COPP MODULE - iapindia.org · Pityriasis alba Pityriasis means brawny scales Alba means white....
Transcript of COPP MODULE - iapindia.org · Pityriasis alba Pityriasis means brawny scales Alba means white....

COPP MODULE
COMMON OFFICE PRACTICE PEDIATRIC PROBLEMS[A MODULE OF IAP TAMILNADU STATE CHAPTER 2017]

TEAM• Scientific advisors Dr P Ramachandran, Dr S Balasubramanian
• Conveners Dr S Thirumalai Kolundu, Dr Sunil Srinivasan
• Scientific Coordinator Dr A Somasundaram
• Academic coordinators Dr S Narmada, Dr R.V Dhakshayani
• Academic committee [MODERATORS]• Dr NC Gowrishankar,• Dr T N Manohar,• Dr K Nedunchelian,• Dr Rema Chandramohan,• Dr R Somasekar,• Dr S Thangavelu,• Dr V V Varadarajan

CONTRIBUTORSDr RV Dhakshayani Dr A SomasundaramDr Giridhar Dr Somu SivabalanDr Hemchand K Prasad Dr S SrinivasDr E Mahendar Dr P SudhakarDr S Mangalabharathi Dr Sudharshana skanda Dr Manikandan Dr B SumathiDr Manikumar Dr Suresh Dr S Narmada Dr VenkateshwaranDr Palaniraman Dr C VijayabhaskarDr R Selvan

Dr.Vijayabhaskar.c MBBS, DCH,MD (Derm)
• Assistant Professor, Department of Dermatology, GGH, MMC• Posts Held
– EB Member in Indian Journal of Practical Pediatrics– President – IAP Dermatology Chapter – From 2004 to 28th January 2012– Treasurer – IAP Dermatology Chapter – From 28th January 2012 till date – Organising Secretary of 1st National congress of Pediatric Dermatology, DERMPED 2004, held in
Chennai.– Organising Secretary of 2nd National Congress of Pediatric Dermatology, DERMPED 2006, held in
Chennai.– Hony. Treasurer, 3rd National Congress of Pediatric Dermatology, DERMPED 2009, held in Chennai.– Faculty for the Refresher Course held for practising pediatrician in the field of pediatric Dermatology,
Chennai in 2005– Organising Committee member for the CME on Pediatric Dermatology held in Chennai in the year
2008, 2009 and 2010– Executive member of INSTED (Indian Society of Tele Dermatology)– Hon. Treasurer, IADVL Tamil Nadu Branch 2011 - 2012
• Special interest -Neonatal Dermatology • Delivering lectures in IMA forum and CME in various places.• Attending Medical camps at various places as a member of IAP• Contributed articles in Indian Journal of Practical Pediatrics on various Pediatric dermatology topics

HYPOPIGMENTATION PATCHES - AN APPROACH
DR.C.VIJAYABHASKAR., Moderator
Dr. Gowrishankar

Hypopigmented patches
Fear
uncertainty
patient
physician
Anxiety

Hypopigmented patchesWith scaling
With out scalingWith organ involvement

Hypopigmentation with scaling
Pityriasis albaPityriasis versicolor
Polymorphous light eruptionSeborrheic dermatitis

Hypopigmentation without scaling
Hansens’s DiseaseEarly vitiligo
Nevus Contact with topical depigmenting agents
Post inflammatory hypopigmentation

Hypopigmentation with organ involvement
Hypomelanosis of ItoTuberous sclerosis

Hypopigmentation with surface changes
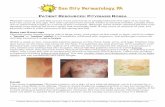
Pityriasis alba

Pityriasis alba
Pityriasis means brawny scalesAlba means white


Diagnostic points
• Scaling • Hypopigmentation• Borders – well defined or ill defined margins• Single or multiple patches over the face or
upper back and arms

Treatment• Reassurance • Emollients only twice daily for 1 month• 1% Hydrocortisone cream twice daily over the patch
for 2 to 4 weeks• If it doesn’t disappear Topical Tacrolimus 0.03% from 2
to 14 years of age or 0.1% ointment above 14 years – once daily at night for 4 to 8 weeks
• If it doesn’t disappear Ref to the Dermatologist• Chronic course – Camouflage• In children above 8 years of age PUVA therapy or
PUVASOL could be tried.

Treatment
• It is an endogenous eczema more common in atopics
• Deworming and Multivitamins have no role

Seborrheic dermatitis
•Multiple scaly macules and patches seen over the face•Asymptomatic •May be associated with scaling over the scalp•Treatment•Emollients•Topical 1% Hydrocortisone cream twice daily over the affected area for 2 to 4 weeks

Treatment for the scalp
• Ketoconazole lotions• Ketaconazole lotions with ZPT • To be applied over the scalp and rinse after 5
to 10 minutes with any antidandruff shampoo twice a week for 3 months



Pityriasis versicolor
• Pityriasis meaning scales• Versicolor meaning various colours• Black or white or both• White patches common over face and trunk• Black common over trunk

Diagnosis
• Commonly over the face, chest, back and arms (Seborrhoeic areas)
• Single or multiple macules to patches• Scaling• Borders are well defined• May be white in colour or black in colour

Pityriasis versicolor
• Diagnosis if in doubt by scraping and examination under KOH -spaghetti and meat ball appearance
TreatmentTopical azole group of drugs -Clotrimazole, micanozole, ketoconazole cream(any
one) twice daily for 6 weeksIf extensive oral fluconazole given along with topicals-8 to 12mg/kg/dose stat and repeat after 1 week

Treatment for extensive trunk lesions
• 2.5% selenium sulphide to be applied below the neck upto arms and waist 10 minutes before bath daily once for 2 weeks.
• Lesions will persist as mycological cure occurs with 2 weeks but cosmetic cure occurs after 6 weeks
• Never selenium suphide over the face and do not leave it for long duration as it is a irritant

Polymorphous light eruption
• Common in the exposed areas like face, neck and forearms
• h/o photosensitivity + and itching present• Erythema • Hypopigmented scaly patch or papules

Polymorphic light eruption

Polymorphous light eruption
•Sun protection in the form of wearing hat or cap•Protection of forearms by wearing cotton gloves•Wearing full sleeve shirts•Avoid sandal containing soaps or powders•Avoid turmeric topically

Treatment
• Topical steroids Desowen or 1% hydrocortisone cream twice daily for 2 to 4 weeks or till lesions disappear whichever is early
• Sunscreen lotions or gel with an SPF of 15 to 26 • Apply before 8 in the morning and repeat at 12 noon
over the face, neck, upper back and arms forearms and hand for 2 to 3 years
• Antihistamines for 2 weeks

Hypopigmentation without scaling
Hansens’s DiseaseEarly vitiligo
Nevus Contact with topical depigmenting agents
Post inflammatory hypopigmentation

Hansen’s disease



Diagnostic criteria
• Hypopigmented non scaly patch• Impaired sensation or loss of sensation over the
patch• May be associated with loss of hair or loss of
sweating over the patches

Hansen’s Disease
• Screen other family members• Incidence in children reflects the disease burden in the
society• Investigation• Slit skin smear may be negative and not done routinely• Biopsy and histopathology is confirmative• Treatment -- paucibacillary and multibacillary
regimens• Better refer to the Dermatologist

Early vitiligo


Hypopigmentation without surface changes
Early vitiligo

Criteria
• Hypopigmented patches and later depigmented patches
• No loss of sensation or impairement of sensation• Hair over the lesional area may be black or white• Normal sweating and no loss of hair

Treatment
• Better refer the patient to the Dermatologist• Reassurance• Topical steroids in the form of fluticasone,
mometasone cream initially for 4 weeks depending upon the age
• Topical tacrolimus or pimecrolimus• Narrow band UVB therapy• PUVA therapy• PUVASOL• Immunomodulatory therapy

Post inflammatory hypopigmentation
•History of impetigenous or some inflammatory lesions at the site•History of topical application of steroids

Treatment
• Reassurance• Most of the lesions repigmented in the course of time

Nevus achromicus

Nevus depigmentosus• Present at birth ( Birth mark )
• Unilateral
• Localized
• Borders may be regular and at times irregular
• Sometimes the lesions may be whorled

Treatment
• Reassurance• If cosmetically disfiguring refer to the Dermatologist• Lasers could be tried

Hypopigmentation with organ involvement
Hypomelanosis of ItoTuberous sclerosis

Tuberous sclerosis complex
Ashy leaf macule

Tuberous sclerosis complex
Neonatal screening is mandatory in some of the countries.Wood’s Lamp is used

Tuberous sclerosis complex
Common sites• Posterior trunk, extremities and head and neck
pathogenesis• Reduction in the amount of epidermal melanin with normal
number of melanocytes
Course and treatment• Fades as child matures into adulthood• Makeups, camouflage

Hypomelanosis of Ito
• Present at birth• Bizarre hypopigmented lesion in the skin that
follow Blaskco’s lines

Hypomelanosis of Ito
Can involve the entire half of the body
Rarely bilateral

Hypomelanosis of Ito
May have associated skeletal, neurological and/or ocular abnormalities

Hypomelanosis of Ito
Treatment• None• Refer to appropriate specialist if they have
neurological, skeletal or ophthalmologic problem.