatment of AA with twin stent placement in the celiac trunk and SMA

Time of Flight MRA
PC MRA
2D ECG gated cine PC MRA
Systolic-gated 3D PC MRA
3D Gd-enhanced MRA

AP projection
Lateral
projection



With or without digital enhancement, provides the most information in defining the anatomy of splanchnic arteries.
Collateral vessels are best visualized on AP projections.
Lateral view is essential in establishing osteal narrowing.


1. Acute Mesenteric Ischemia
2. Retroperitoneal or coelio-mesenteric Malignancy
3. Median Arcuate ligament syndrome
4. Mesenteric venous thrombosis
5. Gastroduodenal Ulcer
6. Non-occlusive Vascular lesions: Aneurysms & dissections.

Percutaneous Transluminal Angioplasty (PTA)
In stenotic or short occlusive lesions & in patients at high surgical risk.
Revascularization is performed in only one obstructive lesion.
SMA revascularization should be attempted before that of CA.
Occlusion: fibrinolytic agents prior to passing catheter.
Stent placement.
Complications: haematoma, spasm & thrombosis, dissection and acute ischemia.


Doppler Ultrasound
PTA in suspected re-stenosis