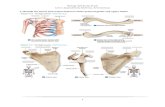
Diafise Clavicula
-
Upload
mvortopedia -
Category
Documents
-
view
216 -
download
0
Transcript of Diafise Clavicula

7/27/2019 Diafise Clavicula
http://slidepdf.com/reader/full/diafise-clavicula 1/10
A c u t e M i d s h a ft
C l a v i c u l a r F r a c t u r e
A b str a ct
Clavicular f ractures represent 2.6% to 5% of all f ractures, and
middle third f ractures account f or 69% to 82% of f ractures of the
clavicle. The junction of the outer and middle third is the thinnest
part of the bone and is the only area not protected by or reinf orced
with muscle and ligamentous attachments. These anatomic
f eatures mak e it prone to f racture, particularly with a f all on the
point of the shoulder, which results in an axial load to the clavicle.
Optimal treatment of nondisplaced or minimally displaced
midshaf t f racture is with a sling or f igure-of-8 dressing; the
nonunion rate is very low. However, when midshaf t clavicular
f ractures are completely displaced or comminuted, and when they
occur in elderly patients or f emales, the risk of nonunion, cosmetic
def ormity, and poor outcome may be mark edly higher. Thus, some
surgeons propose surgical stabilization of a complex midshaf t
clavicular f racture with either plate-and-screw f ixation or
intramedullary devices. Further randomized, prospective trials are
needed to provide better data on which to base treatment decisions.
The clavicle is one of the most
commonly f ractured bones; cla-
vicular f ractures represent 2.6% to
5% of all f ractures.1,2 The incidence
of clavicular f racture in adults is es-
timated to be 71 in 100,000 f or men
and 30 in 100,000 f or women, with
the incidence of midshaf t f ractures
decreasing with increasing age. Mid-
shaf t f ractures account f or 69% to
82% of all clavicular f ractures.1-5
Midshaf t f ractures are more common
in children and young adults. The in-
cidence of high-energy clavicular
f ractures with comminution, dis-
placement, and shortening appears to
be increasing.2
Traditionally, f ractures of the
clavicle have been treated with
closed reduction. More than 200
methods have been described f or
closed reduction, yet a classic text-
book recognizes that “reduction is
practically impossible to maintain,
and a certain amount of def ormity is
to be expected, generally compatible
with satisf actory return of f unction
in the shoulder.”6 The same text-
book states that even completely
displaced f ractures “generally do
well with non-operative manage-
ment....”6
However, most previous studies
describing the results of clavicular
f racture have used surgeon-based or
radiographic outcome measures that
equate union with success. Very f ew
studies on clavicular f racture have
been published using patient-based
outcomes such as the Medical Out-
comes Study 36-Item Short Form
(QualityMetric, Lincoln, RI) or the
Disabilities of the Arm, Shoulder
and Hand questionnaire (DASH; In-
stitute f or Work and Health, Toron-
ta, Canada, and the American Acad-
Kyle J. Jeray, MD
Dr. Jeray is Program D irec tor,
O rthopaedic Surgery Education,
G ree nvill e Hospital System, G ree nvill e,
S C .
Ne ither Dr. Jeray nor the department
with which he is aff ili ated has rec eived
anything of value from or owns stock in a
commercial company or institution
related direc tly or indirec tly to the
sub jec t of this article.
Re print requests: Dr. Jeray, G ree nvill e
Hospital System, University Me dica l
C enter, O rthopaedic Surge ry Education,
701 G rove Road, 2nd Floor E R C
Support Tower, G ree nvill e, SC 2 9 6 0 5.
J Am Acad O r t hop Su r g 2007;15 :23 9-
24 8
C opyright 2007 by the American
Academy of O rthopaedic Surgeons.
Volume 15 , Numbe r 4, Ap ril 2007 23 9

7/27/2019 Diafise Clavicula
http://slidepdf.com/reader/full/diafise-clavicula 2/10

7/27/2019 Diafise Clavicula
http://slidepdf.com/reader/full/diafise-clavicula 3/10
that a direct in jury f rom the shoul-
der (rather than the hand) that pro-
duces a f orce equal to the body
weight would exceed the critical
buck ling load and result in a mid-
shaf t clavicular f racture.16 Several
stu
dies
have de
mo
ns
tr
at
edth
at
a di-
rect f all or blow onto the point of the
shoulder accounts f or 85% to 94% of
the in juries.2,3,5,16,17 When the f orces
are transmitted through the arm, as
with a f all on an outstretched hand,
the f orces are not directly delivered
to the clavicle; thus, they are unlik e-
ly to produce a midshaf t f racture.
This mechanism accounts f or 2% to
5% of all midshaf t f ractures. A direct
blow to the clavicle, such as f rom a
hock ey stick or a seat belt shoulder-
strap in jury, also may produce a f rac-
ture and accounts f or 10% to 13% of
midshaf t f ractures in most stud-
ies.16 Although rare, direct f orce on
the top of the shoulder may drive the
midshaf t clavicle against the f irst
rib, resulting in a f racture.
C l a s s i f i c ati o n
Clavicular f ractures have been
classif ied b y Allman18 into three ana-
tomic regions, with the middle third
being group I. The classif ication sys-tem of the O rthopaedic Trauma As-
sociation separates diaphyseal cla-
vicular f ractures into three types:
06-A (simple), 06-B (wedge) and 06-C
(complex).19 Each type is f urther bro-
k en down into three groups.
The system developed by Robin-
son3 divides midshaf t clavicular f rac-
tures into type 2A (cortical align-
ment f racture) and type 2B (displaced
f racture). In an eff ort to provide di-
rection f or treatment and prognosis,
Robinson f urther divides these into
subgroup types 2A1 (nondisplaced),
2A2 (angulated), 2B1 (simple or
wedge comminuted), and 2B2 (isolat-
ed or comminuted segmental) (Fig-
ure 2). Robinson’s classif ication sys-
tem has demonstrated satisf actory
levels of interobserver and intraob-
server reliability and reproducibility.
However, additional studies are
needed to determine whether this
classif ication system will reliablypredict treatment and f unctional
outcomes.
C l i n i c a l E v a l u ati o n
Of ten with clavicular f racture, a
bruise or abrasion is seen, either over
the point of the shoulder (indicating
a direct blow) or over the midline
(suggesting a seat belt shoulder-strap
in jury). The shoulder has a droop,
the scapula appears slightly internal-
ly rotated, and the shoulder appears
shortened relative to the opposite
side. This characteristic def ormity is
produced by the pull of muscles at-
tached to the clavicle. Immediate
swelling may obscure the def ormity
of the bone, which will be seen on
radiographs if the f racture is dis-
placed. Palpation over the area will
reveal tenderness, and gentle manip-
ulation may produce crepitus and
motion at the f racture site. A non-displaced or minimally displaced
f racture may be suspected when pain
and / or sk in changes are present over
the clavicle.
Because middle third f ractures
f requently occur with high-energy
trauma, a complete examination
should be perf ormed to avoid miss-
ing associated in juries. Sk eletal in ju-
ries include f racture-dislocations of
the SC and AC joints or, in younger
patients, physeal in juries. Chest wall
trauma may result in high rib f rac-
tures, scapular neck and body f rac-
tures, and a pneumothorax or he-
mothorax. Although acute brachial
plexus in jury is rare, the ulnar nerve
is at highest risk because of its loca-
tion ad jacent to the middle third of
the clavicle. When a nerve in jury is
identif ied, a thorough vascular ex-
amination and evaluation of the
scapulothoracic articulation should
Figure 2
Robinson’s class ifica tion system for midshaft clavicular frac tures . (Re produced with
pe rmission from Robinson CM: Frac tures of the clavicle in the adult: Epide miology
and class ifica tion. J Bone J o i n t Su r g B r 1998;80:476-484.)
Kyle J. Jeray, M D
Volume 15 , Numbe r 4, Ap ril 2007 241

7/27/2019 Diafise Clavicula
http://slidepdf.com/reader/full/diafise-clavicula 4/10
be undertak en to avoid missing an
associated in jury. Penetrating trau-
ma is typically the cause of vascular
in jury. However, vascular in jury canoccur f rom blunt trauma, resulting
in spasm or thrombosis of the sub-
clavian vessels.
R a d i o g r a p h i cE v a l u ati o n
To determine the f racture pattern
and displacement, radiographs in
two pro jections are necessary. A
standard anteroposterior view should
be accompanied by a 45° cephalic tilt
view (Figure 3). The shoulder girdle
and upper lung f ields should be
caref ully assessed to avoid missing
associated f ractures or a subtle pneu-
mothorax. The radiographic evalua-
tion should assess the f racture pat-
tern, presence of comminution,
displacement, and shortening or dis-
traction of the f racture.
Several radiographic f indings can
help guide the surgeon’s choice of
treatment. Displacement without
bony contact, especially with a
transversely displaced f ragment, is a
risk f actor strongly predictive of long-term sequelae.7 Additional ra-
diographic parameters predictive of
increased risk f or pain, limitation of
motion, or nonunion include an
overall displacement of the f racture
ends >1.5 cm. This displacement in-
cludes shortening, distraction, or
separation of the ends in the anteri-
or or posterior direction in any radio-
graphic view.20-22 A second view, at
least 45° off plane f rom the f irst,
helps to f urther delineate the dis-
placement. Of ten, the displacement
is diff icult to assess on a single radio-
graph. For example, as seen in Figure
3, both views reveal distraction at
the f racture site of at least 1.5 cm.
M a n a g e m e nt
I n d i c a ti o n s
The primary goal in treatment is
to restore shoulder f unction to the
prein jury level. By allowing the clav-
icle to heal with minimal def ormity,
loss of motion and pain can be min-
imized. Indications f or nonsurgicaltreatment include a nondisplaced or
minimally displaced midshaf t clav-
icular f racture. Indications f or surgi-
cal treatment include open f ractures
and f ractures associated with sk in
compromise or with neurologic or
vascular in jury.
Relative surgical indications in-
clude certain multiple-system trau-
matized patients, a f loating shoulder,
and a painf ul malunion or nonunion.
More recently, relative indications
f or surgical treatment have been ex-
panded to include high-energy closed
f ractures with >15 to 20 mm of
shortening, f ractures with complete
displacement, and f ractures with
comminution.23-26 Although these re-
cently adopted indications have re-
ceived attention in the current liter-
ature, articles dating as f ar back as
the 1960s have described similar sur-
gical indications—including Neer’s
Figure 3
Standard rad iographic anteroposterior view (A) and 45° cephalic tilt view (B). B oth are necessary to de termine the ext ent of
frac ture disp lac ement.
Ac ute Midshaft C lavicular Frac ture
242 Journa l of the American Academy of O rthopaedic Surgeons

7/27/2019 Diafise Clavicula
http://slidepdf.com/reader/full/diafise-clavicula 5/10
article,17 which is of ten cited as sup-
port f or nonsurgical management.
Randomized controlled trials, one of
which has recently been complet-
ed,11 and another that is currently
under way, are necessary to deter-
mine w
he
the
r these
r
ela
tive
ind
ica-
tions should be considered routine
and, if so, in which patients with
which f racture types.
N o n s u r g i c a l T r e atm e nt
Historically, nonsurgical treat-
ment has been the mainstay f or
clavicular f ractures. It has varied
f rom plaster shoulder spica casts to
benign neglect. Most commonly, a
sling or f igure-of-8 brace is applied
in the acute setting. With either de-
vice, immobilization is typically f or
2 to 6 week s, based on the patient’s
level of comf ort. Of ten, mild dis-
comf ort can linger in adults f or
3 months. Return to athletics or
heavy labor is permitted 4 to 6
week s af ter clinical and radiograph-
ic union has occurred. Light work
with restricted overhead activity
can begin once the patient’s comf ort
allows, usually in 2 to 4 week s af ter
f racture healing.
In a prospective, randomizedstudy,27 26% of patients treated with
a f igure-of-8 bandage were dissatis-
f ied compared with 7% of those
treated with a sling. The patients
treated with a sling reported less dis-
comf ort. There was no diff erence in
overall healing and alignment of the
f ractures, indicating that a f igure-
of-8 bandage does little to obtain or
maintain reduction.
S u r g i c a l Te c h n i q u e s
Pl ate s
Open reduction and internal f ixa-
tion using plates and screws can be
done with the patient in either the
supine or the beach-chair position,
with the head and neck tilted away
f rom the surgical site. A bump is
placed behind the scapula to aid in
the reduction. The arm is prepped in
the f ield to allow f or traction and
manipulation to assist in the reduc-
tion. Traditionally, a sk in incision is
made over the clavicle f ollowing
Langer’s lines, as the sk in permits. A
newly described alternative is to in-
cise the inf erior sk in af ter pulling it
over the f racture site.28 As the sk in is
released, it will f all 1 to 2 cm below
the clavicle and prevent the woundf rom being in contact with the plate
on the clavicle. The aim is to im-
prove cosmesis and prevent wound
complications. The dissection is
tak en down to bone with care to
identif y the cutaneous supraclavic-
ular nerves. When necessary, they
can be sacrif iced. It is important to
inf orm the patient bef ore surgery of
the possibility of a patch of numb-
ness in the sk in inf erior to the clav-
icle.
Minimizing subperiosteal strip-
ping with gentle handling of the sk in
and sof t tissue helps avoid complica-
tions. The plate usually is placed on
the tension side of the bone—f or the
clavicle, the anterosuperior position
(Figure 4). Biomechanically, this
position provides the best stabili-
ty.29 However, clinically successf ul
treatment with anteroinf erior place-
ment also has been described.30 The
anteroinf erior position, although
less f avorable biomechanically,29 al-
lows f or drilling in a direction away
f rom the subclavian vessels and
lung. It also k eeps the plate f rom be-
ing placed under the incision. This
position theoretically is less lik ely to
cause irritation, thereby decreasingthe need f or plate removal. However,
the anteroinf erior position demands
additional sof t-tissue stripping and a
more diff icult contouring of the
plate compared with the anterosupe-
rior position.
Ideally, a 3.5-mm dynamic com-
pression plate or plate of similar
strength should be used, with at
least six cortices on each side. Semi-
tubular plates are not as rigid and
should not be used.24,31 Reconstruc-
tion plates are more easily contoured
and have been used with success;
however, they account f or several
f ailures to obtain union and would
not be the author’s f irst choice.24,31
Precontoured plates of suitable
thickness off er the advantage of ease
of placement without manipulation
of the plate. Lock ed plates are not
necessary f or the acute plating of
nonosteoporotic clavicular f ractures;
Figure 4
An teroposterior rad iog raph demons trating clavicle plating in the anterosuperior
position , us ing a 3.5-mm limited-con tac t dynamic compress ion plate.
Kyle J. Jeray, M D
Volume 15 , Numbe r 4, Ap ril 2007 243

7/27/2019 Diafise Clavicula
http://slidepdf.com/reader/full/diafise-clavicula 6/10
there is no signif icant advantage
over conventional plating, and the
cost is higher.
Once plating is completed, the
f ascia is repaired over the plate, if
possible, and the sk in incision is
closed. Suture closure is pref erable
to staples. With a suff iciently stableconstruct, unrestricted shoulder mo-
tion is allowed, with the exception
of overhead lif ting f or 6 week s. Of-
ten, the pain relief associated with
stabilizing the f racture is dramatic,
and eff orts to limit the patient’s ac-
tivity may be needed. Pain relief is
cited as one of the potential benef its
of surgical intervention.
In tr a m e d u l l a r y F i x ati o n
An
alt
ern
ativ
eto pl
ating i
sin-
tramedullary (IM) f ixation. Many
variations of IM implants have been
described over the past 40 years, in-
cluding Hagie pins, modif ied Hagie
pins, Knowles pins, Herbert screws,
Steinmann pins, elastic nails, can-
cellous screws, and Kirschner
wires.32-36 Modif ications in the tech-
nique have led to a resurgence of in-
terest in IM f ixation of these f rac-
tures. The potential benef its of IM
f ixation compared with plate f ixa-
tion include less sof t-tissue stripping
at the f racture site, better cosmesis
with a smaller sk in incision, easier
hardware removal, and less weak -
ness of the bone af ter hardware re-
moval. Biomechanically, however,
the ability to resist torsional f orceswith IM f ixation is much less than
that with a plate. Migration of the
pins also has been a ma jor concern.
Newer designs, which include lock -
ing nuts on the lateral end of the IM
devices, prevent medial pin migra-
tion. Newer techniques that avoid
penetration of the medial f ragment
cortex also prevent medial migration
of the devices.34
Patient positioning is similar to
th
at f or pl
at
ef ix
ation.
A sm
all in
ci-
sion is made over the f racture site,
exposing the f racture ends. The me-
dial segment is prepared by drilling
into the medullary canal, but the an-
terior medial cortex is not violated.
The distal segment is drilled retro-
grade through the canal, exiting the
posterior lateral cortex. The pin is
inserted retrograde through the ca-
nal and exits through the posterolat-
eral hole and out the sk in. Next, the
f racture is reduced, and the pin is ad-
vanced antegrade across the f racture
into the medullary canal of the me-
dial segment. The Rock wood Clavi-
cle Pin (DePuy Orthopaedics, War-
saw, IN) has two nuts that go over
the
thr
eaded en
d of th
ein
sert
ed pin
posterolaterally. Once the pin is
across the f racture, the f irst nut is in-
serted posterolaterally, compressing
the f racture, f ollowed by the second
nut, which is cold-welded to the
f irst. Figure 5 shows the Rock wood
Clavicle Pin in place. Some of the IM
techniques vary slightly depending
on the device, and not all of the tech-
niques allow f or f racture compres-
sion.
Patients are allowed to begin
shoulder motion immediately post-
operatively. When rotational stabil-
ity is a concern, f orward elevation
should be restricted to 90° and ab-
duction to 90° f or the f irst 4 week s.
The Rock wood pin should be re-
moved at 8 to 14 week s. In some sit-
uations, this can be done under local
anesthesia in the off ice; however,
most Rock wood pins need to be re-
moved in the operating room. Some
of the other IM devices, such as Her-
bert screws, do not need to be re-moved.
As with plating, a ma jor benef it is
early return to activities. Several
studies have reported athletes’ re-
turning to their sport activities by
2 to 3 week s.35,37
C o m p l i c ati o n s
Complications can occur f rom non-
surgical treatment as well as surgical
treatment. Both can produce a cos-
metic def ormity (Figure 6). Both can
result in malunion, nonunion, pain,
local tenderness or irritation, and
limitation of motion. Other rare
complications f ollowing surgical or
nonsurgical treatment are residual
nerve paresthesia; subclavian ves-
sel compression, thrombosis, and
pseudoaneurysm; thoracic outlet
syndrome; and brachial plexus neu-
ropathy.
Figure 5
An teroposterior rad iograph demons trating the Rockwood C lavicle Pin (DePuy
O rthopaed ics). No te tha t the anteromed ial cortex is not violated , preventing the pin
from m igrating med ially.
Ac ute Midshaft C lavicular Frac ture
244 Journa l of the American Academy of O rthopaedic Surgeons

7/27/2019 Diafise Clavicula
http://slidepdf.com/reader/full/diafise-clavicula 7/10
Some complications are unique
to surgical intervention, such as in-
f ection and hardware problems. In-
f ection rates vary f rom 0% to 18%,with the lower rates reported in the
more recent studies.24,31,37,38 Painf ul,
irritating hardware requiring plate or
pin removal is reported to be as high
as 50% to 100%.24,39 Following plate
removal, the risk f or ref racture rang-
es f rom 0% to 8%.24,31 Adhesive cap-
sulitis of the shoulder has been re-
ported with surgical treatment in
0% to 7% of cases.24,28
IM devices are associated with
unique complications, including mi-
gration of the pin and hardware irri-
tation, resulting in local sk in break -
down that of ten requires antibiotics
and, ultimately, hardware remov-
al.39 Figure 7 illustrates sk in break -
down f rom an IM pin. Although
most of these complications are rare,
a second surgery f or plate or pin re-
moval is suff iciently f requent to be
considered when reviewing treat-
ment choices.
R e s u lts
Whether treated nonsurgically or
surgically, most clavicular f racturesheal without incident when length
and alignment are maintained. Ac-
ceptable cosmetic and f unctional re-
sults should be expected. Satisf acto-
ry results occur less consistently
when the f racture f ails to heal or
heals with a signif icant def ormity.
N o n u n i o n
Most cases of nonunion are symp-
tomatic, presenting with pain, loss
of f unction, neurologic changes,
and / or unsightly clavicular def ormi-
ty. Although clavicular nonunion
has not been clearly def ined in the
literature, most authors concur that
nonunion is present when healing
has not occurred by 16 week s.
Traditional think ing is that cla-
vicular f ractures treated nonsurgical-
ly almost always heal and that surgi-
cal treatment increases the risk of
nonunion. Rowe4reported a non-
union rate of 3.7% in patients who
underwent surgery compared with
0.8% in those treated without sur-
gery. Neer17 reported nonunion ratesof 0.1% with nonsurgical treatment
and 4.6% with surgical treatment.
Neer17 suggested that the most im-
portant causal f actor f or nonunion of
a midshaf t clavicular f racture is im-
proper open surgery. This may be
true to some extent; aggressive sof t-
tissue stripping, inability to reduce
the f racture, and inadequate internal
f ixation all can lead to poor results.
Several recent studies have re-
ported high union rates with surgical
intervention using a variety of inter-
nal f ixation devices, including plat-
ing and IM pin or rod f ixation.39,40 In
addition, there is evidence that the
nonunion rate af ter nonsurgical treat-
ment may be higher than previously
reported, particularly in certain f rac-
ture types and in certain patients. In
their review of 581 nonsurgically
treated f ractures, Robinson et al20re-
ported an overall nonunion rate of
Figure 6
A, Hea led clavicular frac ture managed nonsurgica lly. The bump, shortened shoulde r width, and subtle droop are evide nt.
B, A healed clavicu lar frac ture trea ted with plate and screw s, showing prominence of the anterior-superior–positioned plate.
Kyle J. Jeray, M D
Volume 15 , Numbe r 4, Ap ril 2007 245

7/27/2019 Diafise Clavicula
http://slidepdf.com/reader/full/diafise-clavicula 8/10
4.5% f or diaphyseal f ractures. Strat-
if ication of Robinson’s data revealed
that women with displaced diaphy-
seal f ractures had a nonunion rate
ranging f rom 19% to 33%. When
comminution was combined with
displacement, the nonunion rate in
women increased to a range of 33%
to 47%.41 In addition to f racture f rag-
ment displacement, f emale sex, and
comminution, other risk f actorsidentif ied with nonunion include ad-
vancing age, lack of cortical apposi-
tion, severity of the initial trauma,
the extent of f racture f ragment dis-
placement,25 and, arguably, sof t-
tissue interposition.42 Early mobiliza-
tion has not been associated with the
development of a nonunion, whether
treated surgically or nonsurgically.
A recently published systematic
review of the literature on nonunion
af ter treatment of midshaf t clavicu-
lar f ractures revealed a 5.9% non-
union rate in nonsurgically managed
f ractures.8 In the completely dis-
placed f ractures, the rate increased to
15.1%. In surgically treated displaced
f ractures, plating of 460 f ractures re-
sulted in a nonunion rate of 2.2%,
and IM f ixation of 152 f ractures re-
sulted in a nonunion rate of 2.0%.8
These data should be interpreted
with caution, however, because most
were f rom evidence-based level III,
IV, and V studies (ie, observational,
retrospective, case series, and expert
opinion studies) rather than f rom
level I and II studies (ie, randomized,
prospective studies).
Surgical treatment of nonunion
has a high success rate. Techniques
include plate f ixation with bone
graf t, IM pin f ixation with bone
graf t, and external f ixation. Unionrates with each method have been
reported to be >92% and as high as
100%.42-45 Plate f ixation has the
largest support in the literature and
is currently the most predictable
and recommended treatment f or
symptomatic nonunion. Other
methods may be successf ul in the
hands of an experienced surgeon.
M a l u n i o n
Most nonsurgically treated cla-
vicular f ractures heal with some de-
f ormity. The literature does not
clearly def ine when a def ormity is
considered to be a malunion; howev-
er, the evidence strongly suggests
that some clavicular def ormities re-
sult in unsatisf actory outcomes. The
def ormity is a three-dimensional
problem; the most consistent char-
acteristic is shortening with inf erior
displacement of the medial f rag-
ment. Symptomatic patients help
def ine the malunion. Symptoms in-
clude weakness and pain in the in-
volved shoulder, loss of shoulder
motion, loss of endurance, neurolog-
ic symptoms consistent with thorac-
ic outlet syndrome and brachial
plexus impingement, and cosmetic
def ormity.46
In 1986, Esk ola et al21 noted in
89 patients that shortening >12 mmwas associated with increased pain.
Wick et al22 concluded in a retrospec-
tive study that shortening of 2 cm in
midshaf t clavicular f ractures was as-
sociated with an increased risk of
pain, limitation of motion, or non-
union. McKee et al9 assessed f unc-
tional outcome f ollowing displaced
clavicular f ractures and noted signif-
icantly inf erior scores f or both the
upper extremity–specif ic (DASH)
outcome scores (P = 0.02) and the
Constant scores (P = 0.01) compared
with the general population. They
concluded that f ractures with >2 cm
of shortening tended to be associated
with decreased abduction strength
and greater patient dissatisf action.
Hill et al25reported on completely
displaced middle third clavicular
f ractures and concluded that f inal
shortening ≥2 cm was associated
with an unsatisf actory result but not
Figure 7
H ea led clavicu lar frac ture trea ted with intramedullary pinning . A, No te inc ision size and loc ation over frac ture and posterolateral
prominence. B,
Ea rly breakdown of the skin resu lting from a prominent pin at the posterolateral inse rtion site.
Ac ute Midshaft C lavicular Frac ture
246 Journa l of the American Academy of O rthopaedic Surgeons

7/27/2019 Diafise Clavicula
http://slidepdf.com/reader/full/diafise-clavicula 9/10

7/27/2019 Diafise Clavicula
http://slidepdf.com/reader/full/diafise-clavicula 10/10