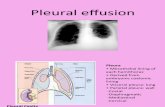
CPC Pleural Effusion
Transcript of CPC Pleural Effusion

Maria Regina Capoquian De Jesus 49 years old female Single Unemployed Catholic Filipino born on July 18, 1962 in Manila presently residing at Block 15 Lot 27
Archilles Street, North Olympus admitted for the first time in FEU-NRMF
Medical Center on March 9, 2012

Shortness of breath

• 2 weeks prior to admission
on and off non-productive cough
pleuritic chest pain radiating to the back with a pain scale of 6/10
intermittent moderate to high grade fever of 39-39.9C usually manifest in the evening
chills easy fatigability.

• Medication taken : Paracetamol 500 mg/tablet, taken every 4 hours which afforded temporary relief.
• No other medications taken.• No associated signs and symptoms
such as loss of appetite, abdominal pain, nausea and vomiting.
• Consultation was done at ACE diagnostics where chest XRAY, CBC, ECG were done.
• Chest X-RAY revealed pleural effusion.

• Had measles, mumps and chicken pox• Unrecalled immunizations• 2009 – Diagnosed with rheumatic heart
disease at Philippine Heart Center.• 2010 –Percutaneous Transvenous Mitral
Commissurotomy (PTMC) was done at Philippine Heart Center ; Blood transfusion was done ; no complications noted.
• No history of accidents, injuries, psychiatric disorders; no known allergies

• Father – Deceased at the age of 79 due to pleural effusion and heart disease
• Mother – 69 years of age, hypertensive
• 6 siblings are all apparently well, one of them with arthritis.
• No other heredo-familial diseases aside from hypertension, stroke, colon cancer (maternal).

• Patient is living with her partner for 20 years with 6 children, all apparently well.
• A high school graduate• used to work as a wedding planner in
the past. • A non- smoker nor an alcoholic drinker• No particular food preference

• She is currently living with 4 household members in a well-lit, well ventilated bungalow type of house with 1 bedroom and 1 bathroom
• Source of water is from Maynilad but drinking water is mineral water.
• Garbage is collected twice a week.

• Menarche at age of 15, with regular 28-day cycle, lasting for 3 days, heavy to moderate in amount.
• LMP – April 26, 2012• Patient is a G5P5(5005).• All pregnancies were delivered via
normal spontaneous delivery, assisted by a birth attendant at home.
• Calendar method is used as method of contraception.

• No abnormal findings

Patient is conscious, coherent, oriented to time, place and person, looks appropriate for her age, in respiratory distress, no gross deformities, with the following vital signs:BP:110/70 CR:81 RR:21 Temp: 37.4

PERTINENT FINDINGS:
Lungs/chest: decreased breath sounds on the right mid to base, decreased tactile and vocal fremitus on the right
Heart: tachycardia , irregular rhythm
Abdomen: globular

• No abnormal findings


Rule in Decreased fremitus Decreased breath sounds Decreased voice transmissions No adventitious soundsRule out Hyperresonant upon auscultation (-) smoker Predilection to upper lobes
(centriacinar)

Rule inDecreased fremitusDecreased breath sounds Decreased voice transmissionsNo adventitious sounds (+) Pleuritic chest painRule outHyperresonant upon auscultation

Rule in Dull Decreased fremitus Decreased breath sounds Decreased voice transmission No adventitious sounds Dyspnea Density on the right upper lobeRule out Trachea is in midline

Rule in (+) density on upper third of right
lungFatigueFeverChest painRule out Non productive cough

Pleural effusion secondary to increased vascular permeability due to community acquired pneumonia

Rule in High fever 39-39.9C Chills (+) Pleuritic chest pain Dullness in percussion Absent fremitus Homogenous density on the right lower lobe
on CXR Febrile Tachycardic Non productive cough Easy fatiguability Has RHD

Rule inDullDecreased fremitusDecreased breath sounds Decreased voice transmissions No adventitious soundsFather died because of pleural effusion

Accumulation of pleural fluid occurs in the following settings:
Increased hydrostatic pressure, as in congestive heart failure
Increased vascular permeability, as in pneumonia
Decreased osmotic pressure, as in nephrotic syndrome
Increased intrapleural negative pressure, as in atelectasis
Decreased lymphatic drainage, as in mediastinal carcinomatosis

Aspiration of oropharyngeal
secretions containing
microorganism
Inhalation of microorganism that have been
released into the air
Overcome of respiratory barriers
Overwhelming of alveolar
macrophagesNon
distressing, non
productive cough

Activation of inflammatory
response
Release of inflammatory
mediators(IL 1 and TNF)
Release of chemokines
(IL 8 and GCSF)
Stimulate release of neutrophils and their attraction to lungs
Fever T 39 – 39.9C,Chills
Increased alveolar capillary membrane permeability **

presence of Infiltrates
Altered gas exchange
Easy fatigabil
ity

Leakage of exudates from
interstitial spaces of lungs to the pleural
space
Increase pleural
fluid
Pleural fluid formation > pleural fluid absorption
Accumulation of pleural
fluid
Pleuritic chest pain
Shortness of breath
Dull upon percussion(-) fremitusXray results decreased
breath sounds
**

Diagnostic Tests/ Laboratory Tests

A. Imaging I. Chest X-ray II.CT-scan III.UTZIV.Microscopy



B. Thoracentesis to determine the cause; specific tests for:
•Chemical composition:– Lactate dehydrogenase (LDH)– Albumin– Amylase– Glucose– pH
•Gram stain and culture•Cell count and differential•Cytopathology •Others:
– lipids, fungal culture, viral culture, specific Igs

DENSE / OPAQUE STRUCTURES
LESS DENSE / SOFT TISSUE
BASIC RADIODENSITIES


-Serosal membrane that envelopes the lungs
-Composed of the visceral and parietal pleura
-Contains less than 5 ml of fluid in each pleural space

Presence of fluid at the pleural space
-Obliteration of the lateral costophrenic angle in an upright view estimates a volume of 150-300 ml
Homogenous lower zone opacity with convex interface – “Meniscus Sign”
Contralateral mediastinal shift Thickening of the pleural septa



To provide adequate ventilation and oxygenation therapy for hypoxemia
To determine the appropriate pharmacotherapy
To provide appropriate supportive care
To give follow-up and preventive care needed.

Surgical intervention: VATS
Oxygen supplementation at 2 to 3 liters per minute via nasal cannula
Relieving the patient of his secretions via chest physiotherapy or coughing exercises


To view inside of the chest cavity after making very small incisions.
To remove masses in the lung and test them for cancer
For diagnosis of infections or tumors of the chest wall and treating collapsing lungs.

Four one inch incisions
1-2 day hospital stay
Markedly reduction in recovery time
Significantly reduced complication rate

Consent
Pulmonary function tests
Stop or adjust the dose of medications like aspirin/ NSAIDs
NPO for at least eight hours before the surgery

• Under general anesthesia
Very small incision on seventh and eighth ribs
Carbon dioxide gas is allowed to flow into
the chest through this opening
A thoracoscope is inserted through the opening on the chest to see the work on a video screen.

1 or 2 small are made along the lower ribcage to cut a section of the lung
Seal the hole in the lung thru staples
At the end of your surgery, the instruments are removed, the lung is reinflated, and all but one of the small incisions are stitched closed.
Chest tube is placed to drain leaking air or fluid that collects after the surgery.


ScarAir LeakBleedingPain in the chest area


1.EMPIRICAL2.DEFINITIVE3.SUPPORTIVE

Initial Antibiotic Treatment:
EmpiricalTo cover most likely pathogens
The coverage is always provided for pneumococcus and atypical pathogens
Atypical pathogen coverage macrolide + cephalosporin / fluoroquinolone



Definitive
CULTURE etiologic agent and susceptibilities are known through culture
Combination therapy (macrolide and ß-lactam)


SUPPORTIVE
Mucolytics: AcetylcysteineRespiratory inhalant that thins mucousExpectorantIt acts by signaling the body to increase the amount or hydration of secretionsNebulization It dilates the lung passages offering relief of symptoms including shortness of breath

Practice good hygiene
Influenza shot each fall
Pneumonococcal vaccine
Practice good preventive measures by eating a proper diet, getting regular exercise and plenty of sleep
No smoking

Take the entire course of any prescribed medications.
Get plenty of rest. Drink lots of fluids, especially
water. Keep all of follow-up appointments. Encourage the guardians to wash
patient’s hands. Tell guardians to avoid exposing
the patient to an environment with too much pollution.
Give supportive treatment. Protect others from infection.