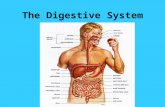
Digestive system 2 AND 3
-
Upload
helao-silas -
Category
Health & Medicine
-
view
257 -
download
0
Transcript of Digestive system 2 AND 3

Digestive System III
LiverGallbladderPancreas

Liver
occupies the upper right region of the abdominal cavity

Liver is the largest internal organ
is subdivided into two large lobes (right and left)two small lobes (quadrate and caudate)
is enclosed in a capsule (capsule of Glisson) is partially covered by the visceral peritoneum is associated with the gallbladder

Liver composition
Parenchyma - consists of epithelial cells - hepatocytes- arises from the endoderm
Stroma - consists of connective tissue trabeculae - contains blood and lymphatic vessels, nerves, and bile ducts- divides parenchyma into lobules

Connective tissue is poor-developed in the human liver
the human liver
connective tissue in the pig liver

Liver functions
Bile production – exocrine function
so-called “endocrine” functions

Liver is involved in many metabolic pathways
produces blood plasma proteins (albumins, prothrombin, fibrinogen,
nonimmune - and -globulins, etc.) stores the blood glucose as glycogen and
releases glucose back after glycogenolysis stores lipid-soluble vitamins – A, D, K synthesizes and stores cholesterol stores iron ions as ferritin or hemosiderin synthesizes urea from ammonium ions

Liver degrades drugs, toxins, alcohol, and hormones
Detoxication and degradation - occur in hepatocyte sER - include
oxidationconjugationconversation

Liver blood supply
Liver receives blood from two blood vessels the hepatic artery the portal vein
the liver hilum or porta hepatis

Portal vein carries the venous blood
from the digestive tract, spleen, and pancreas
portal blood contains– nutrients and toxic materials – erythrocyte breakdown products– hormones

Blood vessels pass in connective tissue with bile ducts
Triad (portal area) includes interlobular– artery– vein (from v. porta)– bile duct

Interlobular vessels give rise to capillaries
capillaries (hepatic sinusoids) – pass trough lobule– empty into the central vein

Hepatic sinusoids carry mixed blood
hepatic sinusoids

Central vein is a terminal venule
receives blood from sinusoids

Central vein begins the vinous blood outflow
a central vein the sublobular veins the hepatic vein the inferior vena cava

Hepatic lobules
are the liver morphofunctional units

Hepatic lobule composition
hepatocytes arranged in plates hepatic sinusoids perisinusoidal spaces (spaces of Disse) bile capillaries (canaliculi) central veins

Classic hepatic lobule
is a hexagonal mass of tissue a central vein is at the center the triads are at the angles
hepatic plates radiate from the center to periphery sinusoids travel between plates blood flows from the periphery towards the center bile flows from the center towards the periphery

Portal lobule emphasizes the liver exocrine function
is a triangular mass of tissue the central veins are at the angles the triad is at the center blood flows from the center to the periphery bile flows from the periphery to the center

Liver acinus
is a diamond-shaped mass of tissue the short axis is between the triads the long axis is between the central veins

Plates of hepatocytes
consist of two anastomosing cell rows bile canaliculus is between the rows are surrounded by the blood sinusoids
delicate network of the reticular fibers supports plates

Hepatocytes
are large polygonal cells contain 1 or 2 nuclei with several nucleoli may be tetraploid

Hepatocytes are rich in organelles
rER and sER mitochondria Golgi apparatus peroxisomes

Hepatocyte inclusions
glycogen clumps
lipid droplets

Hepatocyte polarization
Vascular pole- faces blood sinusoids- is involved in the “endocrine” function (blood-hepatocyte exchange)
Biliar pole - faces bile canaliculi- is involved in the exocrine function (bile secretion)

Hepatocytes are capable for regeneration
Physiologic regenerationhepatocyte lifespan is about 5 monthshepatocytes can be renewed
Reparative regenerationoccurs when liver substance is lost after trauma or surgery
undifferentiated cells are in the periportal areas

Bile canaliculi
are intercellular gaps within the hepatic plates

Bile canaliculi lack their own wall
are isolated by the hepatocyte tight junctions

Bile canaliculi empty into the bile duct
bile duct is a part of the triad

Bile duct is lined with cuboidal epithelial cells

Hepatic blood capillaries – hepatic sinusoids
are sinusoidal fenestrated and discontinuous
are lined with fenestrated endothelial cells

Hepatic sinusoids contain Kupffer cells
Kupffer cells are hepatic macrophages

Kupffer cells
belong to the mononuclear phagocytotic system
arise from blood monocytes
pit-cell is a large granulated lymphocyte

Kupffer cell functions
degradation of damaged or senile erythrocytes conversation ferritin to hemosiderin phagocytosis of bacteria and antigens initiation of immune reactions

Perisinusoidal space (space of Disse)
is between vascular hepatocyte pole and sinusoid contains a few reticular fibers and amorphous substance
hepatocytes project microvilli into space of Disse

Space of Disse is a site of
exchange between blood and hepatocytes hepatic lymph origination hemopoiesis in the fetal period and
in cases of chronic anemia in the adult

Space of Disse contains lipocytes (stellate or Ito cells)
are located between hepatocytes lack contact with bile canaliculi contain numerous lipid droplets

Lipocyte functions
storage of vitamin A synthesis of reticular fibers and amorphous substance
In pathology- lose their lipids and differentiate into myofibroblast-like cells- synthesize collagen fibers resulting in liver fibrosis - may contract resulting in portal hypertension

Gallbladder
is attached to the visceral surface of the liver

Gallbladder functions
bile storage bile concentration bile release to the duodenum as required

Bile takes part in digestion
emulsifies lipids activates pancreatic lipases facilitates fatty acid absorption
Bile composition:waterelectrolytesphospholipidscholesterolbile acidsbile pigments (bilirubin)

Gallbladder wall structure
Mucosa Mascularis externa Adventitia/Serosa

Gallbladder mucosa
epithelium lamina propria

Gallbladder epithelium
simple columnar striated
brush border

Hormone cholecystokinin regulates the bile injection
is produced by enteroendocrine cells of the duodenum is released in response to a fatty chyme induce the gallbladder muscle contractions

Pancreas
is located behind the stomach is enclosed in a capsule and
partially covered with serosa is subdivided into
headbodytail

Pancreas composition
Parenchyma - consists of epithelial cells - arises from the endoderm
Stroma - consists of connective tissue trabeculae - contains blood and lymphatic vessels, nerves, and ducts- divides parenchyma into lobules

Pancreas is mixed gland
Exocrine componentproduces pancreatic juice
Endocrine componentsecretes hormones

Exocrine pancreas
is compoundbranchedtubulo-alveolarserous (protein-producing) gland
main and accessory pancreatic ducts empty into the duodenum

Pancreatic secretory unit - acinus
is round with narrow lumen

Acinar cells
are pyramidal nuclei are round and centrally located broad basal portion is basophilic due to rER apical portion is acidophilic due to secretory (zymogen) granules

Acinar cell ultrastructure
zymogen granules in the apical pole
rER in the basal pole

Acinar cells secrete a variety of digestive enzymes
Trypsin, chymotrypsin, peptidases – digest proteins up to amino acids
Amylase – digests carbohydrates up to glucose
Lipases – digest lipids up to glycerol and fatty acids
Nucleases – digest nucleic acids up to nucleotides

Zymogen granules contain inactive enzymes
proenzymes are activated when reach the intestinal lumen

Exocrine pancreas duct system
Intercalated ducts Intralobular ducts Interlobular ducts
Main and accessory pancreatic ducts

Intercalated duct
is narrow tubule lined with squamous or cuboidal cells may begin within the acinus (compound acinus) its cells in the acinus are called centroacinar cells

Centroacinar cells exist in the compound acinus
but belong to the intercalated duct

Intercalated duct takes part in secretion
Adds watersodiumbicarbonate to the pancreatic juice
Intercalated duct secretion - neuyralizes acidic gastric chyme- establishes the optimal pH for pancreatic enzyme activity

Intralobular and interlobular ducts
are lined with simple cuboidal epithelium

Pancreas exocrine secretion hormonal regulation
Hormones of enteroendocrine cells from the duodenumpancreozymin stimulates acinar cells secretin stimulates intercalated duct cells
Pancreatic hormones insulin and VIP stimulate exocrine secretionglucagon and PP inhibit exocrine secretion

Pancreas exocrine secretion nervous regulation
parasympathetic fibers stimulate both acinar and duct cells

Endocrine pancreas
consists of pancreatic (Langerhans) islets
islets are scattered throughout the gland

Islet composition
endocrine cells fenestrated sinusoidal capillaries

Islet endocrine cell types
B cells A cells D cells D1cells PP cells

B cells constitute about 70% of the islet population
occupy the islet central portion secrete insulin

Insulin decreases blood glucose levels
Effects hepatocytes and skeletal muscles – stimulates uptake of glucose from circulation– activates glycogen synthesis
Effects the white adipose cells– stimulates uptake of glucose from circulation– stimulates glycerol synthesis– inhibits lipase activity

A cells constitute 15-20% of the islet population
occupy the islet periphery secrete glucagon

Glucagon increases blood glucose levels
Stimulates glucose release into the bloodstream glycogenolysis (breakdown of glycogen) gluconeogenesis (synthesis of glucose from amino acids) lipase and lipid mobilization in adipose cells

Insulin and glucagon are antagonists

D cells constitute about 5-10% of the islet population
occupy the islet periphery secrete stomatostatin
inhibits both insulin and glucagon secretioninhibits acinar cell

Minor cell types in pancreatic islets
D1 cells vasoactive intestinal peptide (VIP)– stimulates endocrine and exocrine pancreatic secretion– decreases blood pressure
PP cells pancreatic polypeptide– stimulates gastric chief cells– inhibits
bile secretionpancreatic juice productionintestinal motility

Regulation of the islet activity
Blood glucose levels increase stimulate insulin productiondecrease stimulate glucagon production
Nervous regulation parasympathetic fibers stimulate both insulin and glucagon secretionsympathetic fibers stimulate glucagon release but inhibit insulin secretion

The End
Thank you for attention!